Abstract
Patients’ use of generative AI (GenAI) independently from healthcare is increasing across diseases. Little is known about its use among people with Parkinson's disease (PwP). This exploratory convenience-sample, mixed-methods online survey (n = 149, 19 countries) explored PwP's use of GenAI. Among our respondents, 65% had used GenAI, of which 40% had used it for disease-specific inquiries. Qualitative analysis identified informational, interpretive, and preparational uses of GenAI. As PwP increasingly bring AI-assisted data to consultations, clinicians must now actively engage in discussions about these tools, to support shared decision-making, safety and transparency.
Introduction
The rapid advancement of large language model-powered generative artificial intelligence (GenAI) has begun to transform care. Driven largely by GenAI such as ChatGPT, DeepSeek, and Gemini, research indicates these tools are already reshaping how clinicians manage clinical, administrative, and research tasks. 1 Preliminary studies show patients are also using GenAI for health-related inquiries and self-management.2–6
While research on GenAI tools has largely focused on clinician adoption and operational efficiency, patient perspectives remain under-examined.7,8 Notwithstanding, research suggests that GenAI is likely to be one of the most adopted technologies for self-management across various chronic conditions. 9
Parkinson's disease (PD) presents unique challenges for symptom management, including fluctuating motor and cognitive symptoms, which may specifically influence how patients engage with and benefit from these tools. 10 For example, a recent evaluation of ChatGPT-4o generated PD exercise advice that raised concerns, as the information was rated at a reading level too complex for general health literacy and with low clinical reliability. 11
Despite the development of PD-specific GenAI,12,13 there is currently no research documenting how people with PD (PwP) use GenAI, or the factors that lead them to avoid it. Exploring PwP's experiences and opinions of genAI is crucial to obtain a deeper understanding of how perceptions of benefits and risks, as well as ethical considerations related to trust and privacy, influence their adoption and use of genAI. Therefore, this study aims to identify PwP's experience and opinions about GenAI for self-management of PD.
Methods
Data collection and approach
This study was part of a larger convenience sample survey designed to explore user needs across diverse AI applications for PD-management, including both predictive AI and GenAI tools. The full instrument consisted of 24 items; 14 however, this paper focuses on 14 items specifically addressing GenAI tools. The convergent mixed-methods online survey was disseminated April-November 2025. The project was submitted for ethical review and deemed exempt by The Swedish Ethical Review Authority Dnr 2024-05505-01.
The survey was disseminated through Swedish and international patient networks and social media (Facebook and LinkedIn), including channels managed by one of the authors (SR). Via these channels, we expected to reach primarily PwP who are active and engaged in PD care and research. Participants were informed that the survey was voluntary with no compensation and they could withdraw at any time. The survey was composed of mandatory Likert-scale items, single- and multiple-choice questions, alongside mandatory and optional free-text questions. Available in four languages, the survey was designed in English by a native speaker, then translated into French, Spanish, and Swedish using the EUSurvey platform's AI translation, and each verified by a native speaker. Inclusion criteria were a self-reported PD diagnosis and fluency in one of the four survey languages.
Data analysis
Quantitative data were analyzed descriptively in JASP (v0.19.1.0). Free-text responses were analyzed using inductive qualitative content analysis to identify recurring patterns grounded in participants’ responses. This approach is well-suited to brief, free-text data that includes short and fragmented sentences. 15 Due to the brevity of the responses (1–4 sentences), individual comments were treated as single meaning units. 16 Initial categorization was conducted by one author (JLL), appropriate for short, low-complexity datasets, 17 with categories iteratively refined through collaboration with the co-authors. Responses to the question “How have you used these GenAI tools in relation to your Parkinson's disease?” were analyzed as one unit. Responses to the two questions addressing non-use — “Why have you not used GenAI for any purpose?” and “Why have you not used GenAI in relation to your Parkinson's disease?” — were analyzed together, as they reflected the shared underlying issue of non-use. Analysis began once 100 responses were received to establish preliminary category development, which was updated as subsequent data were collected.
Results
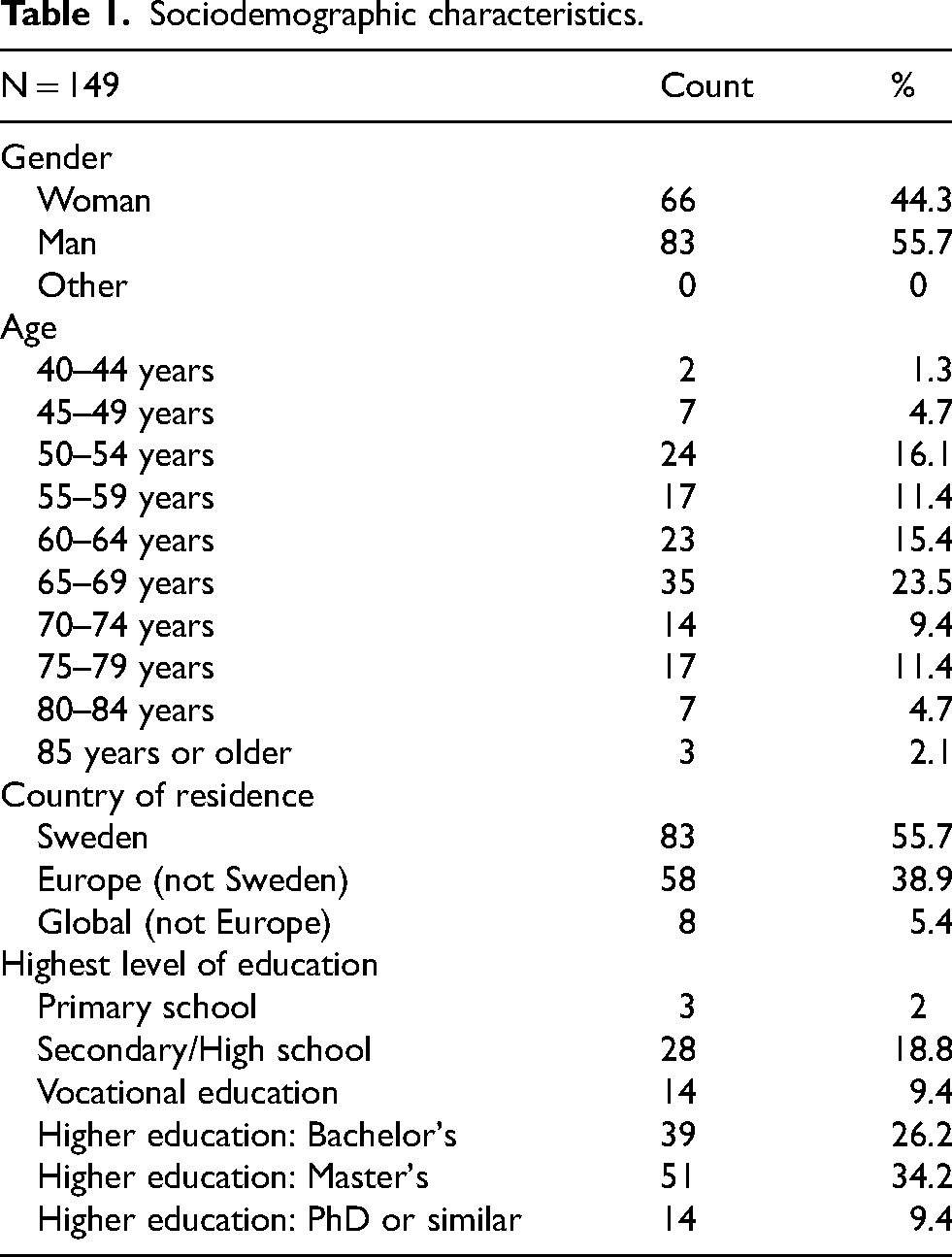
Respondents were 149 PwP across 19 countries, primarily from the EU (88%), including Sweden (56%), see Table 1. Respondents were aged 43–90 years (m = 64.7) and 56% were male (n = 83). Diagnosis duration ranged from 0 to 27 years (m = 7.04). Most reported attaining higher education (70%). When asked how comfortable they are in using digital technology such as a smartphone, computer, or smartwatch, from “1-Not at all” to “4-Very comfortable,” most said “4-Very comfortable” (60%), and nearly a third reported “3-Decently” (32%). 4 in 10 (n = 61) reported that they currently self-track one or more of their PD symptoms, and nearly 3 in 10 expressed intention to start (n = 42).
Sociodemographic characteristics.
Use of GenAI
The majority of respondents reported previously using GenAI (65%, n = 97), however, under half (40%, n = 39) of those had used it in relation to their PD. Respondents used a variety of GenAI in relation to their PD (see Figure 1). About half (51%, n = 39) of users reported “neutral” levels of trust towards the outputs, followed by 46% who indicated “very high,” and the remaining 3% reported “very little” trust.

Types of GenAI used and overview of categories by question. Note: Each respondent was asked to check or list all GenAI assistants used. The number of assistants will total above the number of respondents.
Reasons for using GenAI for PD
Respondents described GenAI as
GenAI was also used to
The third reported use was in
Reasons for not using GenAI
Respondents who reported not using GenAI, whether for their PD or for general purposes, offered a variety of reasons. Several perceived that they
Discussion
Patient surveys on GenAI use are scarce, and this is the first study to examine PwP's specific uses and perceptions of these tools for self-management. Although a majority of respondents in our study had used GenAI, only a smaller subset reported integrating GenAI use into their PD management. The qualitative data augmented these quantitative findings, clarifying use and non-use. Reported usage was categorized into informational, interpretive, and preparational tasks.
A key finding illustrated by our study was the privacy paradox—inconsistencies between an individual's expressed privacy concerns and their actual behavior. 18 One respondent reported a daily relationship with ChatGPT while recognizing it may not be GDPR compliant. This might suggest that performance expectancy—the belief that the tool helps achieve a specific health goal—is a stronger driver of adoption than privacy concerns. This is consistent with research indicating that goal-directed utility often outweighs perceived risks in digital health adoption. 19 However, in our study, we found that adoption remained polarized. This identified divergence also aligns with previous findings that highly educated PwP are often more critical of AI-driven decision-making and data security. 20
The rise of preparational GenAI health use, where increasingly more PwP can be expected to adopt GenAI assistants to summarize clinical information, has direct implications for patient-clinician relationships. Clinicians need to recognize this shift and engage in shared decision-making, helping patients verify AI-generated information to ensure clinical safety. 21 Given that many respondents reported limited knowledge of how to leverage GenAI, research should focus on developing and evaluating educational frameworks that demonstrate concrete, high-value use-cases for GenAI in PD-management.
Another important consideration for all parties—PwP, clinicians, and caregivers—is the inherent risks GenAI poses. Hallucinations, where AI generates inaccurate or misleading information, could lead to harmful decisions if replied on unsupervised.
GenAI also tends to produce responses biased toward pleasing the user, potentially oversimplifying complex medical issues or reinforcing pre-existing beliefs through confirmation bias. 22 This has been found in mental health to amplify placebo or nocebo effects by influencing patient expectations.23,24 These risks highlight the need for clear guidelines, education on AI limitations, and clinician feedback to ensure safe and ethical use of GenAI in neurology contexts. 25
A primary strength of this study is the international sample, with perspectives across multiple geographic contexts and health systems. The study has several limitations. Diagnoses were self-reported rather than clinician-verified, and the absence of disease-related variables (e.g., age of onset, disease duration, treatment type) prevent characterizing disease severity within the cohort. Also, reliance on a convenience sample embedded biases of a predominantly highly educated, and digitally literate respondents who appeared more comfortable engaging with online platforms. Consequently, the findings are not generalizable to the broader PD population, particularly individuals with more advanced disease, cognitive or motor impairments, lower digital literacy, or limited internet access. Future research should prioritize recruitment strategies that enable inclusion of more diverse and clinically representative populations.
Conclusion
PwP are already leveraging GenAI to bridge the gap between complex medical information and daily self-management. As use of these tools is likely to increase, future research should focus on developing guidance frameworks to help patients and clinicians safely navigate AI-assisted care.
Footnotes
Acknowledgements
We thank Carolina Garcia Sanchez and Philippe Boccon-Gibod for validating the survey translations.
The authors acknowledge the contributions of the “Artificial Intelligence-Based Parkinson's Disease Risk Assessment and Prognosis” (AI-PROGNOSIS) project and the funding support from the European Union (grant agreement 101080581).
ORCID iDs
Author contributions
JLL led the survey design, data collection with input from CB and AK. JLL led the drafting of the manuscript and data analysis for this article with support from CB. All authors collected data and contributed to writing and commenting on the manuscript.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by the European Union under the Artificial Intelligence-Based Parkinson's Disease Risk Assessment and Prognosis (AI-PROGNOSIS) project (Grant Agreement No. 101080581). The funder had no role in the design of the study; collection, analysis, or interpretation of data; preparation of the manuscript; or decision to submit the manuscript for publication.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
