Abstract
Parkinson's disease (PD) is a progressive neurodegenerative disease with multiple manifestations including both motor and non-motor symptoms. One manifestation of PD that is often overlooked is the sexual dysfunction (SD) that patients may experience. Individuals with PD can experience impairment in sexual desire, arousal or lubrication, orgasm, ejaculation, pain and the physical aspect of intimacy. This article aims to provide an overview of the current practices in the evaluation and treatment of sexual dysfunction in men in the context PD. Note that this article focuses on the male population as it reviews the available American Urology Association practice guidelines many practitioners follow, which focus on the male population. Sexual dysfunction guidelines for the female population are much more limited, and future work should review the existing literature and gaps to provide a more robust understanding of sexual dysfunction in PD. PD represents a particularly vulnerable population for development of sexual dysfunction given the multifactorial nature of its manifestations. Given its profound impact on not only the patient, but their partner, it is important to be aware of the various manifestations of SD when evaluating individuals with PD. Through thorough history taking and targeted psychosexual evaluation, we as practitioners can ensure a more holistic and comprehensive approach to caring for individuals with PD.
Plain Language Summary
Patients with Parkinson's disease (PD) can experience a myriad of symptoms, ranging from movement symptoms such as tremors to non-movement symptoms such as depression. An often-overlooked symptom associated with PD is sexual dysfunction, which refers to impairment in any component involved in normal sexual function. Individuals with PD can experience changes in sexual desire, arousal or lubrication, orgasm, ejaculation, pain, and the physical aspect of intimacy. It is important that clinicians taking care of individuals with PD are aware of these symptoms as these can have profound impact on the quality of life for the patient as well as their partners. Most initial interventions for sexual dysfunction include non-invasive treatments such as behavioral modification and oral pharmacotherapies. For more advanced treatments, dedicated sexual health clinicians may provide additional expertise. Our manuscript provides a broad and generalized overview of sexual dysfunction for clinicians who evaluate and treat individuals with PD. Note that the article describes practices and treatments directed mostly towards the cis-male population, although the general principles described are applicable regardless of a patient's gender or sexual preferences.
Introduction
Parkinson's disease (PD) is a progressive neurodegenerative disease defined by the hallmark alpha-synuclein deposits (Lewy bodies) within dopaminergic neurons located in the substantia nigra of the midbrain. 1
Dopaminergic neurons within the substantia nigra are crucial for movement and motor coordination. Non-motor symptoms (NMS) including autonomic dysfunction (bowel and bladder dysfunction, hypotension) as well as sensory, behavioral, and sleep-related abnormalities are also common in individuals with PD.2,3 The general neuro-anatomic basis for non-motor symptoms is not as clearly defined in comparison to the motor manifestations. 4
Sexual dysfunction (SD) refers to impairments in one of several domains of normal sexual function: desire, arousal or lubrication, orgasm or ejaculation, and pain. 5 Patients with orthopedic or neurologic concerns may also experience difficulty with certain sexual positions that negatively impacts sexual satisfaction. 6 A series of focused interviews with individuals with PD revealed that the movement difficulties and body inflexibility leads to discomfort with intercourse and significant limitations for possible positions for intercourse. Because of this, individuals with PD and their partners expressed sexual dissatisfaction solely due to these factors. 7 It is estimated that 30–40% of adult men and women experience SD, although the true prevalence rates are hard to ascertain due to reporting biases.8–10
Normal sexual function involves the complex interplay of psychologic, neurologic, vascular, hormonal and local anatomic factors. Neurologic conditions can negatively impact sexual function.11,12 SD is common in individuals with PD. 13 A recent systematic review and meta-analysis of 13 pertinent studies found a significantly greater incidence of SD in individuals with PD compared to healthy controls (odds ratio 3.5, 95% CI – 2.19–5.58). 14 Another review found that male patients have a higher likelihood of experiencing sexual dysfunction compared to healthy controls, whereas there was no significant difference in the prevalence of SD in females. 15 This finding is thought to be the result of reporting bias rather than a true gender difference in the prevalence of sexual dysfunction. 16 Younger individuals with PD experience greater distress from PD-associated SD, likely due to their better baseline sexual function prior to symptom onset.17,18 As with the general population, the true rates of SD in PD are likely significantly higher than what is reported in the literature. 13
Reporting SD is often challenging for patients and clinicians alike who may feel uncomfortable and self-conscious about discussing these sensitive topics or have significant time constraints.19–21 Several intrapersonal, interpersonal, cultural, and institutional barriers have been identified, which limit sexual health conversations in a formal healthcare setting.
22
However, this has important implications not only for quality of life, but also for general health. For example, erectile dysfunction has been linked to adverse cardiovascular outcomes, particularly in younger men.
23
It may also be the initial presenting symptom for some neurologic conditions.
24
Herein, we seek to provide a clinical roadmap for diagnosing and treating sexual dysfunction in male individuals with PD. In the following sections, we will describe male sexual function and dysfunction as it pertains to PD. Moreover, we will provide clinical recommendations for the appropriate initial evaluation and treatment of sexual dysfunction in men with PD. For clarity, henceforth when discussing male sexual dysfunction, we are specifically referencing
Our manuscript is not intended to serve as a comprehensive analysis of data from the currently published literature. Rather, we hope this overview of sexual dysfunction will serve as a helpful tool for clinicians who routinely evaluate and treat patients with PD as they seek to provide comprehensive care for their patients. As we will describe, the current state of literature investigating sexual dysfunction in PD is limited, and our hope is that this review brings light to this important topic to inspire future work in this field.
Sexual function: anatomy and physiology
Normal sexual function involves a complex interplay between the central and peripheral nervous systems, cardiovascular system, and end-organ functions. 25 Visual, auditory, and tactile stimulation from the peripheral nervous system contribute to sexual arousal, but ultimately sexual behavior originates through higher level processing in areas of the brain including the cerebral cortex (prefrontal cortex, septal region, cingulate cortex, insular cortex), amygdala, hypothalamus, thalamus, and central reward system.25,26 Multiple neurotransmitters such as serotonin, norepinephrine, and dopamine are involved in normal sexual function. 26 Centrally, serotonin inhibits sexual arousal and downstream effects, whereas dopamine promotes arousal and desire. 27 Dopamine is of particular importance because of the role it plays in the central reward system. 28 Dopaminergic neuron loss seen with PD can therefore contribute to hyposexuality. Various peripheral circulating hormones are implicated in sexual dysfunction including testosterone and its derivates dihydrotestosterone and estradiol. Patients with diminished libido or sexual desire often have abnormalities in sex hormones such as hypogonadism, although other medical and psychiatric conditions may also be at play (e.g., hypothyroidism, depression, etc.).29–31
Autonomic and somatic peripheral nervous systems are both involved in sexual dysfunction. Somatic nerves originate from the sacral nerve roots as the pudendal nerve, which travels through Alcock's canal along the perineum and ultimately to the pelvic floor and genital musculature where it provides motor innervation. 25 Perineal, scrotal, and penile sensation is transmitted via afferent signaling pathways within the pudendal nerve as well (Figure 1).
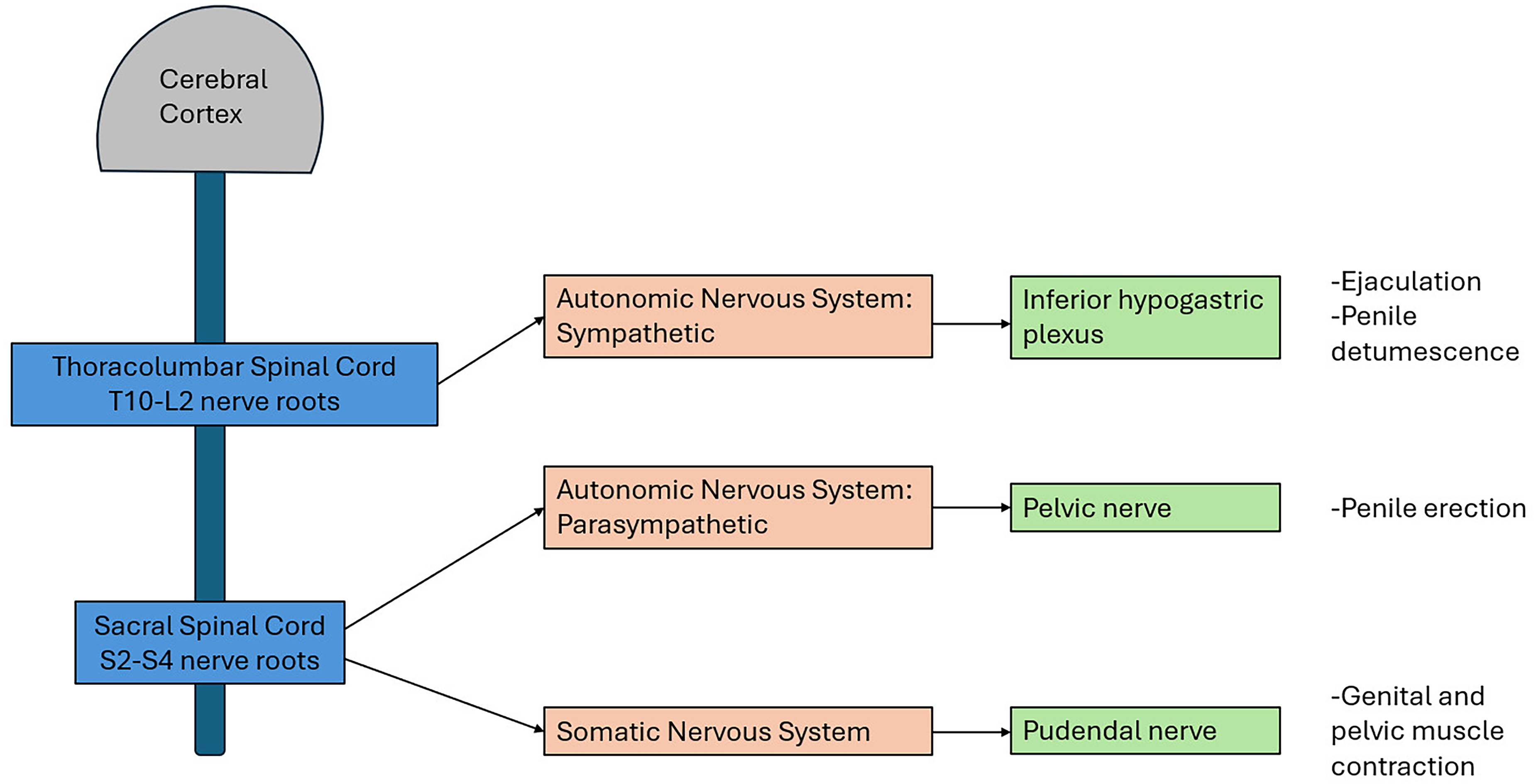
High level overview of autonomic and somatic neural pathways involved in sexual function.
Autonomic nerves originating from the pelvic (parasympathetic arising from sacral nerve roots) and hypogastric (sympathetic arising from thoracolumbar nerve roots) nerves ultimately coalesce in the pelvic plexus lying adjacent to the rectum and bladder.32,33 Distal nerve branches run with the fascial layers adjacent to the prostate gland and through the pelvic floor to the erectile bodies of the penis, also known as corpora cavernosa. 33 These nerves can be inadvertently injured during pelvic surgery such as after radical prostatectomy or low anterior resection for rectal cancer or from pelvic trauma such as a can occur during a high speed motor vehicle accident.34,35 Non-adrenergic, non-cholinergic (NANC) parasympathetic nerve fibers release nitric oxide which stimulates endothelial smooth muscle relaxation within the penile vasculature. 36 The result is greater blood flow into the penile cavernosal (erectile) bodies and subsequent penile engorgement. The cavernosal bodies are surrounded by a fibrous jacket tissue called the tunica albuginea. As the penis fills with blood, small veins at the interface between the erectile tissue and the tunica are passively compressed to allow blood to be trapped within the penis and the erection rigidity to be maintained. 37 In contrast, acetylcholine release from sympathetic nerve fibers contributes to smooth muscle contraction and loss of erection, which is one potential cause for “psychogenic” erectile dysfunction (ED) such as can be seen with anxiety. 38
Ejaculation and seminal emission are a physiologically distinct process from penile erection. Most semen volume is derived from the prostate gland and seminal vesicles, whereas sperm itself is produced within the testicles. Sperm are transported from the testicles and into the pelvis through the vas deferens where they ultimately meet with the prostate and seminal vesicles at the level of the ejaculatory duct. Seminal emission (i.e., the deposition of semen within the urethra) is regulated by the sympathetic nervous system (hypogastric nerve) and ejaculation (expulsion of semen through the urethra) occurs due to somatic input from the pudendal nerve and resulting pelvic and genital muscular contractions. 25 Orgasm or “climax” is defined as the temporary peak of pleasurable sensation most often associated with ejaculation or seminal emission, but again this is a physiologically distinct phenomenon. 25 For example, patients who undergo radical prostatectomy for prostate cancer will no longer experience ejaculation, and many may suffer from temporary or permanent erectile dysfunction due to damage to the periprostatic parasympathetic nerve branches. 34 Despite this, many of these patients are able to experience climax through adequate sexual stimulation. Orgasm is a complex phenomenon involving central and peripheral processes. Functional imaging studies have identified changes in regional cerebral blood flow and activation of various locations with the cerebral cortex and cerebellum during orgasm.39,40 Pelvic and genital muscular contractions also occur and contribute to orgasm intensity in some men.41,42
Sexual dysfunction
Sexual dysfunction in PD can manifest in multiple ways and is multifactorial in nature. It can cause both symptoms related to hyposexuality and hypersexuality. 13 Manifestations of hyposexuality include erectile dysfunction, ejaculatory dysfunction, loss of libido, hypogonadism. It is also important to discuss how motor symptoms of this disease can affect sexual function, and to consider the psychological impact of living with PD can affect sexual function.
Erectile dysfunction
ED is defined by the American Urological Association as the inability to attain and/or maintain penile erection sufficient for satisfactory sexual performance. 43 All patients require an initial thorough medical, sexual, and psychosocial history to determine the diagnosis. Using history-based questions, validated questionnaires have been developed (e.g., Erection Hardness Score, International Index of Erectile Function, and Sexual Health Inventory for Men), that quantify ED severity and also uncover the consequences of ED to the patient's life (relationship, satisfaction, etc.)44,45 The American Urological Association recommends the use of these questionnaires to assess the severity of ED and to also measure treatment effectiveness. 43
While the exact prevalence of erectile dysfunction is unknown, it is reported to be as high as 52% across a cohort of the general population between ages 40 and 70, and is estimated to affect anywhere from 18 to 30 million men in the United States.46,47 The prevalence of ED increases with increasing age, with an estimated 60% of all men over the age of 70 being affected. 48 Of note, studies to date lack good representation of all races, however one larger study has reported that black men are less likely to have severe ED when compared to white men. 49 The research community also understands the need for study designs and more applicable questionnaires to better capture the rates of ED in the non-heterosexual and gender diverse populations. There are several other risk factors for ED in addition to advanced age including: vascular disease, smoking, obesity, hypertension, diabetes, spinal cord injuries, renal insufficiency, medications, prostate cancer treatment and neurodegenerative conditions. 43
The pathophysiology of ED depends upon the primary cause of the disorder. The underlying etiology is not always readily identifiable and is often multi-factorial. For example, individuals with PD who had other medical comorbidities such as diabetes or cardiovascular disease may have a combination of diminished sexual desire, neurogenic ED, and vascular ED.
The most common etiology of “organic” ED in the general population is vascular in nature, in which the balance between endothelial contractile and relaxant factors in the corpora cavernosa and supporting vasculature are altered. The next most common category is medication-induced ED, with antihypertensives, several psychiatric medications including selective serotonin reuptake inhibitor antidepressants and antipsychotics, anti-androgens, and opiates continuing to be common contributors. 50 With neurogenic ED, there is disruption to the neurologic input and/or processing in either the central or peripheral nervous systems, leading to loss of coordinated signaling from the autonomic nervous system and the endothelial cells of the corporal bodies. This is most often due to a neurologic condition or injury to the peripheral or central nervous system (e.g., pelvic surgery, spinal cord injury, neurodegenerative disorders, autonomic neuropathy often due to diabetes, or aging). 51 When the normal neurologic input to the penile tissues is disrupted, the corporal bodies may develop relative hypoxia leading to irreversible corporal fibrosis as can be seen after radical prostatectomy for prostate cancer. 52 It is also important to mention the various psychological factors that can cause and/or contribute to ED, making emotional stress, mental health, and relationships important components to understanding ED. 46 Any form of SD may lead to psychosexual stressors, so it is important to acknowledge this with patients regardless of the anticipated etiology.
ED in PD is thought to be the result of multiple factors, but the actual cause is unknown. Some have postulated that it is difficulty with focusing on one specific task that contributes to ED. 53 However, studies have found that ED is the most common manifestation of sexual dysfunction in men with PD. Singer and colleagues found that 60% of men with PD reported ED, as compared to 37.5% of their age-matched controls. 54 In another study from Basson et al., it was shown that men with PD consider erectile dysfunction to be the most distressing disability they experience from their disease. 55 As we will describe below, the treatment pathway for ED is generally applicable to all patients presenting with ED, regardless of the presumed underlying etiology. This is true for individuals with PD as well.
Ejaculatory dysfunction
Epidemiological studies report that 4% to 39% of the population has some form of PE. However, these studies do not often or comprehensively assess bother, likely inflating the prevalence of true PE. Nonetheless, it is important to note that a large percentage of men self-report having some concern about their ejaculatory function. 57 While the prevalence of self-reported PE has been reported to be as high as 39% of men, the prevalence of clinical PE is estimated to be around 5%.57,58
The exact pathophysiology of PE is unknown, though it has been hypothesized that depression, psychological difficulties, hypersensitivity of the glans penis, robust representation of the pudendal nerve, disturbances in central serotonergic neurotransmission, other sexual comorbidities, prostatitis, metabolic syndrome, physical inactivity, recreational drugs, pelvic pain and thyroid disorders are all risk factors. 56 Additionally, it is hypothesized that the underlaying mechanisms for lifelong versus acquired PE are different.
Studies estimate that 40–50% of men with PD will experience onset of acquired PE. 59 Several of the risk factors for PE that may be pertinent to patients with PD are the following: depression or other psychological disturbances, variable cortical representation of the pudendal nerve, disturbances in central serotonergic neurotransmission, physical inactivity, and detoxification from prescribed psychiatric medication.60,61 Treatment is predicated on the degree of bother and patient willingness to pursue treatment. The algorithm is similar to patients without PD who present with PE. As we will describe later in the review, treatment for PE includes behavioral modification, topical anesthetics, and off-label use of medications such as serotonin-specific reuptake inhibitors.
Based on a large, international study of 13,618 men, it is estimated that roughly 14% of adult men 40–80 years-old have trouble achieving orgasm. 63 As age increases, the prevalence of DE also increases with men over the age of 70 being about 3.6 times more likely than men aged 40–49 to report difficulty achieving orgasm. 63 Other risk factors associated with DE are use of psychiatric medications such as SSRIs, depression, erectile dysfunction, diabetes, altered penile sensation, and low testosterone.53,64
The mechanism for delayed ejaculation/orgasm is variable, dependent upon which part in the emission phase is disrupted. Alteration to the central nervous system can also influence arousal responses, causing many centrally acting medications (i.e., SSRIs, ethanol) to influence the development of DE.
Variations in tactile sensation or psychological response to sexual stimulation can alter the arousal response and ultimately influence the emission phase. In contrast to DEO, ejaculatory dysfunction can also occur as a result of obstruction along the ejaculatory anatomic pathway. Patients with prostatic cysts or scarring around the ejaculatory ducts from prior urethral instrumentation may report lack of fluid expelled at the time of climax. Others may experience retrograde flow of semen into the bladder during orgasm/emission as a result of bladder neck incompetency. It is important for clinicians to determine whether patients are experiencing lack of orgasm/climax or simply lack of fluid expulsion, as the diagnosis and treatment pathway are markedly different.
While most of the literature focuses on PE in men with PD, there is a single study looking at patients’ with PD and their sexual functioning in which 39.5% of men reported difficulty reaching an orgasm. 65
Studies on this condition are limited to small series and prevalence is difficult to interpret. At present, it is estimated that 1–10% of the general male population is affected by painful orgasm/ejaculation.67,68 Painful orgasm/ejaculation is more common in patients with certain comorbidities such as chronic pelvic pain syndrome where ethe prevalence is estimated at 30–75%. 69 In many instances, orgasm-associated pain is considered idiopathic. Commonly associated conditions, in addition to chronic pelvic pain syndrome, include ejaculatory duct calculi, benign prostatic hyperplasia, prostate cancer, prior prostate surgery or hernia surgery, sexually transmitted disease, and use of antidepressants or psychotropics.66,70 Interestingly, dyspareunia and sexual pain is frequently mentioned as one of the most common manifestations of PD in females, but it has not been a reported aspect of sexual dysfunction that men with PD experience. 71
It is important to differentiate orgasmic anhedonia for loss of libido. While these can co-exists, many patients with isolated anhedonia will report excellent baseline sexual desire but experience severe frustration with the lack of pleasure despite reaching climax. In contrast, patients with diminished libido will report less desire to engage in sexual stimulation and associated activities with or without a partner. The mechanisms underlying orgasmic anhedonia are poorly understood but are likely the result of changes in the central neurochemical pathways associated with orgasm and pleasure. It is known that psychiatric medications and psychiatric conditions play a major role in the development of the conditions. 74 Additionally, alterations to the nervous system, or having a neurologic condition may alter the synaptic responses to the action of ejaculation.72,73 The rates of orgasmic anhedonia in individuals with PD are not well-studied .However, anhedonia is a common symptom in PD. It is a recognized to be a specific mood disorder caused by dysfunction of the dopamine reward pathway secondary to the degenerative process that occurs in PD. 75
Low libido and testosterone deficiency
Another aspect of sexual dysfunction is hypogonadism and low libido. Low libido is a common sexual dysfunction observed in the general population. In general, it describes the condition in which a man has a deficient amount of desire for sexual activity and has deficient sexual fantasies, which causes him distress and/or interpersonal difficulty. 76 Some patients may refer to these symptoms as having a low “sex drive”. One of the most recent population-based studies investigating prevalence of low libido comes from data out of the Bavarian Men's Health Study. The data suggests that the prevalence of low libido in men at age 50 can be up to 7.2%. 77 This is consistent with two other population-based studies that suggested a prevalence as high as 4.2% and 7.7%. The prevalence rates vary with age, with increasing prevalence occurring at increasing ages.78,79 Nonetheless, the prevalence of low libido is relatively high, and remains the second most common sexual dysfunction disorder, only inferior to erectile dysfunction.
Associated factors with low libido include older age, depression, low physical activity, obesity, diabetes, alcohol consumption, and lower urinary tract symptoms. 77 Importantly, low libido is also known to be one of the most common “symptoms” of decreased testosterone (hypogonadism). 80 However, it should be noted that not all patients with decreased testosterone will experience low libido and vice versa. Often, the factors underlying low libido go beyond simple (and correctable) hormone imbalances. Interestingly, many associated factors with low libido are modifiable and propose a potential point of intervention for improving symptoms. 77
It has been estimated that decreased libido can occur in up to 80% of men with PD. 13 There has been conflicting data as to whether decreased libido is more common in early onset PD or late onset PD.17,81 However, this discrepancy lends itself to the prevalent nature of this problem across all ages of patients. As discussed above, low testosterone levels are a known cause of decreased libido, and male PD patients have been shown to have testosterone deficiency. 82 One study estimates that 35% of men with PD have plasma evidence of testosterone deficiency. 83 This appears higher than rates reported in the general male population, with an estimated 25% of adult men older than 60 years-old having testosterone deficiency. 84 Importantly, the for the higher rates of hypogonadism in men with PD are unknown, and further study is warranted.
Hypersexuality
Hypersexuality is a well described impulse control disorder seen in individuals with PD, in the same category as other impulsive behavior disorders such as binge eating and compulsive buying. 85 The condition refers to an obsession or preoccupation with sexual thoughts, desires, and behaviors. Some examples of behaviors seen in this condition are an increase in self-stimulation, engaging with more online or other available pornography, or exhibitionism in which the person exposes their genitals to a public audience/in public. 86 Interestingly, hypersexuality is more common than other impulse control disorders in men with PD. 87
Hypersexuality is a side-effect of dopamine agonists t, which are the used for PD treatment. 53 Importantly, hypersexuality can be observed in patients with no prior psychiatric history. 88 For example, one specific treatment used in the treatment of late PD, Apomorphine, a dopamine agonist at the D1 and D2 receptors, has been reported to help facilitate erectile function, while also increasing sexual function by helping to control the physical manifestations of PD. 89 However, this can have negative affects as well if hypersexuality occurs.
One study conducted on 3090 individuals with PD using the Minnesota Impulse Disorders Interview found that 3.5% of patients using a dopamine agonist have reported compulsive sexual behavior. 87 Please refer to the more recent study on EOPD (https://pubmed.ncbi.nlm.nih.gov/38841693/). Another study found that some patients experience increased libido as a side effect of Levodopa. 53 It is important to regularly screen for this at appointments so medications can be adjusted as necessary as discontinuation of the offending agent was usually successful at treating the hypersexual behaviors. 87
Motor symptom related sexual dysfunction
While this review has mainly focused on the non-motor symptomatology of PD and how it relates to SD, we would be remiss to not mention the role that motor symptoms of PD can have on one's sexual function. For example, it is easy to comprehend how rigidity, bradykinesia and tremors can make participating in sexual activities difficult. One study points out that the hypersalivation and increased diaphoresis that men can experience can reduce sexual attraction from their partner, thus negatively influencing self-confidence of the patient. 53 Another unintended consequence from the sequela of PD can be that some couples sleep in different beds or rooms due to the motor dysfunction they can experience which then in turn affects the intimacy that a couple may share. 53
Evaluation and treatment pathway
SD is an important yet often neglected manifestation of PD that can greatly contribute to this phenomena.55,59 It is therefore important to discuss sexuality and screen for sexual dysfunction in individuals with PD. This starts with a thorough psychosexual evaluation, focusing on all aspects of sexual function including arousal / libido, erectile and orgasmic function, and sexual activity-associated motor dysfunction or pain (Figure 2). 53
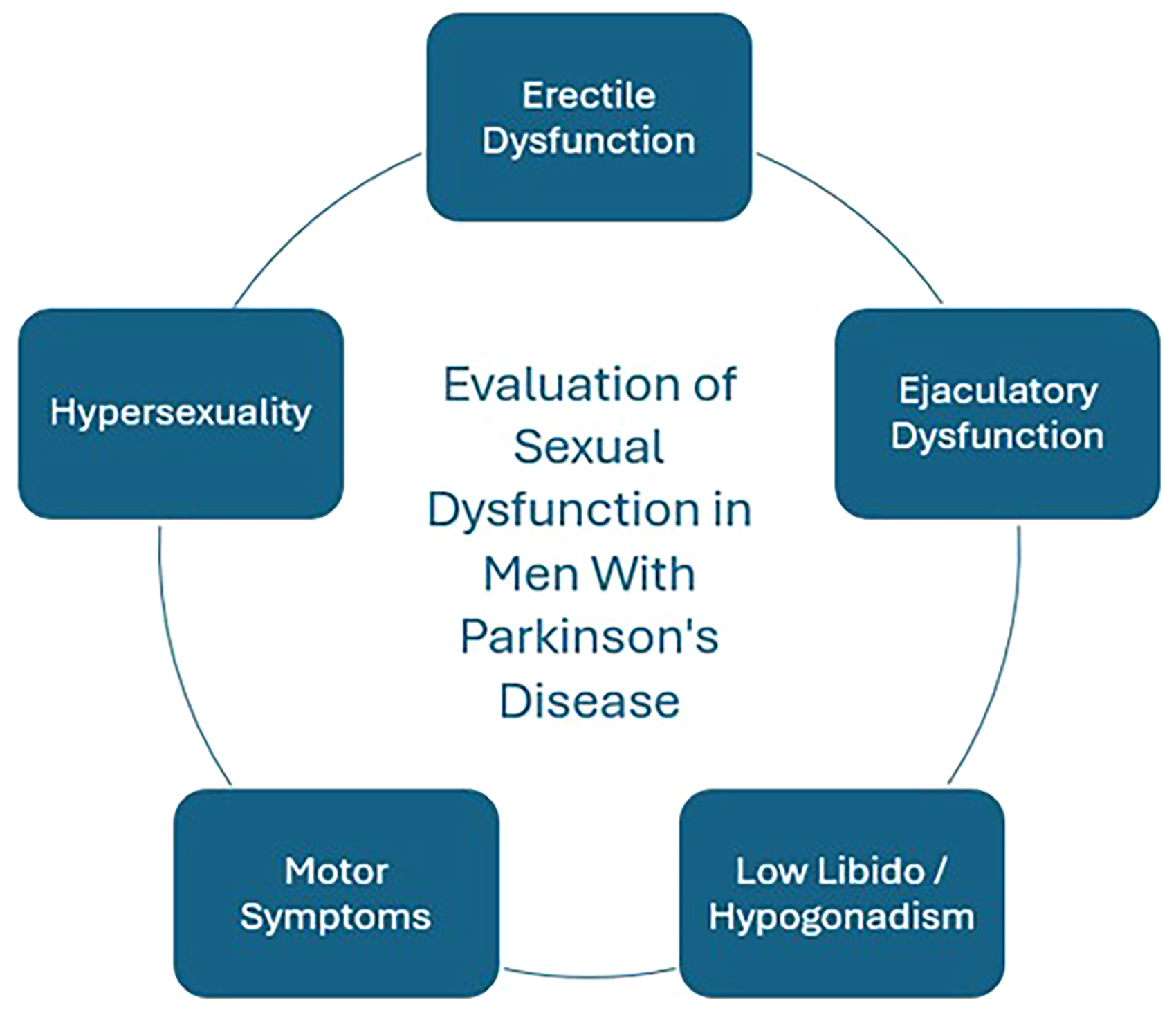
Important components of sexual function to evaluate in patients with Parkinson's disease who report sexual dysfunction.
It is also helpful include partners in these discussions when available, making them aware of the sexual dysfunction that occur from the disease but then to also help look out for some of the hypersexual side effects that can occur from PD treatment. 90 Helping facilitate these conversations for patients and their partners can help relieve the burden of these often-difficult conversations off the patient and help to break through the stigma of having a neurodegenerative disease. 91 A useful tool called the Open Sexual Communication module, was created to assist physicians in discussing and breaching these topics with patients. 91 It is up to us as practitioners to bridge this gap as it can be a difficult topic for patients to bring up on their own but is a topic that can have a monumental impact on a patient's quality of life. A study by Alenko et al. underscores the importance of addressing patient factors in sexual health communication, such as cultural sensitivities and considerations, which advocates for a proactive role from healthcare providers to ensure patient-centered services. 22
Treatment
Advanced treatment pathways for SD are beyond the scope of this review, but in the following section we will describe some basic treatment considerations for patients with SD in the setting of PD (Figure 3).
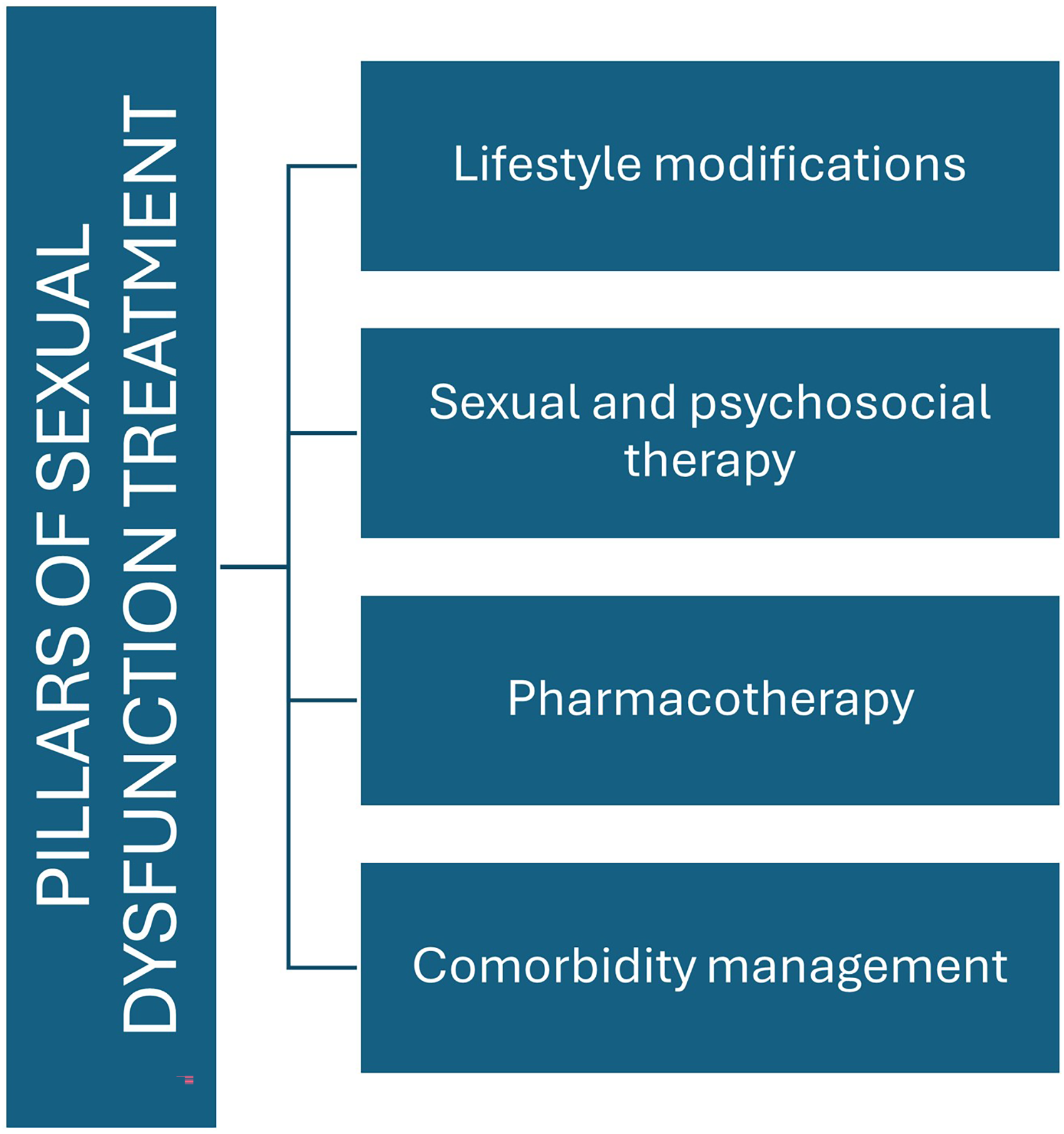
Pillars of sexual dysfunction treatment.
Sleep disturbances are common in individuals with PD. 99 Inadequate and/or poor quality of sleep is associated with hypogonadism and sexual dysfunction. 100 It is thus important to emphasize sleep hygiene and encourage patients to strive for eight hours of sleep per night. 101 Diet is another important consideration. Dietary and nutritional interventions for individuals with PD have been evaluated in several studies albeit with notable limitations including small sample sizes.102,103 Examples include Mediterranean, vegan, and Ketogenic diets, which have been suggested to not only enhance quality of life but also potentially decrease the risk of being diagnosed with PD and other neurodegenerative conditions.103–106 There is evidence that men who adhere Mediterranean or plant-based diets experience less erectile dysfunction.107–109 Finally, limiting alcohol and tobacco use is a general wellness recommendation due to multiple deleterious health effects and increased intake is associated with greater risk of sexual dysfunction.94,110–113 Overall, there is limited research on the influence of lifestyle modification to enhance sexual function in individuals with PD, and this is an area ripe for future study.
Sex therapists also can play a role in helping to address the motor symptoms of PD that can contribute to sexual dysfunction. They specialize in cognitive-behavioral interventions, mindfulness techniques, couples interventions, and physical adaptions that may be needed to enhance sexual function. It has been said that the “goal of sex therapy is to achieve not perfect sexual function, but, rather, the restoration of a lasting and satisfying sexual relationship”. 115 Sex therapists can help these couple think of creative solutions to their unique situation that may be contributing to their sexual dysfunction. For example, they can help brainstorm positions for foreplay and sexual activity that do not require a lot of movement. Additionally, a sex therapist can help investigate any sexual dysfunction that a partner might be experiencing. These can include stress from having a loved one with the disease to the difficulty of separating the caregiver role from their role as an intimate partner. 115 Additionally, a sex therapist can introduce couples to sexual aids such as lubricants and vibrators that may help increase sexual satisfaction in this population. They also can help address any intimacy problems the couple is facing by focusing on nonerotic sexuality. For example, one study has shown that in individuals with PD, the restoration of touch between them and their partners can improve their relationship. 115
For erectile dysfunction, phosphodiesterase-5 inhibitors (PDE5-i) (i.e., sildenafil (Viagara®), tadalafil (Cialis®) have remained a standard of care medication.116,117 These are medications that are taken orally and can be titrated to reach maximal efficacy. A pitfall of these medications is that they often require the patient to take them at a specific time and with the appropriate sexual arousal in order to have effect, somewhat restricting the “on demand” desire of many patients.118,119 The only absolute contraindication for the use of this medication is concurrent use of nitrate-containing medications, such as sublingual nitroglycerin. 120 Several studies have revealed that not only do they promote improved erectile function compared to placebo, but they also lead to improvement in patient satisfaction with sexual experience.121,122 One study exploring erectile dysfunction in individuals with PD found that sildenafil was safe and improved scores on the International Index of Erectile Function (IIEF) scoring system. The starting dose for sildenafil in this study was 50 mg. 123 Interestingly, in a patient with PD that reports failure of PDE5-i use, it is important to consider delayed gastric emptying as a primary cause as this is a common diagnosis in this population. 124 If this is of concern, these patients could benefit from trialing administration of the medication 2–3 h earlier than typical time of administration.
Additional pharmacotherapy offered to patients with erectile dysfunction include intraurethral suppositories (MUSE™), a prostaglandin-E1 medication inserted into the urethra,125,126 and intracavernosal injections, which requires needle injection of a vasoactive agent directly into the corpora cavernosa.127,128 A crossover, randomized, open-label study comparing intraurethral suppositories to intracavernosal injections found that intracavernosal injection therapy was more efficacious, better-tolerated, and more preferred by the patients and their partners. 129 However, the decision to start one of these therapies should be done in conjunction with the patient and their partner, to best understand their goals and comfortability with administration routes. 130 It should be understood also that these pharmacotherapy options do require intact motor ability. However, patients with limited motor function can still be offered these therapies as they may have a partner that is willing to assist with administration of these medications. Importantly, these medications function independently of arousal level and can be a great option for men who may struggle with concentration and/or achieving appropriately arousal levels.
In terms of ejaculatory disorders, the most data supported treatments available are for premature ejaculation.131,132 For patients experiencing symptoms of premature ejaculation, guidelines support the use of daily or on demand SSRIs as first line pharmacologic treatment.56,133 Topical anesthetics are also considered as a first line pharmacotherapy in patients with premature ejaculation. 134 Other medications have been studied and may play a role in pharmacologic treatment for various ejaculatory related symptoms, such as tramadol and alpha-1 antagonists, however the data is limited and less well studied.56,135–137
Regarding testosterone deficiency, there is a high prevalence of low testosterone levels in older men with PD.82,83,138 One study showed that a daily dose of transdermal testosterone gel improved hypogonadism symptoms in this population. Interestingly, these men also had improvements in both non motor and motor symptoms of PD as well with the administration of the gel. 139
Lastly, pharmacotherapy itself should be questioned as a cause for sexual dysfunction in any patient. 140 Many patients will have several medications they take for various conditions they are being treated for. However, polypharmacy in and of itself can be a leading factor for the development of sexual dysfunction. 141 Anti-hypertensives are one medication to be particularly aware of, with a clear link observed between non-specific beta blockers and thiazide diuretics with erectile dysfunction.142–144 Particularly in the Parkinson's population of patients, polypharmacy becomes a pertinent issue to consider. Various psychiatric medications such as antidepressants or antipsychotics play a role in altering the central nervous system response, which can pharmacologically impact sexual function but can also affect a patient's sexual experience.145,146 Working with skilled pharmacists who can understand the intricate relationships between various medications, and taking a multidisciplinary approach to management of a patients medication list can sometimes be the only necessary treatment for a patient experiencing sexual dysfunction.
When applicable, patients should be referred to specialists to manage these conditions.
Conclusion
Normal sexual function is a physiological phenomenon that requires a very complex, coordinated network of responses within the body. When other disease states are present, this complex network can be impacted significantly and lead to sexual dysfunction. PD represents a particularly vulnerable population for development of sexual dysfunction given the impact of disease state on various physiologic networks. The impact of sexual health on one's quality of life can be immense, on the individual and their partner, indicating that early identification and treatment of sexual dysfunction is vital for a patient's overall well-being and health.
Sexual dysfunction comes in various and often overlapping forms but can almost always be identified by taking a thorough patient history that includes a targeted psychosexual evaluation. These topics are not always commonplace for providers in their interviews with patients, but provider education and practice can lead to improved screening for these conditions and overall improved quality of life for our patients.
If a patient with PD is identified to have some form of sexual dysfunction, prompt evaluation by a primary care provider or referral to a sexual health provider should be considered so that a formal sexual health evaluation can be performed. Various treatment options can be discussed at that time, however, the approach to treatment for these patients should remain multi-disciplinary.
There is an overall paucity of research devoted to studying sexual dysfunction in individuals with PD. The current manuscript focused on sexual dysfunction in male patients, whereas data on sexual health in female and transgender patients is lacking to an even greater extent. Despite the shortcomings in the literature the basic principles such as creating a welcoming environment to engage in discussion of these sensitive topics, gathering a thorough sexual health history, identifying potential underlying sexual dysfunctions, and establishing a treatment pathway are important to optimize quality of life for our patients.
Footnotes
Acknowledgements
The authors have no acknowledgments to report.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
