Abstract
The present study aimed to provide an overview of the experiences of couples coping with Parkinson's disease (PD), along with a synthesis of the mechanisms involved in changes within the couple's relationship in the context of PD. These mechanisms were identified using a qualitative approach: dyadic Interpretative Phenomenological Analysis. Forty-five couples separated in three groups according to disease progression, participated. Interviews were conducted separately with each partner. After individual analysis, the salient individual and dyadic phenomena were identified at the group level. Three mechanisms emerged regardless of disease stage: having divergent views on PD, being united and cohesive, avoiding discussing the disease. Other mechanisms were more specific to some stages. Even with few consequences on independence, PD can significantly impact the couple's dynamics. In most cases, strategies for adjusting to PD and/or the changes it causes in the couple's relationship lead to tension and negative emotions. Better support for both partners is needed to promote better adjustment strategies from the early stage of PD.
Plain language summary
This study looked at how couples deal with Parkinson's disease (PD) together. Researchers interviewed 45 couples at different stages of the disease, speaking to each partner separately. They wanted to understand how PD affects relationships. They found three common experiences among all couples, whatever the stage of the disease: i) partners having different views about the illness, ii) couples trying to stay united and supportive, iii) some avoiding talking about the disease. Other couple adjustments depended on how far the disease had progressed. For example, at early stage, some patients and/or partners do not name the disease because they deny its existence. Emotional distancing (a lack of emotional connectivity with the partner) was typically observed at advanced stage. The main takeaway is that even when PD symptoms are mild, it can still change the way couples interact. Efforts to cope with the disease sometimes cause stress and emotional strain. This shows the importance of providing couples better emotional and psychological support early in the disease.
Introduction
Along the course of the disease, people with Parkinson's disease (PwPD) experience a slow progressive alteration of their abilities. While they need support at any stage of the disease, the nature of this support evolves as symptoms worsen and disability increases. In 90% of PwPD, help is provided at home by the spouse, who serves as the primary caregiver. 1
Regardless of the couple's previous dynamics, the illness of one partner inevitably affects the relationship. Studies have shown the interdependence of partners’ distress level and coping strategies in the face of a chronic disease.2–4 In the context of a slowly progressing illness, the coping strategies used by each partner to manage the disease as a couple can be undermined by the illness itself, jeopardizing collaboration and symmetry within the relationship.5,6 This situation can also impact relational quality, which plays a crucial role in both partners’ health and in how they perceive the caregiving experience.7,8 Consequently, many studies have focused on spousal caregivers, reporting an increased burden as the disease progresses, with significant impacts on their quality of life and health.9,10 However, few studies have examined couple functioning11–13 and most have not considered disease severity in their analyses.6,14 There is a clear need for a deeper understanding of the changes that occur in the partner relationships and the mechanisms driving these changes at different stages of the disease.
This article synthesizes the results of a large study carried out in three parts and whose objective was to explore the experience of couples coping with PD, considering disease severity. More specifically, through a qualitative approach, Interpretative Phenomenological Analysis (IPA), 15 used in a dyadic perspective, the aim was to identify the mechanisms through which PD affects the relationship between partners. Among qualitative approaches, IPA is particularly well-suited to explore the experiences of ontological challenges and life transitions, especially those associated with chronic illness. 15 The psychological aspects have already been published in specialized journals.16–18 However, we believe it is equally important to present results of such qualitative studies in a format that is accessible to the broader Parkinson's disease community.
Methods
Participants
The participants whose characteristics are described in Table 1, were recruited through the Movement Disorders Department of the Lille University Medical Center. Forty-five couples were prospectively recruited and divided into three groups according to disease progression of the affected partner. Disease severity was assessed by the score at the Hoehn & Yahr scale. 19 In group 1, patients were at an early stage of the disease, with a time since the diagnosis of less than two years and had been receiving a stable antiparkinsonian treatment for at least six months. Patients in group 2 were at the intermediate stage, with symptoms well controlled by the antiparkinsonian treatment and no fluctuations. In group 3, the disease was more advanced, with a less effective symptoms control and the presence of motor and non-motor fluctuations.
Characteristics of participants.
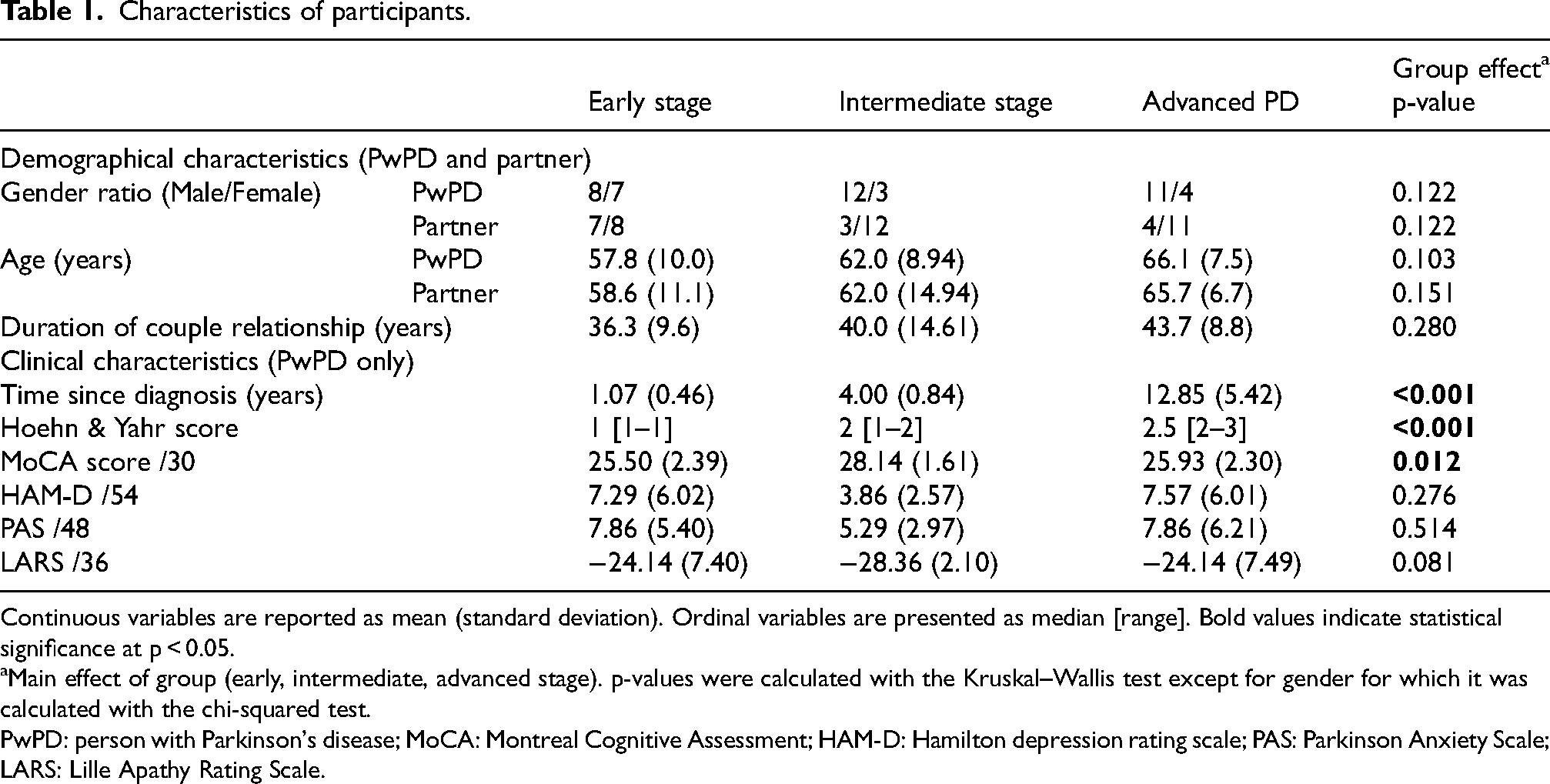
Continuous variables are reported as mean (standard deviation). Ordinal variables are presented as median [range]. Bold values indicate statistical significance at p < 0.05.
Main effect of group (early, intermediate, advanced stage). p-values were calculated with the Kruskal–Wallis test except for gender for which it was calculated with the chi-squared test.
PwPD: person with Parkinson's disease; MoCA: Montreal Cognitive Assessment; HAM-D: Hamilton depression rating scale; PAS: Parkinson Anxiety Scale; LARS: Lille Apathy Rating Scale.
According to Antoine and Smith, 20 this sample size (15 couples per group) enables researcher to consider the entire corpus to gain a comprehensive overview and ensure consistency. Previous qualitative studies in different contexts have shown that data saturation is typically reached with this sample size.21–23 Moreover, sample saturation is not typically considered in IPA, as it primary aims to capture rich, personal, and in-depth accounts of participants lived experiences. 24
Inclusion criteria for both partners included being between 40 and 80 years old and living together as a couple for at least 5 years. Cognitive impairment (scoring <24 on the Montreal Cognitive Assessment 25 ), atypical parkinsonism or another neurological or psychiatric disorder were exclusion criteria for the patients. Severity of depression, anxiety and apathy was assessed by the Hamilton depression rating scale, the Parkinson anxiety scale and the Lille apathy rating scale, respectively.
Before participating, patients and their partners were provided with a detailed information letter, and written consent was obtained from each participant. The information letter clearly stated that the interview would be audio-recorded. Participants were assured of the confidentiality and anonymity of their data, which were coded and associated with pseudonyms.
The study was approved by the National Ethics Committee (Committee for the Protection of Persons, CPP Est IV, IDRCB 2017-A0261152).
Statistical analysis
Demographic and clinical data were compared between groups using the Chi-squared test for gender, the Kruskal–Wallis test for continuous and ordinal variables and the Wilcoxon test for pairwise between-group comparisons, using Jamovi software, version 2.6.44. The significance threshold was set at p-value <0.05.
Interview
Clinical psychologists trained in IPA conducted interviews with each partner separately to encourage more honest and intimate information without fear of hurting the other partner. The interview structure was consistent across all interviews while incorporating the stage-specific features. Topics covered in each group included the experience of diagnosis and previous stages of PD, PD-related emotional experiences, the couple's history and functioning prior the onset of PD, individual and dyadic adjustments, individual and dyadic visions of the future. The interviews lasted an average of 75 min (range: 42–127), were audio-recorded and later transcribed. Further details about how the interviews were conducted can be found in previous articles.16–18
Interviews processing
According to Nizza et al., 26 each interview was systematically analyzed and interpreted by two psychologists who were experts in IPA. IPA is an inductive approach that derives understanding from participants’ discourse rather than testing hypotheses. 24 The researchers analyzed the interviews manually, working first independently and then jointly. They initially explored each partner's experience separately. Then, they cross referenced the two interviews to identify the dyadic processes underlying the experiences of the couples, as well as point of convergence and divergence between the partners. These steps were repeated for each couple. Then, the researchers worked together to identify the significant individual and dyadic phenomena in each group. They then synthetized the experiences of couples in which one partner is affected by PD. Common dyadic processes involved in couple functioning were grouped together, allowing for the identification of relational patterns. Acknowledging the inherently subjective nature of IPA, the collaborative work between the researchers and the maintenance of reflexive stance during the analysis fostered reflexivity and helped to mitigate bias during data interpretation. Each couple's analysis was also presented to the study supervisor, which contributed to greater coherence and reliability in the results. Further details about interviews processing can be found in previous articles.16–18
Results
Demographical and clinical characteristics
The 45 dyads consisted entirely of married heterosexual couples. Among PwPD, 31 were men (8 in the early group, 12 in the intermediate group, and 11 in the advanced group). There was no difference between groups in terms of gender distribution (p = 0.122). The mean age of the participants was 61.86 ± 9.48 years, with no significant difference between groups (p = 0.103) or between patients and partners (p = 0.151). The mean duration of relationship was 39.36 ± 11.94 years, with no difference between groups (p = 0.280).
As expected, there were intergroup differences among patients in terms of disease duration (Kruskal–Wallis chi2 = 38.66, p < 0.001) and disease severity (Kruskal–Wallis chi2 = 29.79, p < 0.001). Despite relatively high mean MoCA scores overall, a significant difference in global cognitive efficiency was observed between groups (Kruskal–Wallis chi2 = 8.81, p = 0.02). Mean MoCA score was significantly higher in the intermediate group compared to the early and advanced groups (early vs. intermediate, W = 3.791, p = 0.020; intermediate vs. advanced, W = −3.374, p = 0.045), while no significant difference was found between the early and advanced groups (W = 0.438, p = 0.949). No significant intergroup differences were observed in the severity of depressive, anxious, and apathetic symptoms. Details are presented in Table 1.
Couple experiences and dyadic mechanisms
Table 2 illustrates the identified dyadic mechanisms. Three emerged regardless of the disease stage, albeit with nuances.
Verbatim excerpts of interviews illustrating the dyadic dynamics identified in couples facing Parkinson's disease at different stages of the disease (G1 = early stage, G2 = when symptoms are stable and well-controlled by treatments, G3 = advanced stage). These excerpts are part of previous publications16–18 of our group in which more details are provided. The first names of the person with Parkinson's disease PwPD (left) and their partner (right) have been changed to preserve anonymity.

Both partners have divergent views on the disease
A non-congruent experience between partners was observed in 11 couples (6 in group 1, 3 in group 2, 2 in group 3), with one partner expressing significant concern about the disease while the other remains more distant and less concerned. In such cases, adjustment becomes difficult. Irritability and tension may arise between partners, placing strain on the relationship. This discrepancy may install a vicious circle of negative interactions, with each conflict escalating the tension and resulting in mutual isolation and feelings of guilt. An asymmetric functioning was also observed at advanced stage of the disease, where one partner worries about becoming a burden or holds excessive hopes for new treatments, while the other is emotionally overwhelmed or lacks the same level of enthusiasm. These tensions can be mitigated by the partners’ ability to reinterpret each other's behavior: for instance, the PwPD's detachment from the disease or their determination to maintain independence despite their limitations can be seen as a strategy to combat the disease and preserve their quality of life together.
Both partners are united and cohesive facing the disease
The disease was considered a life event, like others experienced together by 14 couples (6 in group 1, 3 in group 2, 5 in group 3). Partners relied on the couple as a resource to support each other and relativizing the situation. In these cases, adjustment is harmonious. The partners agreed on how to deal with PD. They express understanding, flexibility, and a willingness to engage in dialogue and adapt to each other's needs. They are aware of present and future challenges and draw inspiration from previously successful strategies to adjust, making individual efforts to maintain the well-being of the couple. This functioning also allows the couple to protect themselves from an uncertain future and share their visions for the future, even on emotionally charged issues like end-of-life decisions. However, in some cases, the dependence of the ill partner can strengthen a fusion or contagion-invasion dynamic. Partners may retreat into their relationship to be together in the present moment. In this form of closeness, expressing one's feelings without harming the other becomes challenging. Consequently, discussions about the disease may be deliberately avoided.
Both partners avoid discussing the disease
In 14 couples (3 in group 1, 6 in group 2, 5 in group 3), communication about the disease was very limited. Some consider that not discussing it is protective, even though it can leave one partner feeling misunderstood. When partners disagree on how to manage the symptoms, they may try to silence their concerns to protect each other or themselves from their partner's reaction. This lack of communication causes tension and misunderstanding, and the distress of one or both partners can be intense.
Other dyadic mechanisms, more specific to particular stages of the disease, were also identified.
In the early stages, some couples (n = 3) choose not to inform their relatives out of fear of disappointment, causing disturbance, or being perceived as invalid. Some PwPD also openly mention the diagnosis but refer to it indirectly, such as “a lack of dopamine.”
Another dyadic dynamic observed in 3 couples in the intermediate group involves resigning to no longer understanding each other. When the differences in experiences have become insurmountable, the partners can no longer alleviate the daily tensions and withdraw from each other, experiencing a form of emotional separation.
Another form of emotional distancing was observed in advanced PD. When dependence is experienced as alienation from the other partner, it causes tensions that can lead to emotional distancing. There may be distancing from the assisting partner as well as a feeling of guilt in the affected person, thinking that they are burdening their partner with inconvenience.
Discussion
Through a qualitative dyadic approach, this study provides an overview of the main mechanisms underlying the dynamics of couples coping with PD at different stages. The results reveal that even when the disease has relatively few consequences on independence, as in the early or intermediate stages, it can still significantly impact the couple's dynamics. Although some couples develop harmonious adjustment strategies to this life event, in most cases, the couple's dynamics breaks down due to maladaptative adjustment strategies, causing tension and negative emotions. While certain strategies, such as avoiding discussions about PD, 4 may provide short-term relief for partners, 4 they have been associated with decreased intimacy and increased distress over the long term. 4 This may help explain why the burden of the disease is experienced as so heavy by most caregivers. 27 It may also contribute to or exacerbate the depressive and anxious symptoms commonly reported by patients and caregivers.3,27–29
This overview represents a necessary first step in highlighting the impact of PD on dyadic dynamics. These results have important implications for healthcare professionals working with patients and caregivers facing PD. Traditionally, only the patient is considered during the care pathway, with a strong focus on medical aspects rather than on psychological or relational dimensions. Yet, these latter dimensions significantly influence individuals’ adjustment, disease experience, and psychological and emotional well-being. Moreover, both partners’ psychological and emotional states affect each other, sometimes leading to interdependence and mutual reinforcement of depressive and anxious symptoms. Emotional and psychological distress can also exacerbate motor symptoms such as gait disturbances, posture issues, and tremors. 30 Thus, the relational difficulties experienced by patients and caregiving partners are highly relevant to the comprehensive management of Parkinson's disease, especially considering the long-term impact on caregivers’ health caused by the progressive loss of autonomy of their loved ones. These results underscore the need to recognize couple-related challenges and their impact, as well as the crucial role of therapeutic work involving both partners. Future steps should include the development of questionnaires or screening tools to help clinicians identify harmful dynamics as early as possible, refer couples to appropriate professionals and create support groups or interventions to assist couples in recognizing and addressing maladaptive patterns—ultimately encouraging participation in supportive care programs.
Although our study was the first to investigate the impact of PD on couples’ dynamics using a qualitative dyadic approach that considered disease severity, we are aware of several limitations. Firstly, the number of dyads in each group may seem small. However, this number is considered sufficient for IPA, according to Antoine & Smith. 20 Secondly, each partner was interviewed individually, without a joint interview. Ideally, an additional joint interview with both partners would have been conducted, but the procedure was already time-consuming, especially for PwPD who often experience fatigue. 31 Social desirability, inherent to self-reported data collection, must also be acknowledged. Thirdly, with the exception of the early-stage group, male patients and female partners were overrepresented in our sample. This imbalance was due in part to the slightly higher prevalence of PD among men but primarily to the prospective recruitment method. This limits our ability to explore the effect of gender on the observed patterns. Future research should consider this, as individual coping strategies that contribute to dyadic adjustment often differ by gender. For instance, female caregivers tend to report greater concern about physical and interpersonal strain 32 and strive to maintain family and home life despite significant personal costs. 33 These reactions may contribute to differing perceptions of the disease and divergent coping strategies within the couple. Fourthly, the groups were not matched in terms of relationship length and caregiver burden, both of which are potential confounding factors not addressed in the present study. Matching for these variables would have made recruitment too restrictive. Nevertheless, no significant difference in relationship duration was found between the groups. Another potential limitation of the study is the lack of exploration into how motor and non-motor symptom subtypes of PD, as well as cognitive and neuropsychiatric disorders, affect dyadic adjustment processes. Investigating these effects would require collecting significantly more data. Our findings show that although cognitive efficiency was slightly higher in the intermediate-stage group, the differences were not pronounced enough to assess their impact on dyadic adjustment. Finally, because we adopted a cross-sectional design, the effect of disease progression was not captured longitudinally but with three separate groups. In chronic conditions like PD, subjective experiences evolve overtime, and capturing the different phases of dyadic adjustment longitudinally would be especially informative. Nevertheless, longitudinal IPA designs present practical challenges that are nearly insurmountable. PD progresses slowly, often over 10 to 20 years, making it difficult to maintain the participation of both partners over such a long period. To overcome these constraints, future studies could include multiple distinct samples, each focused on a specific stage or substage of PD and follow them over a shorter time period to observe changes in dyadic adjustment. This may offer a reasonable compromise between cross-sectional and longitudinal designs.
In conclusion, this study enables better awareness of the experiences of couples coping with PD. Regardless of the stage, some adjustment strategies may be detrimental to the couple's dynamics. This dimension has to be considered in patient care. Better support is needed to promote better adjustment from the early stage of PD.
Footnotes
Acknowledgements
We are grateful to the patients and their partner for their participation in this study and the Lille Centre of Excellence for Neurodegenerative Disorders (LICEND) for their support.
We thank Emilie Constant and Elodie Brugallé for their participation in data collection.
Ethical considerations
The study was approved by the national ethics committee (Committee for the Protection of Persons, CPP Est IV, IDRCB 2017-A0261152).
Consent to participate
Before participation, the patients and their partners were provided with a detailed information letter and written consent was obtained from each participant.
Consent for publication
Participants were assured of the confidentiality and anonymity of their data, with the use of a code and a changed name to designate the participants.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The study was supported by France Parkinson Charity, Grant 951CV723. The funders had no role in study design, data collection and analysis, decision to publish, or preparation of the manuscript.
Declaration of conflicting interests
Guillaume Baille received honoraria for lectures from Abbvie, Lundbeck and Orkyn
Luc Defebvre is member of the scientific board of Abbvie, Aguettant and Alzprotect. He received honoraria for lectures from Abbvie, Orkyn and Sanofi.
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data availability statement
Data cannot be shared publicly because of confidentiality issues and lack of authorization. Data are available from the EST IV Committee for the Protection of Individuals (contact:1, place de l’Hôpital 67091 STRASBOURG Cedex, Tel: 03.88.11.60.03, Fax: 03.88.11.63.48, E-mail: cpp.est4@chru- strasbourg.fr).
