Abstract
Importance
Mentorship is increasingly recognized as a critical part of training across the spectrum of trainees. While explored more in-depth in the literature of other medical specialties, mentorship remains a nascent topic in the Otolaryngology Head and Neck Surgery (OHNS) literature.
Objective
The objective of this study was to assess the current literature on mentorship in OHNS.
Design
The Preferred Reporting Items for Systematic Reviews and Meta-Analyses extension for Scoping Reviews guidelines was used and the methodology was registered on Open Science Framework (https://doi.org/10.17605/OSF.IO/X5FQ7). The Medline, EMBASE, and Web of Science databases were searched. Two authors independently selected studies, with the senior author resolving discrepancies. Study quality was assessed using the Oxford Centre for Evidence-Based Medicine levels of evidence.
Setting and Participants
English language studies employing any methodology that involved mentorship of medical trainees and staff in OHNS were included from the inception of the database up to September 20, 2023.
Intervention or Exposures
Any form of mentorship.
Main Outcome Measure
The primary outcome was the benefits of mentorship afforded to the mentee.
Results
From 415 unique articles identified, 45 studies were included. The median publication year was 2020 (IQR 6.5, range 1999-2023). The major themes of benefits from mentorship include improving residency uptake (n = 22), clinical competency and professionalism (n = 20), diversity and equity (n = 19), research productivity (n = 17), career planning and advancement (n = 17), and quality of life (n = 11). Other common themes included active mentorship (n = 29), near-peer mentorship (n = 13), and utilizing digital tools for mentorship (n = 6).
Conclusion and Relevance
Mentorship in OHNS has seen a sharp increase in publications in recent years. There are numerous benefits to mentorship including improving residency uptake, diversity initiatives, clinical competency and professionalism, research productivity, career planning and advancement, as well as quality of life.

Introduction
Mentorship is defined as the process whereby an experienced, highly regarded empathic person (the mentor) guides another individual (the mentee) in the development of their learning and professional development. 1 Mentees can be individuals at any level of training, including undergraduates, medical students, residents, fellows, and faculty. Traditionally, mentorship in medicine followed a “passive” model, relying on chance encounters and benefiting those with greater social capital and mentor similarities.2,3 Recent studies advocate for “active” mentorship, promoting equal access through structured programs. Other new strategies such as near-peer mentorship and digital tools also improve access.
Mentorship has a variety of benefits at both the system and individual levels. Mentorship can improve residency uptake, which involves medical students becoming interested in, pursuing, and matriculating to Otolaryngology Head and Neck Surgery (OHNS) residency programs. 4 Mentorship is recognized to promote diversity across different specialties,4 -8 which is relevant to OHNS with its lower representation of minorities and women.9,10 Mentorship enhances clinical competencies and virtues of professional behavior, with evidence supporting its role in improving patient outcomes and care quality.11,12 In addition, mentorship in research fosters collaboration on innovative projects and high-quality outputs.11,12 Mentors also provide invaluable career, networking, and professional development advice.12,13 Finally, mentorship could reduce burnout, offer emotional support, promote work-life balance, and improve job satisfaction and faculty retention.6,14,15
While there is a growing body of evidence supporting the benefits of mentorship in OHNS, awareness within the specialty remains limited. This study aims to review the current literature on mentorship in OHNS overall and to identify prominent themes with the primary outcome being the benefits of mentorship.
Methods
This scoping review was conducted according to the Preferred Reporting Items for Systematic Reviews and Meta-analyses Extension for Scoping Reviews (PRISMA-ScR) guidelines utilizing the methodology registered on Open Science Framework (https://doi.org/10.17605/OSF.IO/X5FQ7). 16
Data Sources and Search Strategy
The MEDLINE, EMBASE, and Web of Science databases were queried in September 2023, using a search strategy peer-reviewed by a medical librarian under the Peer Review of Electronic Search Strategies (PRESS) criteria. 17 The medical subject headings (MeSH) terms “Mentors,” “Mentoring,” “mentor,” “otolaryngology,” “neurotology,” and “otorhinolaryngology” with relevant keywords were used to search the databases. The exact searches and their results are found in Supplemental Table 1.
Inclusion and Exclusion Criteria
Articles focusing on the mentorship of medical trainees and staff in otolaryngology were included, from database inception to the time of the search. Any study that involved mentorship of individuals who were allied healthcare professionals or in non-OHNS specialties was excluded. Articles that were not relevant or non-English were also excluded.
Selection and Appraisal of Studies
All search results were uploaded to the Covidence (Melbourne, Australia) reference manager software, which automatically removes duplicates. Title-abstract and full-text review was performed independently by authors D.V. and N.B. Discrepancies were settled by A.H.
Data Extraction
Data were extracted from included studies by D.V. and N.B. utilizing a predefined template that includes the study type, level of evidence, study design, author, years of study, country of the senior author, the objective of the study, details of the mentee population, details of the mentor population, and benefit of mentorship afforded to mentees. Discrepancies were settled by consensus.
Level of Evidence
The 2011 Oxford Centre for Evidence-Based Medicine (OCEBM) levels of evidence were assigned to each study as an indicator of the potential bias. 18
Synthesis of Results
Descriptive statistics were performed. Findings were described qualitatively. The Thomas and Harden framework was utilized for qualitative analysis. 19 No meta-analysis was conducted due to the heterogeneity of reported outcomes in the included studies.
Results
A total of 685 studies were initially identified (Please see the PRISMA flow chart in Figure 1). After duplicate removal (n = 270), and screening of 415 studies, 60 studies were included in full-text review. Forty-five studies were ultimately included.20 -64 The median publication year was 2020 (IQR 6.5, range 1999-2023). The distribution of publication dates are displayed in Figure 2.

Summary flowchart of the outcomes of the identification and screening process. Flow chart format has been adapted from the PRISMA 2020 flow diagram for new systematic reviews. 65
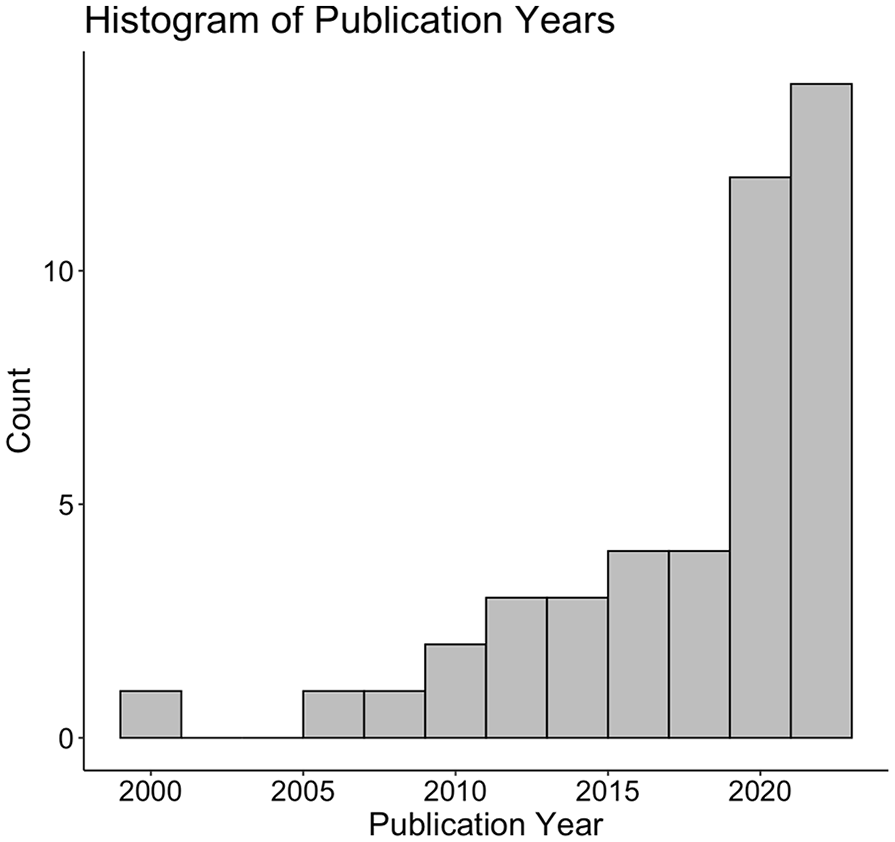
Histogram of the year of publication distribution (binwidth = 2 years). The median year of publication was 2020 (IQR 6.5, range 1999–2023).
Study Characteristics
Study characteristics are summarized in Supplemental Table 2. Studies were from the United States of America (n = 40), Canada (n = 2), United Kingdom (n = 2), and Turkey (n = 1). Most studies discussed mentorship in otolaryngology in general (n = 38). Studies also discussed mentorship in the context of facial plastics (n = 3), rhinology (n = 1), and multiple subspecialties (n = 3). Study designs included opinion (n = 13), cross sectional (n = 11), cohort (n = 6), narrative review (n = 5), case series (n = 4), a systematic review (n = 2), qualitative research (n = 2), case control (n = 1), and bibliometric analysis (n = 1).
Mentees and Mentors
Majority of studies discussed mentoring of medical students (n = 25), residents (n = 19), or faculty (n = 15) mentees. Mentors in the studies were faculty (n = 43), residents (n = 5), retired staff (n = 1), medical students (n = 1), and private practice otolaryngologists (n = 1). Twenty-two studies discussed mentorship in a general group of mentees. Seventeen and 14 studies included mentorship of under-represented minorities (URM) and women, respectively.
Themes
The major themes of benefits from mentorship included improving residency uptake (n = 22), clinical competency and professionalism (n = 20), diversity and equity (n = 19), research productivity (n = 17), career planning and advancement (n = 17), and quality of life (n = 11) as seen in Figure 3. Other identified themes included utilizing active or formalized mentorship (n = 29), near-peer mentorship (n = 13), utilizing digital tools to increase access to mentorship (n = 6), and reverse mentoring (n = 3).

Themes (n = number of studies) broken down by mentee level of training. Number on pie slice indicates the number of studies where mentees of the given level of training are afforded the respective benefit. A study may describe a certain benefit for a variety of mentee levels of training.
Level of Evidence
Majority of studies were level 5 (n = 18). Otherwise, the studies’ levels of evidence were as follows: Level 1 (n = 2), level 2 (n = 0), level 3 (n = 17), and level 4 (n = 5). Three studies were not classifiable per the 2011 OCEBM evidence hierarchy.
Discussion
To the authors’ knowledge, this is the first scoping review assessing the landscape of mentorship in OHNS. Our findings highlight a surge of literature on mentorship in OHNS with more than half of the studies (58%) published between the start of 2020 and September 2023. The majority of the studies were US-based, opinion or survey studies, in the field of general OHNS, and were moderate to low level of evidence. Studies with medical student mentees were most common. More than half of the studies discussed formal models of mentorship.
Residency Uptake
Increased mentorship in OHNS can improve residency uptake, which involves attracting more applicants, aiding in successfully preparing medical students for the match process, and improving their chances of matching.20 -41 Sixteen studies discussed utilizing mentorship to influence medical student career choices.20 -27,29,31,32,34,35,37,38,40 Mentor relationships and early exposure were 2 modifiable factors that influence medical students to pursue OHNS. 35 For example, Shah et al 38 demonstrated that a hands-on laryngoscope workshop hosted by otolaryngology residents and faculty increased medical student interest in OHNS, with 54.5% (6/11) participants ranking as being “very interested” in pursuing OHNS afterward.
Six studies showed that mentorship can significantly improve medical students’ chances of matching into OHNS.27,28,33,36,37,39 In a study by Sethia et al, 37 pre-clerkship students were paired with otolaryngology faculty mentors and attended clinical and education activities. Following the program, 6/6 students involved in the program matriculated to OHNS. Similarly, Ramirez et al 36 demonstrated a successful residency match of students without a home OHNS program who received formal mentorship in clinical skills and research from local private practice otolaryngologists. Furthermore, mentor support throughout the match process itself can significantly enhance a medical student’s likelihood of securing a match. In a study by Solis et al, 39 electronic surveys were distributed to otolaryngology residency program directors (PDs), finding that 81.8% of PDs believed that communication initiated by a student’s mentor influenced whether they received an interview offer and 33.3% of PDs believed mentor initiated communication affected rank lists. Therefore, mentorship enhances interest and equips students with the skills and confidence needed for success in the OHNS residency match.
Enhancing Diversity Initiatives
Nineteen studies highlighted mentorship in the context of increasing diversity in OHNS.21 -31,40,41,44,46,47,53,58,63 Thompson-Harvey et al 40 found that interactions and personality fit with OHNS faculty greatly influenced 388 URM medical students’ decisions to pursue OHNS and having race-concordant role models were significant for continuing pursuit of OHNS. Faucett et al 24 surveyed 46 African American OHNS physicians and found that while early exposure and enjoyment of clerkship were the primary reasons for pursuing OHNS, 37% (17/46) still cited mentorship as significant. A lack of URM mentors may be a barrier for URM students. In a survey by Johnson et al 26 of 104 minority medical students, predominantly female and black, 69% (72/104) and 48% (50/104) of students rated same-race and gender mentors as very important, respectively. One-third (34.6%) reported discouragement due to a lack of same-race mentors.
While many studies have examined factors influencing URM and women to pursue OHNS, only 2 studies looked at using mentorship to improve match rates in these populations.27,28 Nellis et al 27 launched a mentorship program in 2008 that provided URM students with research clerkships or clinical rotations, financial support, and faculty mentorship, ultimately resulting in 6 of 7 applicants successfully matching in OHNS. In a survey study, Newsome et al 28 found a correlation between URM faculty numbers and resident matriculation.
From a program’s perspective, certain factors may influence URM and women in ranking them. Goosmann et al 25 surveyed 62 female residents who stated that having at least 1 female attending (88%, n = 54) and at least 1 female resident (87%, n = 54) were (very) important when creating their rank list.
While the proportion of women and URM OHNS residents has been increasing, the disparities of rank within academic positions have changed minimally.9,10,66 -68 Seven studies discussed utilizing mentorship in a faculty population to improve these inequities.23,46,47,53,58,30,41 One factor thought to contribute to inequity is the “minority tax,” where women and URM carry the majority of the responsibility for Diversity, Equity, and Inclusion efforts, leading to an opportunity cost for other scholarly activities associated with promotion.69,70 Insufficient mentorship, arising from scarcity of URM and women mentors, is thought to contribute to the minority tax. 47 Active mentorship models may help mitigate the scarcity of mentorship.23,30,41,46,47 Lin et al 41 implemented a mentorship program at Johns Hopkins’ Department of OHNS for increasing and retaining women and URM faculty by facilitating connections with experienced mentors, ultimately leading to a 4.1-factor increase in women clinical faculty and a doubling of URM faculty within a 10-year period. It is important to note that the scarcity of mentorship for URM and women faculty may be even more pronounced in OHNS subspecialties. In a survey by Lafer et al 53 surveyed women in the American Academy of Facial Plastic and Reconstructive Surgery, more women in practice felt that they lacked mentorship (38%) compared with men, and 4 of 16 women in training felt they also lacked mentorship versus 0 of 5 men. In cases where there is limited access to mentors, digital technologies may serve as a solution. 21 However, mentorship by itself may not be sufficient. In multi-institutional online interviews by Farlow et al, 46 found that multiple participants reported experiencing paradoxical over-mentorship with under-sponsorship, leading to no change. The mentorship program by Lin et al 41 described above paired mentorship with other strategies such as creating a climate of diversity, increased recruitment, and achieving equal pay by rank.
Once diversity is improved at the faculty level, it is crucial to implement sustainable models to maintain it. One strategy is to ensure continued mentoring of URM trainees, as URM faculty who were mentored as trainees were shown to be more likely to become mentors themselves. 24
Clinical Competency and Professionalism
North American surgical training relies on mentorship to enhance clinical competencies. 42 Ten studies discussed improving clinical competencies through mentorship in the context of medical students.21,22,30,33,34,36 -38,42,43 Some OHNS mentorship programs have been shown to increase medical student’s knowledge of disease and anatomy.33,38 While it is important for all medical students to be familiar with OHNS concepts, mentoring students in a clinical context can improve their clinical skills overall. Sethia et al. 37 found that pre-clerk students paired with otolaryngology faculty mentors, and attending clinical and educational activities, nearly doubled the confidence of their classmates in various clinical skills. Four students who ultimately applied to other specialties successfully matched.
The benefit of strong mentorship for improving resident clinical competencies is well documented and was explored by 11 studies in the OHNS literature.21,30,34,42,48 -51,55,56,59 Despite this, studies where OHNS residents were surveyed found that only 58% (28/48) of residents felt they were mentored for clinical judgment skills 55 and only 63% (246/391) felt that their mentors assisted with their overall resident education. 49 In contrast, a study by Geltzeiler et al, 48 found that residents perceived that mentors most extensively helped with their surgical skills (mean 4.7 on a 5-point Likert scale) and clinical decision-making (4.6). It is important that residency programs make efforts to have mentorship available in all domains of practice. In a study by Hsu et al, 51 residents ranked the availability of mentorship in preparation for a career in private practice versus academic medicine significantly lower. A key component of clinical competency are the soft skills of practice. There is significant discussion of utilizing mentorship in OHNS for facilitating the acquisition of the values, attitudes, and behavior associated with professionalism, humanism, and ethical practice.34,43,50 It is important to note that a student’s capacity for compassion can be positively or negatively influenced by role models.34,43 Nichols et al 59 found that role modeling was the most common method for teaching professionalism, with residents ranking formal faculty mentors as the most effective.
Once out of training, mentorship can be utilized for continued improvement as a surgeon. Four of 5 studies on this topic in the OHNS literature were opinion pieces.56,57,60,30 Two studies had themes of utilizing digital technologies for the mentorship of faculty mentees across geography.56,61 In a study by Snyderman et al, real-time audio and video communication was utilized to telementor Slovenian surgeons for 10 endoscopic endonasal cases over 3 years, demonstrating improved exposure (n = 7), reduced surgery time (n = 5), increased tumor resection (n = 5), and prevention of complications (n = 2). Miller and Choi 57 highlighted the importance of having diverse mentors at different seniorities for continuous learning. Moreover, mentors may also learn from mentoring, solving their own problems through teaching others. 60 Mentorship fosters continuous skill development, promoting long-term professional growth in OHNS.
Research Productivity
Mentoring students in research is critical for the advancement of the field of OHNS. OHNS trainees express strong interest in receiving mentorship in research. 42 Residents reported adequate access to research mentoring with mean 5-point Likert scores for mentors’ support in research as 3.1 to 3.648,49,51 and in a study by Lin et al, 55 it was ranked the 2nd most frequently provided specific domain of mentoring. 55 For medical students, access to mentors appears to be a key barrier to conducting research. Nellis et al 27 found medical students in research and clinical “clerkships” published at similar rates and Ramirez et al 36 found students with private practice mentors exceeded average publication rates. Digital technologies, such as centralized online platforms highlighted by Shah et al, 38 have allowed for increased research mentorship and can further enhance cost-effective mentoring opportunities. 56 In addition, junior trainees seek research mentorship for various reasons, including using research to increase access to mentors and enhancing curriculum vitae for residency.42,63 It is important to note that mentoring students for research can also benefit the research productivity of mentors as well. A bibliometric study by Svider et al 62 of The Laryngoscope and IFAR showed that principal investigators collaborating with students achieved higher H-indexes than those working only with physicians and doctoral-level scientists. Such evidence supports mentoring in programs such as the American Rhinologic Society Mentorship Program, which pairs younger rhinologists who have a basic science research interest with senior clinician-scientists who have successfully obtained funding. 52 Another theme in the OHNS research mentorship literature is that mentoring diverse researchers can help promote research in under-represented patient populations.30,47 Effective mentorship in research is critical to creating future OHNS leaders in research.
Career Planning and Advancement
Residents face stress from competitive job markets and training demands, making career planning mentorship crucial.71,72 Six studies examined this for residents.42,45,48,49,51,55,56 Career planning is among the top mentorship expectations from resident mentees. 42 In studies surveying residents, they reported mean 5-point Likert scores of 3.2 to 4.0, among the highest domains of mentorship they received.48,49,51 Lin et al 55 surveyed 70 residents and fellow mentees, and career mentorship was the most frequently provided (affirmed by 81% of mentees). A key finding elucidated by Abrar et al 42 in senior residents was the need for impartial guidance outside of training regions, which is unaffected by departmental politics. The proposed adoption of digital tools and virtual learning platforms can be a key technique for providing this form of mentorship. 56 Moreover, it is important to consider that the need for mentorship in career planning varies by the healthcare system and is in particular needed where larger job scarcity exists, such as the Canadian system. 73 Cote & Hamour 45 found that employability is a major stressor for Canadian residents and emphasized the need for formal career mentorship programs and increased exposure to community practice.
Like residents, faculty can also benefit from mentoring to improve their careers. Themes of mentorship for career advancement were seen in 10 studies.23,46,47,52,53,41,57,58,60,30 Seven of the 10 studies were related to diversity and equity, covered under that section.23,46,47,53,41,58,30 Three additional opinion pieces highlight the idea that a diverse network of multiple mentors is greatly beneficial for career advancement and that while mentors can open doors for mentees, the mentee must still prove themselves to reap the benefits.52,57,60 Mentorship in career planning plays a critical role in supporting the career progression of residents and faculty alike.
Improving Quality of Life
OHNS residents have been shown to experience high levels of burnout, stress, and job dissatisfaction due to high demands in daily work.54,74 Despite discussion of utilizing mentorship to improve well-being,52,60 OHNS residents reported low access to mentoring around quality of life with mean 5-point Likert scores from 2.5 to 3.2.48,49,51 Moreover, a study by Lin et al, 55 only 42% and 43% of mentees and mentors selected mentorship in well-being was available, making it the least-mentored area of 6 areas of mentorship. 55 Zhang et al 64 at the University of Alberta found that a formal mentorship program improved residents’ quality of life, reducing emotional stress and depersonalization while increasing personal achievement and overall well-being across multiple domains. Similarly, mentorship programs have been shown to significantly enhance faculty retention in academic medicine,23,41 likely due to increased quality of life. 75 Expanding mentorship in otolaryngology may reduce burnout and improve job satisfaction for residents and faculty.
Limitations
This study may have missed articles published after our search in September 2023. Most studies are of low evidence due to the emerging nature of this field. This review was limited in its scope of other aspects of mentorship such as qualities of good mentors or mentorship programs. This could be an opportunity for future research. Only English language studies were included due to the language skills of the authors. While we focused on outcomes related to mentorship from studies, articles primarily addressing sponsorship or surgical coaching were not explicitly excluded and therefore may have influenced the conclusions related to mentorship.
Conclusions
Mentorship is an emerging area of interest in OHNS, as evidenced by the explosion of recent articles in this area. There are numerous benefits to mentorship discussed in the literature including improving residency uptake, diversity initiatives, clinical competency, research productivity, career planning and advancement, as well as quality of life as summarized in this article in a qualitative manner. Future efforts should focus on integrating structured mentorship programs to promote equitable access to mentorship with targeted strategies to foster early exposure and interest in the field. Leveraging digital technologies and near-peer mentoring should be utilized to expand mentorship opportunities. Institutions must also implement sustainable models that utilize mentorship to maintain diversity at the faculty level, ensuring continued support and growth. Further research on supporting resident and other mentee groups’ well-being through mentorship should be considered.
Supplemental Material
sj-docx-1-ohn-10.1177_19160216241307548 – Supplemental material for Mentorship in Otolaryngology Head and Neck Surgery: A Scoping Review
Supplemental material, sj-docx-1-ohn-10.1177_19160216241307548 for Mentorship in Otolaryngology Head and Neck Surgery: A Scoping Review by Norbert Banyi, Dianne Valenzuela, M. Elise Graham and Amanda C. Hu in Journal of Otolaryngology - Head & Neck Surgery
Footnotes
Authors’ Note
This work was presented at the Canadian Society for Otolaryngology Head and Neck Surgery Meeting, Montreal, June 2, 2024.
Authors Contributions
Norbert Banyi: preparation of research protocol, abstract and full-text screening for study selection, data collection, and analysis, preparation of the article, and revisions of the final article. Dianne Valenzuela: project inception, conducting search strategy, abstract and full-text screening for study selection, data collection, and analysis, article editing critical for intellectual content. M. Elise Grant: article editing critical for intellectual content. Amanda C. Hu: project inception, creation of research protocol, resolution of differences in abstract and full-text paper selection, article editing critical for intellectual content.
Consent to Participate
Not applicable.
Consent to Publication
Not applicable.
Data Availability Statement
Data is available on reasonable request.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethical Approval and Informed Consent
Not applicable.
Ethical Considerations
Research Ethics Board approval was not required for this work.
Supplemental Material
Additional supporting information is available in the online version of the article.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
