Abstract
Neurological manifestations related to SARS-CoV-2 infection in adults have been largely reported since the beginning of the pandemic. Subsequent large-scale studies involving children confirmed the occurrence of neurological symptoms associated with SARS-CoV-2 infection also among paediatric patients, especially in the context of paediatric inflammatory multisystem syndrome temporally associated with COVID-19 (PIMS-TS). At this regard, we report the challenging case of a 10-month-old baby with PIMS-TS complicated by acute cerebral oedema successfully treated with intravenous immunoglobulins, corticosteroids and anakinra. Our results, combined with the evidence of larger case series suggest that higher inflammatory burden is more frequent in patients with neuro PIMS-TS. As regards neuroimaging, neuroimmune disorders are found to be more common during acute COVID-19, MERS is more frequent during PIMS-TS. Distinct immune mechanisms may underlie these different types of neurological involvement, which are yet to be understood. Further studies are required to better define the physiopathology of neuro PIMS-TS and its possible therapeutical implications.
Introduction
Since the outbreak of coronavirus disease 2019 (COVID-19) pandemic, it was clear that children had an asymptomatic or mild infection course, with minimal hospitalization rate and mortality.1,2
However, starting from April 2020, several countries reported on children with an acute critical condition subsequent to severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) infection. This new clinical entity was quite similar to other known inflammatory diseases [i.e. Kawasaki disease (KD), septic shock and toxic shock syndrome],3,4 although with peculiar findings. This condition was labelled paediatric inflammatory multisystem syndrome temporally associated with COVID-19 (PIMS-TS) by the Royal College of Paediatrics and Child Health. 5 Subsequently, the Centers for Disease Control and Prevention (CDC) and the World Health Organization (WHO) referred to this condition as Multisystem inflammatory syndrome in children (MIS-C).6,7
Neurological manifestations related to SARS-CoV-2 infection in adults have been largely reported since the beginning of the pandemic. 8 Subsequent large-scale studies involving children confirmed the occurrence of neurological symptoms associated to SARS-CoV-2 infection also among paediatric patients, especially in the context of PIMS-TS. 9
LaRovere et al. 10 reported that 22% of 1695 children with acute COVID-19 or PIMS-TS in the United States presented a neurological involvement. PIMS-TS patients did not show a higher rate of neurological involvement (35% versus 37%) or life-threatening events (47% versus 53%) than acute COVID-19 patients. Transient symptoms (88%) such as fatigue, confusion, headache, loss of smell or taste and seizures were the most frequently reported (88%). Therefore, a minority of patients (12%) experienced life-threatening conditions: severe encephalopathy (34.9%), ischemic or haemorrhagic stroke (27.9%), acute central nervous system infection or acute disseminated encephalomyelitis (ADEM; 18.6%), acute fulminant cerebral oedema (9.3%) and Guillain–Barré syndrome (9.3%). These symptoms were more frequent in patients with underlying neurologic disorders and an unfavourable outcome, including death or neurological disability at discharge, was observed in 65% of patients with severe manifestations.
A further prospective cohort study conducted in the United Kingdom involving 1334 patients 11 detected a much lower rate of neurological manifestations (3.8%) among children with acute COVID-19 and PIMS-TS. In the PIMS-TS subgroup (25 patients) encephalopathy (88%), peripheral nervous system involvement (40%), headache or meningism (40%) behavioural changes (36%), hallucinations (24%) and seizures (16%) were observed. Abnormal neuroimaging consistent with mild encephalopathy with reversible splenial lesion (MERS) was detected in 28% of patients. Neuroimmune disorders were more frequently observed in the COVID-19 group (48%) compared with the PIMS-TS one (<1%).
At this regard, we report the challenging case of a 10-month-old baby with PIMS-TS complicated by acute cerebral oedema. Furthermore, we performed a narrative literature review of PIMS-TS cases with neurological involvement, in order to characterize the spectrum of neurological manifestations of this critical condition, to establish the temporal association between PIMS-TS and neurological symptoms as well as to understand the potential underlying mechanisms of neurological involvement during PIMS-TS clinical course.
Materials and methods
A written informed consent for patients’ information and images to be published and written consent to treatment were provided by the legally authorized representatives. CARE guidelines were followed for the case report drafting. 12
As regards the narrative review of PIMS-TS cases with neurological involvement, the search strategy was carried out in PubMed/Medline and Embase databases using in all fields the key terms [ ‘Paediatric inflammatory multisystem syndrome temporally associated with COVID-19’ OR ‘PIMS-TS’ OR ‘Multisystem Inflammatory Syndrome in Children Associated With SARS-CoV-2’ OR ‘MIS-C’] AND [ ‘Neurological’ AND ‘Nervous’ AND ‘encephalopathy’ AND ‘seizures’ AND ‘papilledema’ AND ‘stroke’ AND ‘headache’ AND ‘hallucination’ AND ‘intracranial hypertension’]. The review includes retrospective cohort, prospective cohort studies, case series and case reports. Only articles published in English were included. Studies reporting poor or not-extractable data were excluded, as well as papers published before May 2020 (first PIMS-TS reported case). Double-reported patients were excluded from the total account.
Case report
A previously healthy 10-month-old African infant developed high-grade fever and emesis with a subsequent widespread urticarial rash and bilateral non-secretive conjunctivitis.
He was admitted to our tertiary care hospital after 4 days of persistent fever. At the physical examination, the infant presented marked irritability with tense, wide and bulging anterior fontanelle, shallow breathing and a widespread macular erythematous rash on trunk and limbs. Brain ultrasounds did not detect intracranial bleeding or meningitis signs. Blood tests evidenced a remarkable increase of inflammatory markers [C-reactive protein (CRP) 32.08 mg/dl, procalcitonin (PCT) 97.7 ng/ml], neutrophilic leucocytosis, NT-pro-BNP (92,230 pg/ml) and D-dimer (2547 ug/l FEU) elevation, and a high ferritin value (810 ng/ml). SARS-CoV-2 IgG antibodies were positive, while RT-PCR for SARS-CoV-2 on nasopharyngeal swab was negative. Echocardiography evidenced slight coronary arteries dilatation and hyperkinetic left ventricle, with normal systolic function. Empiric antibiotic and antiviral treatment was started. Clinical and laboratory findings suggested a PIMS-TS diagnosis. Therefore, a single 2 g/kg dose of intravenous immunoglobulin (IVIG) was administered, followed by intravenous continuous infusion of anakinra (10 mg/kg qd). Moreover, a prophylactic antithrombotic therapy with enoxaparine at 100 UI/kg qd was started because of D-dimer elevation and initial coronary arteries dilatation, according to American College of Rheumatology clinical guidelines for PIMS-TS. 13
Despite this prompt intervention, 24 h after admission, a neurological deterioration was observed with drowsiness alternating with extreme irritability. Brain computed tomography (CT) reported an initial cerebral oedema, with meningeal and cerebral herniation from the anterior fontanelle. The patient continued to get worse and severe hypotension rapidly occurred requiring the admission to the intensive care unit (ICU), hemodynamic support with amines and mechanical ventilation. In order to treat cerebral oedema, dexamethasone and mannitol were administered intravenously. Subsequent cardiological evaluation described increased coronary arteries ectasia.
On day 7 from admission, a new fever rise, and a leucocytosis rebound occurred during the slow tapering of anakinra, therefore, the immunomodulatory regimen was re-intensified. A second 2 g/kg dose of IVIG followed by three boluses of methylprednisolone was administered.
After the maximization of treatment, patient’s clinical conditions gradually improved. He was weaned from ventilation, sedation and vasoactive support. Antibiotics and antiviral therapy were discontinued since all infectious tests resulted negative (aerobic and anaerobic bacteria and fungal blood cultures; Cytomegalovirus, Epstein-Barr virus, Adenovirus, Neisseria meningitidis, Streptococcus pneumoniae, Escherichia coli, Klebsiella pneumoniae, Listeria monocytogenes, Streptococcus agalactiae, Haemophilus influentiae, Human Herpesvirus-6, Human Herpesvirus-7, Enterovirus, Herpes Simplex virus-1, Herpes Simplex virus-2, Parvovirus on blood samples by real-time polymerase chain reaction (RT-PCR); QuantiFERON for the detection of Mycobacterium tuberculosis).
On day 10, the boy was back at his neurological baseline, with a normal anterior fontanelle. He was persistently afebrile, and the rash completely disappeared. Inflammation indexes slowly decreased, and the patient was moved to the paediatric ward. Dexamethasone regimen was suspended. Two weeks after the admission, the baby presented peeling of the extremities and remarkable thrombocytosis. Right coronary artery (RCA) demonstrated a residual deep aneurismatic remodelling (+5.5 SD). Anti-platelet therapy was started, while enoxaparin was discontinued. Anakinra was slowly tapered and shifted to subcutaneous administration, with no fever relapse.
Brain magnetic resonance imaging (MRI), performed on day 14, showed periventricular hyperintensities without restricted diffusion (Figure 1). Slight cerebral and cerebellar trophism reduction was observed, with mild peri encephalic subarachnoid spaces enlargement. Angiography, venography and post-contrast scan were normal.

Radiological findings in our neuro PIMS-TS patient: (a) brain CT reporting cerebral oedema, with meningeal and cerebral herniation from the anterior fontanelle, (b) brain MRI showing periventricular hyperintensities without restricted diffusion, (c) and (d) left and right coronary artery ectasia, respectively.
Coronary arteries dilatation regressed at its normal size (proximal RCA: +2.2 DS; common trunk of left coronary artery +2 DS; proximal anterior interventricular coronary artery: +1.32 DS; circumflex branch of left coronary artery +1.2 DS) within 2 weeks after its peak (Figure 2). As regards neurological status, the infant presented a regular development without sequelae.

Timeline of patient course.
Results
We retrospectively reviewed the clinical history of 75 patients with neuro PIMS-TS reported in literature. We collected epidemiological, clinical, therapeutical, laboratory and instrumental data (Table 1).
Neuro PIMS-TS previously reported cases.
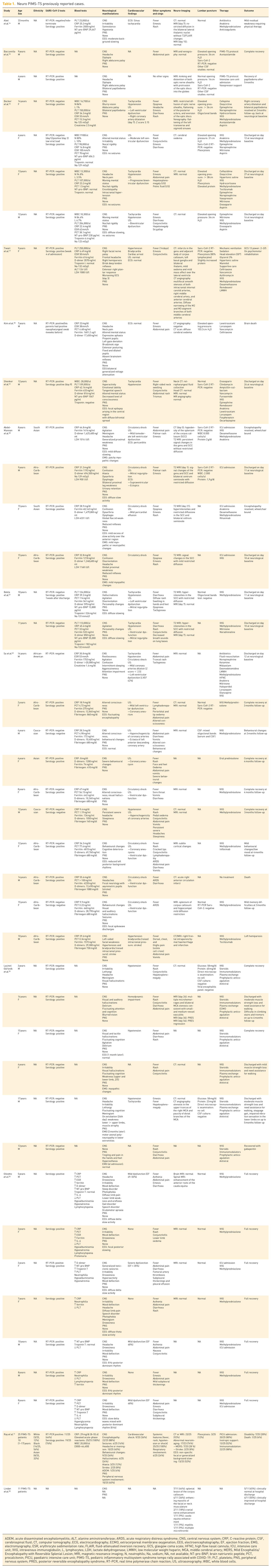
ADEM, acute disseminated encephalomyelitis; ALT, alanine aminotransferase; ARDS, acute respiratory distress syndrome; CNS, central nervous system; CRP, C-reactive protein; CSF, cerebrospinal fluid; CT, computer tomography; ECG, electrocardiography; ECMO, extracorporeal membrane oxygenation; EEG, electroencephalography; EF, ejection fraction; EMG, electromyography; ESR, erythrocyte sedimentation rate; FLAIR, fluid-attenuated inversion recovery; GCS, glasgow coma scale; HFNC, high flow nasal cannula; ICU, intensive care unit; IVIG, intravenous immunoglobulin; L, lymphocytes; LDH, lactate dehydrogenase; LMWH, low molecular weight heparin; MCA, middle cerebral artery; MERS, Mild Encephalitis/Encephalopathy with Reversible Splenial Lesion; MRI, magnetic resonance imaging; N, neutrophils; Na, sodium; NA, not available; NT-pro-BNP, brain natriuretic peptide; PCT, procalcitonin; PICU, paediatric intensive care unit; PIMS-TS, pediatric inflammatory multisystem syndrome tempo rally associated with COVID-19; PLT, platelets; PNS, peripheral nervous system; PRES, posterior reversible encephalopathy syndrome; RT-PCR, real time polymerase chain reaction; US, ultrasonography; WBC, white blood cells.
Epidemiology
51.6% of patients (33/64) were male. The median age was 9 years. Among those with known ethnicity, the majority (59%, 23/39) were African descent. 28.2% was Asian (11/39); only 12.8% was Caucasian (5/39).
SARS-CoV-2 tests
85% of the patients (51/60) who underwent SARS-CoV-2 serology testing resulted positive, while RT-PCR on nasopharyngeal swab resulted positive in 42.6% of patients (26/61).
Signs and symptoms
Among neuro-PIMS-TS reported patients, fever was the most common finding (97.4%, 38/39). Vomiting (53.8%, 23/39), abdominal pain (53.8%, 21/39), and diarrhoea (41%, 16/39) were also frequent clinical signs, together with skin rash (53.8%, 21/39) and conjunctivitis (33.3%, 13/39). Dyspnoea was reported in 20.5% of these patients (8/39).
Blood tests
Among neuro PIMS-TS patients reported in case reports and case series, 75% (18/24) showed a CRP value higher than 20 mg/dl; a CRP value higher than 30 mg/dl was detected in 45.8% of cases (11/24). 46.6% (7/15) showed a PCT value higher than 30 ng/ml.
Ferritin levels resulted higher than 1000 ng/ml in 50% of these patients (10/20); a D-dimer elevation above 2500 ng/ml was reported in 73.7% of them (14/19).
NT-pro BNP was not routinely performed in neuro PIMS-TS children; 26.9% of cases reported a NT-pro BNP determination during the clinical course with a median value of 13,358 pg/ml.
Neurological manifestations
Encephalopathy was the most common neurological finding, involving 82.8% of neuro PIMS-TS patients (53/64). 43.8% of patients (28/64) experienced headache and/or meningism. Behavioural changes were described in 37.5% (24/64) and hallucinations in 21.9% of cases (14/64). Seizures were documented in 9.4% of patients (6/64). 4 stroke episodes (9.4%, 6/64) were also reported.
Signs of intracranial hypertension (abducens palsy 3/39, papilledema 2/39) were described in a minority of cases. Proximal and/or global weakness was sometimes reported, involving 18% of children (7/39). However, Ray et al. reported a higher rate of peripheral nervous system involvement among their patients (40%, 10/25).
Cardiac manifestations
Among neuro PIMS-TS patients, 30% (9/30) presented with tachycardia and 52.7% (29/55) with hypotension and/or shock. Indirect cardiovascular signs of intracranial hypertension (hypertension and bradycardia) were reported in two cases.
Coronary arteries dilatation and/or aneurysm were described in 25% of patients (6/24); ventricular dysfunction was reported in 48.6% of cases (18/37).
Neuro-imaging findings
Signal changes in the genu and/or splenium of the corpus callosum (consistent with MERS) were the most common imaging findings among all neuro PIMS-TS patients, accounting on 30.4% of cases (21/69). 11.6% of them presented with radiological signs of stroke (8/69).
Among neuro PIMS-TS patients reported in case reports and case series, normal brain imaging was quite frequent, being documented in 42.4% of patients (14/33). Cerebral oedema and anomalies of optic nerves were both described in 2 cases. Lindan et al. also reported two cases of cranial nerve enhancement (18.2%, 2/11) among their patients; myositis of the facial or neck musculature was a common finding, involving 36.4% of children (4/11).
Treatment
A first-line immunomodulatory treatment with IVIG and methylprednisolone was received by 84.6% (33/39) of neuro PIMS-TS patients. 23.1% of them (6/26) also required the recourse to anakinra. Antibiotics were administered in 18% of patients (7/39). Vasoactive support was necessary in 34.3% of cases (9/26). 30.8% of patients (12/39) underwent anticoagulant treatment, while aspirin was administered in 10.3% (4/39).
Ray et al. reported a high rate of paediatric intensive care unit admission (80%, 20/25), with inotropic support in 52% of cases (13/25) and immunomodulatory treatment in 88% of patients (22/25).
Outcomes
A complete recovery without sequelae was reported in most cases (64%, 48/75). However, a variable degree of residual disability was observed, involving 32% of patients (24/75) and ranging from hemiparesis and wheelchair bounding to mild behavioural changes. Death was a rare adverse event (4%, 3/62).
Discussion
To the best of our knowledge, we reported the youngest PIMS-TS patient presenting a neurological involvement. Four case reports, five case series, one prospective cohort study and one multicentre study have previously described neuro PIMS-TS patients, recording a total amount of 75 children, with a median age of 9 years (Table 1).
As regards ethnicity, our infant was of African descent. It is well known that most of the PIMS-TS patients are African/Afro-Caribbean, Hispanic and South Asian, mainly in Western countries. 26 Only few cases were described in East Asia, probably because of the lack of knowledge of this new clinical entity at the beginning of pandemic. 26 African ancestry was also one of the most represented in neuro PIMS-TS.
Our patient presented a positive SARS-CoV-2 serology, with negative RT-PCR on nasopharyngeal swab. LaRovere et al. described a 22% of patients reporting neurological symptoms between COVID-19 and PIMS-TS patients and a concomitant positivity of both serology and RT-PCR was often reported10,11 making difficult to distinguish between acute hyperinflammatory COVID-19 and PIMS-TS. Patients with and without neurological involvement presented a similar rate of PIMS-TS diagnosis and life-threatening neurologic events did not show a predominance among PIMS-TS cases.
Considering clinical features, our patient presented high-grade fever, emesis and widespread skin rash as reported in previous cases.
In this group of patients, a severe neurological involvement was associated to a remarkable inflammatory state,10,11 similarly to KD patients. 27 Our infant presented with acute cerebral oedema and deep increase of inflammatory markers. A CRP value >30 mg/dl, a PCT value >30 ng/ml and a ferritin level >1000 ng/ml were observed in about half of the reported neuro PIMS-TS cases.
Our infant presented with wide, tense and bulging anterior fontanelle, with a rapid subsequent neurological impairment and a deep increase of NT-pro BNP (92,230 pg/ml) at the clinical onset, without any sign of myocardial dysfunction. NT-pro BNP represents a marker of left ventricular dysfunction in heart failure patients since it regulates systemic fluid volume through vasodilatation and natriuresis. 28 However, the wide distribution of BNP receptors in the brain may suggest a novel pathway between heart and brain and a potential additional role for NT-pro BNP in the development of cerebral oedema.29,30
As regards the pathogenesis of the neurological involvement observed in our case and in the most of the neuro-PIMS-TS patients, it is reasonable to suppose that is due to an immune-mediated pathophysiological mechanism triggered by previous SARS-CoV-2 infection rather than a direct viral invasion. This hypothesis is supported by the fact that the neurological symptoms occurred during a post-infectious multisystem inflammatory condition. Moreover, cytopathological evaluation of cerebrospinal fluid samples of previous neuro-PIMS-TS cases were negative for SARS-CoV-2 RNA by RT-PCR and reported increased numbers of lymphocytes and macrophages suggesting that the production of cytokines induced by the inflammatory response is responsible of the neurological manifestations. This hypothesis is also supported by the excellent response to immunomodulatory treatment for neurological complications in this group of patients.23,24
Encephalopathy, headache and/or meningism and behavioural changes (33.3%) were the most reported symptoms in neuro PIMS-TS patients. Signs of intracranial hypertension (abducens nerve palsy, papilledema) and cerebral oedema were observed in a minority of cases.
A clinical hallmark was the concomitant presence of myocardial disfunction. Cardiovascular impairment frequently coexists with neurological symptoms since hypotension and/or shock and ventricular dysfunction were frequently observed. Coronary arteries ectasia and/or aneurysm were also reported even if typically transient, usually occurring at the onset of fever and rarely progressing to aneurysms.31–33
As regards neuroimaging, a non-specific periventricular hyperintensities and a slight cerebral and cerebellar trophism reduction was observed in our patient. According to previous data, MERS is a common finding in neuro PIMS-TS patients. 11 MERS is a distinct radiological entity characterized by hyperintensities of the genu and/or the splenium of corpus callosum on MRI T2-weighted, fluid-attenuated inversion recovery and diffusion-weighted images. 34 MERS may have different causes; primarily viral infections as most frequent triggers, 34 although its exact pathophysiology is still unknown. The most accredited hypothesis is that pro-inflammatory cytokines lead to glutamate release and oxidative stress in neurons, resulting in cytotoxic oedema. 34 MERS cases following SARS-CoV-2 infection have been reported. 35 Similarly, anecdotal cases of KD-associated MERS have reported,25,36 strengthening the hypothesis that MERS may be a consequence of systemic hyper-inflammation.
Lindan et al. 25 collected 38 cases of neuroimaging abnormalities in COVID-19 and PIMS-TS children. In the acute COVID-19 subgroup, 50% of patients presented a neuroimmune disorder (ADEM-like and neuritis); 33.3% had fulminant co-infections (tuberculosis, chickenpox, bacterial sepsis) and rapidly died; one patient (8.3%) showed an aggressive necrotizing myelitis; a 27-weeks pregnant adolescent girl presented with posterior reversible encephalopathy syndrome and occipital infarction. In the PIMS-TS subgroup, 64% of patients presented splenial lesions; two patients (18%) had cranial nerve enhancement; one patient (9%) reported cauda equina enhancement and myelitis was observed in one case (9%). Four patients (36%) had enhancing myositis of the facial and neck muscles; one patient (9%) reported multiple brain microthrombi.
These results suggest that neuroimmune disorders (i.e. ADEM-like changes, neuritis, Guillain Barrè syndrome) may be more frequently observed during acute COVID-19 and neurological symptoms during COVID-19 and PIMS-TS may be caused by different immune mechanisms.
Focusing on treatment, our patient presented with a refractory disease and maximal therapy was performed, including IVIG, steroids and anakinra. Considering previous data, IVIG and methylprednisolone were the most common adopted treatment. Anakinra was administered in 23% of these patients, mostly in case of first-line treatment-resistant cases.
As regards thromboprophylaxis, our patient was treated with enoxaparine, while in the subacute phase anti-platelet regimen was started. Anticoagulants were used in 23% of neuro-PIMS-TS patients, while aspirin was used in 15.3% of cases.
Despite being a life-threatening condition with high rates of ICU admission,10,11 PIMS-TS patients, if promptly treated, report a complete recovery. As regards neuro PIMS-TS subgroup, a complete recovery was observed in most of the patients although a significant rate of disability (32%) was reported, thus underlying the importance of a timely diagnosis and treatment.
In conclusion, neurological involvement may be frequent in PIMS-TS patients as expression of the hyperinflammatory state. Symptoms are acute and reversible in most of the patients with a favourable response to immunomodulatory treatment. Available data suggest that paediatric patients experience different types of neurological involvement during acute COVID-19 and PIMS-TS. Further studies are needed to better characterize these different neurological manifestations related to SARS-CoV-2 infection suggesting the opportunity of different patient-tailored therapeutical strategies.
