Abstract
Abstract
Introduction
The volume of shoulder arthroplasties in the United Kingdom continues to rise, with 8221 cases recorded in the National Joint Registry (NJR) in 2023. Amid increasing demand and pressure on NHS resources, reducing hospital length of stay (LOS) is a key priority for improving efficiency. This study aimed to identify independent predictors of prolonged LOS following shoulder arthroplasty.
Methods
NJR data from April 2012 to March 2022 were linked with Hospital Episode Statistics (HES) for England. Prolonged LOS was defined as >2 nights (above the cohort median). Variables analysed included age, sex, Charlson comorbidity index (CCI), comorbidities, surgical indication, implant type, operating surgeon volume, and day of surgery. Univariable and multivariable logistic regression models were used to identify predictors.
Results
Among 47,145 patients, older age, higher CCI, and ASA grades 3 and 4 were significantly associated with extended LOS. Male patients had a 45% reduced risk of prolonged stay. Trauma-related procedures and surgeries conducted Friday–Sunday were associated with increased LOS. Patients treated by high-volume surgeons had a 19% lower risk of prolonged LOS. Several comorbidities were independently predictive; however, differed across implants.
Conclusion
Both patient-level and system-level factors contribute to prolonged LOS. Optimising perioperative care and scheduling may reduce LOS and improve NHS resource utilisation.
Introduction
Shoulder arthroplasty procedures in the United Kingdom (UK) are increasing year on year, with 8221 procedures recorded in the National Joint Registry (NJR) in 2023. 1 The caseload of shoulder arthroplasty is projected to increase by 234% in England by 2050, with an annual cost to hospitals of £235 million, placing significant pressures on the National Health Service (NHS). 2 Optimisation of modifiable factors to reduce length of stay (LOS) after shoulder arthroplasty have been shown to reduce costs and readmission rates. 3
In the UK, there has been limited research into optimising LOS after shoulder arthroplasty. One study of 640 shoulder arthroplasty patients at a high volume shoulder unit looked at predictors of prolonged length of stay and found that increasing age, female sex, chronic kidney disease, congestive cardiac failure, previous myocardial infarction, intraoperative complication and transfusion were independent predictors of increased length of stay. 4 Larger studies from the United States (US) also found increasing age, female sex, chronic renal failure and congestive cardiac failure to be predictors of prolonged length of stay.5,6
Amid the increasing demand and pressure on NHS resources, reducing hospital LOS is a key priority for improving efficiency. This study aimed to identify independent patient and system-level predictors of prolonged LOS following shoulder arthroplasty across a large, nationally representative cohort. The findings aim to inform perioperative planning and, in turn, improve NHS efficiency.
Methods
Data source: Data was requested for all shoulder arthroplasty procedures from 1 April 2012 to 31 March 2022. The NJR has been routinely collecting shoulder arthroplasty data in England, Wales, Northern Ireland, the Isle of Man and the States of Guernsey since 2012. The dataset contains primary shoulder arthroplasty, demographic and surgical details. Data was also requested from the Hospital Episode Statistics (HES) database for the patients contained in the registry. The HES database contains every patient admission to an NHS hospital or publicly funded admission to an independent hospital in England. The dataset contains comorbidity data in the form of ICD-10 codes. Co-morbidities were identified at or prior to primary arthroplasty and used to calculate the Charlson comorbidity index (CCI), which will be used in the latter analysis (Supplemental Appendix 1). 7 These two databases were linked using the pseudo-anonymised NJR index number for the study. The HES dataset does not include privately funded procedures and associated admissions, and this accounts for a large proportion of the patients that are not matched in this study. Prior to merging, the number of arthroplasty procedures completed by each consultant on average per year in the registry was calculated, as well as the average number per year in the surgical unit.
Statistical analysis: LOS was calculated from the primary operation date in the NJR database to the discharge date in the HES database. Prolonged length of stay was defined as greater than the median length of stay for each shoulder arthroplasty subtype. The median LOS was consistent between implants at two nights, and therefore, greater than two nights was defined as prolonged. Demographics of patients receiving a shoulder arthroplasty in England are presented with descriptive statistics sub-grouped by implant type: reverse shoulder arthroplasty (RSA), total shoulder arthroplasty (TSA) and hemiarthroplasty (HA). Data is presented as a percentage, mean and standard deviation (SD) or median and interquartile range (IQR) dependant on the variable and data distribution. Demographics, age, gender, ASA, CCI, day of surgery, consultant cases per year, day of the week, as well as the individual co-morbidities that make up the CCI score were compared between groups with a prolonged LOS and those without. CCI was grouped into very low 0, mild 1–2, moderate 3–4 and severe.8,9 ASA was split into ASA 1–2 and 3–4. Cases per consultant per year were split into quartile groups (lowest 25% ⩽11.17 cases, 25%–50% 11.18–17.5 cases, 50%–75% 17.6–25.2 cases and 75%+ >25.2 cases). For analysis of risk factors, a univariable regression analysis was done for each demographic variable to assess for predictors of prolonged LOS. Significance was deemed if p < 0.050. A multivariable regression analysis was then performed, adjusting for all significant predictors to assess for independent risk factors for prolonged LOS. An interaction term was introduced between Age group and CCI, as the CCI score contains age as a component, potentially modifying its effect. The model with and without the interaction was tested using a likelihood-ratio test, which confirmed the interaction term improved the model fit (p = 0.008). The reference group originally was those patients <60 with a CCI of 0; however, the low sample size gave wide confidence intervals with unreliable estimates. To improve statistical robustness and clinical relevance, the group <60 with mild comorbidity (CCI 1–2) was used, which provided a larger, more stable baseline for comparison, ensuring more interpretable odds ratios. Additionally, the use of a group with some co-morbidity better reflects the shoulder arthroplasty population.
STATA statistics package (StataCorp, 2015. Stata Statistical Software: Release 14. College Station, TX: StataCorp LP) was used for the analysis. The STrengthening the Reporting of OBservational studies in Epidemiology (STROBE) guidelines were adhered to in this study. 10
Results
There were 47,145 shoulder arthroplasty procedures in the merged NJR and HES databases between April 2012 and March 2022. Figure 1 shows the cohort for analysis, and Table 1 shows the patients' demographic data. The median LOS for each implant was two nights, and therefore, prolonged LOS was defined as greater than two nights. A total of 30,620 (67%) of patients had a stay of two nights or less.
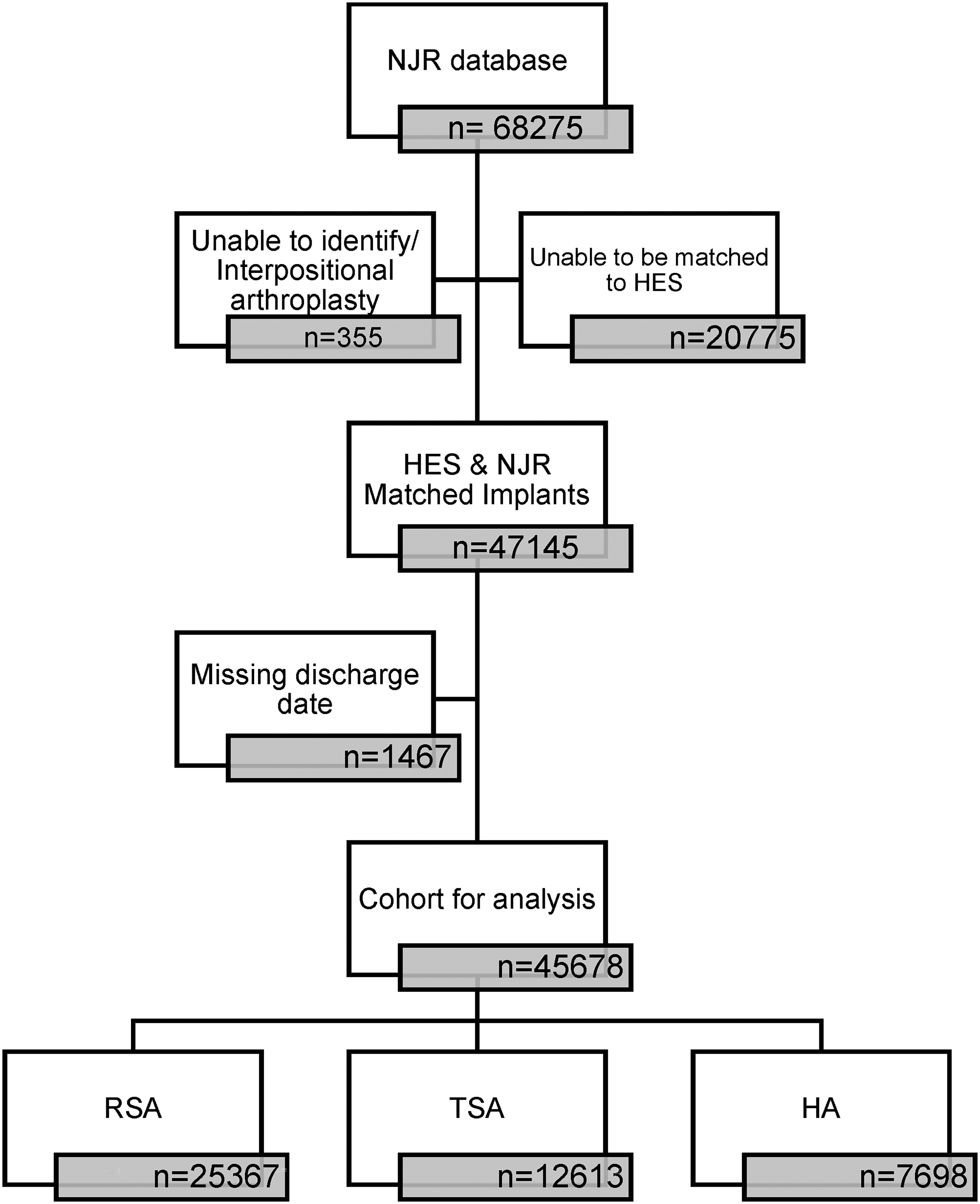
Study flow.
Demographics in patients with and without prolonged LOS.
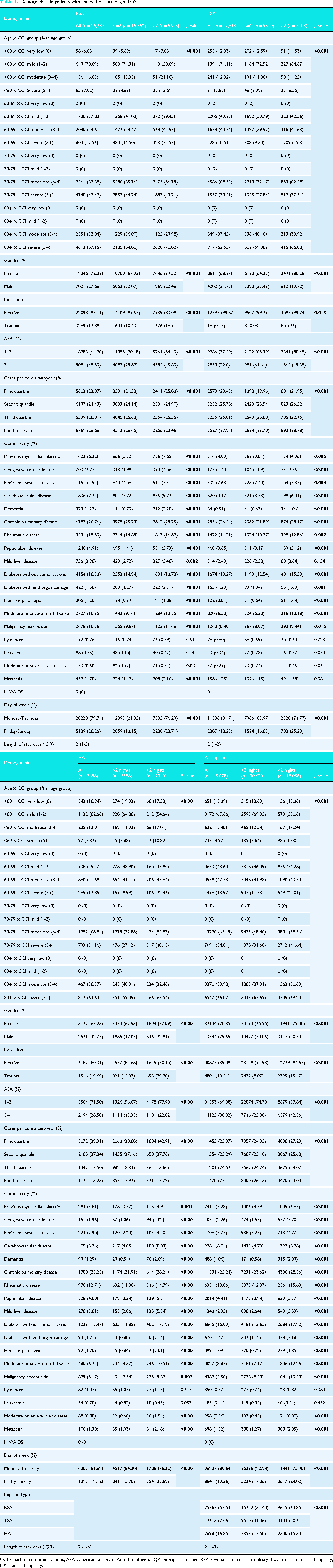
CCI: Charlson comorbidity index; ASA: American Society of Anesthesiologists; IQR: interquartile range; RSA: reverse shoulder arthroplasty; TSA: total shoulder arthroplasty; HA: hemiarthroplasty.
Patients with prolonged LOS were generally older, had a higher comorbidity burden, and more frequently were of ASA grades 3 and 4. Female patients were overrepresented in this group. Prolonged LOS was significantly associated with procedures performed Friday through Sunday, trauma indications and surgeries performed by lower-volume surgeons. If the implant was an RSA, this patient cohort was more likely to have a stay greater than two nights compared to the other implants (Table 1).
When completing univariable and multivariable regression models (Tables 2 and 3) to identify independent risk factors for prolonged LOS in shoulder arthroplasty, age and CCI score are independent predictors of prolonged LOS. The effect of CCI becomes more pronounced in older patients particularly over the age of 70 years, for example, a patient under 70 with a comorbidity scoring 1 point (group 60–69 × CCI moderate (3–4)) confers a 28% increased risk in prolonged LOS, whereas a patient over 80 with a comorbidity scoring 1 point confers a 294% increased risk. Patients under 60 with a score of 0 for comorbidities also had an increased risk of LOS across all implant types. Male patients had 45% lower odds of prolonged LOS compared to females (OR = 0.55), and those with an ASA of 3 and 4 had a 65% increased risk. If the procedure was done for trauma, this conveyed an approximate two-fold increased risk of prolonged length of stay. Consultant volume was an independent predictor of prolonged LOS, with those being operated on by higher volume surgeons having a decreased risk of prolonged stay (19% reduction in the top vs. the lowest quartile). Weekend surgeries (Friday–Sunday) were associated with 58% increased odds of prolonged LOS compared to weekday procedures (OR = 1.58). Individual comorbidities such as previous myocardial infarction, congestive cardiac failure, peripheral vascular disease, cerebrovascular disease, dementia, chronic pulmonary disease, rheumatic disease, peptic ulcer disease, liver disease, diabetes, hemi or paraplegia, moderate or severe renal disease and metastasis all conferred an independent risk for prolonged admission. The odds of prolonged hospitalisation were significantly lower for TSA (20% reduction) and HA (16% reduction) relative to RSA. When running the regression model by implant type, the above trends persisted, except for slightly different individual co-morbidity risk patterns (Table 3).
Univariable regression analysis.
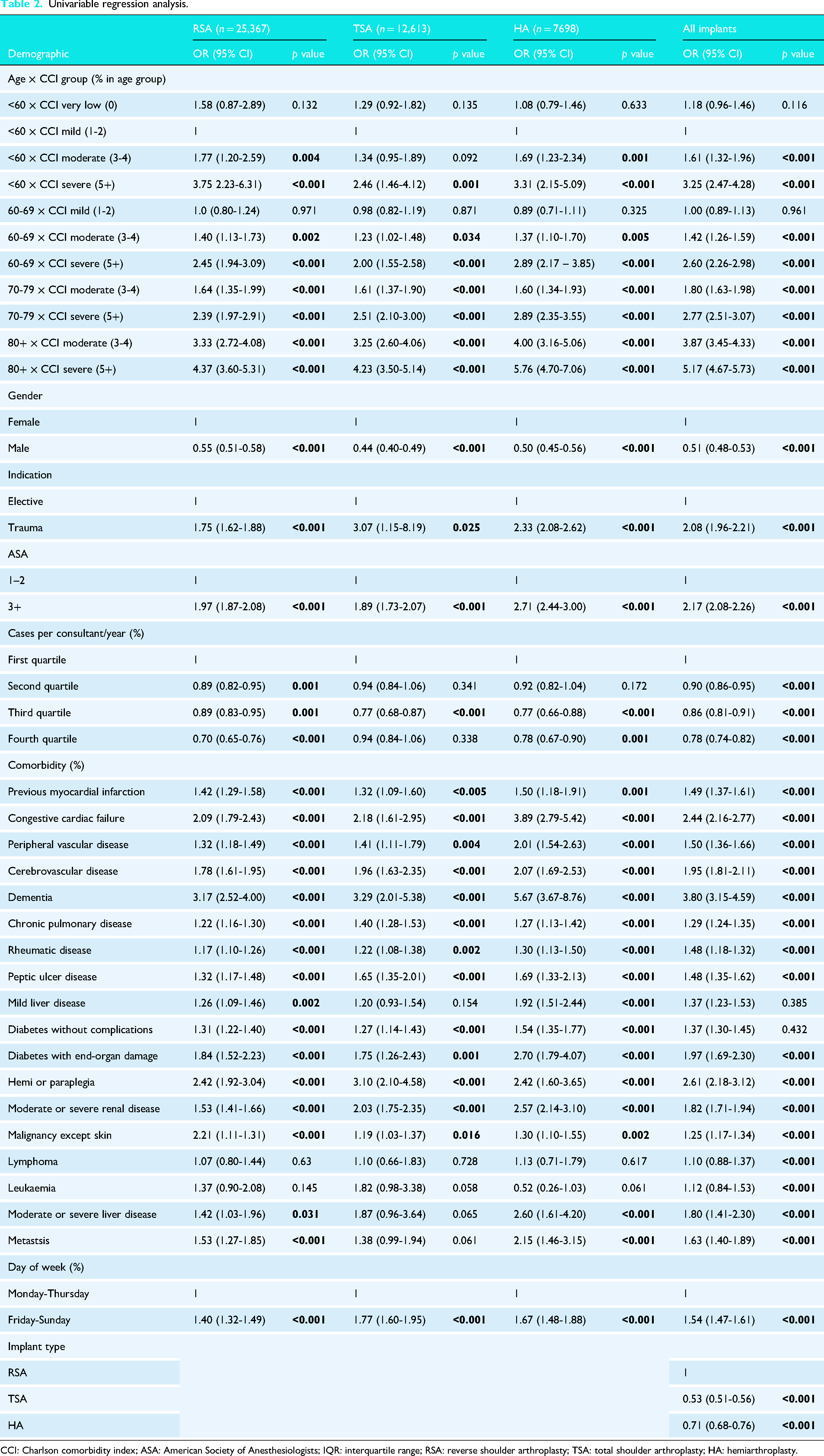
CCI: Charlson comorbidity index; ASA: American Society of Anesthesiologists; IQR: interquartile range; RSA: reverse shoulder arthroplasty; TSA: total shoulder arthroplasty; HA: hemiarthroplasty.
Multivariable regression analysis.
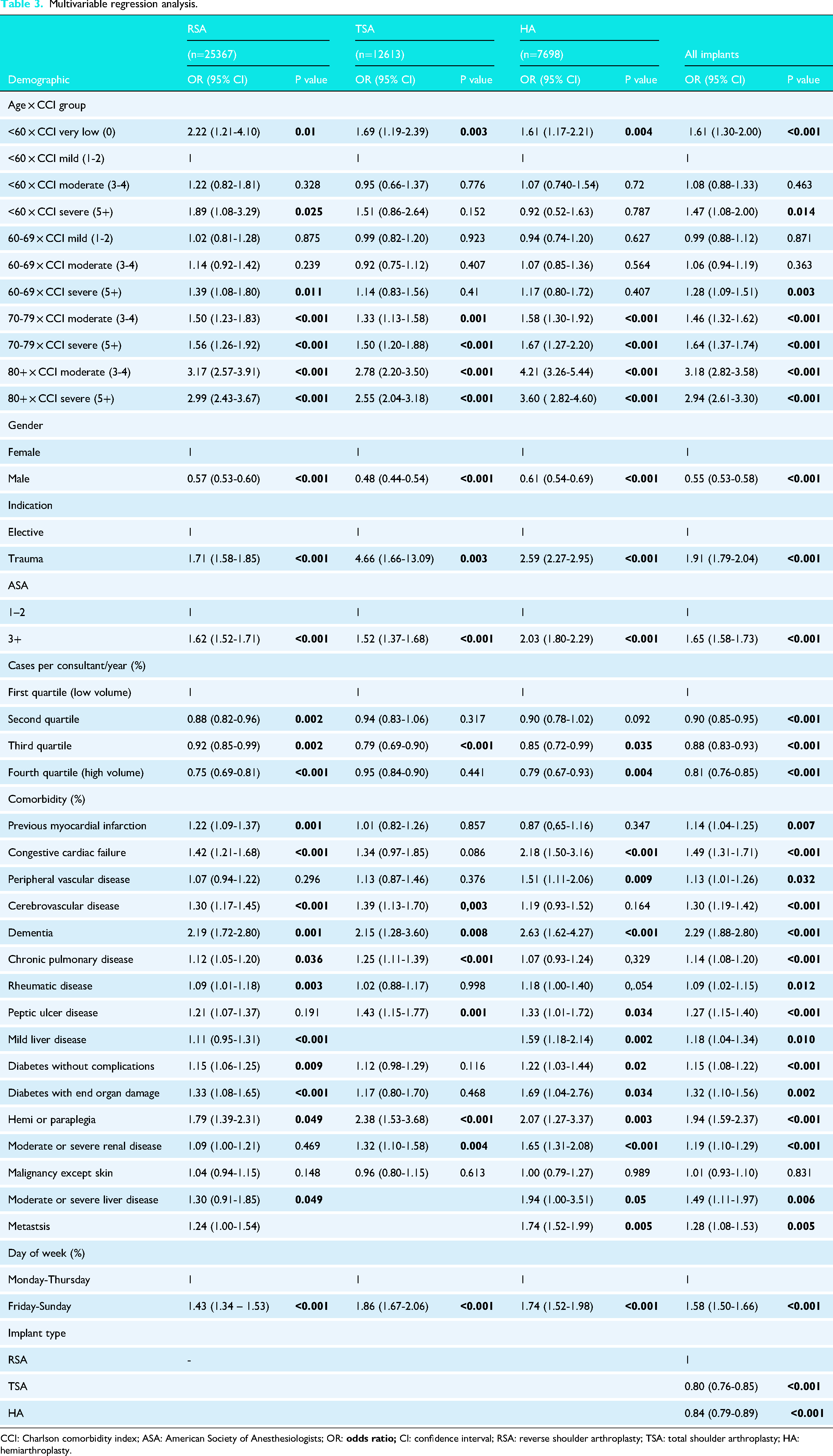
CCI: Charlson comorbidity index; ASA: American Society of Anesthesiologists; OR:
Discussion
This national population reflective study of over 45,000 shoulder arthroplasty cases showed that older age, higher comorbidity burden, female sex, trauma cases, and ASA grades 3 and 4 were associated with prolonged LOS. Surgeries performed on weekends (Friday–Sunday) and by lower-volume surgeons also increased the risk of prolonged LOS. While overall trends were consistent across implant types (RSA, TSA, and HA), individual comorbidities showed some variation in their predictive strength.
Studies conducted in the US have reported comparable predictors of prolonged hospital stay following shoulder arthroplasty. A study of 2004 TSAs showed age of >80, female gender, ASA >3 and renal disease and additionally, operative time >174 minutes to be independent factors in predicting prolonged LOS. 5 A further larger American study of 40,869 patients undergoing TSA and RSA (62.5% and 37.5%, respectively), found advanced age, female sex, and several comorbidities, including congestive heart failure, chronic pulmonary disorders, renal failure, and deficiency anaemia to be predictive of prolonged stay of >4 days in RSA and >3 days in TSA. 6 A risk prediction tool has been proposed in one US study for stay >3 days. The tool found age, marital status, fracture case, ASA score, paralysis, electrolyte disorder, BMI, gender, neurologic disease, coagulation deficiency, diabetes, chronic pulmonary disease, peripheral vascular disease, alcohol dependence, psychoses, smoking status, and revision cases, all factors that increased the risk of prolonged stay. 11 One UK study at a high volume centre showed that for 640 consecutive shoulder arthroplasty patients, linear predictors of length of stay were increasing age, female sex, chronic kidney disease, congestive cardiac failure, and previous myocardial infection, which are findings consistent with our study. 4 Additionally, intra-operative complications and postoperative transfusion were associated with longer stays. 4
In terms of non-patient factors, our finding that operative day was associated with increased LOS had also been shown in a US study of 1784 TSA and RSAs with a significantly longer LOS on a Friday compared to a Wednesday. 12 This may be attributable to reduced resources, for example, physiotherapy/discharge support day one postoperatively (Saturday), prolonging a patient's hospital stay. Planning and optimisation of services that enable hospital discharge at weekends may be strategies to reduce prolonged stays when patients are operated on Friday to Sunday. Weekend operating leading to a higher risk of prolonged LOS was independent of procedure type (elective vs. trauma); trauma cases were also an independent predictor of prolonged LOS, irrespective of the day on which they were operated on. For optimisation, this suggests that elective cases being done Monday-Thursday would have the lowest odds of requiring prolonged LOS, and this may be considered in theatre scheduling. A consultant volume of <10.4 cases per annum has been shown to result in a reduced risk of prolonged stay (>3 nights), a finding mirrored in this study, where there was a reduction in risk of 10%, 12% and 19% in quartiles 2, 3 and 4, respectively, compared to surgeons completing <11.17 cases per annum. 13 As well as surgical skill developed from a higher case load, higher volume surgeons have also been found to have a lower rate of medical complications requiring admission which would in turn lead to longer stays. 13 Consultant surgeon experience has also been associated with longer surgical times in orthopaedic surgery, and longer surgical times have been associated with longer hospital stays.14,15
Trauma cases were included in this study to reflect national practice and to evaluate their independent contribution to prolonged LOS. Trauma-related shoulder arthroplasty is known to be associated with prolonged LOS, likely due to unplanned admission, concomitant injuries, physiological stress and more complex discharge planning compared to elective indications.4,16 Multivariable regression analysis demonstrated that trauma indication remained an independent predictor of prolonged LOS after adjustment for patient factors, implant type, surgeon volume, and operative timing. Importantly, RSA also remained independently associated with prolonged LOS when trauma indication was accounted for, indicating that the observed prolonged LOS in RSA was not solely driven by indication. In the context of the NHS, where there is increasing pressure to deliver ambulatory or short-stay upper limb trauma care due to bed shortages, evaluation of this cohort is particularly relevant. Inclusion of trauma cases, therefore, provides clinically meaningful information for perioperative planning, risk stratification, and service delivery, rather than representing a methodological limitation.
These findings support incorporating LOS risk profiling into preoperative planning and scheduling strategies. For example, older female patients with comorbidities could be targets for medical optimisation of conditions such as diabetes, as well as social support planning to reduce the risk of a delayed discharge. Departmentally, it may be considered that these patients are operated on by higher volume surgeons to improve discharge time. It has been shown in the US that modifying medical factors pre-operatively can reduce readmissions, length of stay and are cost saving. 3 It may also be a consideration to operate on these higher-risk patients earlier in the week (Monday–Thursday), so this does not become a contributing factor to a delayed discharge.
This study has several limitations inherent to large-scale, retrospective database analyses. Limitations to this study lie within the data and its merging. Merging of the NJR–HES databases, while allowing for a nationally represented cohort, may result in missing or incomplete data (e.g. discharge dates and implant classification), which could affect analysis. Important clinical and social factors such as frailty, functional status, socioeconomic background, discharge destination, and home support, which may affect length of stay, are not captured in these datasets and should be considered when planning patient stay. The NJR and HES databases also rely on accurate coding and inaccuracies or consistencies in ASA and comorbidity documentation, for example, are possible in administrative datasets. Finally, whilst surgeon volume is accounted for in this study, averaging cases across time may not fully capture temporal trends in clinical practice or team-based care variations.
Conclusion
This large population-based study of over 45,000 shoulder arthroplasty cases identifies patient-level (age, comorbidity burden, ASA score and trauma indication) and system-level (weekend surgery and surgeon volume) variables that are independently associated with prolonged LOS following shoulder arthroplasty. The findings of this study can aid pre-operative risk stratification, target optimisation for modifiable conditions and aid with surgical scheduling to reduce LOS, improve outcomes, and ease pressure on NHS resources. Targets for future research would be further investigation into functional outcomes or social determinants of discharge that were beyond the scope of this study.
Previous publication/meeting
Not applicable.
Supplemental Material
sj-docx-1-sel-10.1177_17585732261425994 - Supplemental material for Predictors of prolonged length of stay in shoulder arthroplasty: A study using the National Joint Registry and Hospital Episode Statistics for England
Supplemental material, sj-docx-1-sel-10.1177_17585732261425994 for Predictors of prolonged length of stay in shoulder arthroplasty: A study using the National Joint Registry and Hospital Episode Statistics for England by Olivia O’Malley, Andrew Davies, Amar Rangan, Sanjeeve Sabharwal and Peter Reilly in Shoulder & Elbow
Footnotes
Acknowledgements
We thank the NJR research committee and staff at the NJR for facilitating this work. The authors have conformed to the NJR's standard protocol for data access and publication. The views expressed represent those of the authors and do not necessarily reflect those of the NJR steering committee, research subcommittee, or HQIP.
Ethical approval
This study used pseudo-anonymized, routinely collected data from an established clinical registry, and patient consent was obtained by the NJR. According to Health Research Authority guidance, ethical approval was not required.
Funding
The authors disclose receipt of the following financial or material support for the research, authorship, and/or publication of this article: An institutional British Elbow and Shoulder Society pump primer research grant, and a Royal College of Surgeons Research Fellowship.
Declaration of conflicting interests
The authors declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: Olivia O’Malley is an RCS England Research Fellow funded by The Arthritis Research Trust Research Fellowship with support from the Rosetrees Trust. Amar Rangan reports an institutional grant from NIHR and AO UK & I, as well as research and educational grants from DePuy J&J Ltd, unrelated to this study. Amar Rangan is also an Elected Trustee of the British Orthopaedic Association and is on the funding committee of NIHR i4i.
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
