Abstract
Purpose:
The purpose of this review is to evaluate different techniques in urinary diversion and urethral stenting in hypospadias surgery.
Patients and methods:
The surgical procedure included 192 tubularized incised plate (TIP) repairs for distal penile hypospadias. The patients were prospectively randomized into three groups: In group A, a urethral catheter was used as a stent and for diversion of urine (63 patients); in group B we use no urethral stenting (63 patients), only a suprapubic catheter; and in group C we use a suprapubic diversion and we put a small catheter in the anterior urethra only (66 patients). The urethral catheter was removed in group A at the 6th–7th postoperative day and in group C the urethral stent was removed at the 3rd–4th postoperative day. The suprapubic catheter was removed in both groups B and C at the 7th–9th postoperative day. All patients received an injection of antibiotics in the morning of the operation and daily until the day of catheter removal. All of the operations were performed by the same surgeon.
Results:
The mean ages of our patients were 3, 5, and 5 years in groups A, B, and C, respectively. The mean hospital stay was 5 days (3–8). Follow-up ranged from 8 to 48 months (mean of 21.5 ± 10.1 months). Bladder spasm was observed in 33% of our patients in group A while there were no cases of spasm in the other two groups with a statistically significant difference (p < 0.05). Fistula was reported in eight patients (12.7%) of our urethral catheter group A, while it was observed in three patients (2.3%) of our suprapubic diversion groups B and C with a statistically significant difference between the two groups (p < 0.05). Meatal stenosis was reported in eight patients in group B (12.7%; nonstented group) versus three patients of both groups A and C (2.4%; stented groups) with a statistically significant difference (p < 0.05).
Conclusion:
Suprapubic diversion is an important step in hypospadias repair as it provides a better success rate with a significantly lower rate of occurrence of fistula. However, the addition of a stent in the anterior urethra to suprapubic diversion avoids the development of meatal stenosis and also avoids the bladder spasm observed with a urethral catheter.
Introduction
Selection of the appropriate method for urinary diversion after hypospadias repair remains controversial [Demirbilek and Atayurt, 1997].
Most pediatric urologists use suprapubic or urethral drainage routes to permit the repair to be watertight, immobilize the suture line and provide patient comfort [Oesterling et al. 1987].
There are two methods of transurethral diversion either to insert a catheter that enters the bladder or to insert it provided that the tip is placed distal to the external sphincter with the aim of reducing postoperative complications such as fistula and meatal stenosis [Buson et al. 1994; Maizels and Firlit, 1986].
Recent studies in animal models have reported that indwelling catheters are unnecessary for normal epithelization of uretheral reconstruction based on their finding that showed unstented repair has very good healing potential [Hafez et al. 2003].
In this study we report our experience with regards to urinary diversion and urethral stenting in distal penile hypospadias repair using a tubularized incised plate (TIP).
Patient and methods
It is a prospective, randomized study in which 192 patients with distal penile hypospadias underwent TIP urethroplasty using the same technique as described previously by Snodgrass [Snodgrass, 1994]. The study protocol was reviewed and approved by our institutional review board and informed consent was obtained from the parents of participating children. All of the operations were performed by the same surgeon.
Patients were randomly subdivided into three groups. In group A, a urethral catheter was used as a stent and for the diversion of urine; in group B, we use no urethral stenting, only suprapubic catheter; and in group C, we use suprapubic diversion and we put a small catheter in the anterior urethra only. The randomization list was concealed from the operators during this study to avoid selection bias as subjects were enrolled.
A urethral catheter 6F was used for infants less than 1 year old and 8F for older children. Closure of the urethral plate was done using absorbable monofilament (PDS 6/0). A penile tourniquet was used to achieve a bloodless field and for an erection test that was performed to confirm that the penis was straight. Compressive dressing with bactericidal ointment was used at the end of the procedure.
Caudal analgesia was used for all patients to prevent postoperative pain. The compressive dressing was removed in the first postoperative morning.
Urethral catheters were removed in group A the 6th–7th postoperative day and in group C the urethral stent was removed at the 3rd–4th postoperative day. The suprapubic catheter was removed in both group B and C at the 7th–9th postoperative day.
All patients received an injection of antibiotics in the morning of the operation and daily until the day of catheter removal. Analgesics were given during the first postoperative voiding if required.
The patients were re-examined by the surgeon regularly after catheter removal every 2 weeks in the first 3 months and then every 6 months thereafter. Regular dilatation of the neourethra was taught to all parents.
Fisher’s exact test was performed to compare the outcome between different groups. Statistical analysis was done with Graphpad software.
Results
A total of 192 patients with a mean age of 4.2 ± 2.6 years were included in the study. Group A included 63 patients with a mean age of 3.3 ± 1.6 years (range 1–7 years), group B included 63 patients with a mean age of 4.9 ± 2.5 years (range 1–9 years) while group C included 66 patients with a mean age of 5 ± 2.6 years (range 1–12 years). The mean hospital stay was 4.5 ± 1.8 days (range 3–8). There was no statistically significant difference between the three groups with regards to hospital stay. Follow up ranged from 8 to 48 months (mean 21.5 ± 10.1 months).
During the early postoperative period, mild edema and/or bruising was seen in nearly all cases with no significant hematomas. However, two cases of infection localized to the penis were reported, one in group A and the other one in group B.
Bladder spasm was assessed clinically by the presence of suprapubic pain and/or pericatheter leakage.
Mild bladder spasm was documented in 33% (21 patients) of group A (treated with oxybutynin), but none of the patients in groups B or C with a statistically significant difference (p < 0.05).
As regard the late postoperative complications (Table 1), fistula was reported in eight patients (12.7%) of urethral catheter group A, while it was observed in only three patients (2.3%) of our suprapubic diversion groups B and C with a statistically significant difference (p < 0.05).
Postoperative complications.
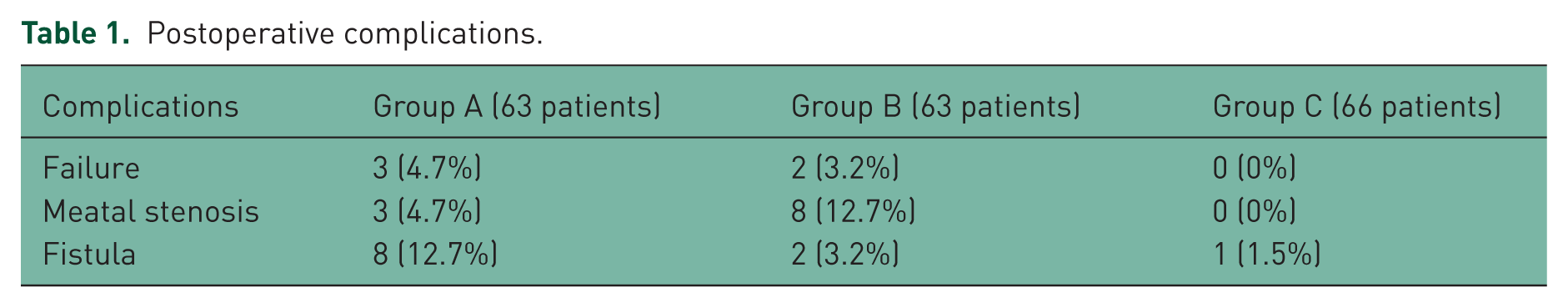
On the other hand, fistula was reported in 3.2% of group B (nonstented group) versus 6.2% of both groups A and C (stented groups) with no statistically significant difference (p > 0.05).
It was also reported in eight patients (12.7%) in group A and only one patient in group C (1.5%) with a statistically significant difference between the two groups (p < 0.05).
Meatal stenosis was assessed clinically and confirmed with uroflowmetry. It was reported in eight patients in group B (12.7%; nonstented group) versus three patients of both groups A and C (2.4%; stented groups) with a statistically significant difference (p < 0.05)
On the other hand, meatal stenosis was noted in three patients (4.7%) in group A versus no patients in group C with no statistically significant difference between the two groups (p > 0.05).
Discussion
The technique of TIP for distal hypospadias repair has become the procedure of choice as it provides satisfactory functional and cosmetic results [Snodgrass, 1994].
Failure, fistula, and meatal stenosis are the most common complications encountered and they most likely develop within 6 months postoperatively [Borer et al. 2001; Elbakry, 2002].
Selection of the most appropriate method for urinary diversion appears to be an important step in avoiding these complications and achieving good results [Demirbilek and Atayurt, 1997].
In a study by Demirbilek and Atayurt comparing 49 patients with urethral catheter for urinary diversion with 56 patients with only suprapubic urinary diversion after hypospadias repair, there was a significant difference between the two groups in the development of fistula (14.2% versus 7.1%) in the urethral catheter group and the suprapubic diversion group, respectively [Demirbilek and Atayurt, 1997]. These results are similar to ours where fistula was reported in 12.7% versus 2.3% in the urethral catheter group (group A) and the suprapubic diversion groups (groups B and C), respectively, with a statistically significant difference.
In the same study of Demirbilek and Atayurt, mild bladder spasm responding to oxybutynin occurs in 25% of patients with urethral stent while no case of bladder spasm was reported in the suprapubic diversion group [Demirbilek and Atayurt, 1997]. This is similar to our finding where 33% of our patients in group A (patients with urethral catheter) suffer from bladder spasm while no case of spasm was reported in the other two groups with a statistically significant difference (p < 0.05). On the other hand, Arda and colleagues reported no case of bladder spasm in their urethral catheter group [Arda and Mahmutoglu, 2001].
In this latter study, the authors compared two groups: group I, in which an 8F feeding tube was used as a stent; and group II, in which the same size catheter was passed into the bladder. Both meatal stenosis and fistula occurrence were higher in the stent group with a statistically significant difference. Meatal stenosis was noted in five patients (22.7%) and three patients (13.6%) and fistula in two patients (13.6%) and only one patient (4.5%) of groups I and II, respectively. Also, the authors reported that stents that are positioned in the anterior urethra cause significant pain and irritation in 86.3% of patients caused by bladder distension [Arda and Mahmutoglu, 2001]. These results are different from our study where a lower rate of occurrence of fistula and meatal stenosis were reported in the stent group (group C) in comparison with the urethral catheter group (group A).
None of our patients in the stent group complained of significant pain or had bladder distension. This can be explained by the presence of suprapubic diversion in our stent group (group C).
On the other hand, some authors recommend stent-free repair based on their studies that show excellent results and avoid catheter-related morbidity such as infection and bladder spasm with an absence of pain and subsequent better patient comfort postoperatively [Hakim et al. 1996; Leclair et al. 2004; Minevich et al. 1999; Samuel et al. 2002].
However, other authors found that nonstenting the neourethra after hypospadias repair was associated with early postoperative complications such as extravasation and retention [Buson et al. 1994; El-Sherbiny, 2003].
A retrospective study by Hakim and colleagues reported their experience in Mathieu repair. They reviewed the records of 336 consecutive boys who underwent the modified Mathieu repair for primary distal hypospadias. A urethral stent was placed in 114 patients and nonstented repair was performed in 222 patients. They had no cases of urine retention in the non stented group [Hakim et al. 1996]. Similarly, Samuel, Turial, Almodhen and colleagues had the same finding [Almodhen et al. 2008; Samuel et al. 2002; Turial et al. 2011]. However, Leclair and colleagues had a retention rate of about 2.4% in their series of 162 children managed with unstented repair after TIP [Leclair et al. 2004].
On the other hand, El-Sherbiney reported up to 24% of retention and about 20% reoperation rate in their series of 29 toilet-trained children in their nonstented group [El-Sherbiny, 2003].
In comparison to our study, we did not report any case of retention in the unstented group (group B) due to the presence of a patent suprapubic catheter.
As regards the incidence of fistula in stented versus unstented hypospadias repair, Buson and colleagues reported a 13.5% fistula rate in unstented Mathieu repair compared with 1.5% when a stent was used [Buson et al. 1994].
A recent study by Turial and colleagues reported their experience in nonstented hypospadias repair using TIP in 41 patients with 4.9% of cases complicated with fistula [Turial et al. 2011]. Similarly, Lecalir and colleagues reported 5.6% fistula rate in a similar series of unstented repair [Leclair et al. 2004]. The high fistula rate of unstented repair was explained by the high incidence of meatal stenosis and by the excess uretheral manipulation in cases of urine retention [Rabinowitz, 1987].
On the other hand, Hakim and colleagues found no difference between stented versus unstented hypospadias repair groups with regards to fistula (2.36% versus 2.7%) [Hakim et al. 1996]. This result is nearly similar to our results where fistula was reported in 3.2% of group B (nonstented group) versus 6.2% of both groups A and C (stented groups) with no statistically significant difference (p > 0.05).
Meatal stenosis is an uncommon event. Turial and colleagues reported 2.4% of cases complicated with meatal stenosis irrespective of age. This results are nearly similar to Leclair and colleagues who reported 2.5% of meatal stenosis in their series of unstented repair [Leclair et al. 2004; Turial et al. 2011].
In comparison to the results of the present study in which meatal stenosis was reported in 12.7% of group B (nonstented group) versus 2.4% of both groups A and C (stented groups) with a statistically significant difference (p < 0.05).
In group C in our study, in which we use suprapubic diversion and we put a small catheter in the anterior urethra (66 patients), no cases of failure and no complications were reported except for one case of fistula (1.5%).
In other words, in this group we avoid the high rate of fistula and bladder spasm reported in group A by the presence of suprapubic diversion and avoid the high rate of meatal stenosis reported in group B (unstented group) by the presence of the stent in the anterior urethra.
Conclusion
Suprapubic diversion is an important step in hypospadias repair as it provides a better success rate with significantly lower rate of occurrence of fistula. However, the addition of a stent in the anterior urethra to suprapubic diversion avoids the development of meatal stenosis and also avoids the bladder spasm observed with a urethral catheter.
Footnotes
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
Conflict of interest
The authors declare no conflicts of interest in preparing this article.
