Abstract
Scrub typhus shows a high prevalence in South-East Asia. In pregnant females, it can cause both maternal and fetal adverse outcomes. We report a case series of two women with scrub typhus and their varied outcomes.
A 25-year-old primigravida treated for scrub typhus at 23 weeks' gestation presented at 34 weeks with stage three fetal growth restriction (FGR). Caesarean delivery was performed. The neonate had biliary atresia.
A 24-year-old primigravida at 31 weeks' gestation was referred from a local hospital due to scrub typhus induced multi-organ dysfunction. She had FGR stage 1 with oligohydramnios. Emergency caesarean delivery was performed in view of acute fetal bradycardia.
There is an emerging need for research to reassess what is already known about scrub typhus in pregnancy and to develop techniques for its treatment inorder to achieve a positive maternal and neonatal outcome in these cases.
Introduction
Scrub typhus, a chigger transmitted zoonotic disease caused by intracellular obligate bacterium Orientia tsutsugamushi and the newly identified Candidatus Orientia chuto, has struck back globally in terms of geographical expansion beyond traditional areas of endemicity, as well as associated morbidity and mortality. 1 Community seroprevalence has been found to be as high as 34.2% across several states of India. 2 The impact of Scrub typhus during pregnancy in terms of clinical severity, diagnosis, optimal management as well as fetal outcome is a clinical priority. There are anecdotal reports of adverse outcomes for both the mother and the baby due to scrub typhus in pregnancy.
Here, we describe two women with scrub typhus detected and managed at a tertiary care centre and their maternal and neonatal outcomes with a brief discussion on available evidence of scrub typhus in pregnancy.
Case report
Case 1
A 25-year-old woman in her first pregnancy at 23 weeks of gestation with no known co-morbidities presented to the antenatal clinic with a history of fever for six days. She was admitted for further evaluation. She was negative for malaria and dengue by peripheral smear examination and Immunoglobulin M (IgM) capture Enzyme-Linked Immunosorbent Assay (NIV IgM capture ELISA (MAC-ELISA)) respectively. She was positive for IgM antibodies for scrub typhus by ELISA (InBios International, Inc., Seattle, WA, USA), for which she was treated with oral azithromycin 500 milligrams for five days. The patient was discharged in a stable condition and advised to return for fortnightly review in the antenatal clinic, but she was lost to follow-up and subsequently presented at 34 weeks of gestation with the complaint of inability to perceive fetal movements for three days. Trans-abdominal ultrasonography (TAS) was performed, which showed a single live intrauterine fetus with an estimated fetal weight (EFW) of 1553 grams, which was below the third centile for gestational age. A diagnosis of fetal growth restriction (FGR) was made and Doppler ultrasonography was performed which showed reversal of end-diastolic flow in the umbilical artery (UA). Other causes of FGR were ruled out by normal blood pressure recordings, negative TORCH profile (toxoplasma, rubella, cytomeglovirus and herpes), and a normal glucose tolerance test. Intramuscular dexamethasone was given for fetal lung maturity and magnesium sulphate was given for fetal neuroprotection. Caesarean delivery was performed in view of FGR stage three beyond 32 weeks of gestation. 3 She delivered a female baby, weighing 1580 grams, who was admitted to the neonatal intensive care unit (NICU) in view of prematurity and low birth weight. The neonate subsequently developed cholestatic jaundice. Hepatobiliary Iminodiacetic Acid (HIDA) scan was performed which was suggestive of biliary atresia. The mother recovered well post-operatively.
Case 2
A 24-year-old unbooked primigravida who had had an uncomplicated antenatal course presented at 31 weeks of gestation with fever and malaise for eight days along with yellowish discolouration of sclera, dark urine and rash on the mouth for four days. On examination, an eschar was seen at the right angle of the mouth (Figure 1). The patient was referred from a local hospital in view of scrub typhus IgM positivity by ELISA, deranged liver function tests in the form of hyperbilirubinemia with raised serum transaminase levels and features of acute kidney injury and pneumonitis, suggestive of scrub typhus induced multi-organ dysfunction. The patient was admitted for further evaluation. Intravenous ceftriaxone and meropenem were initiated alongside oral azithromycin, following multidisciplinary discussion including Dermatology and General Medicine teams. TAS was performed which revealed a single live intrauterine fetus with EFW of 1456 grams (below the third centile for gestational age), and an amniotic fluid index (AFI) of 2.5 centimetres. Ultrasound Doppler was performed in view of FGR with oligohydramnios which was normal. Further evaluation failed to reveal any other cause of FGR. A diagnosis of scrub typhus induced FGR stage 1 with oligohydramnios was made. 3 Intramuscular dexamethasone was given for fetal lung maturity. Maternal vital signs were monitored regularly, as was urine output and bloods including renal and liver function. Fetal monitoring was performed by daily fetal movement count, serial non-stress tests (NST), and weekly AFI with Doppler monitoring. TAS performed after one week showed a cerebro-placental ratio of less than one, AFI was nil and NST showed prolonged fetal bradycardia. Emergency caesarean delivery was performed in view of acute fetal bradycardia. She delivered a female baby weighing 1545 grams. The baby was admitted to NICU in view of prematurity with low birth weight. During the postpartum period, the mother developed a secondary bacterial lung infection due to Klebsiella pneumoniae, which was treated with injection colistin. Both the mother and the baby were discharged in stable condition after fourteen days of hospitalization with follow up planned in the medicine, dermatology and obstetric clinics.
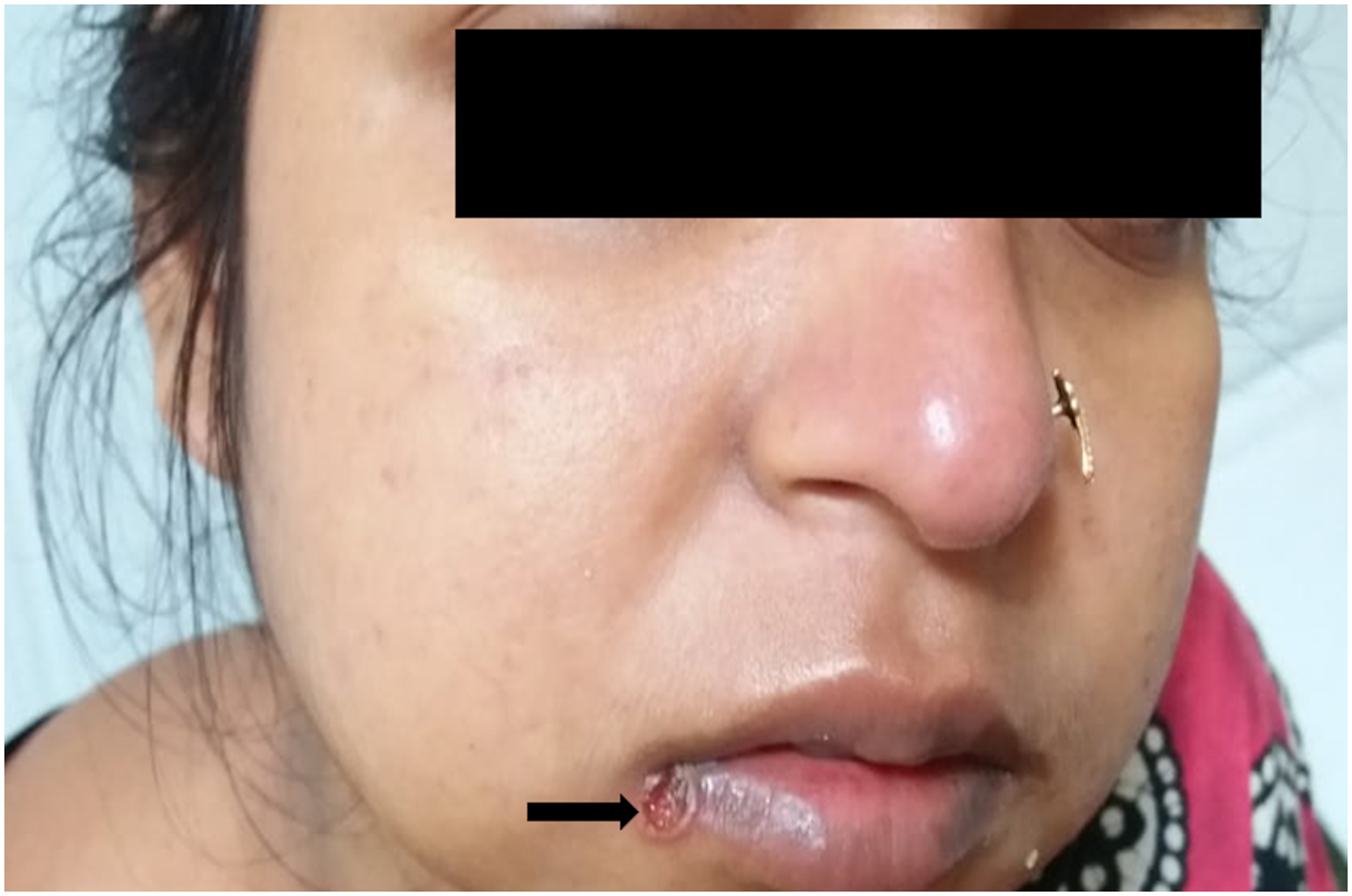
Eschar (arrow) seen at the right angle of the mouth.
Discussion
The clinical presentation, complications and response to treatment with antibiotics in scrub typhus vary among adults, children and high-risk populations such as pregnant females.2,4,5 Unfortunately, awareness about scrub typhus amongst physicians and obstetricians still remains rudimentary despite the prevalence of the disease in the South-East Asian region, which comes under the “tsutsugamushi triangle”. 6 The initial manifestation in the area of the chigger bite is a painless necrotic ulcer called the eschar, which can commonly be missed. This is followed by multi-systemic involvement which can range in severity from self-limited febrile illness to multi-organ dysfunction and even death in some cases. Maternal pneumonia, pulmonary oedema, congestive heart failure, central nervous system dysfunction and even mortality have been reported. Fetal adverse outcomes like miscarriage, stillbirth, preterm delivery, small for gestational age fetus, fetal growth restriction and low birth weight have also been noted. 6–8
Cases of scrub typhus in pregnancy have been reported before. 5 Older studies show a generally favourable feto-maternal outcome when treated with azithromycin 500 milligrams for three to five days. 5 However, antibiotic resistance is a growing concern and adverse feto-maternal outcomes, despite treatment with azithromycin have been increasingly reported. In a retrospective study conducted in 2015 by Rajan et al., fetal loss was seen in 42.4% of women and preterm births were noted in 9.1% despite treatment with injectable azithromycin 500 milligrams for one week. 6 McGready et al. also found that maternal treatment with azithromycin did not improve neonatal outcomes in women with scrub typhus. 7 At our centre also, the first case, despite receiving treatment for scrub typhus in the second trimester, developed FGR stage three in the third trimester. The second case describes a more severe form of scrub typhus presenting with multi-organ dysfunction with FGR stage one in the third trimester. Both women received treatment with azithromycin. The second woman was given ceftriaxone and meropenem in addition in view of multiorgan dysfunction.
Maternal hepato-biliary system involvement with hepatotoxicity has been reported in women with scrub typhus, with severity ranging from transient transaminitis to fulminant hepatic failure. 9 However, to the best of our knowledge, neonatal biliary atresia in babies of mothers with antenatal scrub typhus has not been reported before. This is interesting since biliary atresia is a complex disease resulting from interactions between multiple susceptibility loci and environmental factors like viral infections. 10 Whether maternal scrub typhus could also be a contributing environmental factor is worth exploring.
There is a need for research to learn more about scrub typhus in pregnancy and its possible adverse effects on mother and fetus. Developing techniques for screening as well as new treatments are also important clinical priorities. Interventions could include: i) Screening for scrub typhus amongst pregnant women in disease-prone areas by IgM ELISA ii) Studies to assess the utility of higher antibiotics/ multi-drug therapy, especially since the proven therapy by tetracyclines cannot be considered in pregnant women and azithromycin is not associated with an improved neonatal outcome iii) Establishment of a registry of scrub typhus in pregnancy to note the maternal and neonatal outcomes.
Conclusion
To conclude, scrub typhus is a common burden in a large part of the developing world and its effects on pregnancy outcomes are potentially concerning. These two cases highlight serious feto-maternal adverse outcomes associated with scrub typhus in pregnancy. There is an emerging need for further research on this topic to achieve a positive outcome for both the mother and the baby.
Footnotes
Declaration of conflicting interests
The authors declare that there is no conflict of interest.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article
Ethical approval
All India Institute of Medical Sciences, Bhubaneswar does not require ethical approval for reporting individual cases or case series.
Informed consent
The patient provided written informed consent for the publication of this case report.
Guarantor
On behalf of all authors, Dr Sweta Singh will act as the guarantor and will guarantee the manuscript's accuracy and contributorship of all co-authors.
Authorship and contributorship
Dr Advika Thamarai Selvan collected the data, designed the case report and played a central role in writing the manuscript. Dr Ishita Agarwal defined the concepts and helped in patient management. Dr Sweta Singh conceived the idea, managed the cases and helped with patient recruitment and data collection. Dr Bijayini Behera helped in confirming the diagnosis of the cases. All authors have read the manuscript and agree to its final version being published.
