Abstract
Aims:
People on probation, considered an inclusion health group, face significant barriers to accessing healthcare including stigma and lack of appropriate services. Better data are needed to evidence this population’s needs and the quality of care that they receive from probation staff and healthcare commissioners and providers. This article aims to describe the development of standards and quality indicators linked to objectives within a probation health and social care strategy, which can contribute to filling this evidence gap and inform wider initiatives to support improved health in people on probation.
Methods:
The standards and indicators were developed using a modified RAND approach. This combined a systematic scoping review and input from professionals and individuals with lived experience of probation to identify the characteristics of high-quality care and create measures of them.
Findings:
A set of 22 standards and 31 quality indicators were developed which could be used routinely to measure the quality of care (structures, processes and health outcomes) for people on probation – highlighting good practice and where improvements are needed (e.g. to overcome barriers to access to care). Findings could inform cross-agency quality improvement initiatives to address areas where standards are not being met.
Conclusions:
A set of standards and indicators has been developed that can be used as a framework for quality improvement work to improve the quality of care (including health outcomes) for people on probation. Further research is needed to pilot the measures within probation and to investigate (1) perceptions of their acceptability and feasibility for use within routine practice and (2) how they can inform quality improvement work by probation, public health and other professional groups to address areas where standards are not being met, and through this, improve the health of people on probation.
Introduction
A Public Health England report identified that ‘compared with the general population, people in contact with the criminal justice system have significant health and social care needs and can face significant barriers to accessing services’. 1 A small body of research suggests that people on probation are likely to experience many of the negative social determinants of health, worse (healthy) life expectancy than the general population, and have complex health needs, with rates of drug and alcohol misuse, mental illness, neurodiversity, suicide, and self-harm being higher in this population than in the general population.1–9 Inclusion health is ‘an umbrella term used to describe people who are socially excluded, who typically experience multiple interacting risk factors for poor health’. 10 Inclusion health groups include people in contact with the criminal justice system, and people experiencing homelessness and/or drug and alcohol dependence. Consequently, people on probation fit this definition and should be a priority for public health intervention.
Reducing health inequalities is a priority for NHS England who state that ‘delivering effective services that address the issues faced by inclusion health groups is an important contribution to this ambition’. 10
The Probation Service in England and Wales is a statutory service that advises the courts on sentencing through preparation of presentence reports, contributes to preparation for release from prison, and manages people serving community sentences, in prison, released on licence, and subject to postsentence supervision. This includes supervising people living in the community and in probation Approved Premises across four tiers of risk. Probation practitioners in this Service are civil servants that undertake probation-specific professional training to perform a dual role consisting of protecting the public (including risk assessment, working with other agencies as part of Multi-Agency Public Protection Arrangements, and enforcement of sentences) and supporting rehabilitation. Community orders supervised by probation may include numerous requirements such as community payback, accredited programmes, community sentence treatment requirements, curfews, and electronic monitoring. The Service is committed to improving the health of people on probation, and this is believed to contribute to both the public protection and rehabilitative elements of probation’s role. 11
People on probation should be able to access health and social care in the same way as the general population. However, factors such as stigma, poor past experiences and a lack of appropriate service provision mean that despite a high level of need, many people on probation find it difficult to access services and over-use crisis services.12–14 This may be further complicated at a local level. For example, in Wales there are longer waiting lists than in England and while responsibility for health is devolved to the Welsh government, responsibility for justice is not. 9
The benefits of improving the health of people on probation stretch beyond individual improvements in health and wellbeing, encompassing wider societal benefits like reductions in re-offending, avoidable use of crisis care, and health inequalities. 1
Direct provision of care is not within the remit of probation practitioners in England and Wales but contact with the probation service does offer an opportunity to help improve access to services for this marginalised population. Indeed, probation practitioners perform a health-related role involving identifying health-related drivers of offending behaviour and facilitating access to services to improve the health of people on probation. This includes supporting people on probation to register with a GP; considering health needs in sentencing recommendations such as the use of Community Sentence Treatment Requirements (CSTRs – Alcohol Treatment Requirements (ATRs), Mental Health Treatment Requirements (MHTRs) and Drug Rehabilitation Requirements (DRRs)); working on the Offender Personality Disorder Pathway, and supporting postcustodial continuity of care. Probation practitioners are not expected to be health experts, and as such, this role is conducted through partnership working with health and social care agencies.
When this study was conducted, the most up-to-date description of this role was in the National Probation Service (NPS) Health and Social Care Strategy. 11 This has since been echoed in a recent partnership agreement 15 and the probation workforce has been expanded to include HMPPS Health and Justice Partnership Managers and Coordinators, who focus on building partnerships with health and social care agencies to support access to care and treatment for people on probation. Arguably, meeting the Health and Social Care Strategy objectives will lead to improved health outcomes for people on probation.
People in inclusion health groups are often invisible in health data sets. 10 Currently, while probation practitioners do record some data about the health of people on probation, this is not always consistently done and data that are recorded are often based on simple self-report rather than established screening tools. 1 Such data rarely inform joint strategic needs assessments (which inform service commissioning decisions in England and Wales). Perhaps partly as a consequence of this, services that are accessible to people on probation and capable of catering for the complex needs that many in this population have, are not always available. There is also a lack of evidence on the most effective ways of improving the health of this population and of the quality of health and social care that they receive.16–18 We aimed to create standards and quality indicators that could form the basis of future work to address these issues.
Quality indicators are used in numerous settings, including within the criminal justice system to measure and improve the quality of health and social care. They can be used within plan, do, study, act cycles – providing measures of the quality of care at baseline and after improvement activities have been introduced. They are often classified into measures of three aspects of care quality – structure (attributes of care settings like material and human resources and organisational structure), process (what actually occurs in interactions between practitioners and those receiving care such as making a referral or diagnosis or administering an intervention), and outcome (health status, quality of life, knowledge, behaviours, satisfaction and experience) indicators.19,20 Evidence for such measures can be based on the literature or on consensus of expert opinion. Quality indicators can measure adherence to recommended practice, identify areas for improvement and variations in practice over time and place, enable identification of good practice, and guide improvement initiatives.20,21 While they are used in UK prisons and in Community Justice Scotland, no such measures are currently routinely used in probation in England and Wales.
We aimed to create standards and quality indicators linked to probation’s health-related role as described above, that is, to enable users to evidence whether the right structures and processes are in place for probation practitioners to achieve the objectives in the NPS Health and Social Care Strategy 1 (and through this, improve the health of people on probation). We believe that introducing such measures will also enable the creation of an evidence base that is currently lacking on what high-quality care looks like within this context and whether it is being delivered. We envisage that the measures could be used as part of a quality improvement approach to identify where improvements to practice are needed. Indicators measuring health status and outcomes will facilitate assessment of the impact of new (multi-agency) approaches to improving the quality of care and health outcomes for people on probation in areas identified as needing improvement. Thus, introducing such measures should support inclusion health principles and provide a framework to test new approaches and facilitate learning on how to improve care quality and outcomes for people on probation, ultimately leading to better care and better health for this group. This article describes the development of these quality indicators.
Methods
To develop the measures we followed a modified RAND method, 22 adapting it slightly to better fit the context of the study, as described below. This is a consensus technique that builds on the original RAND procedure commonly used to develop standards and indicators. It combines existing measures identified in a literature review with lived experience and expert (professional) perspectives on what ‘high-quality care’ looks like within a given field (Figure 1). This approach was selected to ensure that the measures have good face validity – being based on lived experience input and consensus from professionals across the criminal justice and health field, are feasible for use in probation practice (using existing data where possible), and utilise existing measures employed in other adult criminal justice settings where appropriate.

Modified RAND approach to quality indicator development.
Overall, data were collected between November 2021 and December 2022, and participants provided informed consent for all elements. Using our professional networks and publicly available contact information, we invited people to join a professional panel. Potential participants were purposively selected to represent a variety of relevant roles. Our panel of 15 professionals was a geographically diverse group of individuals performing roles at local and national levels in probation (experience at frontline and managerial levels), primary care (in community and prison settings), public health, academia, justice policy and the probation inspectorate. The panel completed an online survey. This shared the probation health and social care strategy objectives and asked open questions on what respondents considered the characteristics of high-quality health and social care for people on probation to be (what standards should be met), and how they could be measured (what quality indicators should be used) in relation to these objectives.
We also conducted a focus group with a purposive sample of seven people selected because they had lived experience of being on probation and their contact with the criminal justice system was driven by multiple unmet health and social care needs. Participants were asked to consider the same issues as the professionals and were also asked about their experiences of discussing health and accessing care while on probation, and what they thought probation practitioners should know about their health.
Both groups were asked to share details of any quality indicators that already exist within other parts of the UK criminal justice system or in probation internationally that could be used or adapted for use within probation in England and Wales.
The focus group was transcribed verbatim, and qualitative survey data were extracted into Word files. Data from the survey and focus group were coded by academics and people with lived experience of being on probation using thematic analysis. 23 The team familiarised themselves with the data and conducted line-by-line coding to represent the meaning of each line. Initial codes were then grouped into themes representing the characteristics of high-quality care and suggested ways of measuring them. These themes were reviewed and refined through group discussion.
Alongside this, we conducted a systematic scoping review to identify existing quality indicators, guidelines, and performance measures used in other adult criminal justice settings that could be relevant to the probation strategy objectives. 24 Any specific existing measures suggested by the professional and lived experience panels were included in the literature review as grey literature.
Findings from these three strands were then combined. A draft set of standards was created to reflect the characteristics of high-quality care identified by the professional and lived experience panels. Quality indicators were created to measure the standards. Where possible, this was done with reference to existing standards and indicators identified in the scoping review. The draft list was shared with key groups within the probation service for feedback and rated on three criteria by the professional panel. The list was then ranked and shortened by mean score, with those receiving the highest mean scores being further discussed by the professional panel. Feedback was also provided on specific indicators by people with suicide prevention expertise within probation. Finally, amended indicators were rated by the panel for a second time and a final set of indicators were selected. The approach taken in Steps 1–3 has been described fully in our previous publications.24,25 An illustrated example of the process is available in Supplemental Material.
Results
Characteristics of high-quality care
There was considerable overlap between the core themes created during our analysis of the data from the professional survey and the lived experience focus group. 25 Consequently, we combined the themes from both data sources. We created an over-arching model, which was refined through discussion with professionals in the field (Figure 2). Here, bold type shows 11 themes created during the thematic analysis to represent characteristics of high-quality health and social care for people on probation. The themes were organised within the model to reflect the steps that responses suggest are needed to achieve high-quality care.
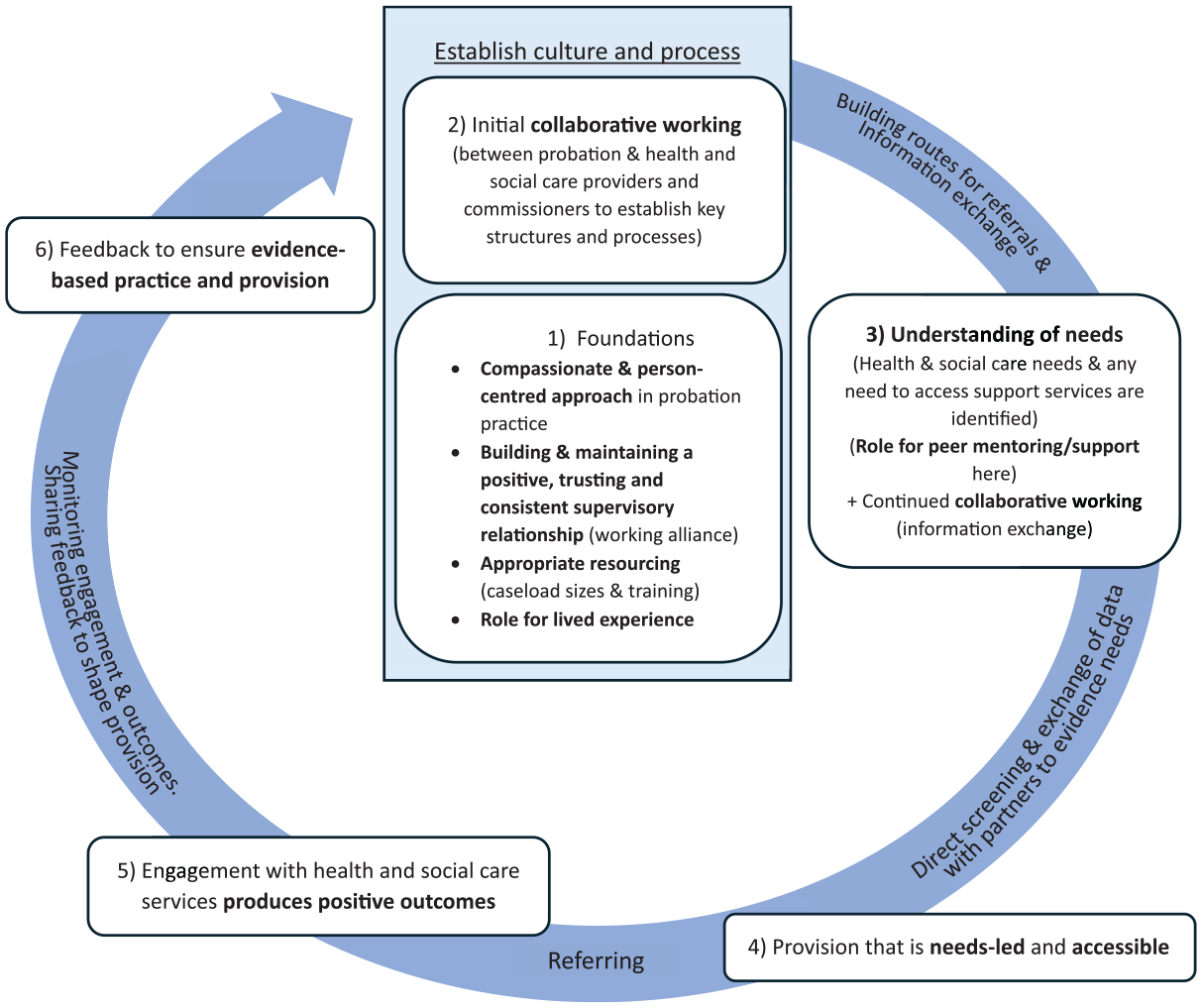
Joint model of the characteristics of high-quality health and social care for people on probation
Analysis suggested that the foundations of high-quality care for people on probation are an organisational culture, training, and resources that enable probation practitioners to establish positive, consistent, and trusting supervisory relationships that support health improvement work.
Alongside this, collaborative working between probation and health and social care providers and commissioners is needed to create systems and processes to identify and record health and social care needs, and make referrals for support. This should include validated screening and assessment tools being available within probation systems and clear referral routes from probation into health and social care services. There should also be mechanisms for sharing (1) individual-level data about health needs when required to make a referral and (2) anonymised group-level data and/or reports to inform service commissioning decisions and practice within probation and partner agencies.
Once unmet needs have been identified probation practitioners should then be able to support people on probation to self-refer into services and directly refer people to services where they consent to this. Practitioners should also ask if people are registered with a GP and assist with registration where needed, and consider and record the risk of suicide and employ appropriate prevention measures.
Feedback should be sought on people’s experiences of and barriers to accessing health and social care services to evidence where things are working well and where improvements are required. Data should also be collected to evidence to what extent attending services and engaging with interventions is improving outcomes for people on probation. A summary of feedback and outcomes should be shared between probation and health and social care commissioners to inform commissioning decisions and improve provision. Through this, the evidence base would develop, helping to ensure that appropriate services are available that can accept referrals in a timely fashion, and that where this is not the case, problems can be identified and addressed through quality improvement initiatives.
Existing indicators
We searched MEDLINE, CINAHL, Cochrane Library, IBSS, and Web of Science databases, to identify any existing quality indicators, guidelines or performance measures for health and social care services in adult criminal justice settings that may be transferable to the context of this study, and identified 6170 papers. We also searched the grey literature, identifying an additional 106 papers, and we acquired copies of 14 publications recommended by our professional panel. 24 A total of 17 papers met the inclusion criteria for the review. Papers were categorised by the setting they related to, the methods used to develop them, associated probation objectives, and whether they comprised standards, indicators, guidelines, or a combination thereof.
Overall, the review highlighted the dearth of guidance specific to healthcare in probation as most papers focused on prison populations, with just two papers specific to probation.26,27 However, it showed that we could draw upon the wider criminal justice system literature to inform the development of our standards, with several standards and indicators available that were relevant to the probation strategy objectives. The use of objective, clearly defined indicators providing a direct measure of the related standard was lacking in some of those available publications, and we aimed to address this when developing our indicators.
Creating draft indicators
After mapping the measures identified in the literature review against the characteristics of high-quality health and social care identified by the professional and lived experience panels, we presented a draft list of 51 standards and 54 quality indicators to the professional panel in a second online survey (some standards had more than one corresponding indicator), grouped by the characteristics of high-quality care that we identified from our data. Participants rated the indicators on three five-point Likert-type scales (Figure 1). Participants were also able to submit comments about the indicators (e.g. thoughts on how they could be re-worded, or potential difficulties with their use in practice) as free text responses. Ten participants rated the indicators, and we calculated a mean score per criterion and an overall mean score for each quality indicator.
Scores and comments suggested that overall, the panel were supportive of the draft standards and indicators, with just two indicators receiving overall average scores of less than 3 (the midpoint of the scale) at this stage. The main concerns expressed in the free text responses related to: the resources needed to operationalise some of the indicators; the timeframe within which probation staff should identify people’s health and social care needs; ensuring that the measures encompassed recent developments in probation practice where possible, for example, work around neurodiversity; the potential challenges around improving cross-system working and information exchange; the potential lack of services within the community to address unmet needs once they had been identified; and being clear about expectations in relation to how staff should respond to unmet needs. There were also suggestions for specific changes to the wording of some of the measures and for potential tools to use to identify health and social care needs.
We refined the wording of the standards and quality indicators in response to the feedback, merging several standards into one and several indicators into one where this was felt to be appropriate to increase the feasibility of their use in practice (considering concerns about resource pressures expressed in the free text responses). For example, the original set of measures included separate standards and indicators for screening for different types of health and social care needs. These were merged into standard number two, with associated indicators being merged too (Table 1).
Final list of quality indicators.
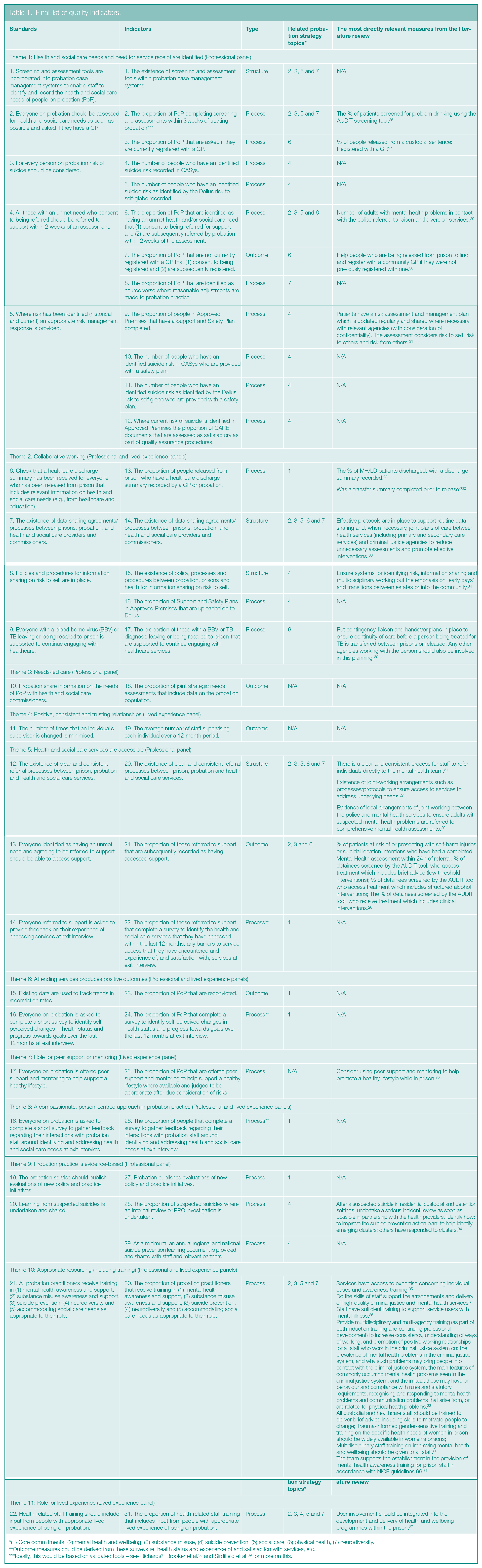
(1) Core commitments, (2) mental health and wellbeing, (3) substance misuse, (4) suicide prevention, (5) social care, (6) physical health, (7) neurodiversity.
Outcome measures could be derived from these surveys re: health status and experience of and satisfaction with services, etc.
Group discussion and selection of final indicators
We invited the professionals that had rated the draft indicators to participate in an online discussion group. The discussion was based on a summary of the overall scores that each original indicator received and the associated qualitative feedback (from the professional panel and key groups within HMPPS), and a list of the suggested revised indicators, which were shared with participants prior to the meeting.
Van Engen-Verheul et al. 22 used the nominal group technique to achieve consensus on a final set of indicators. However, as most of the indicators had already received good ratings, we instead presented the main points of feedback received from the professionals (as above) and asked participants to discuss if, and how, the indicators could be improved.
Six professionals participated in the discussion and again were supportive of the suggested standards and indicators. The discussion centred on how to ensure the practicality of the indicators and demonstrating their value to probation’s objectives. After the discussion, the panel rated a revised set of indicators using Likert-type scales as above. 2 A final set of 22 standards and 31 quality indicators was created based on these ratings (see Table 1) and shared with probation. Recommendations were also shared on how some of them could be put into practice. These were grounded in feedback that participants had provided during the discussion, and the literature included in the systematic scoping review. They included screening tools that could be used, and questions that could be included in surveys to gather data in a straightforward way.
Discussion
We have developed measures to support health improvement among people on probation and, within the context of probation’s health-related role, to measure the quality of health and social care that they receive. These indicators measure the characteristics of high-quality health and social care that were identified by professionals in the criminal justice and health field and people with lived experience of being on probation. Implementing the standards and indicators as part of a quality improvement approach would support the objectives within probation’s health and social care strategy and NHS England’s inclusion health principles.
A strength of the study is that the development of the standards and indicators was based on the consensus of people with considerable professional and lived experience expertise, drawn from multiple organisations. This ensures that while they may describe ideals, the standards and indicators are relevant to current practice, have face validity and should be acceptable and feasible to use, although pilot testing is needed to confirm the latter.
We aimed to base the measures on those used in other adult criminal justice settings where possible, and we were able to do so to an extent. However, the number of measures identified in the literature review that had clear specifications – ‘clear and comprehensive information . . . about the construction of an indicator, including details of numerator and denominator data and the calculations necessary to derive the indicator value’: 40 (p. 242) was limited, with just one paper being identified which contained such measures that were specific to probation (as opposed to offering guidance for the criminal justice system as a whole, or targeting other parts of the criminal justice pathway). 3
We believe that the standards and indicators have implications for future research and practice in probation and health and social care organisations. Quality standards have been used in healthcare systems to improve treatment and care for numerous populations, to target efforts to reduce inequalities in access and outcomes, and to inform the development of competence frameworks that aim to achieve consistency in practice. Developing the standards and indicators alone is not enough to improve the health of people on probation and the quality of care that they receive. For this to happen, they need to be implemented as part of a quality improvement initiative involving stakeholders from a range of agencies/perspectives. Here, improvement plans would be developed to address areas where standards are not being met. For example, data collected against standard 14 may inform work drawing on improvement and behavioural science perspectives to address barriers to people on probation accessing services which could include structural (e.g. access times) and motivational (e.g. trust in services) barriers.
We have co-designed an implementation plan with staff from one probation delivery unit for a pilot of the standards and indicators. Indicators would be populated from existing data sources, surveys of people on probation, and an ‘audit checklist’ containing indicators relating to the existence of necessary structures and processes. 4 We also propose creating a multi-agency change team (e.g. representatives from probation, lived experience, public health, commissioner and provider perspectives) to jointly develop and test approaches to improving performance where standards are not being met. Our findings highlight the need for appropriate foundations within the Probation Service to enable practitioners to focus on health improvement, the need for collaborative working between health and justice agencies, and for improved processes for data collection and information sharing. These may all pose challenges that can be explored in a pilot. Process and impact evaluations would be needed to capture learning in terms of the acceptability and feasibility of the measures, barriers and facilitators to implementation, and the impact of quality improvement work undertaken.
Conclusion
As an inclusion health group, people on probation are a population that is of key concern to multiple organisations. There is a lack of data to evidence the needs of this group and the standard of care that they receive from probation staff and healthcare commissioners and providers. Probation practitioners have a health-related role set out in probation’s health and social care strategy. Working with professionals and people with lived experience, we developed standards and quality indicators linked to the objectives within this strategy. Embedding these within routine practice could provide a framework for multi-agency work to measure and improve the standard of care and health outcomes for this population in the future. Their use and the impact of quality improvement initiatives informed by these measures should be evaluated in future research.
Supplemental Material
sj-docx-1-rsh-10.1177_17579139251335216 – Supplemental material for Developing standards and quality indicators to support health improvement in people on probation
Supplemental material, sj-docx-1-rsh-10.1177_17579139251335216 for Developing standards and quality indicators to support health improvement in people on probation by C Sirdifield, T Parkhouse and J McManus in Perspectives in Public Health
Footnotes
Acknowledgements
The authors thank everyone who supported the study.
Conflict of Interest
The author(s) declared the following potential conflicts of interest with respect to the research, authorship and/or publication of this article: Dr C.S. and Dr T.P. do not have any conflicts of interest to declare. Professor J.M. (third author) is on the Editorial Board for Perspectives in Public Health.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This project is funded by the National Institute for Health and Care Research (NIHR) under its Research for Patient Benefit (RfPB) Programme (Grant Reference Number NIHR201091). The views expressed are those of the author(s) and not necessarily those of the NIHR or the Department of Health and Social Care. ISRCTN 16014381.
Ethical Approval
Ethics permission for the study was gained from the University of Lincoln (2021_6947) and the National Research Committee (2021-124). Informed consent was provided by all participants.
Supplemental material
Supplemental material for this article is available online.
Notes
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
