Abstract
Purpose
This study aimed to identify the perceptions of pediatric physical therapists, identifying barriers and facilitators to providing telehealth services during the COVID-19 pandemic.
Methods
Using a mixed methods design, an online, national survey gathered demographics and participants’ perceptions.
Results
A total of 165 pediatric physical therapists participated in the study. Sixty-four percent of respondents rated their pre-pandemic perception of telehealth services as “somewhat” to “very” negative. After utilizing telehealth, 66% of therapists reported perceptions of telehealth as “somewhat” or “very” positive. Barriers were 1) poor patient and parent participation and 2) technology issues. Facilitators were 1) hands-on involvement, 2) ability to share information, and 3) ability to use items in the home. Predominate themes to open-ended responses further elucidated pre- and post-pandemic telehealth perceptions.
Conclusion
After implementing telehealth services during COVID- 19, most therapists indicated their perceptions of telehealth were somewhat or very positive.
Background
The mandate to maintain social distancing during the COVID-19 pandemic forced physical therapists in the United States (US) to adapt the provision of rehabilitation services, including those for the pediatric population, through means such as telehealth. In the US, telehealth had not been widely utilized by pediatric rehabilitation services prior to the COVID-19 pandemic. Several studies have examined the potential use of telehealth services in providing physical therapy (PT) intervention for various diagnoses in the adult population, including effectiveness in rural and remote areas.1–5 Additionally, systematic reviews have pointed to the effectiveness of telehealth rehabilitation for adults. 6 However, little research existed assessing the effectiveness or feasibility for the pediatric population. As pandemic restrictions have eased over the last 1-2 years, studies have begun to emerge, assessing the role of telehealth in providing pediatric PT services.7,8
The COVID-19 pandemic forced significant changes in service provision, including pediatric PT. As a result, telehealth transitioned from a novel to necessary approach to providing pediatric telehealth therapy services almost overnight. 9 A search of the literature demonstrated that, prior to the COVID-19 pandemic, there were studies that examined the efficacy of using telehealth for pediatric weight management, 10 promoting physical activity for children with disabilities, 11 and mental health services provided to families with children with traumatic brain injury. 12 However, few if any studies existed to indicate the feasibility or effectiveness of utilizing a telehealth platform for pediatric PT services, a critical prerequisite for expanded use. Since the COVID-19 pandemic, several studies have been published regarding the impact of providing pediatric PT services through telehealth.13–15 To better understand how telehealth may be utilized in a post-COVID era, especially with regards to potential application in remote, rural or underserved areas, continued analysis and research into the efficacy of pediatric PT services provided through telehealth is warranted. Additionally, continued research is necessary to identify the facilitators and barriers to providing telehealth PT services for therapists and patients, to be able to improve access to care.13–15
The purpose of this study was to identify the perceptions of telehealth as a delivery service method for pediatric PT services as well as barriers and facilitators to providing those services from the perspective of pediatric physical therapists. The specific aims of this study were to 1) assess pediatric physical therapists’ perceptions of telehealth and 2) identify facilitators and barriers that families, patients, and pediatric physical therapists might encounter with respect to participating in telehealth.
Methods
A mixed methods design was used to assess perceptions of pediatric physical therapists regarding provision of pediatric PT services during the COVID-19 pandemic. Inclusion criteria included pediatric physical therapists licensed and practicing in the US during the COVID-19 pandemic from December 2020-April 2021. This study was conducted with approval and in accordance with the Institutional Review Board (IRB). Purposeful sampling was utilized to recruit participants for this study. Following IRB approval, the survey was disseminated through online forums, specifically the Academy of Pediatric Physical Therapy of the American Physical Therapy Association (APTA) monthly newsletter “Milestones,” and APTA Special Interest Groups (SIGs) including the Pediatric Residency and Neonatal Intensive Care Unit Fellowship SIG. Additional recruitment sources included social media forums directed specifically to pediatric physical therapists. The level of education and experience of the reviewing pediatric physical therapists ranged from Doctor of Physical Therapy to certified pediatric clinical specialist to Doctor of Philosophy, totaling greater than 30 years of clinical experience.
Data Collection: The online survey was developed utilizing Qualtrics; questions were developed by the research team. A link was provided within the research flyer to allow for easy access to the survey. The survey included both multiple choice questions and additional follow-up questions (Appendix 1). Respondents were able to further elaborate on their responses via an open-text box format to better capture the depth and richness of perceptions. In addition to gathering demographic data, therapists’ current and previous perceptions of telehealth and facilitators/barriers to participation in telehealth sessions for themselves and their patients/families were assessed.
Several questions had multiple components and were formatted utilizing the following strategies: 1) Likert scale; 2) Rating system, ‘least to most;’ and 3) Word bank which allowed for a quantitative analysis of responses. Participants were also asked to elaborate on their experience through a series of open-ended questions.
Prior to national dissemination of the survey, four licensed pediatric physical therapists provided survey feedback to ensure content validity. To prevent a participant from submitting more than one survey response, specific fail-safes were activated through Qualtrics that limited survey responses to one submission per participant.
Data analysis
Utilizing complete case analysis, survey responses that were incomplete were removed from the data set. Due to the limited responses from pediatric physical therapists who had not implemented telehealth during the pandemic, analysis focused on the data of only pediatric physical therapists who had implemented telehealth during the COVID-19 pandemic. Quantitative data was transferred from Qualtrics to an Excel spreadsheet. Responses were calculated as percentages of the total to identify trends in the data. Qualitative data from the open-ended, structured interview questions regarding perceptions of telehealth prior to and following the COVID-19 pandemic were provided. These responses were then analyzed, and in-vivo code assigned for every line to retain each unique response. Most responses were short (1–3 sentences in length). These codes were further analyzed to identify emerging themes.
Results
A total of 202 pediatric physical therapists participated in this study. After removing incomplete surveys from the data set, a total of 165 completed surveys were included in the analysis. The largest number of participants had 20 or more years of clinical experience. The second largest represented group had 0–3 years of clinical experience (Figure 1). The majority of participants reported their areas of pediatric practice as either 1) outpatient pediatric PT; 2) early intervention; or 3) school-based practice (Figure 2). When asked about their previous training or prior education on telehealth, 97% of therapists surveyed reported they had no prior training related to provision of telehealth therapy services prior to COVID-19. Likewise, 97% of therapists stated that they had not practiced telehealth prior to COVID-19.
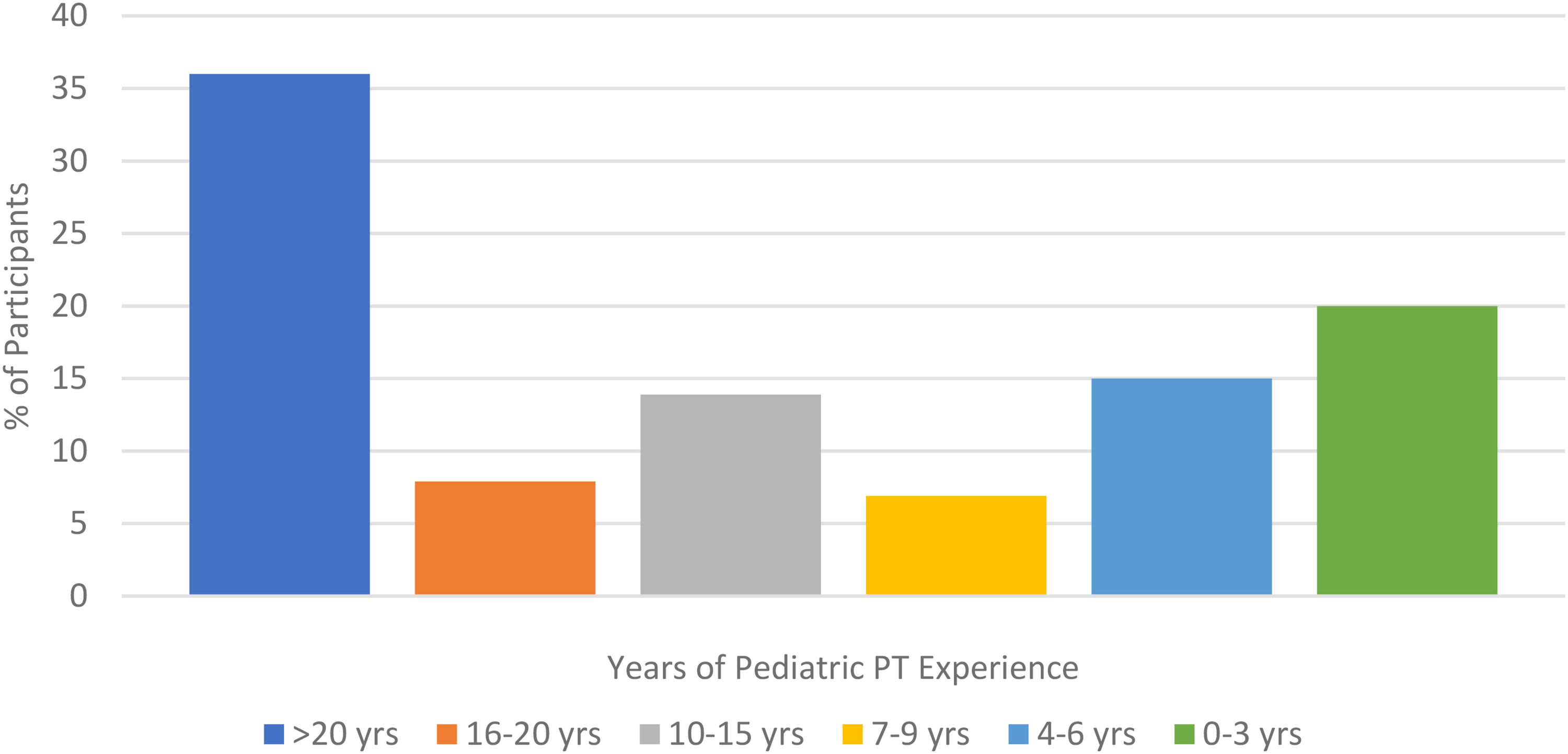
Demographic data, years (yrs) of pediatric physical therapy (PT) experience.
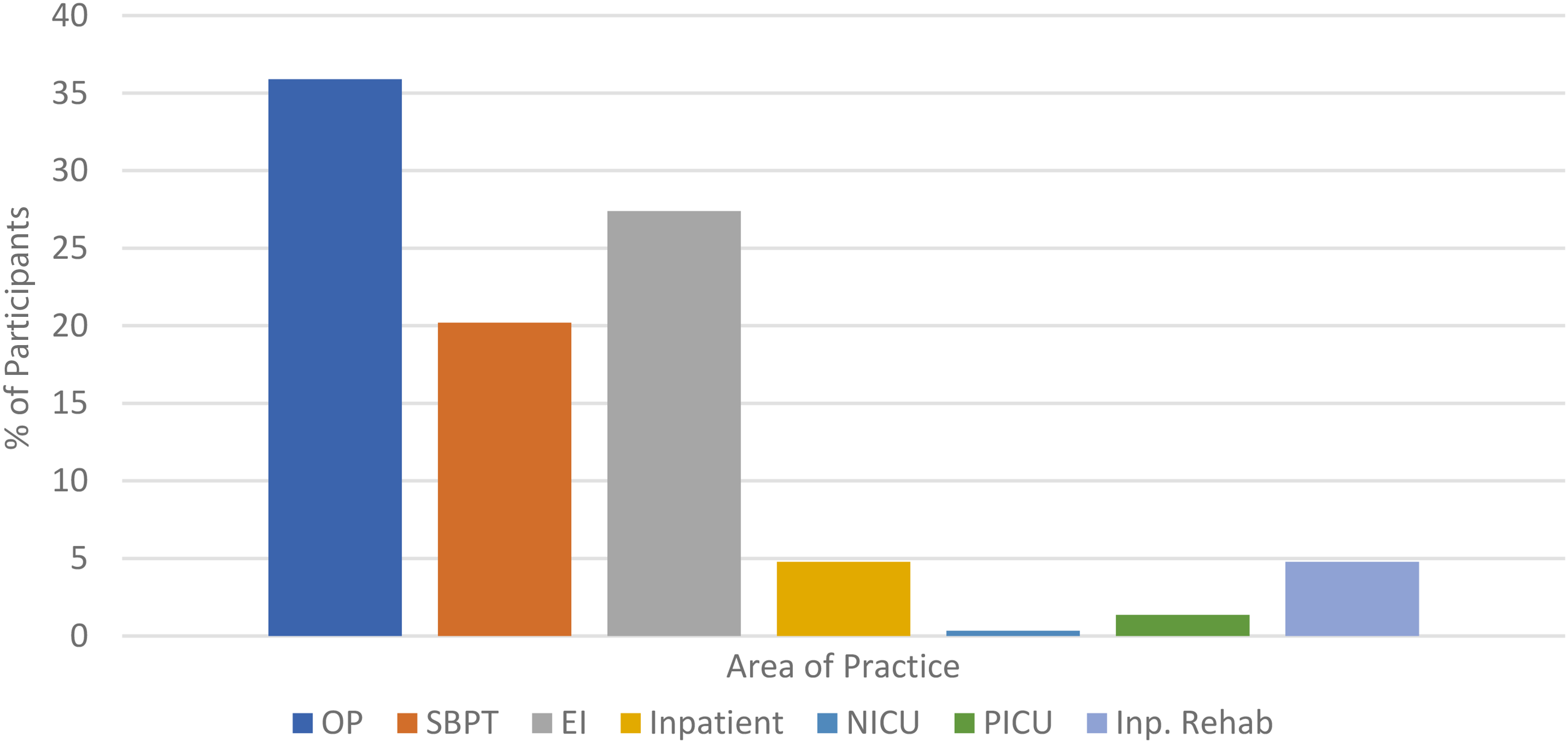
Demographic data, area of practice. OP: Outpatient, SBPT: School Based Physical Therapy, EI: Early Intervention, NICU: Neonatal Intensive Care Unit, PICU: Pediatric Intensive Care Unit, Inp. Rehab: Inpatient Rehabilitation.
Participants were then asked a series of questions regarding their level of comfort with providing telehealth services. Therapists were asked to recall their perceptions of telehealth prior to the COVID-19 pandemic as well as indicate their level of comfort following provision of these services during the pandemic. Twenty-nine percent rated their pre-pandemic perception of providing telehealth services as “somewhat negative,” and 35% as “very negative”. After utilizing a telehealth platform, 48% of therapists reported their perception of telehealth as “somewhat positive,” and 18% as “very positive”.
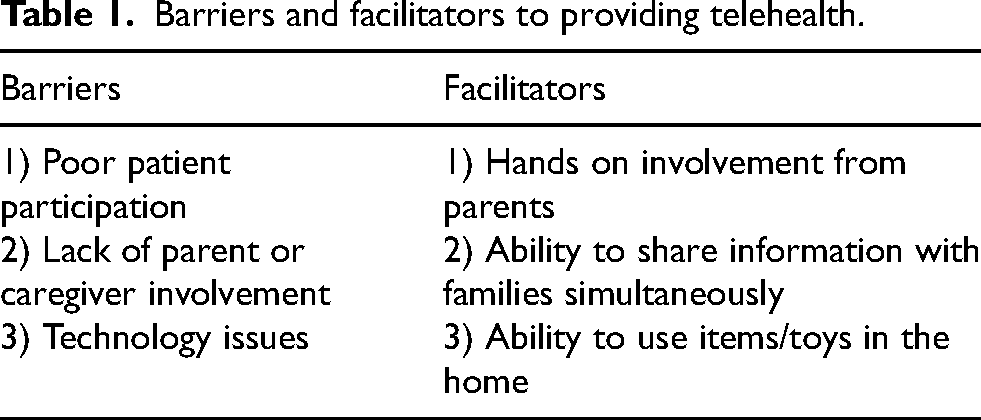
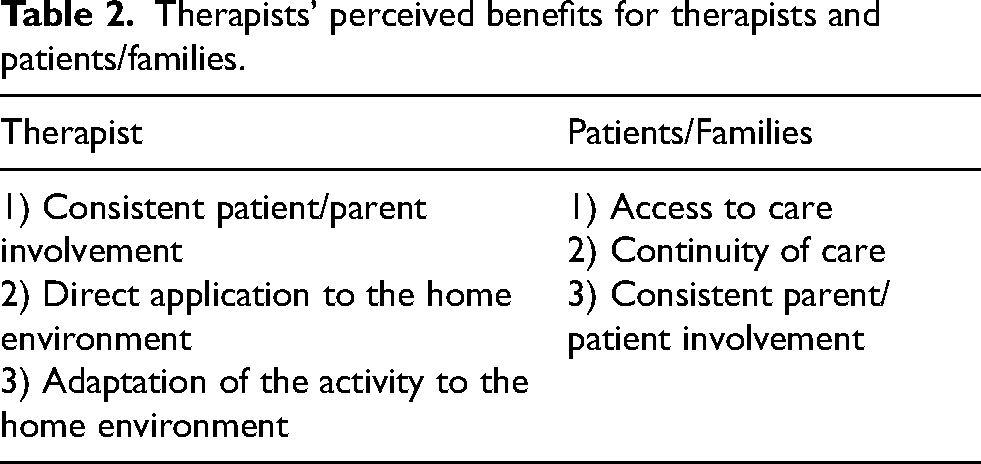
Out of a drop-down list (10 choices for each category) of possible facilitators and barriers, three main facilitators and barriers emerged (Table 1). Themes emerged of therapists’ perceived benefits for patients and families. (Table 2).
Barriers and facilitators to providing telehealth.
Therapists’ perceived benefits for therapists and patients/families.
For the question regarding perceptions of telehealth prior to COVID-19, three main themes emerged (Table 3). For the question regarding perceptions of telehealth services following the COVID-19 pandemic, there were also three themes (Table 4).
Question 1: based on your response above, please further describe your perceptions of telehealth prior to COVID-19.
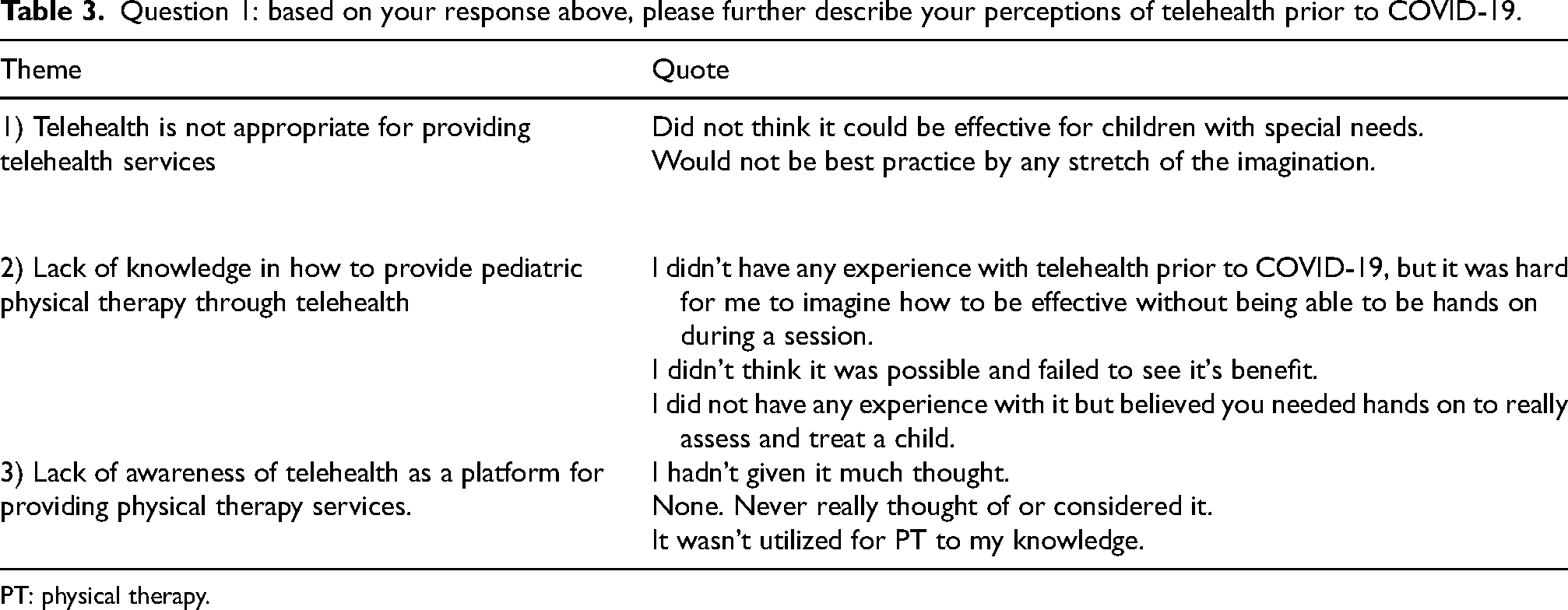
PT: physical therapy.
Question 2: based on your response above, please further describe your perceptions since implementing telehealth due to COVID-19.
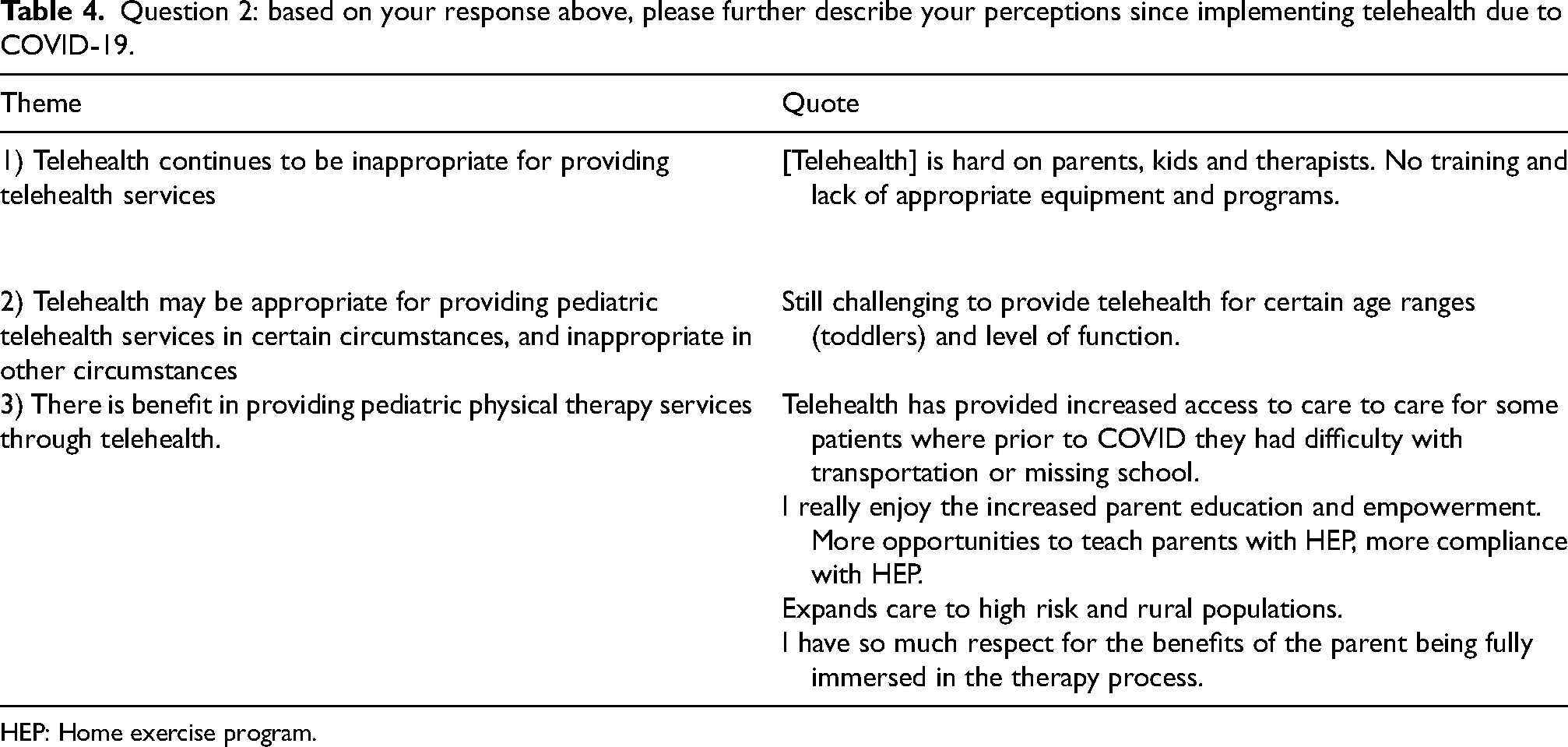
HEP: Home exercise program.
The survey also asked therapists to provide recommendations for education or resources.
Discussion
The mixed methods approach utilized in this study allowed for a deeper understanding of pediatric physical therapists’ perceptions of using telehealth for providing PT services. Both the quantitative and qualitative data show that greater numbers of therapists had positive perceptions of telehealth after the pandemic compared to before. This survey noted that prior to the COVID-19 pandemic, 64% of the respondents had a negative perception of telehealth. Consistent with findings in other recent studies,10,11 following implementation of telehealth during the COVID-19 pandemic, 66% of respondents reported a “somewhat” to “very” positive perception of telehealth.
This study also addressed their perceived barriers and facilitators to providing telehealth services and perceptions of the perceived barriers for both the child and the family. Participants in this study noted lack of participation as well as socioeconomic, technological and infrastructural barriers. Specifically, therapists noted that a lack of parent or patient participation was a barrier to a successful telehealth session for both the therapist and the patient and family. Parent involvement within their child's therapy sessions, specifically in goal writing, developing home exercise plans collaboratively with the physical therapist and being present during the intervention, has been linked with positive outcomes.13,14 Pediatric PT utilizes a service delivery model that relies on collaboration and family-centered care.
14
The telehealth platform reflects this tenet, as it requires greater parent involvement, wherein the therapist must coach the parent through therapeutic interventions during a session, resulting in direct parent involvement. As one participant noted: “I have so much respect for the benefits of the parent being fully immersed in the therapy process. I think TeleTherapy is beneficial when the family is motivated to be engaged in it.” (Participant 42)
Without adequate parent or child involvement, therapists noted the effectiveness of the therapy was lost. This finding was consistent with a recent study by Hall et al., in which parent or caregiver engagement in a session was reported as “the most important feature necessary for effective telehealth.” 15 Therapists also noted a family's lack of access to the internet or appropriate technology was a barrier to access and participation: “…I also work predominately in a low socioeconomic area and there is a lack of tools/resources for the parents to utilize with their children during sessions” (Participant 178). For another participant, telehealth showed them health inequities amongst their patients: “Inequities have been vastly exposed” (Participant 111). This finding was supported in a recent qualitative study, where emerging themes indicated that access to appropriate technology was another important factor to conducting an effective PT telehealth session. 16 Lack of training on successfully implementing telehealth for therapists was noted. Respondents indicated that telehealth was still not appropriate for pediatric populations. They cited barriers and lack of training as complicating factors for success, which were different from their initial responses (Table 4).
Responses to the open-ended questions allowed for a richer understanding of the respondents’ perceptions of telehealth before and after its implementation. Themes regarding perceptions of telehealth prior to the COVID-19 pandemic were largely negative and indicated that many respondents felt that telehealth would be inappropriate for providing pediatric PT services. Therapists also stated that they had no idea how to translate their skills through a telehealth platform (Table 3). Following implementation of telehealth during the COVID-19 pandemic, perceptions of telehealth as a platform for delivering pediatric PT services shifted from negative to positive: “It certainly took practice to feel competent with virtual services, and certainly not every family is ready for this type of practice, but I honestly feel like embracing a coaching model has enhanced my practice both virtually and in-person. I am still working to get by-in from some families, and still working to get by-in [sic] from my co-workers, but I believe virtual appointments can be very meaningful and beneficial for many of my patients.” (Participant 155) “Telehealth has allowed me to continue to positively impact the families with which I work. I had to improve my description of techniques and be creative to find ways to help families understand, and for about 60–70% of my families, it has worked well!” (Participant 182)
This study was a step in understanding telehealth's potential as a method for service delivery, by analyzing pediatric physical therapists’ perceptions following implementation during the COVID-19 pandemic. Therapists’ responses to the provided questions not only pointed to facilitators and barriers to providing telehealth, but also the perceived benefits of telehealth for therapists and the families they served. Overall, pediatric physical therapists did have a positive perception of telehealth following its implementation during the COVID-19 pandemic. However, like other recent studies have suggested, there were facilitators and barriers to providing an effective telehealth session which need to be further addressed and explored. The benefits of utilizing telehealth for service delivery that respondents identified were 1) direct application of therapeutic activities to the environment, 2) direct parent and patient involvement, and 3) adaptation of activities to the environment. Teneforde et al. and Bican et al. both noted similar findings in their qualitative studies, specifically that families reported similar benefits such as direct application to the environment and parent training through hands-on involvement.9,17 Another recent study by Fergus et al. in 2021 further supported this idea of perceived benefit of telehealth, specifically the benefit of direct parent involvement. In their qualitative study, themes of parent empowerment were reported following parent's participation with their child in a PT telehealth session. 18 In a qualitative study by Wittmeier et al. in 2022, one of the themes that emerged from interviews with pediatric physical therapists regarding the use of telehealth was congruent with findings in this study, specifically with observation and direct application of activities to the home environment. 19
Based on findings in similar studies and responses in this study, telehealth may have implications for patients in rural or underserved communities where transportation or other resources may be limited. Respondents noted this in their open-ended responses: “I thought it was a valuable option for clients who did not have access to specialized care in their region.” (P174) Additionally, there may be implications for improved access and continuity of care through telehealth, 9 and greater opportunity for therapists to visualize the home environment for direct application of therapeutic activities. 17
Currently, there is a gap in the literature describing telehealth utilization for pediatric PT services in the post COVID-19 era. In a study by Hall et al., qualitative themes pointed to the use of a hybrid model of both telehealth and in-person services following the end of the pandemic. 20 However, this data was collected during the height of the COVID-19 pandemic in 2020, when pediatric physical therapists were asked to reflect on benefits and concerns with continued use of telehealth. Current perspectives on the use of telehealth in pediatric PT were not represented. Research is further warranted to explore the possible or continued use of telehealth for pediatric PT services now that restrictions have been lifted.
There were several limitations in this study. First, there was a small sample size, predominantly capturing physical therapists from the southern and northeastern US. Second, there was potential for bias as respondents were members of the APTA, had sufficient access to online resources, and were interested in the topic. Parents were not sampled in this study; rather pediatric therapists were asked to reflect on perceived facilitators and barriers to care on behalf of their patients and families. And finally, for the qualitative portion of this study and triangulation of the data, specific member-checking was difficult due to factors such as the anonymity of the survey. Therefore, results cannot be generalized for all licensed pediatric physical therapists in the US.
Conclusion
Overall, pre-COVID-19 perceptions of telehealth by pediatric physical therapists were negative. However, after implementing telehealth services during COVID-19, a majority of these same therapists indicated their perceptions were somewhat or very positive. These results mirror similar studies published recently, indicating promising applications for the use of telehealth to deliver pediatric therapy services. However, future studies need to address the potential educational, socioeconomic, infrastructural, or technological barriers that may prevent access to telehealth services for families.
Supplemental Material
sj-docx-1-prm-10.1177_18758894251315639 - Supplemental material for Pediatric physical therapy during a pandemic: Assessing perceptions of providing services through telehealth
Supplemental material, sj-docx-1-prm-10.1177_18758894251315639 for Pediatric physical therapy during a pandemic: Assessing perceptions of providing services through telehealth by Katelyn McNamara and Deborah E Thorpe in Journal of Pediatric Rehabilitation Medicine
Footnotes
Acknowledgements
At the time this research was conducted Katelyn McNamara was the 2020–2021 UNC Pediatric Physical Therapy Resident at the University of North Carolina Chapel Hill. The authors would like to acknowledge and thank the UNC Pediatric Physical Therapy Residency program for the opportunity to initiate and perform this study.
Ethical considerations
This study was conducted with approval and in accordance with the IRB through UNC Chapel Hill. The IRB number associated with this study is IRB# 20-2486.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
