Abstract
Purpose
Despite knowing that adolescents with disabilities face substantial barriers transitioning from pediatric to adult health care, little is known about how pediatricians experience transition-related tasks for their patients with disabilities.
Methods
The 2023 American Academy of Pediatrics (AAP) Periodic Survey utilized a cross-sectional random sample of post-trainee, non-retired, US-based AAP members to derive a nationally representative sample. Several questions related to transition services were compared. Data were weighted for non-response bias. Only AAP staff conducting the statistics had access to the non-anonymized data.
Results
Over half of the pediatricians reported discussing consent for care (56.3%), assisting with referrals to adult care (56.5%) and providing anticipatory guidance about sexual health and development (52.7%) to most or all adolescents with disabilities. In addition, 22.7% reported providing all four transition services to most or all of their adolescent patients with disabilities. A majority identified barriers that impeded successful transition of their patients with disabilities.
Conclusion
While many pediatricians engaged in a variety of transition-related activities for their adolescent patients with disabilities, they also identified numerous barriers. These findings underscore the importance of addressing both the practice and system level barriers that limit pediatricians’ abilities to provide transition services for their patients with disabilities.
Keywords
Introduction
Adolescents with disabilities face substantial barriers transitioning from pediatric to adult health care.1,2 Fewer families of adolescents with disabilities report having their transition needs met compared to adolescents without disabilities. 1 Current data are lacking on pediatricians’ experiences related to transitioning adolescents with disability to adult care. 3 To address this gap in knowledge, US pediatricians were surveyed to assess transition services and perceived barriers to transition for their adolescent patients with disabilities. The associated hypothesis was that pediatricians would endorse that there are barriers to transition for adolescents with disabilities.
Methods
The 2023 American Academy of Pediatrics (AAP) Periodic Survey utilized a cross-sectional random sample of post-trainee, non-retired, US-based AAP members to derive a nationally representative sample. The survey was developed by AAP staff in close consultation with subject matter experts and contained two sections: one on immigration and one on caring for children with disabilities. After piloting, the survey was fielded from May to November 2023. Surveys were mailed to 1996 pediatricians and included a $2 bill as a token incentive. There were 10 follow-ups to non-responders (emails with a link and paper versions) sent at four-week intervals. This yielded a 33% response rate. The analytic sample consisted of 308 pediatricians who reported providing ongoing primary or subspecialty care to adolescents with disabilities. The AAP Institutional Review Board deemed the study exempt from review.
Pediatricians were asked to consider a patient to have a disability if they were “usually or always limited in their abilities to do the same thing children of the same age typically do, such as walking, taking care of oneself, communicating, etc.” Survey items identified the average age at which pediatricians thought transition services should begin and the percentage of pediatricians whose practice offered transition services (discussing consent and confidentiality; assisting with establishing referrals to adult providers; assisting with medical documentation for program eligibility; and providing anticipatory guidance and education regarding sexual health and development). Pediatricians were asked if they had a dedicated staff member who was responsible for coordinating transition of care planning for adolescent patients with disabilities. Other questions addressed potential barriers to providing transition services including lack of knowledge on the part of the adolescent about their own condition and/or skills to self-advocate, lack of available physicians who accept young adults with disabilities as new patients and lack of dedicated staff to provide transition services. Data were weighted for non-response bias (respondents were slightly older and more often female than non-respondents). Only AAP staff had access to the raw non-anonymized data. The descriptive statistics were calculated using IBM SPSS Statistics 25.0 (Armonk, NY).
Results
Pediatricians (see Table 1 for demographic characteristics) reported that transition planning should begin at an average age of 17.4 years and 17.6 years for their patients with and without disabilities, respectively. More than half reported discussing consent for care (56.3%), assisting with referrals to adult care (56.5%) and providing anticipatory guidance about sexual health and development (52.7%) to most or all adolescents with disabilities [Figure 1]. Forty-two percent reported assisting with medical documentation for program eligibility for their adolescent patients with disabilities. One in five (22.7%) reported providing all four transition services to most or all their adolescent patients with disabilities.
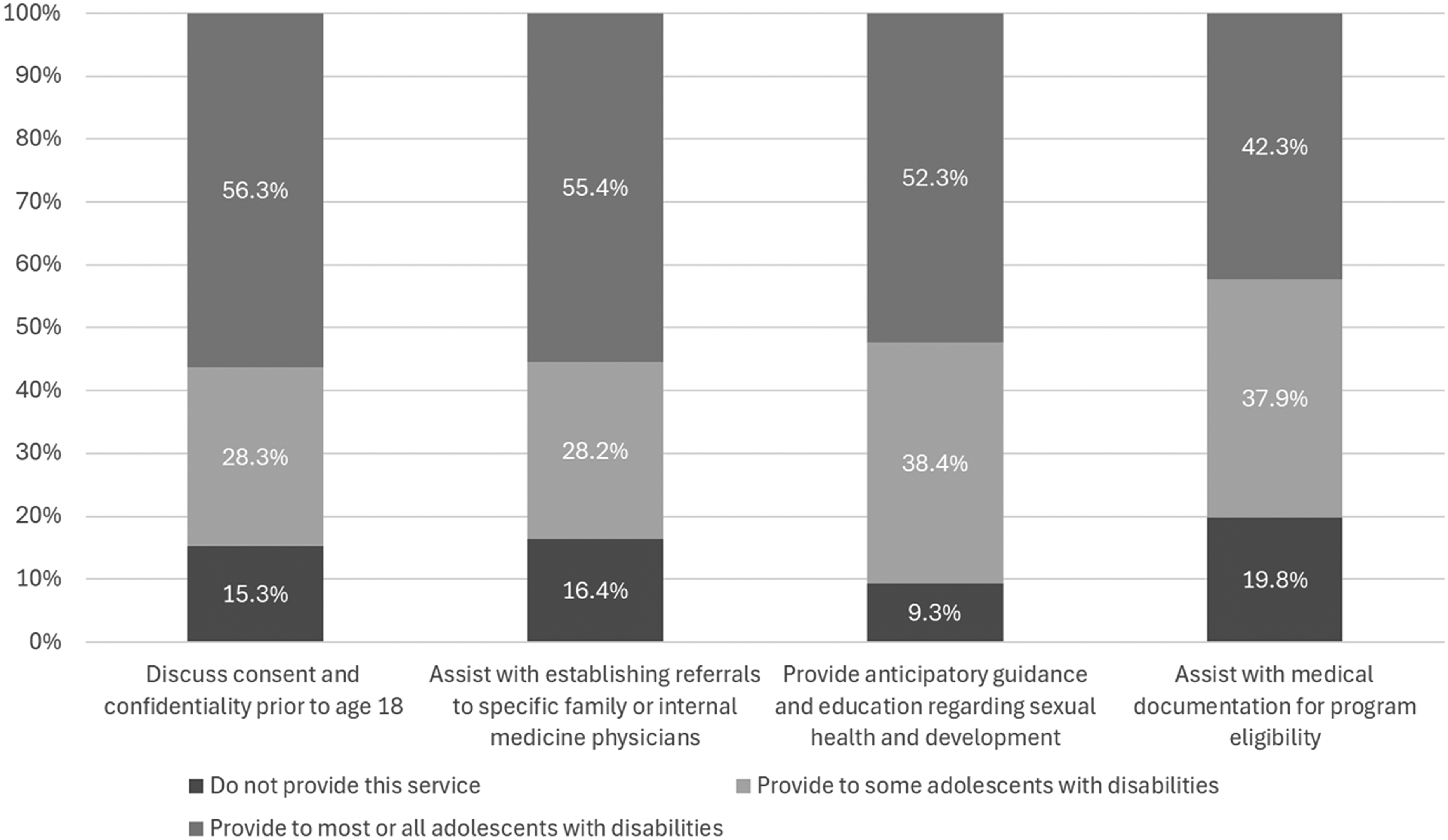
Pediatrician reported transition of care services for adolescent patients with disability (N = 308).
Demographic and practice characteristics of the analytic sample (n = 308).

*Other includes multi-racial, American Indian/Alaska Native, Native Hawaiian/Pacific Islander and other.
**HMO = Health Maintenance Organization (hired staff model).
Seven in 10 (68.9%) reported their practice did not have dedicated staff responsible for coordinating transition of care planning for adolescent patients with disabilities. Other barriers reported as ‘major’ or ‘moderate’ by the majority of pediatricians included adolescents’ lack of knowledge about their condition (70.4%), lack of available physicians to assume care after adolescents transition from pediatric care (62.2%), and lack of sufficient staff to provide transition services (59.6%) [Figure 2].
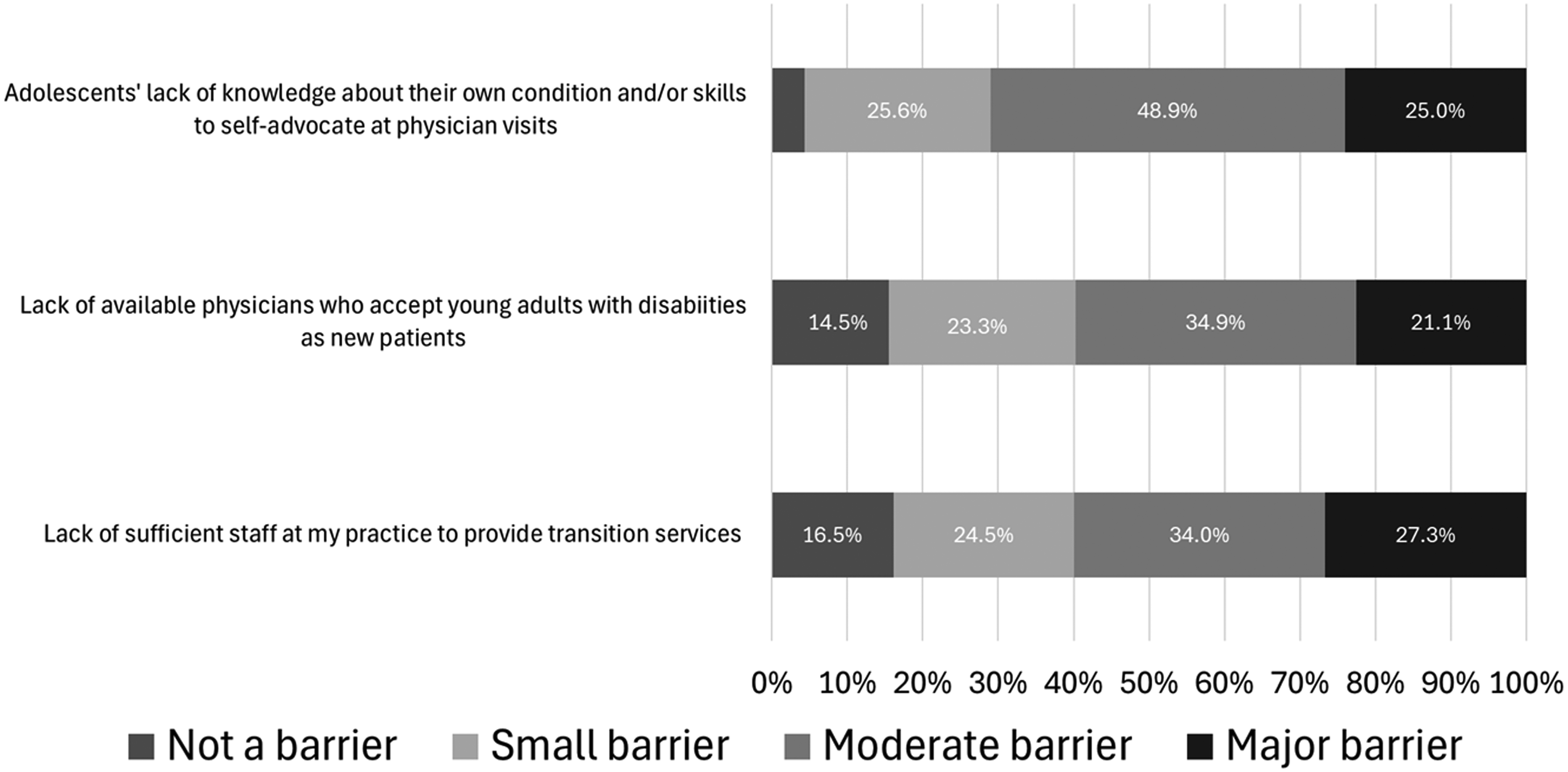
Pediatrician reported barriers to transition of care for adolescents with disability (N = 308).
Discussion
AAP guidance recommends starting transition planning between 12–14 years of age. 1 Pediatricians in this study indicated their practice initiates care transitioning for adolescents about three years later than recommended regardless of disability status. These data indicate an opportunity for pediatricians to align their practice with existing guidance for all adolescent patients and develop their transition services accordingly, 4 especially for adolescents with disabilities who often rely on numerous systems of service for which continuity is important.
Roughly one-quarter of pediatricians reported their practice has four key services in place to support the transition of their adolescent patients with disabilities to adult care. Notably, nearly six in 10 pediatricians surveyed reported discussing consent and assisting with referrals to adult care; this is higher than pediatricians reported in a 2008 Periodic Survey report. 3 This indicates active practice improvement on the part of pediatricians. Most pediatricians in the current study also reported a lack of available physicians to whom to transition services and lack of dedicated staff as barriers. These findings underscore the importance of addressing both the practice and system-level barriers that limit pediatricians’ abilities to provide transition services for their adolescent patients with disabilities. 5 Research indicates that health care providers who care for adult patients lack knowledge, experience, skills and the desire to care for adults with disabilities. 6 Limited availability of quality primary care for adults with disabilities is a known problem that requires strategies and reforms beyond the pediatric workforce.6,7 To help mitigate adverse health outcomes related to inadequate transition services, 8 practices may consider quality improvement projects aimed at increasing provision of transition services in accordance with recommended timing of delivery.1,9,10 For example, Got Transition recommends hosting in-service trainings for staff involved in the care of adolescents with disabilities as well as identifying an office champion who can keep the practice supplied with resources for adolescents and their families. 11 Health system investments to support team-based transition services could enhance the system of care for adolescents with disabilities, especially programs targeted to help practices with fewer resources. 12 Of note, the findings presented here are of a cross-sectional survey that did not allow for the assessment of causality and was self-reported, so actual differences in how care was delivered cannot be evaluated. Further, the response rate was 33% requiring correction for non-response bias and limiting sub-group analysis. Nonetheless, these data identify important opportunities to improve transition services for adolescents with disabilities and set the stage for future research into how to best provide anticipatory guidance regarding transition-related needs for physical and mental health services.
Footnotes
Acknowledgements
Work was done without funding
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
