Abstract
Increased reactive oxygen species production and oxidative stress have been implicated in the pathogenesis of numerous neurodegenerative conditions including among others Alzheimer’s disease, Parkinson’s disease, Huntington’s disease, Friedrich’s ataxia, multiple sclerosis, and stroke. The endogenous antioxidant response pathway protects cells from oxidative stress by increasing the expression of cytoprotective enzymes and is regulated by the transcription factor nuclear factor erythroid 2-related factor 2 (NRF2). In addition to regulating the expression of antioxidant genes, NRF2 has also been shown to exert anti-inflammatory effects and modulate both mitochondrial function and biogenesis. This is because mitochondrial dysfunction and neuroinflammation are features of many neurodegenerative diseases as well NRF2 has emerged as a promising therapeutic target. Here, we review evidence for a beneficial role of NRF2 in neurodegenerative conditions and the potential of specific NRF2 activators as therapeutic agents.
Introduction
Reactive oxygen species (ROS) serve as critical intracellular signaling molecules but in excess can cause oxidative stress and damage organelles and macromolecules, eventually leading to cell death (Zuo et al., 2015). Increased ROS production and oxidative stress have been implicated in the pathogenesis of numerous neurodegenerative conditions, including, among others, Alzheimer’s disease (AD; Behl, 2005), Parkinson’s disease (PD; Trist et al., 2019), Huntington’s disease (HD; Browne and Beal, 2006), Friedrich’s ataxia (Lupoli et al., 2018), multiple sclerosis (MS; Di Filippo et al., 2010), and stroke (Rodrigo et al., 2013). Aging is the primary risk factor for most neurodegenerative diseases, and oxidative stress is known to increase with aging. Although increased oxidative stress is the cumulative result of many factors including changes in tissue antioxidant status, increased mitochondrial dysfunction, and altered metal homeostasis, the majority of the excessive ROS are produced by the mitochondria (Buendia et al., 2016). The endogenous antioxidant response pathway protects cells from oxidative stress by increasing the expression of cytoprotective enzymes that can scavenge free radicals and reduce the risk of cellular damage caused by ROS (Itoh et al., 1997; Motohashi and Yamamoto, 2004; Buendia et al., 2016). The transcription factor nuclear factor erythroid 2-related factor 2 (NRF2, also called NFE2L2) regulates this pathway by binding to antioxidant response elements (AREs) in the promoters of antioxidant genes (Itoh et al., 1997; Motohashi and Yamamoto, 2004). These AREs are cis-acting enhancer sequences. Past studies identified a necessary ARE core sequence of RTGACnnnGC, but this sequence alone is insufficient to mediate induction and requires additional flanking nucleotides that can vary between different AREs (Wasserman and Fahl, 1997).
NRF2 is a member of the cap-n-collar family of basic leucine zipper proteins. NRF2 is normally bound in the cytosol to Kelch-Like ECH-Associated Protein 1 (KEAP1) that targets it for degradation by the proteasome. However, in the presence of electrophiles or oxidative stress, the nucleophilic cysteine sulfhydryl groups on KEAP1 are modified, resulting in an allosteric conformational change that diminishes KEAP-dependent degradation of NRF2 and allows the transcription factor to accumulate in the nucleus (Kobayashi et al., 2006). While this is the classical mode of NRF2 activation, other mechanisms, including phosphorylation, can also result in its dissociation from KEAP1 and increased nuclear localization (Huang et al., 2002; Chen et al., 2019; Xiao et al., 2019). Within the nucleus, NRF2 forms a heterodimer with small musculoaponeurotic Maf proteins and binds to ARE consensus sequence in the promoter of target genes (Esteras et al., 2016).
NRF2 is ubiquitously expressed (Moi et al., 1994) and in the brain is an important defense against toxic insults in both glial cells as well as neurons (Lee et al., 2003; Jakel et al., 2007; Chen et al., 2009; Vargas and Johnson, 2009). In addition to upregulating numerous antioxidant enzymes, NRF2 can also increase expression of anti-inflammatory mediators, Phase I and II drug-metabolizing enzymes as well as mitochondrial pathways (Nguyen et al., 2009; Sandberg et al., 2014; Dinkova-Kostova and Abramov, 2015; Buendia et al., 2016; Hayashi et al., 2017; Sivandzade et al., 2019).
Antioxidant Role of NRF2
Within the central nervous system, upregulation of NRF2 target genes, such as heme oxygenase-1 (HMOX1), glutathione S-transferase (GST), superoxide dismutase (SOD), catalase (CAT), NAD(P)H dehydrogenase (quinone) 1 (NQO1), and others, can make neurons more resistant to oxidative insults (Chen et al., 2000; Satoh et al., 2006; Giordano et al., 2007; Tanito et al., 2007; Lim et al., 2008).
Anti-Inflammatory Role of NRF2
Because of the cross talk that exists between antioxidant and anti-inflammatory pathways, many of the anti-inflammatory and mitochondrial actions of NRF2 have been considered secondary to its antioxidant effects. For example, the classical proinflammatory transcription factor NFkB is activated by oxidative stress that can be blocked by the NRF2-dependent induction of antioxidant target genes, and thus, the transcription of proinflammatory cytokines is decreased (Lee et al., 2009a; Bellezza et al., 2012). However, NRF2 has been shown to directly regulate the expression of anti-inflammatory mediators such as interleukin (IL)-17D, CD36, macrophage receptor with collagenous structure, and G protein-coupled receptor kinase (Thimmulappa et al., 2002; Ishii et al., 2004; Saddawi-Konefka et al., 2016). Moreover, NRF2 has recently been implicated in reducing the expression of the proinflammatory cytokines such as tumor necrosis factor (TNF)-α, IL-6, IL-8, and IL-1β in microglia, macrophages, monocytes, and astrocytes (Kobayashi et al., 2016; Quinti et al., 2017).
Mitochondrial Role of NRF2
A complex interplay also exists between mitochondrial function and antioxidant response. By inducing free-radical scavenging enzymes, NRF2 protects mitochondria from oxidative damage. NRF2 can also directly regulate mitochondrial biogenesis as well as function and by improving mitochondrial function diminishes overproduction of intracellular ROS. NRF2 activation affects the expression of many mitochondrial enzymes important for proper bioenergetic function including malic enzyme 1, isocitrate dehydrogenase 1, glucose-6-phosphate dehydrogenase, and 6-phosphogluconate-dehydrogenase (Morgan et al., 2013; Ku and Park, 2017). A role has also been described for NRF2 in maintaining mitochondrial integrity and regulating mitochondrial biogenesis. It has been reported that NRF2 activation protects mitochondria by opening the mitochondrial permeability transition pore (Lee et al., 2000; Greco and Fiskum, 2010; Greco et al., 2011) and that declining NRF2 signaling is associated with increased damage to mitochondrial DNA (mtDNA; Li et al., 2018). In addition, NRF2 activation modulates the expression of ATP synthase subunit α and NDUFA4, two components of the electron transport chain (Abdullah et al., 2012; Agyeman et al., 2012), and mice in which NRF2 has been deleted have lower mtDNA globally than wild-type (WT) mice (Zhang et al., 2013). In addition, NRF2 activation affects the expression of several regulators of mitochondrial biogenesis including Sirt1 (sirtuin 1), PPARγ (peroxisome proliferator-activated receptor γ), and Pgc1α (PPARγ coactivator 1α), considered to be the master regulator of biogenesis (Cho et al., 2010; Bellezza et al., 2012; Lai et al., 2014; Ping et al., 2015; Huang et al., 2017a; Song et al., 2018).
Role of NRF2 in Aging
NRF2 expression and activity are diminished in both aged mice and humans (Suh et al., 2004; Collins et al., 2009; Duan et al., 2009; Demirovic and Rattan, 2011; Cheng et al., 2012; Rahman et al., 2013). Because oxidative stress, inflammation, and mitochondrial dysfunction are all features of the aging brain and because aging is the primary risk factor for most neurodegenerative diseases, NRF2 has emerged as an attractive target for clinical intervention. In fact, the NRF2-activating compound dimethyl fumarate (DMF) is an existing FDA-approved therapy for use in MS. This review will primarily focus on the therapeutic potential of NRF2 activation in other neurodegenerative conditions.
NRF2 and MS
MS is a chronic inflammatory neurodegenerative disorder that currently affects more than 2.3 million people worldwide (Browne et al., 2014). Demyelination, astrocytosis, axonal degeneration, and sclerotic plaques are all features of the autoimmune response that occurs in the disease (Compston and Coles, 2008). Elevated levels of proinflammatory cytokines are seen in the cerebrospinal fluid (CSF) of MS patients (Khaibullin et al., 2017) as have increased levels of chemokines involved in B cell migration (Kalinowska-Lyszczarz et al., 2011). Large-scale gene expression studies using either peripheral blood monocytes or brain tissue from MS patients have also found altered expression of several genes involved in the activation of T and B cells (Ramanathan et al., 2001).
Oxidative stress and mitochondrial dysfunction are also prominent features of the disease. The activation of microglia and macrophages is a major contributor to the increased ROS seen in MS (Genestra, 2007). These elevated ROS levels along with the enhanced inflammatory response negatively affect mitochondrial function. Mitochondrial injury, oxidative stress, and altered metabolism are thought to be connected to the formation of plaques and subsequent neurodegeneration in both white and gray matter lesions (Fischer et al., 2012).
Several mouse models of MS effectively recapitulate the inflammatory response, mitochondrial dysfunction, and oxidative stress seen in the disease. In the experimental autoimmune encephalomyelitis (EAE) model, mitochondrial dysfunction appears early in the disease progression with damage to the mitochondria being evident even before the inflammatory processes of the disease develop (Qi et al., 2006; Sadeghian et al., 2016). EAE mice also show high levels of oxidative damage in the spinal cord along with elevated levels of oxidative stress-induced enzymes (Wang et al., 2017a) and reduced frequency of TH1, TH17, and B cell MHCII expression (Schulze-Topphoff et al., 2016). Similar observations have been made in the lipopolysaccharide (LPS)-induced model of MS. Elevated TNFα, IL-6, and IL-10 is seen in the blood of LPS-treated animals as are increased markers of oxidative stress (Yang et al., 2018). Widespread mitochondrial dysfunction is also observed throughout the brains of LPS-treated animals (Noh et al., 2014).
Multiple reports suggest a role for NRF2 in MS pathogenesis. Loss of NRF2 has been shown to result in more rapid onset and a more severe clinical course following EAE treatment that was accompanied by increased glial activation and exacerbated spinal cord damage and axonal degeneration as well as increased levels of proinflammatory cytokines (Johnson et al., 2010; Larabee et al., 2016; Table 1). Conversely, a number of NRF2-activating compounds have shown beneficial effects in MS model systems. NRF2 activation by resveratrol, lycopene, quercetin, and ferulic acid has been shown to reduce LPS-induced neurotoxicity, improve synaptic and mitochondrial function, and reduce inflammatory markers as well as gliosis (Chen et al., 2017; Khan et al., 2018; Rehman et al., 2019; Wang et al., 2019). In the EAE model, DMF treatment increased NRF2 activation in neurons and glial cells and improved disease score ratings, an effect that was lost with NRF2 deletion (Linker et al., 2011).
NRF2 activation as a clinical target is also well established in MS. DMF, also known as Tecfidera or BG-12, was licensed as an oral therapy for relapsing remitting MS in 2013. DMF treatment has been evaluated in Phase I and Phase II trials and has been shown to reduce relapse rates and decrease the number and progression of lesions, even though no differences were seen on the expanded disability status scale (Kappos et al., 2008; Fox et al., 2012; Gold et al., 2012; Table 2). DMF has also been shown to be comparable or superior to several other MS treatments. DMF-treated patients had lower annualized relapse rates and 12-week disability progression when compared with patients treated with glatiramer acetate (Chan et al., 2017). Patients who switched from first-generation platform disease-modifying therapies to DMF also saw reductions in annualized relapse rates and lesions, and switching to DMF treatment was found to be comparable with fingolimod and superior to teriflunomide (Fernandez et al., 2017; Prosperini et al., 2018; Ontaneda et al., 2019; Table 2).
DMF treatment has been shown to increase the expression of the NRF2 target gene NQO1 in the blood of MS patients (Gopal et al., 2017; Hammer et al., 2018), and those patients who showed a significant increase in NQO1 expression after 4 to 6 weeks of treatment were more likely to achieve no evidence of disease activity status 1 year later (Hammer et al., 2018; Table 2).
The exact mechanism by which DMF exerts its beneficial effects has not been fully described, although multiple mechanisms including shifting toward anti-inflammatory immune balance, inhibition of T cell activation, induction of B and T cell apoptosis, inhibition of proinflammatory cytokines, and reduction of memory T cells have all been suggested as contributing factors (Treumer et al., 2003; Longbrake et al., 2016; Schulze-Topphoff et al., 2016; Smith et al., 2017; Montes Diaz et al., 2018a). There have been many clinical and basic science studies of DMF in MS. An excellent and thorough review of the history and mechanism of DMF as an MS therapy was recently published by Montes Diaz et al. (2018b).
Treatment with other NRF2-activating compounds has likewise demonstrated beneficial results in MS patients. It has been reported that Vitamin D, omega 3 fatty acids, and lipoic acid all result in decreased inflammatory markers, increased antioxidant capacity, and improvements on the expanded disability status scale (Gallai et al., 1995; Khalili et al., 2014; Kouchaki et al., 2018; Table 2), although NRF2 activation was not investigated as a mechanism in any of these studies. Vitamin D supplementation has also been associated with improved cognitive function in MS patients, especially those that were vitamin D deficient (Darwish et al., 2017; Table 2).
NRF2 and AD
AD is the most common form of dementia. It currently affects an estimated 5.7 million people, and this number is predicted to reach 14 million by 2050 (Alzheimer's Association, 2017). The two pathological hallmarks of AD are intracellular neurofibrillary tangles comprised of the protein tau and extracellular β-amyloid (Aβ) plaques. The relationship between these hallmarks and the inflammation, oxidative stress, and mitochondrial dysfunction that occurs in AD is complex. The Aβ plaques activate nearby microglia which can result in increased release of proinflammatory cytokines and ROS which can result in mitochondrial dysfunction (Galasko and Montine, 2010). However, oxidative stress and neuroinflammation are also believed to facilitate the pathological protein aggregation seen in AD (Di Bona et al., 2010).
Increased oxidative stress is considered to be an early event in AD brains (Lovell and Markesbery, 2007), and diminished antioxidant capacity along with increased markers of oxidative stress are evident in both the blood and brains of AD patients (Gubandru et al., 2013; Schrag et al., 2013; Zabel et al., 2018). Reduced neuronal mitochondrial function and number have also been reported in AD patients (Hirai et al., 2001), and studies suggest that alterations in mitochondrial bioenergetics in the brain precede and may even induce cognitive decline in AD (Yao et al., 2009).
It has been reported that NRF2 nuclear expression is decreased in AD and a recent meta-analysis of microarray datasets identified 31 downregulated ARE genes in AD patients (Ramsey et al., 2007; Kanninen et al., 2008; Wang et al., 2017b). Similarly, in transgenic mouse models of AD, loss of NRF2 has been shown to increase levels of Aβ and phosphorylated tau (Branca et al., 2017; Rojo et al., 2017); increase glial activation, markers of oxidative stress, and neurodegeneration; and exacerbate cognitive decline (Rojo et al., 2017; Rojo et al., 2018; Table 1).
Summary of Studies Using NRF2KO in Neurodegenerative Disease Models.
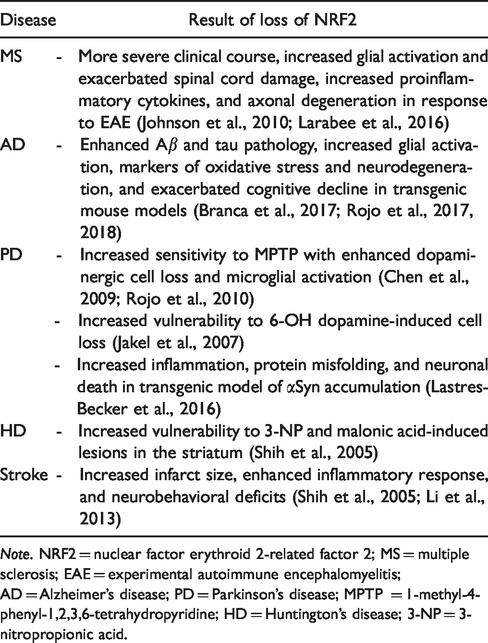
Note. NRF2 = nuclear factor erythroid 2-related factor 2; MS = multiple sclerosis; EAE = experimental autoimmune encephalomyelitis; AD = Alzheimer’s disease; PD = Parkinson’s disease; MPTP = 1-methyl-4-phenyl-1,2,3,6-tetrahydropyridine; HD = Huntington’s disease; 3-NP = 3-nitropropionic acid.
Summary of Clinical Interventions With NRF2-Activating Compounds.
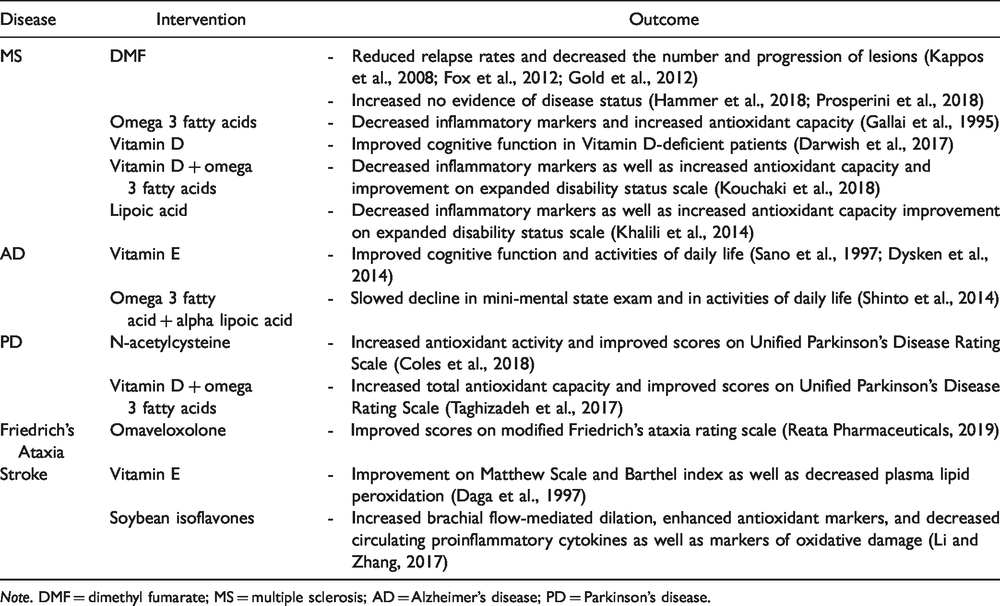
Note. DMF = dimethyl fumarate; MS = multiple sclerosis; AD = Alzheimer’s disease; PD = Parkinson’s disease.
Conversely, the activation of NRF2 has been shown to be beneficial in models of AD. A recent study found that NRF2 activation by sulforaphane reduces amyloid secretion and normalizes cytokine in AD astrocytes derived from human-induced pluripotent stem cells (Oksanen et al., 2019). In in vivo studies, the NRF2-activating compound tert-Butylhydroquinone (tBHQ) was found to protect against cell death in isolated neurons exposed to Aβ (Kanninen et al., 2008), and oral curcumin, another NRF2 activator, has been shown to prevent synaptic degradation and improve spatial learning in the 5xFAD mouse model of Aβ accumulation (Zheng et al., 2017). DMF has likewise been shown to protect against Aβ-induced cell death in vitro (Campolo et al., 2018) and also to improve spatial memory in a rat model of AD (Majkutewicz et al., 2016).
While therapies specifically targeting NRF2 have yet to be investigated clinically, there is some evidence that treatment with antioxidant compounds could be beneficial. Trials with vitamin E have shown slight improvements in cognitive function and activities of daily life at high doses (Sano et al., 1997; Dysken et al., 2014), and treatment with a combination of omega 3 fatty acids and alpha lipoic acid slowed decline in mini-mental state exam as well as activities of daily life (Shinto et al., 2014; Table 2). Although these compounds are known to activate NRF2, none of these studies investigated that specifically.
NRF2 in PD
PD is a progressive and incurable movement disorder that is accompanied by varying degrees of cognitive dysfunction and dementia and is the second most common neurodegenerative disease (Goris et al., 2007; Tufekci et al., 2011). PD is characterized by loss of dopaminergic neurons in the substantia nigra and the accumulation of intracellular protein aggregates known as Lewy bodies, enriched with α-synuclein (αSyn; Bhat et al., 2018). Oxidative stress, mitochondrial dysfunction, and neuroinflammation have all been implicated in the development and progression of the disease (Navarro and Boveris, 2009; Di Filippo et al., 2010).
Imaging studies have observed mitochondrial dysfunction in the dopamine neurons in the substantia nigra early in PD progression (Hattingen et al., 2009), and reduced expression and activity of enzymes in the electron transport chain has been observed in the brains of PD patients throughout the course of the disease (Schapira et al., 1989, 1990; Trimmer et al., 2000). In late-stage PD patients, increased mutations in mtDNA are seen which lead to dysfunction in Complex I and increased oxidative stress (Schapira, 2008; Moon and Paek, 2015). Increased markers of oxidative damage along with decreased antioxidant enzyme activity have also been observed in the blood of PD patients as well (Wei et al., 2018). Inflammation is also prevalent in PD patients. Proinflammatory cytokines such as TNFα and IL-6 are known to be elevated in both the brain and CSF of patients with PD (Dzamko et al., 2015; Hirsch et al., 2012). In fact, it has even been hypothesized that PD pathogenesis may result from an inflammatory infection of the gut and that inflammation then spreads systemically (Weller et al., 2005).
There are multiple lines of evidence suggesting that NRF2 may be a viable therapeutic target for PD. NRF2 expression and activity has been shown to be altered in nigral dopaminergic neurons in PD patients (Schipper et al., 1998; Ramsey et al., 2007) and a functional haplotype in the human NRF2 promoter that increases transcriptional activity of the gene is associated with decreased risk and delayed onset of PD (von Otter et al., 2010). Pharmacological alteration of NRF2 expression levels can phenocopy this protective haplotype in mice (Huang et al., 2017b; Meng et al., 2017).
In addition, in the 1-methyl-4-phenyl-1,2,3,6-tetrahydropyridine (MPTP) model of PD, decreased NRF2 activity has been reported, and it was observed that loss of NRF2 exacerbated the phenotype (Chen et al., 2009; Table 1). Dopaminergic neuronal loss and microglial activation were both also more severe in mice in which NRF2 has been deleted (Rojo et al., 2010; Table 1). These mice show a similar increase in vulnerability to 6-OH dopamine, and this damage can be prevented by transplantation of astrocytes overexpressing NRF2 (Jakel et al., 2007; Table 1). Likewise, in a model of αSyn accumulation, loss of NRF2 exacerbated inflammation, protein misfolding, and neuronal death (Lastres-Becker et al., 2016; Table 1).
Activation of NRF2 has been associated with neuroprotection in various PD model systems. In MPTP-treated mice, NRF2 activation, via siRNA mediated knockdown of KEAP1, was associated with a reduction in oxidative stress and neuroinflammation (Williamson et al., 2012). NRF2 activation by sulforaphane also induced the expression of antioxidant enzymes and protected against dopaminergic neuronal loss in MPTP-treated mice (Jazwa et al., 2011) as did a NRF2-activating synthetic triterpenoid that also reduced ROS levels and upregulated genes involved in mitochondrial biogenesis (Yang et al., 2009). In addition, in neuroblastoma-overexpressing αSyn, treatment with tBHQ reduced ROS levels and improved mitochondrial respiratory rates (Fu et al., 2018).
Although NRF2 has not yet been targeted in clinical interventions in PD, epidemiological evidence suggests that high levels of consumption of the NRF2-activating vitamins E and C are associated with decreased risk of PD (Zhang et al., 2002; Seidl and Potashkin, 2011). In addition, 4 weeks of treatment with N-acetyl cysteine, which also activates NRF2, improved scores on the Unified Parkinson’s Disease Rating Scale and increased peripheral markers for antioxidant activity (Coles et al., 2018) as did 12 weeks of intervention with omega 3 fatty acids and vitamin E (Taghizadeh et al., 2017; Table 2). However, NRF2 activation was not specifically implicated as a mechanism of action in either of these studies.
NRF2 and HD
HD is an autosomal dominant neurodegenerative disorder caused by a polyglutamine expansion in the huntingtin protein (Jimenez-Sanchez et al., 2017). Its primary symptoms are motor impairment, cognitive decline, and psychiatric problems which worsen as the disease progresses. Degeneration of both the neostriatal and cerebral cortex are believed to contribute to the cognitive impairment and motor symptoms (Vonsattel et al., 1985; Halliday et al., 1998). As the huntingtin protein aggregates, it becomes toxic to neurons and promotes the generation of ROS (Goswami et al., 2006). Oxidative stress is particularly prominent in the neostriatum of HD brains (Sorolla et al., 2008) and is thought to be an important driver of degeneration. Markers of increased oxidative stress are also evident peripherally. Plasma lipid peroxidation is increased, and glutathione levels are decreased in HD patients. This imbalance can be observed prior to symptom onset and continues to be proportional to the severity of the disease as it progresses (Chen et al., 2007; Klepac et al., 2007). Increased oxidative damage to proteins as well as mtDNA has also been observed in the brains of HD patients (Chen et al., 2007; Duran et al., 2010; Johri and Beal, 2012). Postmortem analysis also revealed that the levels of mitochondrial enzymes involved in oxidative phosphorylation are also depressed in the brains of HD patients, especially the basal ganglia (Chen et al., 2007; Duran et al., 2010). In addition to reports of increased oxidative stress (Browne et al., 1997; Browne and Beal, 2006; del Hoyo et al., 2006; Chen et al., 2007; Klepac et al., 2007; Chang et al., 2012) and mitochondrial dysfunction (Browne, 2008; Damiano et al., 2010; Kim et al., 2010), chronic inflammation is also evident in HD (Pavese et al., 2006; Tai et al., 2007; Bjorkqvist et al., 2008; Politis et al., 2011). Inflammation appears to be an early event in the pathogenesis of HD, and PET imaging has revealed increased microglial activation that is already evident in the striatum and cortex of presymptomatic HD carriers (Tai et al., 2007; Politis et al., 2011). Plasma concentrations of inflammatory cytokines are likewise elevated prior to the onset of disease symptoms, and increased immune activity persists in the CSF of HD patients (Bjorkqvist et al., 2008).
The same mitochondrial dysfunction, oxidative stress, and neuroinflammation are also seen in the brains of animal models of HD, and using these models, studies have demonstrated an important role for NRF2. In the 3-nitropropionic acid (3-NP)-induced model of HD, NRF2 activation is reduced and mice in which NRF2 has been knocked out have been reported to be significantly more vulnerable to both 3-NP and malonic acid-induced lesions in striatum (Shih et al., 2005a; Table 1). Conversely, intrastriatal injections of NRF2 overexpressing astrocytes has been found to be protective against 3-NP and malonic acid-induced damage (Calkins et al., 2005).
Pharmacological activation of NRF2 likewise shows beneficial results in mouse models of HD. DMF treatment protects cortical and striatal neurons, slows weight loss, helps maintain motor function, and increases lifespan in WT but not mice lacking NRF2 (Ellrichmann et al., 2011; Jin et al., 2013). Oral administration of NRF2-activating synthetic triterpenoids similarly attenuated motor deficits, increased longevity, and reduced oxidative stress in a transgenic HD mouse model (Stack et al., 2010), and a NRF2-activating compound isolated from the plant Panax ginseng Meyer decreased ROS and restored antioxidant enzyme levels in the striatum and ameliorated behavioral impairments in the 3-NP mouse model (Gao et al., 2015). In addition, sulforaphane has beneficial effects in both transgenic and 3-NP-induced models of HD. Sulforaphane promoted huntingtin protein degradation and reduced cytotoxicity in both central and peripheral tissues of transgenic animals (Liu et al., 2014) and was also able to suppress 3-NP-induced proinflammatory cytokine production in the striatum and improve behavioral impairments (Jang and Cho, 2016).
In humans, disrupted NRF2 signaling has also been observed. The NRF2 target antioxidant enzymes glutathione peroxidase and SOD1 are reduced in the leukocytes of HD patients compared with controls (Chen et al., 2007). In addition, it has been reported that in striatal neurons, abnormal huntingtin protein disturbs NRF2 signaling, promoting mitochondrial dysfunction and increased oxidative stress (Kim et al., 2010). Although NRF2-activating compounds have not been tested in clinical trials in primary monocytes from HD patients, NRF2 induction by the KEAP1 modifying small molecule C151 repressed IL-1, IL-6, IL-8, and TNFα production (Quinti et al., 2017).
NRF2 and Friedrich’s Ataxia
Friedrich’s ataxia is an inherited degenerative neuromuscular disorder for which there are no approved therapies (Aranca et al., 2016). It is the most common hereditary ataxia affecting about 1 in 50,000 people worldwide (Polek et al., 2013; Vankan, 2013). The disease is an autosomal recessive condition primarily affecting the dorsal root ganglia, cerebellar dentate nuclei, and the heart. It is caused by a GAA repeat expansion mutation in the frataxin gene. This leads to transcriptional silencing which results in a progressive decrease of frataxin protein expression. Frataxin helps assemble iron sulfur clusters necessary for proper mitochondrial function (Li et al., 2008). In Friedrich’s ataxia patients, the decreased frataxin expression causes mitochondrial iron overload, impaired ATP production, and increased oxidative stress (Li et al., 2008; Santos et al., 2010; Aranca et al., 2016). The reduced ATP production is believed to account for the progressive muscle weakness, fatigue, and decreased coordination seen in patients with the disease. The increase in oxidative stress is also thought to be pathogenic, leading to chronic depletion of antioxidants and causing neurodegeneration (Nickel et al., 2014). Cerebellar granule neurons are particularly susceptible to these changes exhibiting significant increases in ROS and lipid peroxidation along with reduced glutathione. Studies using these cerebellar granule neurons have shown that reduced frataxin production leads to increased ROS which induces mitochondrial impairments (Abeti et al., 2015, 2016).
NRF2 signaling dysfunction has been widely reported in animal models of Friedrich’s ataxia. A conditional frataxin knockout mouse line showed decreased NRF2 expression and increased KEAP1 expression (Anzovino et al., 2017) and in the mouse motor neuron cell line NSC-34, frataxin shRNA likewise reduced NRF2 expression and activity (Paupe et al., 2009). In contrast, inducing NRF2 with sulforaphane or the NRF2-activating compound EPI-7443 in neural stem cells isolated from a Friedrich’s ataxia mouse model was shown to reestablish proper differentiation which was previously impaired in those cells (La Rosa et al., 2019). In cultured motor neurons, sulforaphane also increased frataxin levels as well as neurite number and extension (Petrillo et al., 2017). Similar reductions in NRF2 expression have been seen in fibroblasts isolated from patients (Paupe et al., 2009; Petrillo et al., 2017), and sulforaphane treatment likewise increased frataxin levels and enhanced neurite outgrowth in these cells (Petrillo et al., 2017).
The NRF2-activating compound omaveloxolone has been shown to be beneficial in the KIKO and the YG8R mouse models of Friedrich’s ataxia as well as in fibroblasts isolated from human patients. In these models, omaveloxolone restored Complex I activity, increased glutathione levels, decreased ROS, and restored the mitochondrial membrane potential preventing cell death (Abeti et al., 2018). Based on these promising preclinical studies, omaveloxolone is currently undergoing clinical testing. A recent press release announced the results of their Phase II trial that found that 48 weeks of treatment with the compound was generally well tolerated and resulted in significantly improved scores on the modified Friedrich’s ataxia rating scale (Reata Pharmaceuticals, 2019; Table 2).
NRF2 and Stroke
Stroke is the second leading cause of death worldwide and the leading cause of acquired adult disability (Lozano et al., 2012; Murray et al., 2012). Ischemic stroke is characterized by decreased blood flow to parts of the brain resulting in injury to brain tissue and impaired neurologic functioning (Jauch et al., 2013; Ding et al., 2017). A cascade of biochemical events occur following an ischemic stroke that promote tissue damage including inflammatory activation and mitochondrial dysfunction leading to an overproduction of ROS. Eventual restoration of blood flow (reperfusion) exacerbates inflammatory responses and ROS generation leading to further damage from oxidative stress, including degradation of vascular wall proteins and deterioration of blood–brain barrier (BBB) integrity (Stephenson et al., 2000; Kunz et al., 2008; Harari and Liao, 2010; Pradeep et al., 2012).
Animal studies have shown that mice in which NRF2 has been deleted have enhanced infarct size, inflammatory response, and neurobehavioral deficits when compared with NRF2 expressing mice (Shih et al., 2005b; Li et al., 2013; Table 1). Conversely, NRF2 activation has been shown to be beneficial in protecting the brain from injury. tBHQ treatment attenuated neonatal hypoxic-ischemic brain damage in rats (Zhang et al., 2018), and the NRF2-activating compound metformin likewise reduced infarct volume and was able to attenuate cognitive impairments in a mouse model of transient middle cerebral artery occlusion (Kaisar et al., 2017). Trichostatin A-induced NRF2 activation (resulting from decreased KEAP1 expression) similarly increased neuronal cell viability and reduced infarct volume following stroke (Wang et al., 2012).
A number of plant-derived NRF2-activating compounds have also been shown to have beneficial effects in rodent models of stroke. When given prior to injury, the plant-derived flavanol (-)-epicatechin was able to reduce infarct size and the subsequent cognitive impairment, but this effect was lost in mice that do not express NRF2. Posttreatment also improved the same outcome but in a time-sensitive manner (Shah et al., 2010). NRF2 activation by sulforaphane increased the expression of cytoprotective genes in brain tissue and preserved BBB integrity (Zhao et al., 2007), while ginkgolides and bilobalide have been shown to activate NRF2 and decrease both cerebral ROS levels as well as infarct volume ratios in middle cerebral artery occlusion rats (Liu et al., 2019b). Activation of NRF2 by the isoquercetin also attenuated oxidative stress and neuronal loss following ischemia/reperfusion injury in mice by inhibiting NFkB activation (Dai et al., 2018).
Clinical research into NRF2 activation as a stroke therapy is limited, but a few dietary interventions with compounds that can activate NRF2 do suggest a potential benefit. Following ischemic stroke, 6 weeks of vitamin E supplementation was shown to elicit a greater improvement in both the Matthew scale and Barthel index than placebo. This was accompanied by a significant reduction in plasma lipid peroxidation suggesting increased antioxidant activity, although it is unknown the contribution of NRF2 activation specifically to this effect because while vitamin E can activate NRF2, it also possesses free radical scavenging properties in and of itself (Daga et al., 1997; Table 2). However, when patients with ischemic stroke were given soybean isoflavones for 24 weeks, NRF2 activation was implicated in the improvements observed. Supplementation resulted in increased brachial flow-mediated dilation and NRF2 and SOD expression along with decreased circulating levels of C-reactive protein, 8-isoprostane, malondialdehdye, IL-6, and TNFα. The effects on circulating oxidative stress markers were lost when NRF2 was silenced (Li and Zhang, 2017; Table 2).
The potential benefits of NRF2 activation as a means of preventing stroke are somewhat less clear. A number of large-scale prospective studies have been conducted investigating supplementary with vitamins and have yielded conflicting results. In one study of 8,171 female health professionals with a history of cardiovascular disease who received vitamin C, vitamin E, or beta carotene for a mean follow-up time of 9 years, it was determined that those individuals who received vitamin C or vitamin E experienced fewer strokes (Cook et al., 2007), although again, whether this was due to their abilities to activate NRF2 specifically was not determined. Conversely, in another study where more than 20,000 adults with coronary artery disease, occlusive arterial disease, or diabetes were given supplementation with a combination of vitamin E, vitamin C, and beta carotene for 5 years, there was no difference in the incidence of stroke (Heart Protection Study Collaborative Group, 2002). More studies are clearly needed to determine whether directly targeting NRF2 would be beneficial as a preventative agent for ischemic stroke.
NRF Activating Compounds
While NRF2 activation occurs endogenously in response to increased oxidative stress, it can also be induced by exogenous agents. As previously mentioned, many botanically derived and synthetic compounds have been shown to potently activate the NRF2 pathway.
Botanically Derived NRF2 Activators
Sulforaphane is an organic isothiocyanate found in cruciferous plants such as broccoli, brussels sprouts, cabbage, and cauliflower. Sulforaphane activates NRF2 through direct electrophilic modification of the cysteines on KEAP1 allowing for dissociation of NRF2 and nuclear translocation (Takaya et al., 2012). This activation has been reported to increase the expression of antioxidant enzymes in the hippocampus of treated animals (Wang et al., 2014). Sulforaphane can also modulate mitochondrial dynamics through both NRF2-dependent and -independent mechanisms (O'Mealey et al., 2017; de Oliveira et al., 2018). It has also been demonstrated to inhibit TNFα-induced NFkB activation both through directly blocking the interaction of NFkB and its consensus sequence as well as inhibiting IkB-α phosphorylation and degradation (Moon et al., 2009; Checker et al., 2015). These effects of sulforaphane have resulted in neuroprotection in both in vitro and in vivo in models of stroke, traumatic brain injury (TBI), AD, PD, HD, and MS (Zhao et al., 2005, 2006; Han et al., 2007; Kwak et al., 2007; Zhao et al., 2007; Jazwa et al., 2011; Kim et al., 2013; Srivastava et al., 2013; Liu et al., 2014; Jang and Cho, 2016; Yoo et al., 2019).
Lycopene is an aliphatic hydrocarbon carotenoid that can be found in plants such as tomatoes, papayas, and watermelons. Lycopene has been shown to increase antioxidant enzyme activity and decrease inflammatory response in both d-galactose model and transgenic models of AD (Yu et al., 2017; Zhao et al., 2017a). It also attenuated Aβ-induced mitochondrial damage in isolated cortical neurons (Qu et al., 2011; Qu et al., 2016) and reduced proinflammatory cytokines in the brain of Aβ-exposed animals (Liu et al., 2018). Similar effects of lycopene on oxidative and mitochondrial damage have been demonstrated in a pentylenetetrazol-induced model of seizure where it also decreased convulsive activity (Bhardwaj and Kumar, 2016; Kumar et al., 2016). Lycopene also decreased markers of oxidative stress and reduced neuronal cell loss in models of PD and stroke (Prema et al., 2015; Lei et al., 2016) and was able to attenuate BBB disruption and neurological deficits in a model of subarachnoid hemorrhage (Wu et al., 2015).
Curcumin is a polyphenol derived from Curcuma longa rhizomes and has potent antioxidative and anti-inflammatory properties (Agarwal et al., 2011; Kakkar and Kaur, 2011; Dong et al., 2018). Curcumin activates NRF2 both by electrophilic modification of KEAP1 as well as by repression of KEAP1 expression (Ren et al., 2019; Robledinos-Anton et al., 2019). Curcumin treatment has been shown to suppress proinflammatory gene expression through prevention of NFkB activation in microglial cells (Cui et al., 2010; Zhang et al., 2010). In a model of cerebral ischemia and reperfusion, this downregulation of NFkB resulted from NRF2 activation by curcumin and reduced overall brain edema as well as neurological dysfunction (Li et al., 2016). Curcumin was similarly beneficial in models of intracerebral hemorrhage and TBI where again its neuroprotective effects were linked to NRF2 activation (Wang et al., 2015; Kobayashi et al., 2016; de Alcantara et al., 2017; He et al., 2019).
Epigallocatechin gallate (EGCG) is the most abundant catechin found in green tea. It was shown to upregulate NRF2 activity via phosphorylation downstream of p38MAPK and ERk1/2 signaling pathways (Yang et al., 2015), although it can also activate NRF2 through electrophilic disruption of its association with KEAP1 (Mori et al., 2010). In mice, EGCG has been shown to protect against ischemia reperfusion injury in a NRF2-dependent manner (Han et al., 2014) and has also been shown to inhibit NFkB activity, reduce Aβ fibrilization, and improve memory in Aβ exposed animals (Lee et al., 2009b). Neuroprotective effects of EGCG have also been demonstrated in vitro and in vivo in models of PD, MS, and TBI accompanied by increased NRF2 activity and enhanced antioxidant activity and reduced inflammatory responses (Ma et al., 2010; Itoh et al., 2013; Wu, 2016; Semnani et al., 2017; Xu et al., 2018).
Resveratrol is a bioactive polyphenol found in fruits such as grapes and berries. Resveratrol activates NRF2 by phosphorylation via p38MAPK (Shi et al., 2018). Resveratrol treatment has potent antioxidant and anti-inflammatory effects and has been shown to regulate mitochondrial biogenesis (Chiang et al., 2018; Chuang et al., 2019). The NRF2-activating and mitochondrial effects of resveratrol are thought to underlie its protective effects in a rotenone model of PD (Gaballah et al., 2016; Peng et al., 2016). Activation of NRF2 by resveratrol also has been shown to both prevent against ischemic injury and mitigate the oxidative stress induced by ischemic injury in rodents (Narayanan et al., 2015; Gao et al., 2018). In addition, resveratrol treatment can also attenuate TBI-induced cognitive deficits in mice via NRF2 activation (Shi et al., 2018) and can ameliorate cellular and mitochondrial damage in a drosophila model of spinocerebellar ataxia by upregulating the same pathway (Wu et al., 2018).
Alpha lipoic acid is another naturally occurring NRF2-activating compound with neuroprotective effects. While it can be found in low amounts in a number of plants including spinach, broccoli, carrots, and beets, it is more frequently consumed as a dietary supplement. The exact mechanisms by which alpha lipoic acid activates NRF2 is not currently known, although the compound can form lipoyl-cysteinyl mixed disulfides on KEAP1 which would prevent newly synthesized NRF2 from binding to its chaperone (Dinkova-Kostova et al., 2002; Kobayashi et al., 2006). However, alpha lipoic acid has also been shown to activate protein kinase C, one of the kinases that can activate NRF2 that could represent an alternative mechanism of activation (Sen et al., 1999). Activation of NRF2 by alpha lipoic acid has been shown to inhibit cell loss following TBI (Xia et al., 2019) as well as reduce infarct volume, oxidative damage, and edema and promote neurologic recovery following stroke (Lv et al., 2017). In models of PD, alpha lipoic acid has been shown to decrease ROS, upregulate mitochondrial biogenesis, restore ATP content, and preserve dopaminergic neurons (Zaitone et al., 2012; Zhao et al., 2017b), although whether NRF2 activation was required for these effects was not investigated. Alpha lipoic acid also potently reduces inflammation in mouse models of MS (Morini et al., 2004; Chaudhary et al., 2015), yet, again, these studies did not investigate whether this was linked to NRF2 activation.
The medicinal plant Centella asiatica (L) Urban also contains many NRF2-activating compounds. The plant contains high levels of four triterpene compounds, Asiatic acid, madecassic acid, asiaticoside, and madecassoside (MS) that have all been shown to activate NRF2 but do not possess strong electrophilic properties (Yang et al., 2016; Jiang et al., 2017; Fan et al., 2018; Liu et al., 2019c; Meng et al., 2019). Centella asiatica also contains many caffeoylquinic acids that we and others have shown can activate NRF2 as well (Boettler et al., 2011; Gray et al., 2014; Liang et al., 2019). Our lab has demonstrated that a water extract of Centella asiatica can activate NRF2 in neuroblastoma cells and isolated primary neurons as well as in the brains of treated animals, and this activation is accompanied by improved mitochondrial function, enhanced synaptic density, and improved cognitive function in mouse models of aging and AD (Gray et al., 2015; Gray et al., 2017a, 2017b; Gray et al., 2018a, 2018b). Other groups have likewise shown antioxidant, anti-inflammatory, and cognitive-enhancing effects of the plant in rodent models of chemically induced neurotoxicity, stroke, seizure, PD, and HD (Gupta et al., 2003; Flora and Gupta, 2007; Shinomol and Muralidhara, 2008a, 2008b; Haleagrahara and Ponnusamy, 2010; Prakash and Kumar, 2013; Tabassum et al., 2013; Doknark et al., 2014). Work is ongoing in our lab to determine the requirement of NRF2 activation for the beneficial effects of Centella asiatica in both normal as well as pathological aging. Our most recent work has indicated that the cognitive benefits of the water extract of Centella asiatica (CAW), at least in healthy aging, do require NRF2. The Object Location Memory task is a test of spatial memory wherein the mouse using identical objects one of which is moved during testing to a location distinct from where it was during training (Figure 1(a)). If the mouse remembers the training location, it should spend a greater amount of time with the object in the new location. NRF2KO mice exhibited cognitive impairments relative to WT animals and while long-term CAW treatment improved the performance in the Object Location Memory test of 18-month-old WT mice but had no effect on age-matched NRF2 knockout mice (Figure 1(b)).
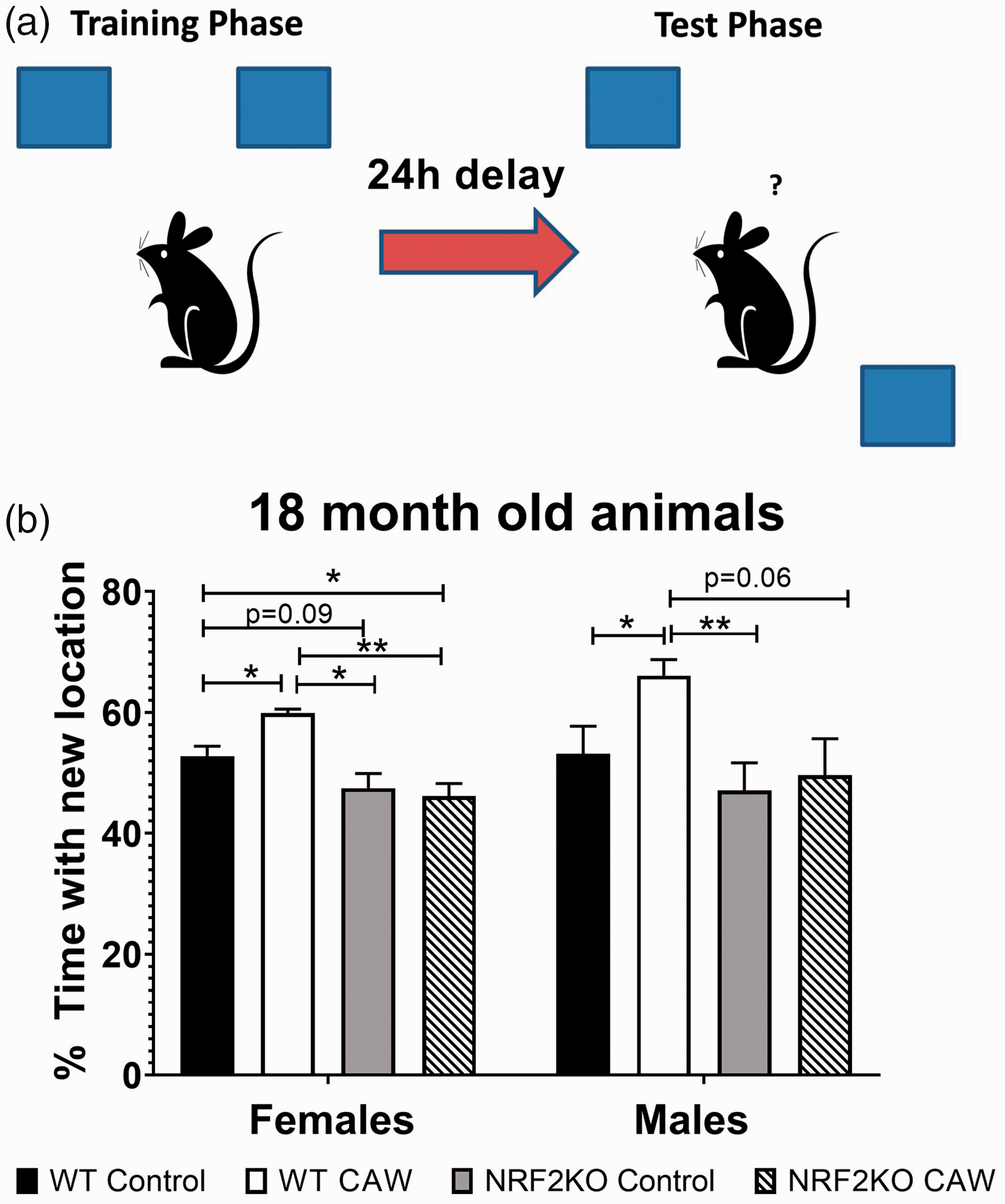
Object location memory. CAW treatment (2g/L for 13 months) improved performance in 18-month-old WT but not NRF2KO mice. NRF2KO mice were also impaired relative to age-matched WT animals. n = 4–8, *p< .05, **p < .01.
Synthetic Activators of the NRF2/ARE Pathway
DMF is an enoate ester formed by the condensation of fumaric acid and methanol. It is currently an FDA-approved disease-modifying drug for the treatment of relapsing MS under the name Tecfidera® (Deeks, 2016). Because DMF is a thiol-reactive electrophile, it is thought to primarily activate NRF2 via cysteine modification on KEAP1 (Saidu et al., 2019), although it has also been shown to affect NRF2 phosphorylation via PI3K and ERK1/2 pathways in neutrophils (Muller et al., 2016). Perhaps because of its well-documented anti-inflammatory and antioxidant effects, DMF has also been shown to be neuroprotective in many different neurodegenerative conditions. It has also been shown to prevent hippocampal injury following ischemia, reduce edema volume, and protect BBB integrity in mouse models of stroke (Kunze et al., 2015; Yao et al., 2016; Liu et al., 2019a) as well as improve cognitive function in models of AD and subarachnoid hemorrhage (Liu et al., 2015; Majkutewicz et al., 2016; Majkutewicz et al., 2018). In addition, as mentioned previously, DMF protects against both αSyn and Aβ toxicity and can reduce tau hyperphosphorylation (Lastres-Becker et al., 2016; Campolo et al., 2018; Bahn and Jo, 2019).
tBHQ is another known activator of NRF2 commonly used as a food preservative. tBHQ is an electrophile with the ability to disrupt the KEAP1/NRF2 complex and regulate oxidative stress. tBHQ has demonstrated antioxidant and neuroprotective effects. Treatment with tBHQ reduced oxidative stress and prevented neuronal toxicity and Aβ formation in NT2N neurons (Eftekharzadeh et al., 2010) and prevented Aβ-induced cell death in rats (Nouhi et al., 2011). It has also been shown to decrease secondary injury and improve function recovery following TBI and attenuate neurological injury after intracerebral hemorrhage in mice (Sukumari-Ramesh and Alleyne, 2016; Chandran et al., 2018).
Metformin is a highly prescribed antihyperglycemic drug that is often used as a treatment for type II diabetes. However, metformin can also activate NRF2, likely through its induction of AMPK which subsequently phosphorylates NRF2 (Ashabi et al., 2015; Joo et al., 2016), and has been shown to be neuroprotective in many neurodegenerative model systems. Metformin protects against oxidative stress-induced BBB damage, and this was determined to be through NRF2 activation (Prasad et al., 2017). Metformin is also well known for its effects on mitochondrial function and biogenesis (Vial et al., 2019) and also has documented antioxidant and anti-inflammatory effects in rodent models of ischemic stroke, AD, PD, and MS (Ashabi et al., 2015; Katila et al., 2017; Ou et al., 2018; Mudgal et al., 2019).
The tricyclic compound acetylenic tricyclic bis(cyano enone) (TBE-31) is considered to be one of the most potent NRF2 inducers because it contains two electrophilic Michael acceptors (Dinkova-Kostova et al., 2010). TBE-31 has been investigated in cancer model systems and has been found to have strong antioxidant and anti-inflammatory effects which are thought to contribute to its anticancer activity (Onyango et al., 2014; Knatko et al., 2015; Chan et al., 2016). It has also been shown to reduce lipid peroxidation and improve mitochondrial imbalance in Friedrich’s ataxia (Abeti et al., 2015).
Conclusions
It is increasingly clear that NRF2 could represent a viable therapeutic target in neurological conditions. Its activation attenuates many processes involved in neurodegenerative disorders including mitochondrial dysfunction, oxidative stress, and neuroinflammation (Figure 2). NRF2-activating compounds are already FDA approved for use MS, and clinical testing is underway in Friedrich’s ataxia, but the literature suggests that such activators could be warranted in many other neurodegenerative conditions as well.
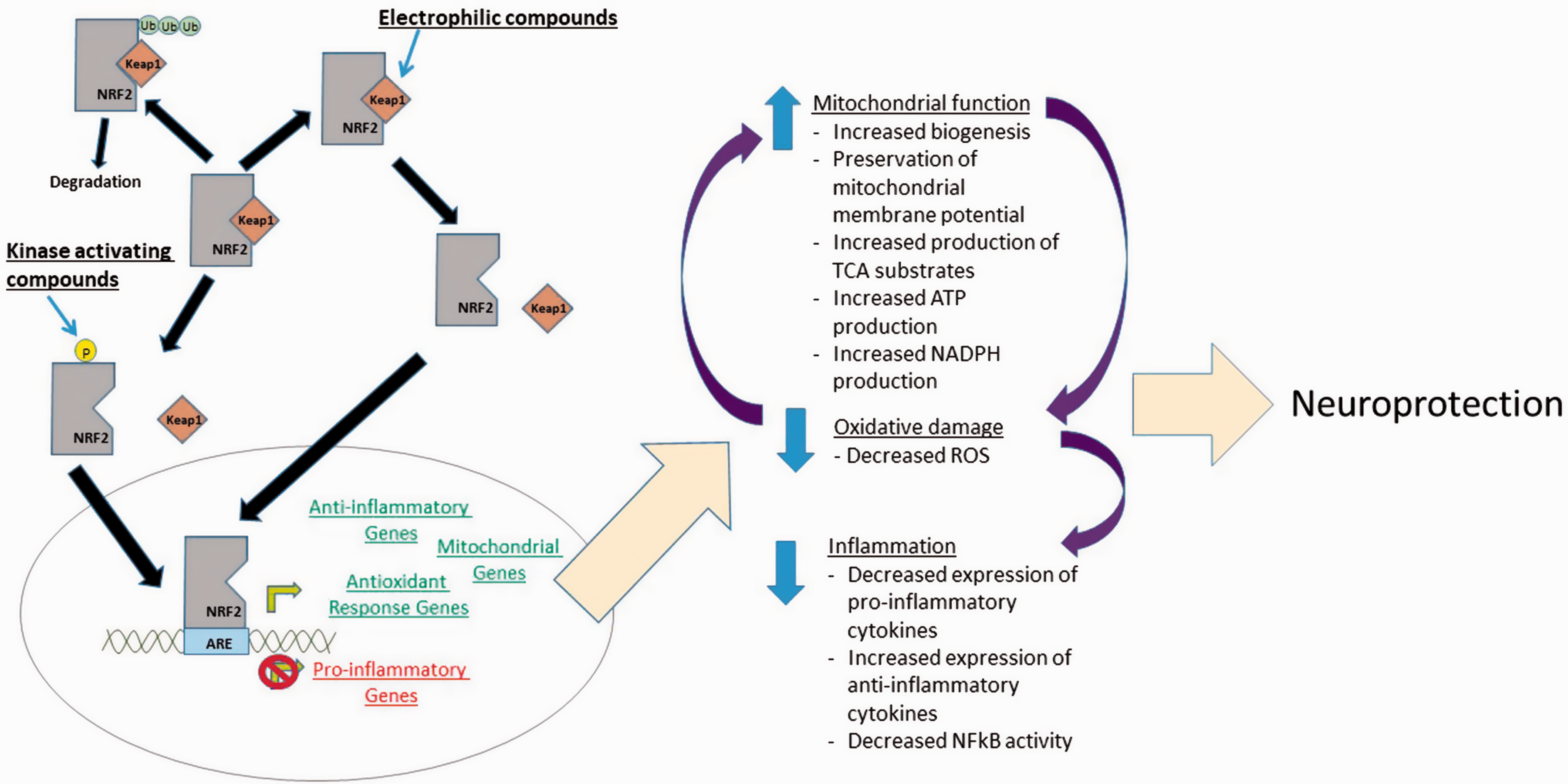
Summary of neuroprotective effects of NRF2 activation.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
