Abstract
Gender differences in progressive supranuclear palsy (PSP) may become relevant for clinical trials, treatment decisions and patient counseling. To study gender associated differences we conducted a retrospective data analysis of 191 male and 157 female PSP patients from a large multicenter observational cohort in Germany. While no differences in motor skills, disease severity, daily living abilities, global cognitive status and depressive symptoms were observed between genders, male patients showed significantly higher apathy scores, a finding also noted in other neurological diseases. In this study, apart from male patients exhibiting higher levels of apathy, no significant disease-specific gender differences were observed in PSP patients.
Plain language summary
This study investigated whether there are any differences between men and women with a rare brain disorder called progressive supranuclear palsy (PSP). By damaging certain areas of the brain, it can cause progressive problems with balance, movement, vision, speech and swallowing. It can also affect mood, behavior, and thinking abilities. We analyzed data from 191 men and 157 women with PSP who were part of a large study in Germany. It turned out that men and women had similar abilities in movement, daily activities, overall mental ability, and mood (specifically depressive symptoms). However, among people with PSP, men showed higher levels of apathy - a lack of feeling, emotion, interest, or concern about something - than women. Such phenomenon has also been observed in patients with other brain disorders. Overall, this study found no significant gender differences between men and women in PSP, suggesting that gender may not play a major role in the progression of PSP.
Introduction
Gender is a multidimensional concept influenced by social, cultural, and behavioral factors and may modulate health. 1 Gender differences in neurodegenerative diseases are drawing increased attention. Progressive supranuclear palsy (PSP) is a neurodegenerative disorder encompassing a spectrum of clinical phenotypes involving parkinsonism, early postural instability and falls, vertical supranuclear gaze palsy, pseudobulbar symptoms, and cognitive decline. 2 There were only a handful of studies on gender differences in PSP,3–6 and the impact of gender-related factors on PSP are not well established yet. An enhanced understanding of the gender differences is crucial for improvements in diagnosis, treatment as well as clinical trial research in PSP.
Methods
In this study, we retrospectively investigated gender differences in patients from a prospective multicenter observational cohort (n = 348) in Germany. The PSP diagnosis was determined by a movement disorder specialist according to the Movement Disorders Society diagnostic criteria for PSP. 7 The demographic information was collected, including gender, age at disease onset, age at baseline, height and bodyweight. To comprehensively evaluate cognitive functions, motor skills, quality of life and depressed mood in PSP patients, various scales were used. The Montreal Cognitive Assessment (MoCA) was applied to assess global cognitive status, while the Luria Sequence and Three Claps Test evaluated executive functions and motor control. Disease severity was monitored using the Progressive Supranuclear Palsy Rating Scale (PSPRS). Daily living abilities and clinical deficits were evaluated through the PSP Quality of Life Scale (PSP-QoL) and Progressive Supranuclear Palsy Clinical Deficits Scale (PSP-CDS). 8 The Starkstein Apathy Scale (SSAS) measured levels of apathy, and the Geriatric Depression Scale-15 items (GDS-15) was used to detect depressive symptoms. To compare clinical progression over one-year the annualized progression was calculated for each patient according to other studies of our group.8,9
Results
In total, this study examined 191 men and 157 women diagnosed with PSP at baseline. A follow-up examination was carried out 52 weeks after the baseline evaluation including 81 men and 70 women. Men and women with PSP exhibited similar ages of disease onset and ages at baseline.
Out of all patients, specific PSP phenotypes were documented for 241 patients. The distribution of different phenotypes of PSP showed slightly more male patients with the diagnosis of PSP-P, which did not reach statistical significance (Table 1, n = 241, Fisher test, p > 0.05).
Distribution of PSP phenotypes in male and female patients (n = 241).
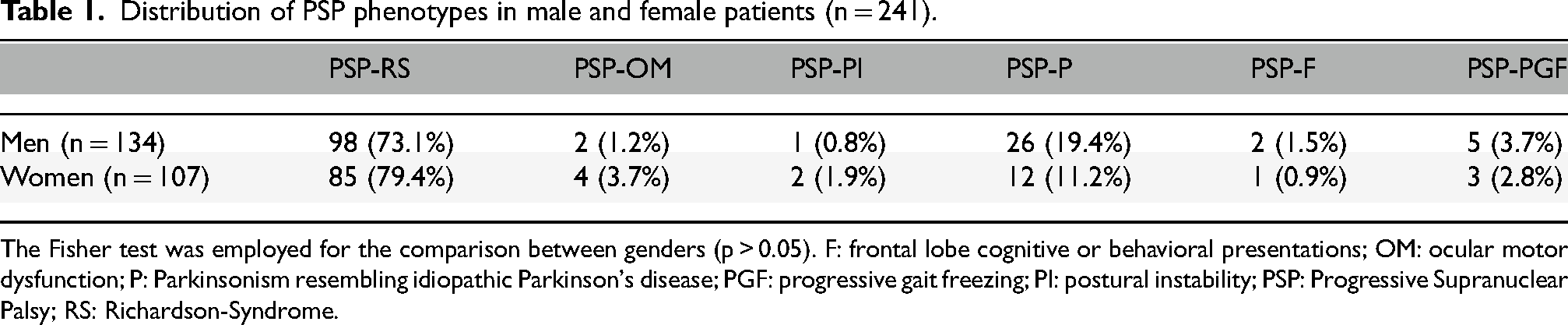

The Fisher test was employed for the comparison between genders (p > 0.05). F: frontal lobe cognitive or behavioral presentations; OM: ocular motor dysfunction; P: Parkinsonism resembling idiopathic Parkinson's disease; PGF: progressive gait freezing; PI: postural instability; PSP: Progressive Supranuclear Palsy; RS: Richardson-Syndrome.
Demographic data and outcome variables at baseline and one-year follow up are displayed in Table 2. Both men and women showed a significant increase in disease severity over 52 weeks with increased PSPRS scores (men: baseline vs. 52 weeks: 34.3 ± 14.8 vs. 42.2 ± 16.4, Mann-Whitney U test, p < 0.05; women: baseline vs. 52 weeks 36.2 ± 15.2 vs. 42.1 ± 18.7 Mann-Whitney U test, p < 0.05). However, there was no significant difference between both genders in the PSPRS over one year (men vs. women at baseline: 34.3 ± 14.8 vs. 36.2 ± 15.2, Mann-Whitney U test, p > 0.05; men vs. women at 52 weeks: 42.2 ± 16.4 vs. 42.1 ± 18.7; Mann-Whitney U test, p > 0.05). In the longitudinal analysis using a linear mixed-effects model, there was a significant effect of time (Estimate = 9.911, SE = 1.276, t = 7.768, p < 0.05), a non-significant effect of gender (Estimate = 2.660, SE = 2.600, t = 1.023, p > 0.05), and a non-significant interaction between time and gender (Estimate = −2.578, SE = 1.869, t = −1.380, p > 0.05).
Male and female PSP patient (n = 348) characteristics at baseline and annualized progression.
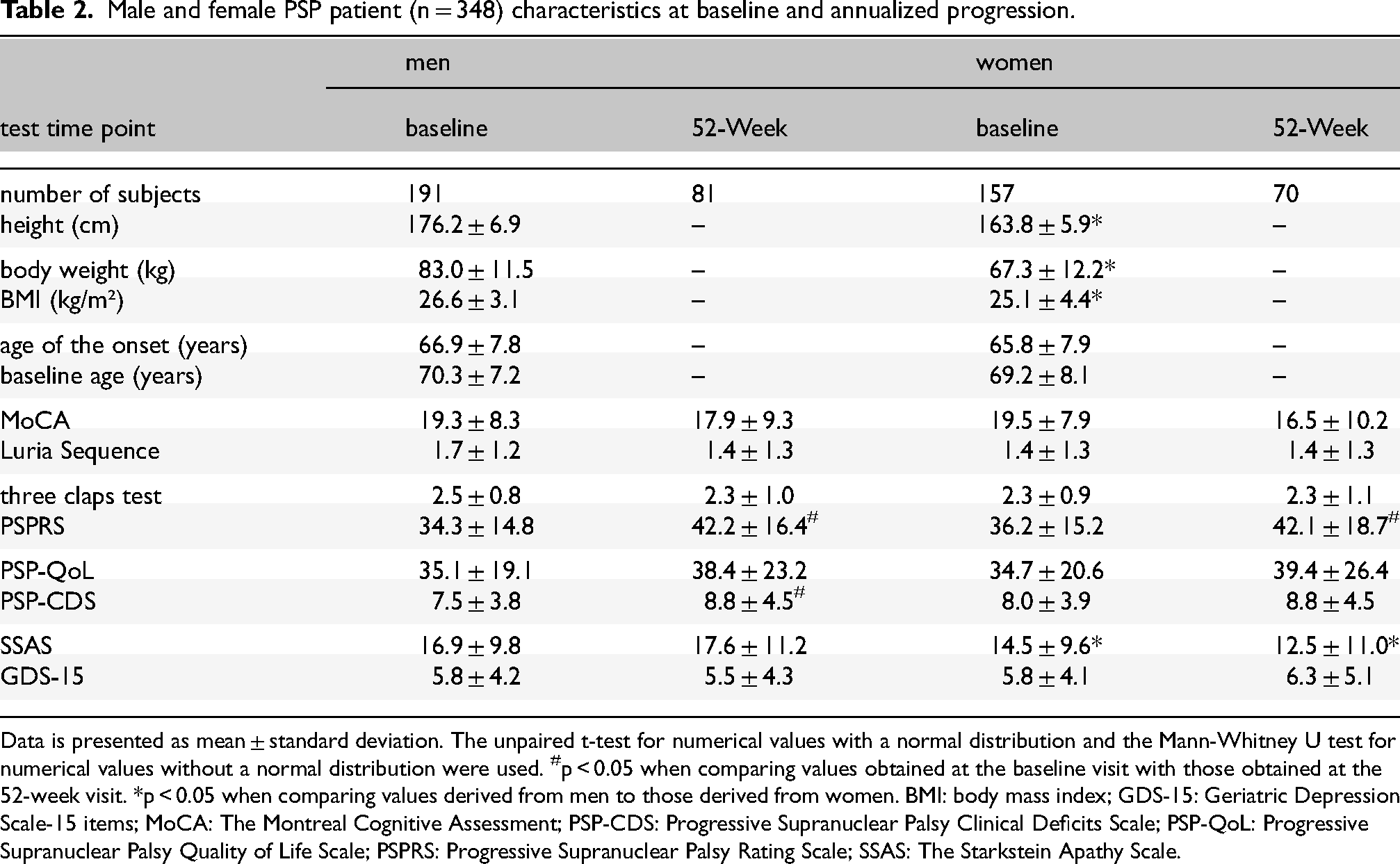
Data is presented as mean ± standard deviation. The unpaired t-test for numerical values with a normal distribution and the Mann-Whitney U test for numerical values without a normal distribution were used. #p < 0.05 when comparing values obtained at the baseline visit with those obtained at the 52-week visit. *p < 0.05 when comparing values derived from men to those derived from women. BMI: body mass index; GDS-15: Geriatric Depression Scale-15 items; MoCA: The Montreal Cognitive Assessment; PSP-CDS: Progressive Supranuclear Palsy Clinical Deficits Scale; PSP-QoL: Progressive Supranuclear Palsy Quality of Life Scale; PSPRS: Progressive Supranuclear Palsy Rating Scale; SSAS: The Starkstein Apathy Scale.
The severity of motor symptoms and their impact on daily activities were comparable between men and women, showing similar baseline PSP-CDS scores (men: 7.5 ± 3.8, women: 8.0 ± 3.9; Mann-Whitney U test, p > 0.05). This similarity persisted after 52 weeks (men: 8.8 ± 4.5, women: 8.8 ± 4.5; Mann-Whitney U test, p > 0.05). Additionally, PSP-QoL scores were also comparable at baseline (men: 35.1 ± 19.1, women: 34.7 ± 20.6; Mann-Whitney U test, p > 0.05) and after 52 weeks (men: 38.4 ± 23.2, women: 39.4 ± 26.4; Mann-Whitney U test, p > 0.05). Moreover, no differences were observed in depressive symptoms assessed by GDS-15 between men and women with PSP at baseline (5.8 ± 4.2 vs. 5.8 ± 4.1; Mann-Whitney U test, p > 0.05) as well as at the 52-week follow-up (men vs. women: 5.5 ± 4.3 vs. 6.3 ± 5.1; Mann-Whitney U test, p > 0.05). The linear mixed-effects model revealed no statistically significant effects of time (p > 0.05), gender (p > 0.05), or their interaction (p > 0.05) on the scores of MoCA, Luria Sequence, three claps test, PSPRS, PSP-QoL, PSP-CDS and GDS-15. This suggests that there were no significant longitudinal changes in these scores between men and women over one year.
However, male PSP patients showed significantly higher SSAS scores already at baseline, i.e., more apathy than women (men vs. women: 16.9 ± 9.8 vs. 14.5 ± 9.6, Mann-Whitney U test, p < 0.05). This difference increased after a 52-week follow-up period (men vs. women: 17.6 ± 11.2 vs. 12.5 ± 11.0, Mann-Whitney U test, p < 0.05). In the linear model analysis, there was a significant intercept (Estimate = 16.9172, SE = 0.8125, t = 20.822, p < 0.05) and a significant effect of gender (Estimate = −2.4598, SE = 1.2098, t = −2.033, p < 0.05), while the effects of time (Estimate = 0.7192, SE = 1.4935, t = 0.482, p > 0.05) and the interaction between time and gender (Estimate = −2.6604, SE = 2.1692, t = −1.226, p > 0.05) were non-significant. These results suggested a consistent gender-related disparity in apathy symptoms among PSP patients.
Discussion
In summary, the present study analyzed a large cohort of PSP patients (n = 348) for gender related aspects. The findings revealed only minor gender-specific differences among male and female PSP patients. The ratio of male to female in PSP patients is generally considered to be 1:1. In our study, a slightly higher proportion of male participants was observed. Consistent with national physical attribute data from Germany, men displayed significantly higher values in height, body weight, and body mass index. No differences were found in executive functions, motor control, disease severity, or daily living abilities between men and women. Consistent with a previous report, 3 no difference in global cognitive status was observed between genders. Although it has been reported that women generally suffer more often from depressed mood and depression than men, 10 we did not find the gender disparity in depression in PSP patients.
Notably, male patients with PSP present more apathy. Actually there are multiple factors that could complicate the assessment of apathy, such as bradykinesia and depression, which might interfere with the assessment of apathy. However, the SSAS is a validated 14-item questionnaire designed to assess apathy. It contains aspects such as learning, general interest, engagement, and goal-directed behavior, many of which help differentiate apathy from akinesia, although certain items (e.g., items 8, 12, and 14) may be influenced by factors affecting overall energy levels. Moreover, similar gender differences in apathy were also shown in studies of Parkinson's disease,11,12 Alzheimer's disease, 13 vascular dementia 14 and multiple sclerosis. 15 The greater severity of apathy in men across various neurological disorders suggests that this phenomenon may not be disease-specific but rather gender-related. Understanding these gender differences can facilitate clinical trials, for example, when recruiting participants. Further studies should concentrate on gender differences in treatment response in patients with PSP.
As limitations, dropout occurred during our study follow-up, which is typical and almost unavoidable in a PSP observational cohort because of the severity of the disease. Additionally, we did not conduct extended neuropsychological assessments, such as Consortium to Establish a Registry for Alzheimer's Disease (CERAD) Plus, and no imaging data were available for this analysis.
Footnotes
Acknowledgments
We would like to thank our patients and research volunteers.
ORCID iDs
Ethical considerations
We obtained approval of the local institutional review boards at Hannover Medical School and all participating study centers for this work (Ethics vote number: 3558-2017).
Consent to participate
All patients or legal caregivers gave their written informed consent.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data availability statement
The data supporting the findings of this study are available from the corresponding author Dr Lan Ye upon reasonable request.
