Abstract
More than a million men worldwide are diagnosed with prostate cancer every year. After androgen deprivation therapy (ADT), chemotherapy has been the only subsequent intervention to improve survival in the metastatic setting but has limitations for patients who may not tolerate its toxicity profile or are not candidates on the basis of comorbidities. Novel anti-androgens such as abiraterone acetate have shown promise for such patients. This review draws on clinical evidence and experience to identify abiraterone as a well-tolerated, effective alternative to docetaxel. In the castration-resistant setting, studies demonstrated a survival benefit over placebo, prompting further trials in the hormone-naïve population. More recently the STAMPEDE and LATITUDE studies suggest abiraterone has comparable survival outcomes to docetaxel in the castration-sensitive setting, with evidence in favour of its quality of life profile. Available comparisons with docetaxel are limited, but those available suggest they have comparable efficacy. However, the significant cost compared with docetaxel is a major barrier in resource-rationed healthcare settings. Overall, abiraterone is an effective alternative to chemotherapy for men with castration-sensitive prostate cancer, but this should be balanced with the significantly greater cost.
Introduction
Prostate cancer makes up 15% of all new cancer cases worldwide, with over a million new cases diagnosed each year. In developed countries, it makes up of the big cancers (the others being breast, lung and colorectal) that make up over half of the total cancer incidence and is the commonest cancer amongst men in this population.1,2 After a period of relative stagnation, the last decade has seen a revolution in the management of patients with metastatic disease. This review explores the journey to abiraterone, its peaks and pitfalls as a treatment modality, and the challenges of placing it as a first-line option for newly diagnosed patients.
The historical perspective
Huggins and Hodges are credited with presenting the scientific rationale behind androgen deprivation therapy (ADT) after the Swiss Urologist Paul Niehans presented his experience of hormonal manipulation in prostate cancer in 1940.3–5 Initially, surgical castration was the only means of achieving androgen deprivation. This was followed by the development of chemical castration via gonadotrophin releasing hormone (GnRH) agonists and, much later, antagonists. GnRH agonists in the form of luteinizing hormone releasing hormone (LHRH) analogues were found to inhibit testosterone through over-stimulation of pituitary GnRH receptors, therefore shutting down release of luteinizing hormone (LH) and folllicle stimulating hormone (FSH) and subsequent downregulation of testosterone production. 6 ADT has therefore been, and remains, the first-line treatment for metastatic prostate cancer until 2015, with most patients being treated long term with LHRH agonists which range in application from monthly to 6-monthly. 7 The inevitable development of castrate resistance has proven the main limitation of ADT. Once castration resistance occurs, the only remaining options were steroids, synthetic oestrogen such as diethylstilbestrol, and mitoxantrone in the early part of this millennium.8,9 Consequently, new approaches were sought.
The role of chemotherapy
The challenge of managing castrate-resistant prostate cancer (CRPC) remained, and chemotherapy proved to be the next major innovation. The approval of docetaxel chemotherapy for patients with metastatic CRPC was the results of findings from randomized controlled trials (RCTs), TAX327 and the Southwest Oncology Group (SWOG) 9916. These studies demonstrated a survival benefit of around two months for docetaxel plus prednisone versus the then standard of care, mitoxantrone (in the latter study, docetaxel was given with estramustine).9,10
Chemotherapy was even more successful when trialled in the hormone-sensitive setting a decade later; the large RCTs, CHAARTED, STAMPEDE (docetaxel) and GETUG-AFU-15 formed the evidence basis for first-line docetaxel chemotherapy alongside ADT in international guidelines for metastatic prostate cancer 7 (Table 1). CHAARTED included 790 men with metastatic hormone-sensitive prostate cancer (mHSPC) comparing ADT with ADT plus docetaxel. The primary outcome measure, median overall survival (OS), was significantly longer in patients receiving chemotherapy in addition to ADT (57.6 months versus 44.0 months). 11 STAMPEDE is an ongoing multi-arm multi-stage trial of which the first studies compared ADT (1184 patients) with ADT plus docetaxel (592 patients). STAMPEDE includes patients who do not have metastatic disease, for example, high-risk local disease, but for this article we focus on the data concerning patients with metastatic prostate cancer. Despite different stratification criteria, STAMPEDE identified similar median OS in patients with metastatic disease who received ADT plus docetaxel versus ADT alone (60 months versus 45 months). 12 GETUG-AFU-15 recruited 385 patients, and although they identified a difference in survival in ADT + docetaxel group, this was not significant (62.1 months versus 48.6 months).13,14 A meta-analysis of these studies suggested an improvement in OS with ADT plus docetaxel over ADT alone (HR 0.73). This also noted 33% reduction in risk of death in patients with high volume disease, versus a 20% reduction in low volume disease. 15 Another meta-analysis that included patients with metastases from the ADT + zoledronic acid (ZA) arm of STAMPEDE further confirmed these findings (HR 0.77). 16 As a consequence, docetaxel is now recommended alongside ADT in patients with hormone-sensitive prostate cancer, and in Europe represents first-line treatment in appropriate patients.16–18
Key studies of docetaxel in metastatic hormone-sensitive prostate cancer setting.

data only patients with metastatic disease.
ADT, androgen deprivation therapy; CI, confidence interval; mHSPC, metastatic hormone-sensitive prostate cancer.
The introduction of chemotherapy as first-line therapy alongside ADT was the first intervention shown to significantly improve survival in metastatic prostate cancer in over 50 years. But there are remaining questions and uncertainties. A subsequent follow-up analysis of patients with low volume disease in the CHAARTED study suggested these patients may not gain significant benefit from docetaxel. 19 As STAMPEDE did not report the extent of metastatic disease, comparisons cannot be made of this metric. Docetaxel is associated with significant grade 3–5 toxicity, with the main toxicities of neutropenia, febrile neutropenia and fatigue. Nearly 30% and over 50% of patients experienced some form of grade 3–5 toxicity in the docetaxel arms of CHAARTED and STAMPEDE respectively. Although a broad and appropriate age range of patients was included in these studies, most were performance status (PS) 0–1 patients fit enough for chemotherapy, and this may not represent the entire presenting population.
The age of abiraterone
Targeted drug design around the mechanism of castrate resistance and testosterone synthesis led to the development of the next important group of treatments for prostate cancer. Studies suggested that tumours developed an overexpression of androgen biosynthesis enzymes and therefore harboured a high intratumoural androgen level, alongside overexpression of mutated androgen receptors with a higher affinity for testosterone. Abiraterone acetate was developed to inhibit testosterone synthesis by blocking cytochrome P450 c17 at a number of androgen biosynthesis sites. 20
A large RCT (COU-AA-301) of 1195 patients with CRPC who had previously received docetaxel was the first phase III study to demonstrate a survival benefit in patients receiving abiraterone versus placebo (14.8 versus 10.9 months). 21 The study of chemotherapy-naïve CRPC patients that followed also showed a survival advantage of a similar magnitude (34.7 versus 30.3 months). 22 A systematic review of ‘real-life’ data in this setting, although suggesting a lower, more wide-ranging OS, appears to corroborate this. 23 Studies of enzalutamide in this setting also demonstrated similar benefits24,25 (Table 2).
Key randomized controlled trials (RCTs) of abiraterone acetate and enzalutamide in metastatic castrate-resistant prostate cancer setting.

CI, confidence interval; mCRPC, metastatic castrate-resistant prostate cancer; OS, overall survival; PFS, progression-free survival.
Abiraterone in the castration-sensitive setting
The positive findings of novel androgen-targeted drugs, and the limitations of upfront chemotherapy for certain patients, raised the question of abiraterone as an alternative option to chemotherapy in patients with HSPC.
Two studies have presented their findings from large RCTs of abiraterone in HSPC – LATITUDE and STAMPEDE (Table 3). A third, PEACE-1 (ClinicalTrials.gov identifier: NCT01957436), is still recruiting and will offer insights into the addition of, rather than the alternative of, abiraterone alongside ADT, docetaxel or radiotherapy.
Completed RCTs of abiraterone acetate in patients with mHSPC.
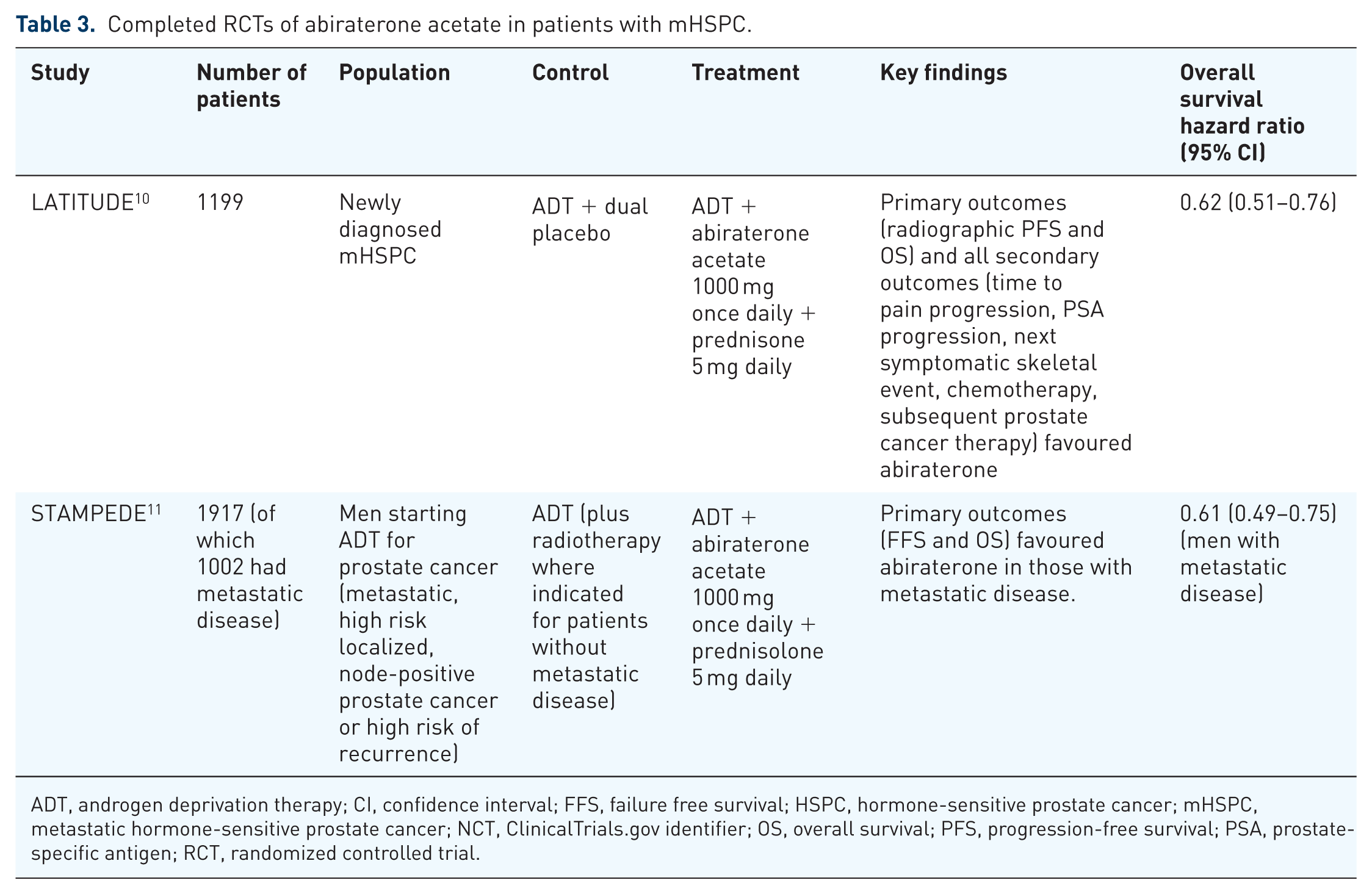
ADT, androgen deprivation therapy; CI, confidence interval; FFS, failure free survival; HSPC, hormone-sensitive prostate cancer; mHSPC, metastatic hormone-sensitive prostate cancer; NCT, ClinicalTrials.gov identifier; OS, overall survival; PFS, progression-free survival; PSA, prostate-specific antigen; RCT, randomized controlled trial.
The LATITUDE study recruited 1199 men with newly diagnosed, high risk, hormone-sensitive prostate cancer in 235 sites in 34 countries. 26 ‘High risk’ was defined as two or more of the following features: Gleason score ⩾ 8, more than three bone metastatic sites, or visceral metastases. Patients were randomized either to ADT + abiraterone (n = 597) or ADT + placebo (n = 602). Abiraterone was dosed with prednisone 5 mg. The predefined endpoints were OS and radiographic progression-free survival (PFS). At the predefined interim analysis time point (median follow up 30.4 months), abiraterone was superior to placebo in all primary and secondary outcomes. Median OS had not been reached in the abiraterone group, versus 34.7 months in the placebo group, indicating a statistically significant reduction in the risk of death by 38%. Median PFS was 33 months versus 14.8 months respectively. Notable side effects included hypertension, hypokalaemia, raised ALT/AST, hyperglycaemia and cardiac disorders. Secondary outcomes of pain progression [hazard ratio (HR) 0.7, 95% confidence interval (CI) 0.58–0.3, p < 0.001], prostate-specific antigen (PSA) progression (HR 0.3, 95% CI 0.26–0.35, p < 0.001) and symptomatic skeletal events (HR 0.7, 95% CI 0.54–0.92, p = 0.009) all favoured abiraterone over placebo. Consequently, the study was unblinded at this point to allow all patients access to abiraterone.
The STAMPEDE investigators compared ADT with ADT plus abiraterone with prednisolone 5 mg. 27 1917 patients were randomized, of which 1002 (52.3%) had metastatic disease. 941 (93.9%) of these were patients with newly diagnosed metastases, so although analysis of efficacy in the preplanned subgroup of patients with metastases included newly and previously treated metastases, the latter comprised a small proportion. OS was significantly improved in the ADT + abiraterone subgroup in patients with metastatic disease (HR 0.61, 95% CI 0.49–0.75). Improvement in failure-free survival seen in all patients (ADT versus ADT + abiraterone 30 months versus 43.9 months respectively) was also seen in the metastatic patient subgroup. The side effect profile was similar to LATITUDE with 47% versus 33% grade 3 or more toxicity seen in the ADT+ abiraterone and ADT alone groups respectively.
LATITUDE complemented their study of efficacy with an evaluation of patient-reported outcomes (PROs) and health-related quality of life (HRQOL) in this same population. 28 PRO data were collected using electronic devices available to patients during the study, and patients provided data through completion of pain and fatigue rating questionnaires, as well as quality of life and prostate-specific functional assessment scales. The authors demonstrated longer median times to worst pain intensity progression, fatigue intensity progression and functional deterioration (assessed on prostate cancer-specific tools) in patients in the abiraterone arm versus placebo. They also showed a maintained or improved HRQOL in the abiraterone arm, although there was no significant difference in functional, emotional, social and family wellbeing between the arms. This study is particularly relevant given the increasing appreciation of correlation between changes in quality of life measures and survival outcomes. 29
The only study allowing comparison of abiraterone and docetaxel in this setting comes from STAMPEDE during the period of overlapping recruitment to the docetaxel and abiraterone arms of the study. Patients were contemporaneously randomized to either Arm C, standard of care (SOC) + docetaxel/prednisolone (n = 189) or Arm G, SOC + abiraterone (n = 377). Direct comparison demonstrated no difference in OS or prostate-specific survival, although importantly the study was not powered to identify differences. 30 This remains, however, the only direct comparison available between abiraterone and docetaxel upfront for patients with HSPC. A network meta-analysis of 11 trials (10 completed, 1 open to recruitment) by STOPCAP which aimed to utilize individual patient data to account for variations between trials also concluded that both abiraterone and docetaxel were effective and suggested the data favoured abiraterone but that the extent and validity of this could not be certain. 31
The National Institute of Health and Care Excellence (NICE), the organization that makes recommendations regarding drug approval in the United Kingdom (UK), have recently ruled against recommending abiraterone as an alternative to upfront docetaxel in HSPC. 32 This is in contrast with elsewhere in the world, the National Comprehensive Cancer Network (NCCN) lists ADT plus abiraterone and ADT plus docetaxel as options for hormone-naïve patients. 33
Moving forward
In the HSPC setting, a number of clinical trials are currently active, relevant examples of which are summarized in Table 4. STAMPEDE continues to recruit patients to its multi-arm study set up. Arm H (prostate radiotherapy) and Arm J (abiraterone and enzalutamide) have finished recruiting and the results are awaited. Current open arms are for SOC, SOC plus metformin (‘Arm K’) and SOC with ADT exchanged for transdermal oestrogen patch (‘Arm L’). Arm K addresses the association observed in diabetic patients who take metformin and reduced risk of cancer incidence and mortality 34 as well as studies demonstrating a role for metformin in AMPK, PI3K-AKT, MTOR and other important cancer-associated pathways. Transdermal oestrogen is intended to ameliorate the oestrogen-suppressing properties of LHRH agonists that give rise to problematic side effects of long term ADT. The PATCH trial has published a phase II study suggesting the safety of this route of administration as an alternative to ADT as it avoids the prothrombotic risks of oral oestrogen therapy, with the phase III study ongoing. 35
Examples of active or recruiting phase II and III clinical trials in patients with metastatic hormone-sensitive prostate cancer (at time of submission).

ADT, androgen deprivation therapy; HSPC, hormone-sensitive prostate cancer; LHRH, luteinizing hormone releasing hormone; n/a, not applicable.
Another trial in progress involves the novel anti-androgen apalutamide, which was recently licensed by the US FDA for men with nonmetastatic CRPC as a result of findings from the SPARTAN study. 36 TITAN is a phase III trial where patients with HSPC are randomized to ADT or ADT plus apalutamide. This is active but has completed recruitment and the results are awaited. Of note, patients were allowed to have treatment with docetaxel as the new SOC in the hormone-naïve setting. The ARASENS study is evaluating the anti-androgen, darolutamide, in the same situation (ADT + docetaxel plus darolutamide or placebo) and closes in 2020.
Exploitation of the immune system either via a vaccine (e.g. PROSTVAC) or immunotherapy are also notable in active earlier phase trials and are likely to expand as interest in immunotherapy continues to grow.
Conclusion
Abiraterone represents a new era of treatment for hormone-sensitive prostate cancer. The significance of treating men at diagnosis alongside testosterone suppression through LHRH agonists was demonstrated by chemotherapy. All available evidence suggests abiraterone is a comparable treatment, in spite of representing a completely different class of agent, and therein lies the challenge of comparing the two. Mechanistically, clearly chemotherapy and abiraterone are very different, and there may be circumstances where abiraterone currently has no role, such as neuroendocrine differentiation. Chemotherapy represents a discrete treatment course which is relatively inexpensive but can come with life-changing and life-threatening toxicities, rendering it an inappropriate choice for some men who therefore miss out on upfront treatment. On the other hand, abiraterone is expensive and continues until the point of progression (and therefore is potentially taken for much longer), but has a more tolerable toxicity profile, opening up its utility to patients who might otherwise receive LHRH agonist treatment only must feel it is only a matter of time before this becomes widely available, but in resource-rationed healthcare systems, it may be some time before all men who might be eligible have the choice of abiraterone have such an option.
