Abstract

The Public Health Challenge
Cancer outcomes in the UK are significantly behind those in some other European and high Human Development Index countries. 1 Evidence points to later stage diagnosis as one reason for this. 2 Cancer survival rates are strongly associated with stage at diagnosis, with earlier stage disease leading to longer survival. 3
Effective communication between patients and primary care clinicians is vital for early cancer detection as open dialogue enables accurate articulation of symptoms and timely clinical responses. However, communication barriers disproportionately affect marginalised populations, 4 including the African and Caribbean communities in the UK. These barriers, shaped by cultural differences, systemic bias, and historic mistrust of healthcare systems, likely contribute to delays in help-seeking and late-stage diagnoses, particularly for conditions such as head and neck cancers (HNCs), which often present with vague symptoms.
Head And Neck Cancer
HNC’s occur in a many areas within the head and neck including the mouth, pharynx and larynx; they are now the eighth most common cancer and are increasing. 5 There is currently no effective screening approach, therefore patients are normally diagnosed due to the presence of symptoms. However, symptoms are often vague (e.g.: neck lump, persistent sore throat, hoarseness, non-healing ulcers) and patients can present at a GP or dentist. For communities with additional layers of social and cultural complexity, these symptoms may be misunderstood or deprioritised, and this is further exacerbated by barriers to access to GPs. This public health challenge calls for interventions that are not only medically informative but also culturally attuned and community led.
Patient Empowerment And Health Equity
Patient empowerment is a recognised strategy to reduce health inequalities. 6 It centres on giving individuals greater control over their health and building confidence to navigate health systems better. Empowerment is particularly critical in cancer care, where early symptom presentation can significantly affect prognosis. Yet, many health communication initiatives are clinician-driven, often failing to resonate with the nuanced realities of marginalised communities. Culturally responsive and participatory methods could help bridge this gap. 6
Forum Theatre As A Tool For Health Communication
Forum Theatre 7 is an interactive form of performance that enables participants to explore real-life scenarios and rehearse alternative responses. It has been applied in various health contexts, 8 offering a structured yet flexible method to address sensitive issues and systemic power imbalances.
This project applied Forum Theatre to address delayed presentation of HNC symptoms within African Caribbean communities. Through watching scenarios, participants (audience members) could then engage in rehearsals of difficult healthcare conversations, practicing how to voice symptoms and concerns effectively. This method encourages both skill-building and reflection, fostering a deeper sense of agency.
Project Description
The production was underpinned by the authors’ (JD and LS) empirical research. Four in-person sessions and two online sessions were held with six representatives from the Afro-Caribbean community in Leicester, in partnership with Oracle, a Head and Neck Cancer charity. Sessions were also attended by a head and neck cancer surgeon. The sessions focused on exploring barriers and facilitators to accessing primary care, specifically in relation to GPs and dentists, with an emphasis on prioritising the most significant barriers.
The workshops were run (by JD and NP) over 3 months. One session included a virtual meeting between the community representatives and the theatre company. Scenes were developed by the theatre company (TSF) and the researcher (JD) using information from these sessions and the research findings.
The final session comprised two main components. The first featured two scenes devised and performed by the community representatives. These scenes explored culturally specific responses to illness, including consulting traditional healers, relying on prayer, perceptions of racism, and reliance on herbal remedies. The second was a traditional Forum Theatre element that depicted key moments in the diagnosis pathway: recognising symptoms and discussing them with family, deciding to make an appointment, interacting and communicating with a GP when seeking help for symptoms, and interacting with a dentist when cancer is found as an incidental finding while seeking help for tooth pain. Each scene was introduced and facilitated by a member of the theatre company. Audience members were invited to ‘meet’ the characters, discuss their situations, and recommend different courses of action. The scenes were then replayed by the actors, with the audience giving the characters new directions and words to say. Clinicians were involved throughout the process, including a GP who assisted the theatre company during development and rehearsals.
The final session took place at a community venue. Prebooking was required, although no one was turned away if they hadn’t booked. A multidisciplinary panel was convened after the performance, comprising a dentist, researcher (JD), HNC surgeon (OO), and religious leaders from the community. Although GPs were invited, none attended. A community meal was provided after the session to continue conversations. Throughout the evening, support was on hand for anyone experiencing distress or concerns. Information about support networks was also made available for those who wished to seek support post the session.
Preliminary Outcomes And Reflections
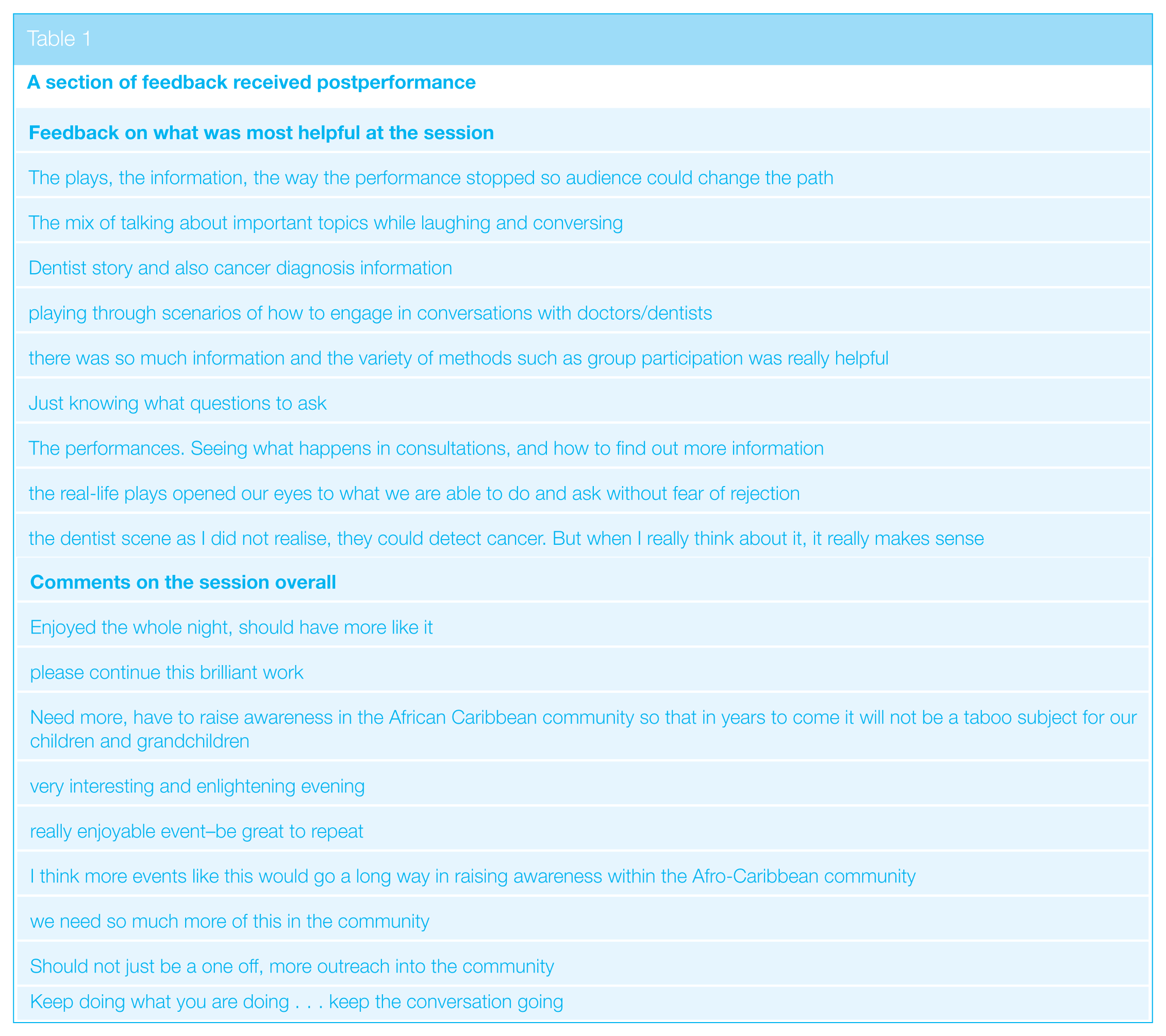
Sixty people attended the final session. Audience members were invited to complete feedback forms; 45 did so (Table 1). All reported that postsession, they felt more confident discussing cancer with family and friends, GPs, and dentists. They reported that the session was very helpful and informative, providing entertainment, information, and the ability to interact, and that they felt that this was something which should be repeated.
A section of feedback received postperformance
Discussion
Forum Theatre offers a compelling model for addressing communication barriers within healthcare. Its emphasis on experiential learning and co-production aligns with broader calls for equity in public health intervention design. By centring the lived experiences of Afro-Caribbean individuals, this approach contributes to a more inclusive model of cancer awareness and early detection.
However, rigorous evaluation is necessary to assess its replicability and long-term impact. Questions remain about how best to integrate such methods into wider public health strategies and primary care education.
Conclusion
This Forum Theatre project demonstrates the potential of culturally tailored and participatory methods in addressing health inequalities in cancer. As public health initiatives increasingly seek to engage marginalised communities, innovative approaches like this can help reshape narratives around help-seeking and empower patients to act earlier on potential cancer symptoms.
Footnotes
Acknowledgements
The authors would like to thank the actors involved in the development of the forum theatre scenes – Sarah Kemp, Tony Neilson, Marva Alexander, Wayne Nelson, Becky Jameson and Claire Webster. The authors would also like to thank Dr Paula Bradley (GP and Head and Neck Cancer Researcher) for her support during rehearsals and scene development in making sure the GP role was accurate.
Conflict of Interest
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The research which funded this Forum Theatre production was funded by Newcastle University (PhD studentship: J Deane) and the National Institute for Health and Care Research (NIHR) under the Research for Patient Benefit programme [NIHR201966]. LS is funded by the NIHR Newcastle Patient Safety Research Collaboration. The views expressed are those of the author(s) and not necessarily those of the NIHR or the Department of Health and Social Care.
The development of the forum theatre element was funded by Gilead ‘Look and you will see us’ Grant, as well as additional funding from University Hospitals Leicester NHS Trust.
