Abstract
Background:
The Traveller population is a distinct minority ethnic group, formally recognised by the Irish Government in 2017. Irish Travellers have a lower life expectancy and poorer health expectancy than the general population. Internationally, HPV self-sampling is being considered as an option to improve uptake in cervical screening, particularly in underrepresented groups. It is not currently offered in Ireland, but assessment of acceptability is ongoing. The aim of this study was to determine the uptake of cervical screening and the acceptability of HPV self-sampling in eligible Traveller women.
Methods:
A face-to-face survey by and with Travellers, adapted from the National Cancer Control Programme’s (NCCP) 2022 National Survey on Cancer Awareness, was conducted by Traveller Community Health workers in partnership with Pavee Point Traveller and Roma Centre.
Results:
483 Travellers participated; 306 (63.1%) were women and 191 (39.5%) were in the eligible group for cervical screening (women aged 25-65). Of these, 142 (74%) had ever received an invitation; of those who received an invitation, 125 (89%) attended at least once. Over 73% of those attending cervical screening advised they attended all screening appointments. 37 (19.4%) reported HPV self-sampling as acceptable, 87 (45.5%) as unacceptable to them and 31 (16.2%) were unsure and would like more information. Of the 37 who reported HPV self-sampling as acceptable, 18 (50%) were non (7) or irregular (11) attenders at screening.
Conclusion:
HPV self-sampling has the potential to overcome, for some Traveller women, the practical and personal barriers which may prevent them from responding to standard cervical cancer screening.
Keywords
Introduction
The Traveller population is a distinct minority ethnic group, formally recognised by the Irish Government in 2017. Irish Travellers make up less than 1% of the total population of Ireland at just under 33,000, according to 2022 census data. 1 This may be an underestimate, as the All-Ireland Traveller Health Study (AITHS) 2 reported 40,129 Travellers living in Ireland. Irish Travellers have a lower life expectancy and poorer health expectancy than the general population.2,3 According to AITHS, almost 20% of all deaths in Travellers are cancer-related, underlining the importance of focusing on cancer prevention and early cancer detection, aiming to reduce mortality and morbidity. 2 The impact of the Social Determinants of Health on health and disease has long been identified as having a significant influence on health, a finding supported by the AITHS.2,3 In the most recent national census, the average age of Irish Travellers was 27 years compared with an average age of 39 for all people living in Ireland. 1 Children under the age of 15 made up 20% of the total population but 36% of Irish Travellers. Unemployment is very high among Travellers compared to the general population. 2
The AITHS 2 found that Travellers experienced discrimination in their use of health services in general. Most respondents (66.7%) agreed either that it sometimes occurred (40.1%) or more often than that (26.6%). Perceived discrimination starts early, with 62.1% and 67% of Travellers reporting discrimination in school. Traveller educational status has been recorded repeatedly as considerably lower than that of their general population peers, to an extent unmatched by any other community in Irish society. 2
CervicalCheck is the Irish national cervical screening programme for women aged 25–65 years. Human papillomavirus (HPV) primary screening was introduced by CervicalCheck in 2020. Eligible women can attend any one of 1400 registered sample takers across Ireland, including GPs and Well Woman clinics. Those eligible, including all Traveller women in the eligible age group, should receive a letter from the programme advising them to make an appointment. The list of registered sample takers is on the CervicalCheck website, where users can also check when their next appointment is due and update their address details.
Internationally, HPV self-sampling is being considered as an option to improve uptake in cervical screening, particularly in underrepresented groups. It is not currently offered in Ireland, but assessment of acceptability is ongoing. 4 It is becoming routinely available in several high-income countries with long-standing cervical screening programmes and has the potential to increase the uptake of cervical screening among under-screened women.
A 2018 review confirmed that self-collected HPV samples showed reasonably high diagnostic accuracy. 5 The aim of this study was to determine the uptake of cervical screening and the acceptability of HPV self-sampling in eligible Traveller women. Specific objectives included documentation of cervical screening participation in the eligible age group (receipt of letter of invitation, attendance, frequency of attendance) and documentation of potential barriers to cervical screening, such as unreliable/non-receipt of post and poor literacy, both potential barriers to health service engagement.
Methods
This was a co-designed study developed and conducted in partnership with Pavee Point Traveller & Roma Centre (a national, non-governmental organisation committed to the attainment of human rights for Irish Travellers and Roma), the Irish Health Service Executive (HSE) National Cancer Control Programme (NCCP) and the HSE National Social Inclusion Office. A questionnaire was adapted from the NCCP’s 2022 National Survey on Cancer Awareness and modified to enhance clarity, based on feedback from Traveller Community Health Workers (TCHWs). 6 The sample of Travellers to be recruited for the cross-sectional survey was initially based on representation from the North, South, East and West regions of the Republic of Ireland. This recruitment strategy was based on the number of Travellers in each area in accordance with 2016 census data (2022 data unavailable at that time) and in consultation with Pavee Point Traveller and Roma Centre. Consistent with the methodology used in previous studies with Travellers, 2 we collaborated with Primary Health Care for Travellers Projects (PHCTPs) across Ireland to recruit TCHWs to act as peer researchers to undertake data collection. Detailed training on the completion of the questionnaire was provided separately to TCHWs in each PHCTP to ensure questionnaire understanding and to facilitate comprehensive, consistent, accurate data collection. Survey data were collected by the TCHWs using hard copy questionnaires, completed in person with each respondent. Data collection took place from 11th July to 24th November 2023. One coordinator in each PHCTP was responsible for overseeing data collection. Written informed consent was obtained prior to the completion of each survey. All data were anonymised.
Traveller women in the eligible age group for cervical screening were asked about their receipt of a letter of invitation, attendance at screening and if they attended every time they were invited. The specific question included about HPV self-sampling was, ‘If asked, would you take a test (swab (like using a longer cotton bud) of your vagina) at home yourself?’ The answer options provided were: (1) Yes, this is a good idea, and I would like more information, (2) No I would never do this, (3) Unsure and I would like more information and (4) Refused to answer. Informed consent was obtained from all respondents. Respondents self-reported literacy and were asked about postal deliveries.
Descriptive analysis was carried out using SPSS version 29.
Results
A total of 483 Travellers participated in the survey overall. In total, 306 (63.1%) were women, and 191 (39.5%) were in the eligible group for cervical screening (women aged 25–65 years). Of these, 142 (74%) had ever received an invitation; of those who received an invitation, 125 (89%) attended at least once. A high proportion of those attending cervical screening advised they attended all screening appointments (Table 1).
Uptake of cervical screening among those eligible for cervical screening (N = 191)
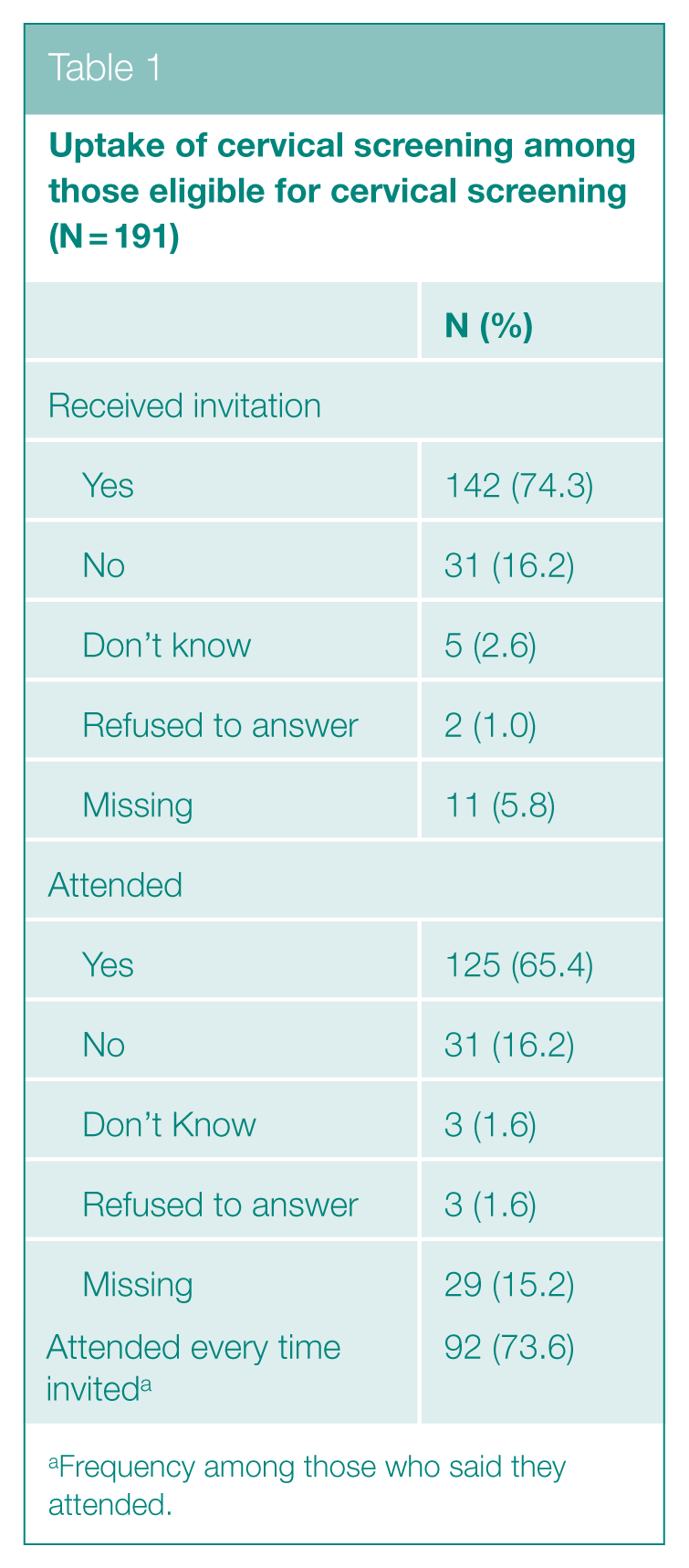
Frequency among those who said they attended.
In total, 37 (19.4%) reported HPV self-sampling as acceptable, 87 (45.5%) as unacceptable to them and 31 (16.2%) were unsure and would like more information. Of the 37 who reported HPV self-sampling as acceptable, 18 (50%) were non- (7) or irregular (11) attenders at screening. Similar proportions of 25- to 45-year-olds (18.5%) and 45- to 65-year-olds (20.5%) would use HPV self-sampling. Of the 87 (45.5%) who reported HPV self-sampling as unacceptable, 62 (71.3%) were previous participants in cervical screening.
In total, 125 (65.4%) of the 191 eligible women reported a literacy level whereby they can usually read and fill out forms; the majority (156 (81.7%)) have direct post to home.
Discussion
Previous studies have examined preferences for HPV self-sampling versus clinician-sampling in the context of cervical screening, but, to our knowledge, this is among the few to address acceptability in a minority ethnic group. The overall acceptability among eligible Traveller women in this study was 19.4%, which compares with 51%–54% in a general population study. 6
Half of those open to HPV self-sampling were non- or irregular attenders at CervicalCheck. These findings suggest that, while self-sampling should not replace clinician-sampling as the standard of care, it has the potential to increase uptake in under-screened Traveller women.
It is clear that Traveller women are engaged with the cervical screening programme, but there is room for more engagement. In this study, we asked whether Traveller women had ever attended screening, which was 73% overall; the measure of 5-year coverage used in the general population was not captured in this study. 7
HPV self-sampling has the potential to overcome, for some Traveller women, the practical and personal barriers which may prevent them from responding to standard cervical cancer screening. Discrimination (both systemic and individual) plays a significant role in poor experience of and non-engagement with health services in Traveller populations. 2 Should HPV self-sampling be introduced by CervicalCheck, it would require careful consideration of how Traveller women can access and use it successfully. There are barriers to participation in the existing screening programme by Traveller women that may equally be barriers to a self-sampling approach, including access to postal services and literacy. A systematic review showed that delivering self-sampling kits via community outreach workers increased participation in cervical cancer screening. 8
Home test kits are in use in other settings in Ireland, including the BowelScreen programme and home testing for sexually transmitted infections (STIs) with varying results; in the younger age cohort, home STI kits are popular, 9 whereas the BowelScreen programme, which targets an older age group, has the lowest uptake of our three national population cancer screening programmes at 46.6%. 10 In another part of this study, we found that lower proportions of Travellers agreed/strongly agreed with the statement ‘There are things I can do to reduce my risk of developing cancer’ than in the general population (NCCP report) (77% versus 90% overall with 43% versus 55% strongly agreeing).
The strength of this study was the partnership with the Traveller community across Ireland, resulting in a greater than expected sample size overall; the limitation is that this was not a fully nationally representative sample. The other limitation is that we cannot be certain that all Traveller women asked would have understood fully the question about HPV self-sampling; this question replicated the self-sampling question asked in a national study but with additional explanation.
Conclusion
HPV self-sampling has the potential to overcome, for some Traveller women, the practical and personal barriers which may prevent them from responding to standard cervical cancer screening. Travellers face barriers to accessing mainstream health services, so ways must be developed to ensure access to screening for all, following informed consent. The potential of introducing HPV self-sampling to the Traveller population (as part of a general introduction in Ireland) would have to be examined carefully in partnership with Traveller advocacy organisations, Traveller women and PHCTPs to see how this might work in practice, once a decision to introduce HPV self-sampling is made. There is also a need for universal ethnic identifiers to facilitate routine monitoring of access, participation and outcomes in Travellers in relation to cancer screening programmes.
Footnotes
Conflict of Interest
The authors declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Funding
The authors disclosed receipt of the following financial support for the research, authorship and/or publication of this article: Funding for this study was provided by the HSE National Cancer Control Programme, Ireland.
Ethics
Ethics approval for this study was granted by the Royal College of Physicians of Ireland on 4th May 2023 (RCPI RECSAF 191). Approval was also received from the Pavee Point Research Advisory Committee.
