Abstract

Introduction
Despite rapid development of advanced diagnostic methods, antimicrobial agents, and modern surgical devices, the incidence of infective endocarditis (IE) has remained almost unchanged over the past few decades [Mylonakis and Calderwood, 2001]. In developed countries, however, rheumatic disease is no longer the main underlying disease. Instead, degenerative valve disease of the elderly, mitral valve prolapse, and intravenous (iv) drug use are becoming the leading causes [Hoen et al. 2002].
The management of IE is a challenge because the usually proposed standard antibiotics often are not very efficient, which can be attributed to several factors, namely, allergic reactions, antibiotic toxicity due to prolonged therapy, and increasing microbial resistance to antibiotics used as first-line therapeutic options [Elliott et al. 2004].
Herein, we aimed to present two young intravenous drug users (IDUs) with tricuspid valve infective endocarditis (TVIE) and reviewed our treatment strategy.
Case reports
Case 1
A 17-year-old boy was referred to our emergency unit with the complaint of high fever, dyspnea, and palpitation for about 1 week. The patient had an 18-month history of iv drug (heroin) use. Physical examination on presentation was significant for abdominal distention. Pulmonary auscultation showed that there was a ral and roncus. Laboratory results included leukocytosis of 28,400/mm3 and C-reactive protein (CRP) level 92.5 mg/L. Computed tomography (CT) of the chest revealed multiple infiltrates in both lung fields and multiple pulmonary embolisms. Echocardiographic examinations showed grade 3 regurgitation and mobile vegetation of 43 × 27 mm on the tricuspid valve, and right atrial and ventricular dilatation (Figure 1). Blood cultures were positive for methicillin-sensitive Staphylococcus aureus. The patient was admitted to the intensive care unit and antimicrobial treatment was initiated (vancomycin 1 g iv once every 12 h, gentamicin 80 mg iv once every 8 h, oxacillin 2 g iv once every 4 h) for 6 weeks. The patient was admitted to the intensive care unit and antimicrobial treatment was initiated. Although the size of the vegetation decreased to 2.3 mm with medical treatment, arterial blood gas analyses showed a saturation of 85–90%. After 4 weeks, the patient underwent surgery because of repeated pulmonary embolism. When the right atrium was explored, a large vegetation was found attached to the anterior leaflet of the tricuspid valve. The septal leaflet was detached from the annulus. As the infection involved all leaflets, a total resection of the tricuspid valve was performed. The tricuspid valve replacement was performed using a 33 mm Carpentier–Edwards pericardial bioprosthesis (Edwards Lifesciences, Irvine, CA, USA). The postoperative course was uneventful and there was no recurrence of endocarditis 36 months after surgery.
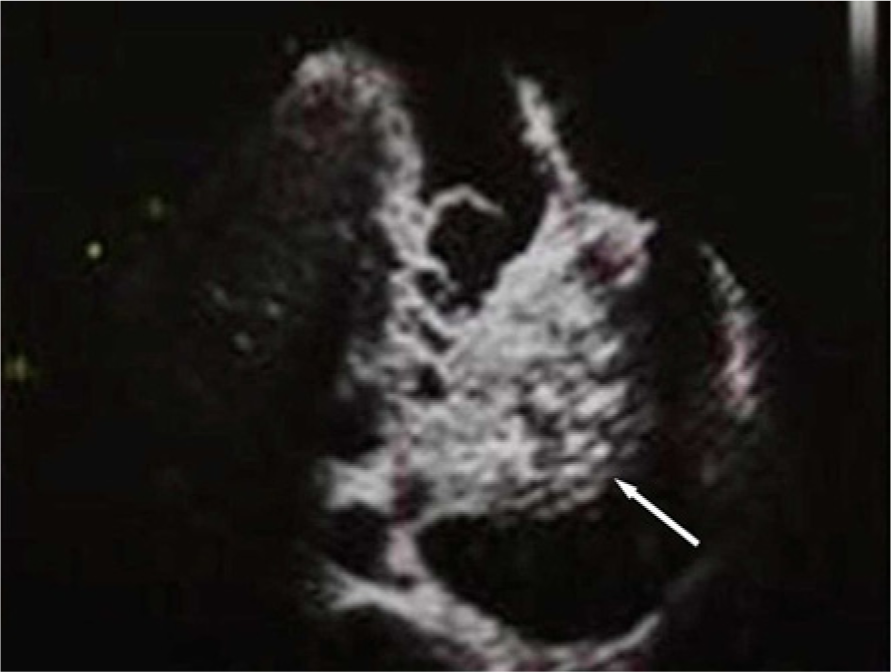
The echocardiographic examination shows severe tricuspid regurgitation and mobile vegetation (white arrow). The size of the vegetation on the tricuspid valve is 43 mm × 27 mm.
Case 2
A 22-year-old male IDU was referred to our hospital with a 1-week history of cough, fever, appetite loss, fatigue, and dyspnea. The patient had a 36-month history of iv drug (heroin) use. Physical examination was normal. Laboratory results included leukocytosis of 16,500mm3 and a CRP level of 53.5 mg/L. CT of the chest revealed multiple infiltrates and cavitations in both lung fields and multiple pulmonary embolisms (Figure 2). Echocardiography showed grade 4 regurgitation and mobile vegetation of 24 mm × 11 mm on the tricuspid valve. There was a perforation on the anterior leaflet of the tricuspid valve. Blood cultures were positive for methicillin-resistant Staphylococcus aureus. The patient was admitted to the intensive care unit and antimicrobial treatment was initiated (vancomycin 1 g iv once every 12 h, gentamicin 80 iv once every 8 h). Two weeks after medical treatment, the patient underwent surgery during the healed stage. When the right atrium was opened, multiple vegetations were found attached to the anterior, septal leaflet of the tricuspid valve. Torn chordae were seen in the operation. As the infection was generalized, and there was a valvular perforation, a total resection of the tricuspid valve with its vegetation was performed. A 33 mm Carpentier–Edwards pericardial bioprosthesis was replaced. The postoperative course was uneventful and there was no recurrence of endocarditis 48 months after surgery.

Chest computed tomography demonstrates multiple infiltrations and cavitations in both lungs due to multiple pulmonary embolisms (white arrows).
Discussion
In developed and developing countries iv drug use is a social, health, and economic burden [Aceijas et al. 2006]. Overdose, cutaneous complications, pulmonary embolism, IE, community-acquired pneumonia, pulmonary tuberculosis, septicemia, and the transmission of blood-borne infections are well-known complications. It has been estimated that there are 13 million drug abusers in 130 countries worldwide, of whom 10 million live in developing and transitional countries [Panduranga et al. 2010]. From the available data, the prevalence in eastern Europe and Asia, is 0.65%, whereas in the Middle East and Africa, it is 0.2%, which is low [Panduranga et al. 2010].
The tricuspid valve is infected in 50–70% of IDU cases of IE. The mitral and aortic valves are involved in 20–30% of cases. The tricuspid valve may be more susceptible to heroin use, as heroin can cause an increase in pulmonary arterial pressure, creating more turbulence at the tricuspid valve. Substances such as cocaine and metamphetamines, on the other hand, increase systemic afterload, causing increased turbulence at the sites of the aortic and mitral valves [Jain et al. 2008; Cooper et al. 2007]. In the present report, the patients had a history of iv heroin use.
Staphylococus aureus is responsible for most of the IE cases among IVUs [Sousa et al. 2012]. The most commonly isolated fungi are Candida albicans (24%), and non-Candida albicans accounts for 24% of fungal isolates [Fowler et al. 2005]. Also, due to iv drug use, high-risk behaviors, IVUs are subjected to needle-borne infections by organisms that are usually nonpathogenic. Owing to the habit of cleaning their needles with saliva and using the saliva to dissolve the drug, IVUs are therefore prone to infection from normal oropharyngeal flora microorganisms (e.g. Haemophilus parainfluenzae, Eikenella corrodens, and Streptococcus milleri) [Miro et al. 1997]. The sensitivity of blood cultures is over 90% if they are sent before administration of antibiotics. Culture-negative IE is mostly a consequence of prior antibiotic usage [Brouqui and Raoult, 2001]. Diagnosis of culture-negative IE is made by modified culture conditions, serology, molecular techniques, or immunohistology of the surgically removed specimens. When suspicious for IE, transthoracic echocardiography is sensitive for detecting vegetations and identifying the affected valves. Overall, the sensitivity is 60–70%, and it can detect tricuspid vegetations with higher sensitivity (80%) [Brouqui and Raoult, 2001; Winston and Bolger, 2006; San Roman et al. 1993]. Blood cultures were positive for the cases in the present study. The Duke criteria for IE were applied, and each case was classified as either a definite or possible IE; rejected cases were excluded.
In right-sided IE, the usual manifestations are persistent fever, bacteremia, and multiple pulmonary embolisms [Moss and Munt, 2003]. The majority (80%) of these IDUs are 20–40 years old and male, the sex ratio being 4–6:1 [Baddour et al. 2005]. It is difficult to predict the presence of IE from the history and physical examination findings alone [Weisse et al. 1993]. In our first case, the patient was referred with the complaint of abdominal distension and the physical examination was significant for pulmonary ral and roncus. The second case was admitted with a history of cough, fever, appetite loss, fatigue, and dyspnea of 1 week, and the physical examination was normal.
Similar to other causative agents of IE, treatment of IE in IDUs is still largely dependent on antimicrobial chemotherapy. The choice of antibiotics essentially depends on the likely microorganisms, involved valves, and the types of injected drugs the patient has used. In IDU-related IE, the duration of antibiotic therapy is normally 4–6 weeks [Winston and Bolger, 2006; San Roman et al. 1993]. In the present cases, vancomycin, gentamicin, and oxacillin were preferred for the patient with methicillin-sensitive Staphylococcus aureus; while vancomycin and gentamicin were preferred for the patient with methicillin-resistant Staphylococcus aureus. The duration of the treatment was 6 weeks for both patients. Surgical intervention is indicated if the patient has refractory heart failure, persistent or recurrent infections including bacteria and fungi, prosthetic valves, development of a ring abscess, fistulae, or worsening conduction abnormalities. In both of our patients, early surgical approach was indicated because of septic recurrent pulmonary embolisms from vegetations during the active stage.
Although, it is standard procedure that operations are performed under cardiopulmonary bypass, some patients with TVIE cannot tolerate it because of severe lung injury as a result of pulmonary embolism. If it is possible, tricuspid valve repair is now the choice of surgical option for patients with TVIE. However, we believe that if tricuspid destruction is severe and not suitable for valve repair due to infection, involves all three leaflets and the subvalvular apparatus, tricuspid valve replacement is indicated. In the present cases, the surgeries were performed under cardiopulmonary bypass, however, valvular repair was not possible. Thus, we chose bioprosthetic tricuspid valve replacement for the treatment of choice. There were no side effects of the biologic valves during the follow-up period in both patients.
There has been a continuous debate as to whether it is ethical to withhold valve surgery in an active, noncompliant IDU. The first-valve surgery is normally offered to those patients who are willing to undergo a drug rehabilitation program and be compliant with treatment. However, any IDU who becomes noncompliant, relapses, and acquires a second episode of IE generally will not be offered further valve surgeries [Yeo et al. 2006].
Conclusion
We report two rare surgical cases of isolated TVIE in young IDUs and the clinical outcomes. We believe that tricuspid bioprosthetic valve replacement can be performed safely for a surgical option in patients with TVIE with regard to freedom of recurrence of IE and valvular competence.
Footnotes
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
Conflict of interest statement
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
