Abstract
Background
Compensation strategies have been shown to improve functional mobility in people with Parkinson's disease (PD) who live independently. However, knowledge on its utilization in in long-term care (LTC) settings is unknown.
Objective
This study aimed to establish the knowledge and utilization of compensation strategies for functional mobility for individuals with PD among healthcare professionals working in LTC facilities in the Netherlands. Secondary aims included assessing subgroup differences among healthcare professionals and exploring perceived barriers to utilizing these strategies in LTC.
Methods
A cross-sectional online survey design was conducted with (allied) healthcare professionals working in LTC facilities across the Netherlands.
Results
Overall knowledge and utilization of compensation strategies among 130 healthcare professionals was high, with a median of 5 out of 7 known categories, 4 out of 7 used for gait, and 3 out of 5 for transfers. Variations among professions existed, with physiotherapists and occupational therapists demonstrating higher scores than nurses and personal care assistants. Professionals specifically trained in PD care and those working in specialized PD departments demonstrated a higher level of knowledge. Main identified barriers for utilization were limited knowledge and time of the healthcare professionals, and concerns regarding limited feasibility in patients with severe cognitive impairments.
Conclusions
While knowledge and utilization of compensation strategies for PD in LTC facilities was widespread, the findings highlight a need for tailored training programs for healthcare professionals to improve patient care. Future research should evaluate the feasibility and usefulness of such training programs.
Plain language summary
The number of people with Parkinson's disease in nursing homes is large and continues to grow. Parkinson's disease is a progressive neurological condition that leads to stiffness, slowness of movement and problems with balance and walking. These movement issues can make it harder for individuals to stay independent, and it can increase their risk of falling, lowering their quality of life. Besides the use of medication, compensation strategies can help to improve movement for those with Parkinson's disease. Compensation strategies are also known as ‘tricks’ that can be applied in daily life to improve movement, such as walking while listening to a metronome. So far, there has been limited research on the use of these strategies in the long-term care setting. In this study 130 healthcare professionals working with people with Parkinson's disease in long-term care completed a survey about their knowledge and the use of compensation strategies. The results showed that overall knowledge and use of compensation strategies was high, but some groups scored higher than others. Physiotherapists and occupational therapists had higher scores than nurses and personal care assistants. Professionals trained in Parkinson's disease care and those working in specialized PD departments also scored higher. The study also explored barriers for using the strategies in daily practice. Main obstacles included limited time and knowledge among healthcare providers and cognitive problems in patients. We concluded that while the use of compensation strategies in Dutch nursing homes is widespread, more effort is needed to reduce differences between different professions and to address the barriers that hinder the proper use in daily practice.
Keywords
Introduction
The prevalence of individuals with Parkinson's disease (PD) is substantial in long-term care (LTC) facilities, and this number continues to rise due to an aging population, and advancements in medical care. 1 In 2020 the estimated number of people with parkinsonism in LTC in the Netherlands was 5000 out of approximately 60,000 patients.2–4 There has been limited research into the treatment strategies tailored for individuals with PD in these facilities. 1
Decrease in functional mobility is a major concern for those with PD. Functional mobility refers to the ability to move around in the environment and includes activities such as standing up, sitting down and positioning in bed. These actions are often part of what is referred to as a ‘transfer’, which involves moving from one surface to another. Additionally, gait is considered a crucial aspect of functional mobility. Individuals with PD residing in LTC facilities generally exhibit more advanced motor and cognitive impairments, both impacting on functional mobility.5,6
While dopaminergic medication can offer some relief from gait disturbances, they frequently fall short of providing a comprehensive solution. 7 To support functional mobility in people with PD, compensation strategies can be used. 8 Compensation strategies are thought to induce a shift from automatic motor control to goal-direct gait control and to activate motor programs that are more goal-directed. 9 Furthermore, they may help to reduce anxiety, which can contribute to improved mobility. 9 For functional mobility, these strategies have been divided into seven categories namely: external cueing, internal cueing, motor imagery and action observation, altering the mental state, changing balance requirements, adopting a new walking pattern, and using alternatives to walking. 10 A personalized approach is needed as the effectiveness of a given strategy can differ significantly from one individual to another. 7 Additionally, people often need multiple strategies tailored to their unique needs to optimize functional mobility, since the effectiveness of a strategy can depend on the specific context in which it is applied. 11 This highlights the importance of personalized approach. 12
A study focusing predominantly on primary care in the Netherlands, showed that a lack of knowledge among healthcare professionals about compensation strategies is a major limiting factor in their utilization in clinical practice. 11 In another study, feedback from both LTC facility staff and patients indicated that there is room for improvement regarding PD-specific knowledge and treatment methodologies for motor symptoms within this setting. 13 As individuals residing in the LTC are reliant on a variety of different healthcare professionals, this knowledge gap in LTC facilities could present a barrier in utilization of compensation strategies. Furthermore, due to the lack of research in LTC facilities there may be some unknown barriers that can hinder the utilization for compensation strategies. 1
Here we establish the knowledge and utilization of compensation strategies for individuals with PD among (allied) healthcare professionals working in LTC facilities in the Netherlands. Secondly, we assess subgroup differences in knowledge and utilization across various professions and whether or not they have received training in PD-specific care. Lastly, we explore the barriers for utilization of compensation strategies in the LTC setting.
Methods
Study design
This study used a cross-sectional online survey design, to reflect on the knowledge and utilization of compensation strategies among healthcare professionals in LTC facilities for patients with PD. The survey (Supplemental Material 1) was distributed through an open survey link via CastorEDC, an online data management platform. Respondents were asked to indicate their workplace and profession, which allowed us to verify afterwards whether they met the inclusion criteria.
The survey consisted of three sections. Part 1 gathered general participant and work-related information. The demographic information gathered in part 1 of the survey included occupation, work setting, region, affiliation with a nationwide network of healthcare professionals specializing in PD management (ParkinsonNet) 14 and specialized PD department, treatment frequency and years of experience. To be affiliated with ParkinsonNet, healthcare professionals must first complete a specialized training program focused on PD management. Further demographic details were omitted to ensure participant privacy. Part 2 focused on participants’ knowledge, utilization, and perceived barriers regarding categories of compensation strategies in the context of gait and transfers. A brief explanation about compensation strategies and an overview of the seven categories with some examples were given. Utilization in gait consists of seven categories of compensation strategies namely: external cueing (e.g., making movements at the beat of a metronome), internal cueing (e.g., focusing on making a heel strike at every count), motor imagery and action observation (e.g., observing someone else walking or imaging a correct transfer from sit to stance), altering the mental state (e.g., decreasing anxiety), changing balance requirements (e.g., making wider turns or using a wheeled walker), adopting a new walking pattern (e.g., running), and using alternatives to walking (e.g., riding a bicycle). Compensation strategies for transfers consist of only five categories, because ‘adopting a new walking pattern’ and ‘using alternatives to walking’ do not apply. Part 3 explored how the healthcare professionals had obtained information regarding compensation strategies and whether they would be interested in further information or training on this topic.
Setting
Data collection was performed from January 16 to April 1, 2024. To improve generalizability, 35 different organizations with LTC facilities across the Netherlands were approached, including those affiliated with the VIP2 Project (a project that explores how to create and improve specialized PD departments in nursing homes in the Netherlands) 15 or recognized by the Dutch Parkinson Association (a national patient organization that provides information and support for people with PD and their caregivers) 16 for providing PD-specific care. However, it is important to note that not all facilities within these organizations necessarily provided Parkinson's-specific care. Reminders were sent to all parties after four weeks to maximize participation.
Participants
Inclusion criteria required participants to be 1) physiotherapists, exercise therapists (trained in movement therapy and rehabilitation with a focus on improving physical function through exercise), occupational therapists, nurses or personal care assistants (a personal care assistant mainly supports daily living activities and basic care, while a nurse can also provide more complex medical care), 2) working in a Dutch LTC facility, 3) involved in treating or caring for at least one person with PD in the past year.
Ethical considerations
This study was conducted according to the principles of the Declaration of Helsinki (version 2013) and in accordance with the EU GDPR (General Data Protection Regulation). As non-WMO research, this study did not require approval from the CMO Radboudumc (the local medical ethics review committee of the Radboudumc). Participants provided online informed consent through CastorEDC before accessing the survey. Data handling and storage adhere to both the FAIR principles and the guidelines of the Radboudumc.
Primary and secondary outcomes
Primary outcomes were the number of categories of compensation strategies known and utilized by healthcare professionals in LTC.
Secondary outcomes included treatment frequency, work experience, profession and PD-specific education or department, to perform subgroup analysis on the knowledge and utilization of compensation strategies between groups. Treatment frequency was divided into the categories: daily, weekly, monthly, now and then, never. Work experience was presented as: 0–3, 4–5, 6–10, 11–15, and 16 + years. While the survey initially distinguished between physiotherapists and exercise therapists these professions were grouped in the analysis process as these professions make use of the same Dutch guidelines in PD. Professions were classified into categories including physiotherapist, occupational therapist, nurse and personal care assistant.
Other outcomes included the perceived barriers for the use of compensation strategies in the LTC setting, collected via free-text entries.
Statistical methods
Analysis was performed using IBM SPSS Statistics (Version 29). The questionnaire was designed in CastorEDC to only allow submission upon full completion. This ensured the absence of missing data in the final analysis.
The primary outcomes knowledge and utilization of compensation strategies by healthcare professionals, were analyzed using descriptive methods. These findings were presented as median and range. Specifically, the analysis focused on the number of categories known and used for gait (ranging from 0 to 7) and transfers (ranging from 0 to 5), as well as the identification of specific known and used categories.
Subgroup analysis was performed using the Mann-Whitney U test to compare professionals with and without ParkinsonNet affiliation, as well as those working in specialized PD departments versus other departments. Additionally, the Kruskal Wallis test was used to analyze subgroup differences based on profession and clinical experience. Clinical experience was categorized into two groups: ≤ 5 years and >5 years, based on a consensus among the authors.
Results
A total of 174 completed surveys were gathered through CastorEDC. Among these, 26 participants were excluded for not working in LTC and 18 were excluded for having professions outside our predetermined scope (e.g., speech therapists, psychologists, dietitians). Therefore, 130 participants were included in the final analysis. The geographical distribution of the included participants covers various regions across the Netherlands (see Supplemental Material 2). Table 1 presents the participant characteristics. Overall, the sample was diverse, with participants distributed across different professions, years of working experience, affiliation with ParkinsonNet and working at PD-specific departments. Notably, over 85% of healthcare professionals in each category reported treating individuals with PD on a weekly basis. Differences were observed in the amount of ParkinsonNet affiliated healthcare professionals among different professions. Specifically, occupational therapists displayed a high level of affiliation, whereas personal care assistants showed a comparatively lower level of affiliation.
Participant characteristics.

Variables are denoted n (%).
not mutually exclusive.
Table 2 displays the median and range of categories known and utilized by the participants. Across all healthcare professionals, the median number of known categories was 5 out of the 7 available categories of compensation strategies. The median number of categories reported as utilized in practice for gait was 4 out of 7 and for transfers 3 out of 5. When asked which category healthcare professionals used the most for gait, 50% reported the use of external cues and 35% internal cues. For transfers, the answers varied between 4 most used categories: 29% external cues, 22% internal cues, 19% changing balance requirements, and 17% motor imagery and action observation.
Knowledge and utilization of categories of compensation strategies.
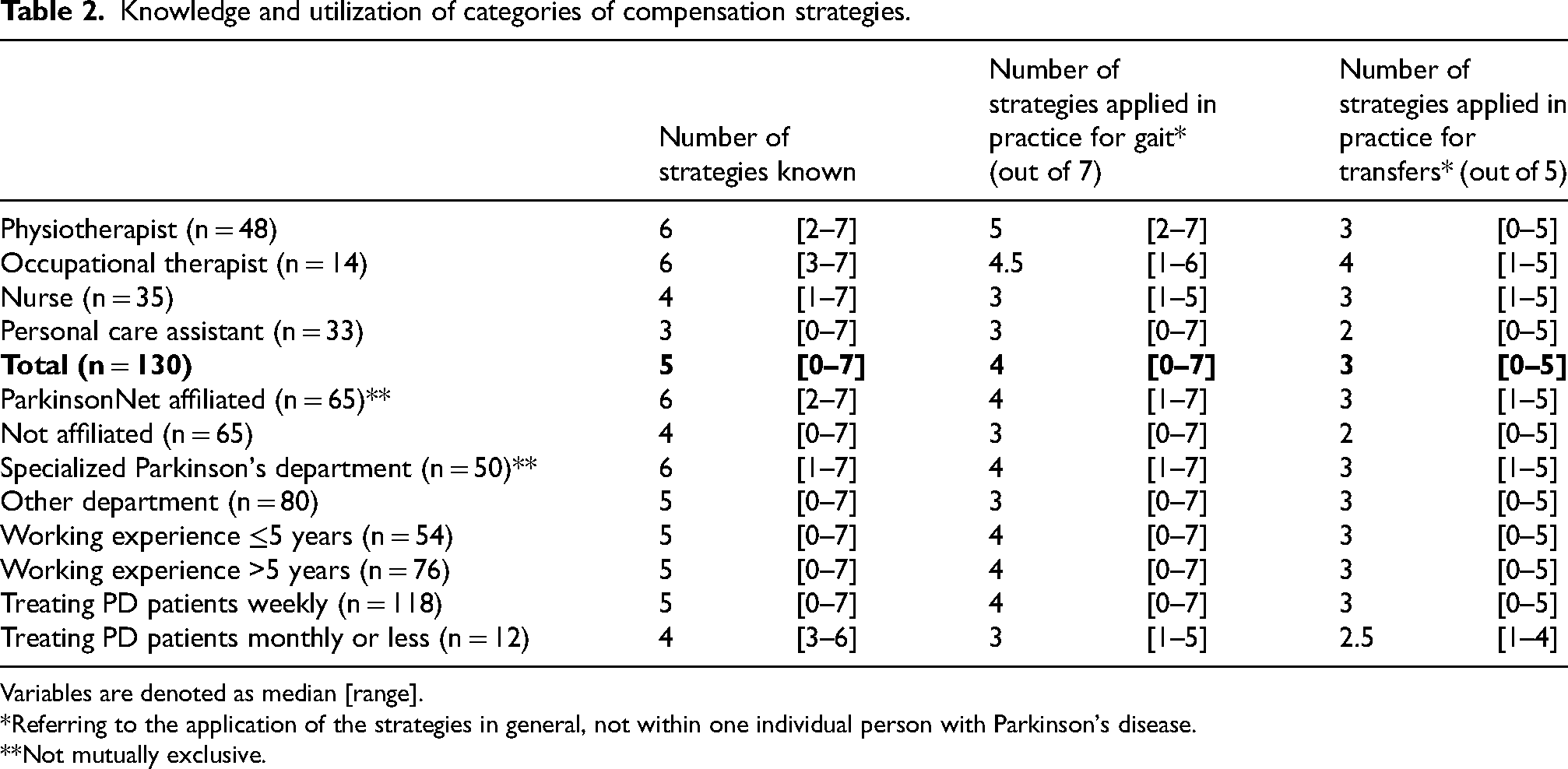
Variables are denoted as median [range].
Referring to the application of the strategies in general, not within one individual person with Parkinson's disease.
Not mutually exclusive.
Figure 1 illustrates the knowledge and utilization per category of compensation strategies across all professions. Overall, the category ‘internal cues’ was best known, while ‘alternatives to walking’ was the least known. All categories showed higher knowledge than utilization, with variations between them. The category ‘alternatives to walking’ displayed the largest gap between knowledge and use. Less than half of the professionals who knew the category, actually applied it in practice. Additionally, ‘altering the mental state’ scored relatively low. The categories of ‘external cues,’ ‘internal cues,’ and ‘motor imagery and action observation’ exhibited the highest utilization in relation to knowledge.
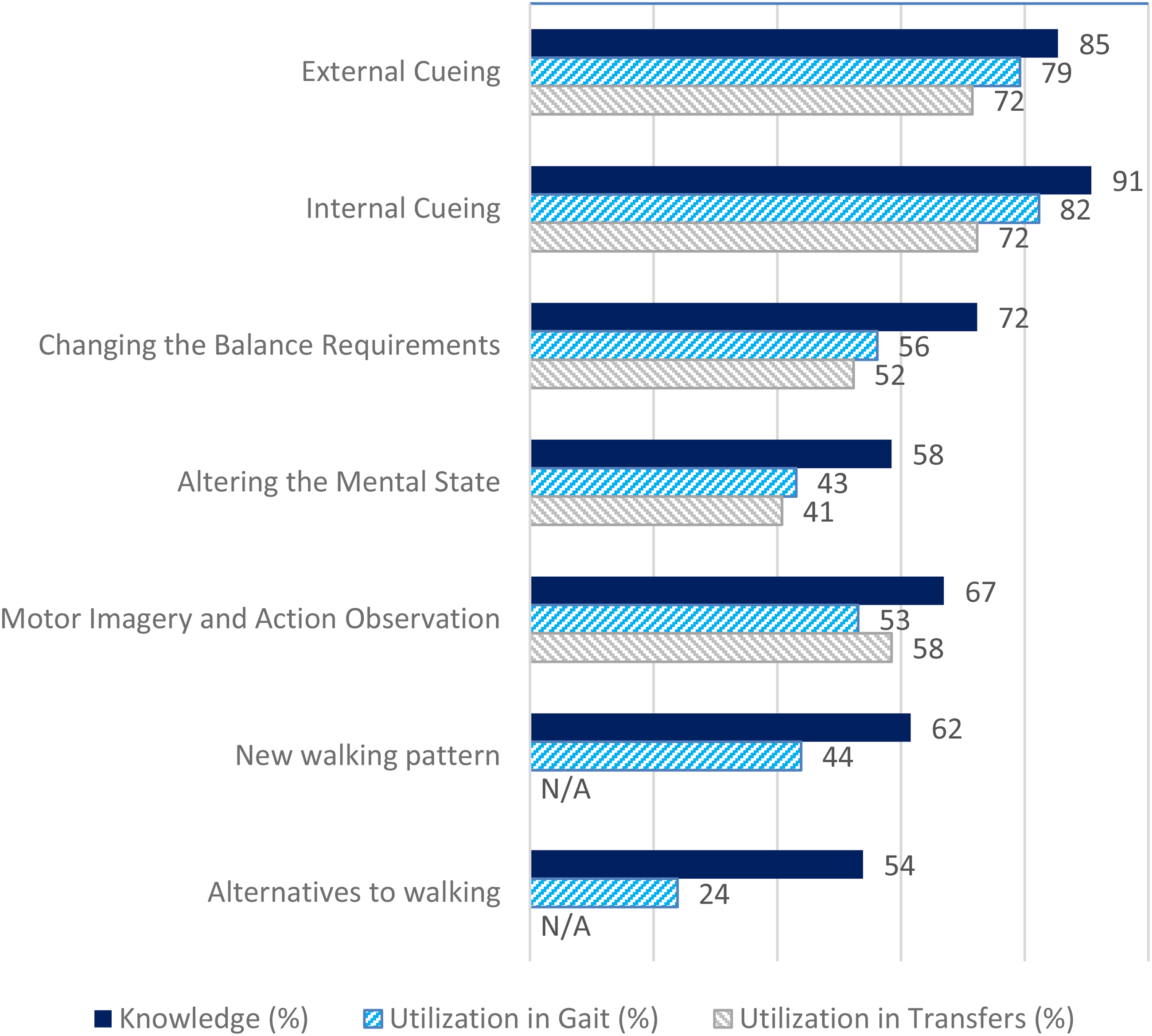
Respondents (%) knowing and using compensation strategies per category (total n = 130).
Subgroup analysis
Subgroup analysis demonstrated a difference between professions for both knowledge and utilization of compensation strategies (p < 0.001). Physiotherapists and occupational therapists presented higher scores in the median number of categories known (Mdn = 6) compared to nurses (Mdn = 4) and personal care assistants (Mdn = 3). Affiliation with ParkinsonNet was associated with greater knowledge of compensation strategies compared to non-affiliated professionals (Mdn = 6 vs. 4; p < 0.001). Similarly, professionals working in specialized PD departments exhibited greater knowledge compared to those not working in specialized PD departments (Mdn = 6 vs. 5; p = 0.001). Years of working experience or frequency of treating people with PD did not show significant differences between groups of healthcare professionals. Supplemental Material 3 provides the median scores, interquartile ranges for each subgroup, and all p-values from the analysis.
Perceived barriers
Several barriers to use compensation strategies in LTC were reported by the participants. Lack of knowledge (22%) and time constraints (32%) were common concerns across all professions, with nurses and personal care assistants expressing them most frequently. Notably, 57% of occupational therapists also highlighted time constraints as a significant barrier to the utilization of compensation strategies in their daily practice. Among 35% of participants the specific nursing home population was cited as a barrier for utilization, with cognitive impairments (including hallucinations) being the primary obstacle. Other factors mentioned were decreased muscle strength, reduced mobility and reliance on wheelchairs. Notably, 63% of physiotherapists in this study identified the patient population as a barrier, a higher proportion compared to other professions. Finally, six respondents (i.e., physiotherapists and occupational therapists) pointed to insufficient implementation within clinical wards. They mentioned the importance of integrating the compensation strategies applied in their treatment sessions into the daily practices of nurses and personal care assistants. However, consistent application was reported to be lacking, resulting in a limited carryover of compensation strategies into daily routines for patients.
Among participants, 85% indicated to be interested in additional training materials to learn more about the different compensation strategies and 82% indicated to have a need for additional patient information material on the different compensation strategies. This interest was spread across the various subgroups. A detailed overview of the interested healthcare professionals by subgroup can be found in Supplemental Material 3.
Discussion
This study investigated the knowledge and utilization of compensation strategies for people with PD, among healthcare professionals in long-term care facilities (LTCs). Using a cross-sectional survey design, we found that: 1) compensation strategies were widely known and used for both gait impairments and transfers among professionals working in LTCs; 2) knowledge and utilization varied across individuals, with higher rates among physiotherapists, occupational therapists, and those affiliated with ParkinsonNet or working in specialized PD departments; 3) discrepancies between knowledge and utilization exist across various categories of strategies, with the largest gap in ‘alternatives to walking’; 4) key barriers to the use of compensation strategies in the LTC setting include the specific population, primarily due to patients’ cognitive impairments. The following sections will provide a more detailed discussion of these findings.
Overall knowledge and utilization
In our study, we found that compensation strategies are widely known and used, with the total study population showing median scores of over half of the categories known and used for both gait and transfers. These scores surpassed our initial expectations based on the findings from a previous study in 2014, 13 which revealed insufficient PD-specific knowledge among healthcare professionals in nursing homes. However, our results are consistent with a more recent study from 2020, 11 which explored the knowledge and use of compensation strategies for individuals with PD among Dutch healthcare professionals, particularly in primary care settings. The observed improvement since 2014 may be attributed to a combination of interventions aimed to improve PD specific care in Dutch nursing homes. Notable initiatives include the establishment of specialized PD departments in nursing homes, along with educational efforts by ParkinsonNet, providing in-company training for nurses and personalized care assistants. 15 Furthermore, an online educational platform on the subject of compensation strategies for PD was launched in 2021. 17
Subgroup differences
Variations among professions demonstrate that physiotherapists and occupational therapists have a higher level of knowledge and utilization of compensation strategies than nurses and personal care assistants. One explanation for this difference is that interventions to improve gait and transfers are integral to the job profiles of physiotherapists and occupational therapists.18,19 In contrast, nurses and personal care assistants often encounter challenges related to functional mobility in patients throughout the day and provide counselling, but typically direct to other professions for interventions. 20 Individuals with PD in LTC facilities often have substantial cognitive impairments,1,5,6 which imposes a reliance on LTC staff for on-demand usage to execute these strategies throughout the day. 21 Ensuring improved knowledge among nurses and caregivers is therefore crucial for effective practical application and can facilitate their daily caregiving tasks.
Healthcare professionals affiliated with ParkinsonNet demonstrated higher scores in both knowledge and utilization compared to their non-affiliated counterparts. Among professionals working within PD specific departments, higher knowledge scores were seen, although utilization showed no significant difference. Notably, a greater proportion of physiotherapists and occupational therapists compared to nurses and personal care assistants in our study were affiliated with the ParkinsonNet organization, benefiting from specialized education on PD. Previous research underscored the benefits of specific education, which likely accounts for the elevated scores within these groups of professions. 22 Interestingly, the majority of participants reported to be interested in (extra) training.
Most used strategies & differences between knowledge and use
Internal and external cues were the most frequently applied categories for both walking and transfers. The prevalence of external cues aligns with previous research findings in the primary care setting 23 and remains the most familiar category, likely due to the abundance of examples people encounter and their ease of variation to suit the patient. A high score on internal cues was unexpected in this population given the cited barrier of cognitive impairments. It is possible that healthcare professionals misinterpreted some external cues as internal cues, such as counting for the patient.
The greatest difference between knowledge and utilization was observed in alternatives to walking. Given that a significant portion of the population relies on wheelchairs, this result was unexpected. Participants may not have recognized that actively moving around in a wheelchair constitutes to ‘alternatives to walking’, possibly leading to an inaccurate view of this category. Additionally, altering the mental state shows a relatively big gap between knowledge of the category and the actual application. This contrasts with findings in a previous study in a general PD population, presenting it as an effective and commonly used strategy. 23 Further investigation is necessary to determine the cause of these gaps in knowledge and utilization.
Perceived barriers
The primary barrier, identified by a third of our study population and mostly by physiotherapists, was that compensation strategies seem to be unsuitable for the nursing home population, with cognitive impairments noted as the most common challenge. Future research should focus on evaluating the effectiveness of compensation strategies specifically within the LTC population, as this has not yet been determined. Additionally, healthcare professionals perceived time and knowledge as barriers for utilization. A new finding from our study reveals that some allied healthcare professionals reported limited integration of the strategies used in therapy sessions into the daily patient care, preventing the development of consistent routines for patient. This inconsistency may be linked to nursing staff having less knowledge and utilization of these strategies. Future interventions should be directed towards addressing this issue by providing training to nursing staff specifically about compensation strategies. Furthermore, common staff turnover and the high number of self-employed workers in the Dutch healthcare sector may also contribute to challenges in integration. 24
Limitations
The sample's heterogeneity captures some of the diversity of healthcare professionals in Dutch nursing homes. However, the findings within the Dutch healthcare system may not be directly applicable to healthcare systems in other countries due to a high-standard network such as ParkinsonNet and the existence of specialized PD departments in the Netherlands. Furthermore, these highly-organized networks likely give an overestimation of the global knowledge and use of compensation strategies in LTC. The majority of participants treated individuals with PD weekly, which could present potential selection bias. With those more involved in the PD care being overrepresented in our study, the scores may be overestimated compared to the global knowledge of compensation strategies. Furthermore, some categories of compensation strategies, such as internal cues and alternatives to walking of compensation strategies may have been misinterpreted by participants. We acknowledge that the survey could have benefited from specific examples relevant to the nursing home context, such as the use of walking aids to illustrate ‘changing the balance requirements’. The lack of specific examples may lead to a skewed view of the results. Given that a significant portion of the LTC population relies on using a wheelchair, future studies may delve deeper into how or whether active wheelchair use could also be facilitated or improved through the application of compensatory strategies.
Conclusion
In conclusion, our study provides new insights into the knowledge and use of compensation strategies for PD, among healthcare professionals in LTC facilities. Whilst knowledge and utilization of different categories of strategies was high, variations exist among professions, possibly contributing to a limited carryover of compensation strategies into patients’ daily routines. Affiliation with ParkinsonNet and specialized departments showed a positive impact, but challenges like limited knowledge, time constraints and patients’ cognitive impairments persist. Addressing the group differences through tailored training programs is important to improve patient care. Further research is needed to evaluate the feasibility and effectiveness of these programs to support the use of compensation strategies in people with PD living in LTCs.
Footnotes
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data availability statement
The data supporting the findings of this study are available upon reasonable request to the corresponding author.
Supplemental material
Supplemental material for this article is available online.
