Abstract
In this piece Nunes addresses the importance of population health approaches and Multi-Hazards Early Warning Systems (MHEWS) in public health, particularly considering climate change and its associated risks and hazards. The article aims to highlight the challenges posed by climate change to public health and how integrating MHEWS with population health approaches can help address these challenges effectively.
Introduction
In today’s climate change landscape, communities face an array of risks and hazards with significant implications for public health and societal welfare.1 –7 The need for robust multi-hazard early warning systems (MHEWS) and proactive health strategies has never been more evident.8–10 Safeguarding our collective future requires a comprehensive approach that links the improvement of population health11,12 with the establishment of effective MHEWS. 8 This integration not only encourages community resilience but also serves as a cornerstone for addressing health disparities and increasing overall health outcomes.
Understanding the Significance of Population Health
Population health11,12 is a strategic imperative aimed at improving the overall health and wellbeing of populations, covering both physical and mental health dimensions while striving to reduce health inequalities. 13 It represents a holistic approach spanning efforts to reduce morbidity and mortality, ensure access to healthcare services, and address the wider determinants of health. 14 By acknowledging the wider determinants of health – ranging from social and economic to environmental and behavioural factors – population health initiatives aim to improve community health while narrowing inequalities.
Emphasising individual responsibility overlooks systemic disparities and societal conditions that constrain choices for all. Instead, a comprehensive population-based approach is vital. By focusing on the wider determinants of health, population health initiatives address the fundamental drivers shaping overall population health and highlight the landscape of health inequalities.15–17 Neglecting crucial wider determinants such as poverty perpetuates health inequality and undermines efforts to improve population health. 18
Understanding the broader societal forces and systems shaping everyday life is crucial for addressing health at the population level. By adopting a holistic perspective on public health issues and recognising the pivotal role of wider determinants of health, effective societal policies and practices can be developed.
Challenges and Opportunities in Mhews
MHEWS are crucial for alerting communities to potential threats and providing them with timely and accurate information and guidance for appropriate actions. 8 Designed to address an array of hazards, from natural disasters to pandemics, these systems play a pivotal role in issuing warnings that consider the intricate interplay of hazards and their impacts. 10 Coordinated efforts are essential to accurately identify and monitor hazards, ensuring the reliability and effectiveness of warning and preparedness mechanisms.
A people-centred approach is indispensable in the design and implementation of MHEWS. 10 By actively engaging affected communities and considering their needs and vulnerabilities, people-centred MHEWS strengthen resilience and foster adaptive capacity. Collaboration among stakeholders is crucial to ensure the efficacy of MHEWS, involving the integration of indigenous knowledge, leveraging geospatial technologies for hazard mapping, using information and communication technologies for effective dissemination, and continually refining the system based on operational experiences. 8
While MHEWS serve as pivotal instruments in delivering timely warnings and risk assessments across diverse hazards, constraints such as data integration problems, communication barriers, and resource constraints can undermine their efficacy. By integrating MHEWS with population health approaches and public health initiatives, communities can overcome these challenges and have opportunities to strengthen health outcomes while reducing vulnerabilities.
The Importance of Integrating Population Health with MHEWS
Integrating population health with MHEWS is crucial for several reasons. First, it serves to protect public health by anticipating and mitigating the risks and impacts of hazards like natural disasters, pandemics, and climate change–related events, which can lead to injuries, illnesses, and deaths. Second, it helps in reducing vulnerabilities, especially among populations such as children, the elderly, and those with chronic illnesses, by identifying and addressing their specific needs during emergencies. Third, integrating population health into MHEWS improves preparedness and response efforts, providing actionable information to healthcare providers, emergency responders, and public health authorities. Fourth, it enhances resilience by promoting health equity, reducing disparities, and strengthening adaptive capacity within communities. Finally, by understanding the intersection of population health and hazards, stakeholders can optimise resource allocation for preparedness, response, and recovery efforts, thereby minimising the burden on healthcare systems. Overall, integrating population health with MHEWS is essential for safeguarding the health and wellbeing of communities and ensuring a more effective response to emergencies.
A Comprehensive Framework for Integrating Population Health and MHEWS
MHEWS serve as indispensable tools for promoting population health and mitigating the risks and impact of disasters. Aligned with the principles of population health, which prioritise the health and wellbeing of communities, these systems seamlessly resonate with the essence of MHEWS designed to enable proactive measures and reduce disaster risks.
The integration of population health approaches with MHEWS presents a range of challenges and opportunities. Barriers may encompass institutional silos, resource constraints, and a lack of awareness regarding the potential benefits of integration. Nevertheless, facilitators such as collaboration and partnerships, data sharing and integration, community engagement, capacity building, and policy development and support can overcome these barriers and foster effective integration.
Approaches to Safeguard Our Future
Achieving a unified vision for safeguarding our future through population health and MHEWS involves several key steps (see Figure 1):
Step 1. Collaborations and partnerships: Establishing joint committees or task forces to develop integrated strategies for addressing community health and hazard management.
Step 2. Data sharing and integration: Implementing data sharing agreements and protocols for integrating data from multiple sources.
Step 3. Community engagement: Mandating community involvement in planning and implementing MHEWS and health promotion initiatives.
Step 4. Capacity building: Allocating funding for training programmes focused on population health and emergency management.
Step 5. Policy development and support: Enacting legislation to mandate population health considerations in MHEWS and disaster management plans.
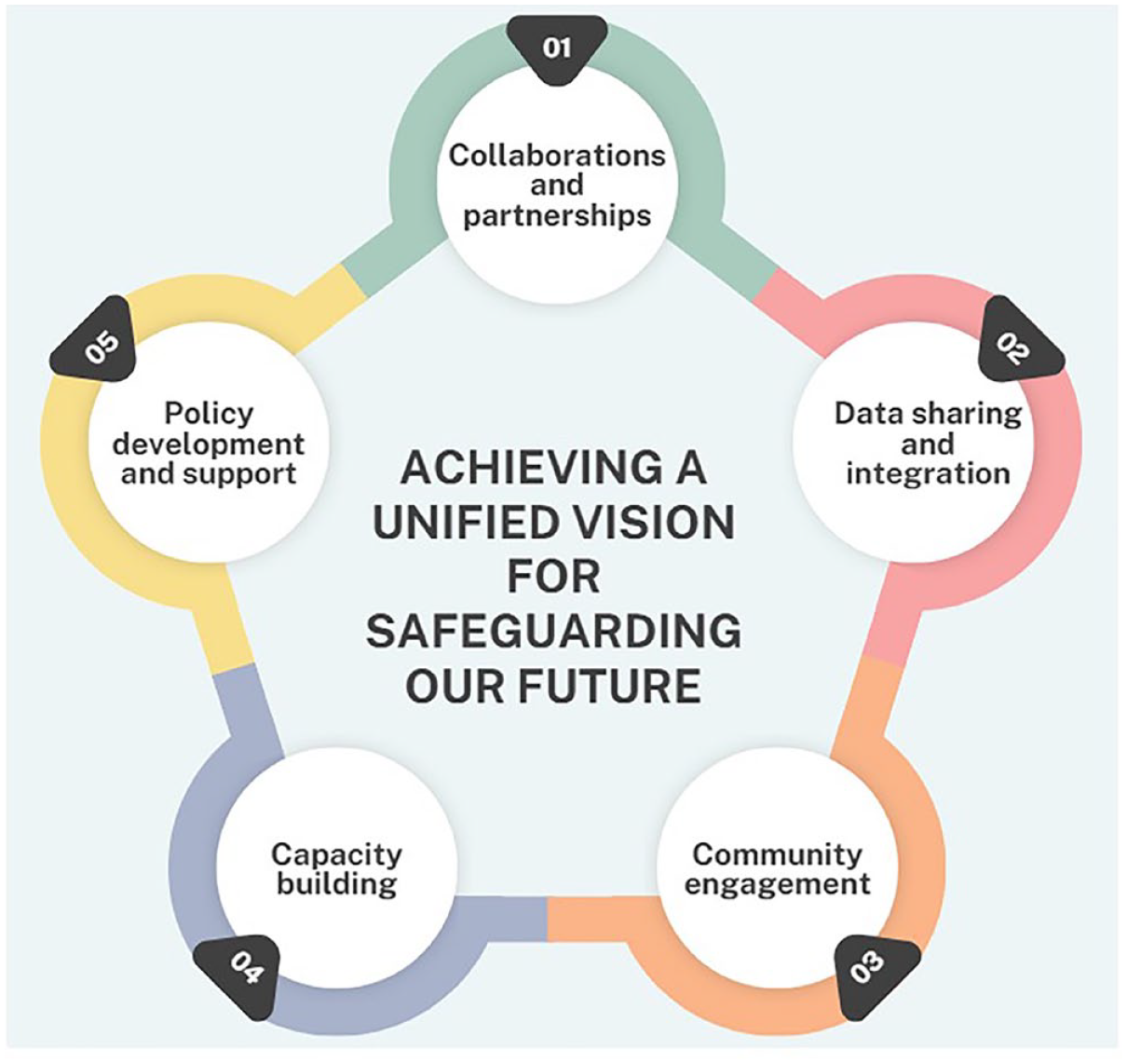
Steps to achieve a unified vision for safeguarding our future
Despite this, the above will only be possible through action from several stakeholders, such as government agencies (national and local), public health authorities (local and national), disaster management organisations (e.g. International Federation of Red Cross (IFRC), Doctors Without Borders), healthcare providers (e.g. primary care, secondary care), community organisations (i.e. Non-Governmental Organisations (NGOs)), academic and research institutions, as well as international organisations (e.g. WHO, United Nations Office for Disaster Risk Reduction (UNDRR).
By taking these steps, we can work towards a future where communities are better prepared to anticipate and mitigate the health risks and impacts of hazards, ultimately enhancing resilience and safeguarding health and wellbeing.
To strengthen integration efforts, proposals such as establishing Inter-Agency Task Forces, allocating resources for research and innovation, launching public awareness campaigns, securing institutional support, and fostering knowledge dissemination and networking initiatives should be explored.
Conclusion
The convergence of MHEWS and population health represents a transformative opportunity to proactively address complex challenges and build a healthier, more resilient future. By embracing this unified vision, stakeholders across sectors can collaboratively work towards mitigating risks, promoting equity, and safeguarding the health and wellbeing of current and future generations. MHEWS and population health approaches emerge as interlinked pillars within the realm of public health, collectively contributing to robust strategies, policies, and practices aimed at improving community health, alleviating disparities, and creating resilient societies capable of navigating an array of health threats.
Footnotes
Conflict of Interest
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethical Approval
Research ethics approval was not required as this was desk research.
