Abstract
Background:
Extracellular adenosine 5′-triphosphate (ATP) plays important mechanistic roles in pulmonary disorders in general and chronic obstructive pulmonary disease (COPD) and cough in particular. The effects of ATP in the lungs are mediated to a large extent by P2X2/3 receptors (P2X2/3R) localized on vagal sensory nerve terminals (both C and Aδ fibers). The activation of these receptors by ATP triggers a pulmonary-pulmonary central reflex, which results in bronchoconstriction and cough, and is also proinflammatory due to the release of neuropeptides from these nerve terminals via the axon reflex. These actions of ATP in the lungs constitute a strong rationale for the development of a new class of drugs targeting P2X2/3R. DT-0111 is a novel, small, water-soluble molecule that acts as an antagonist at P2X2/3R sites.
Methods:
Experiments using receptor-binding functional assays, rat nodose ganglionic cells, perfused innervated guinea pig lung preparation ex vivo, and anesthetized and conscious guinea pigs in vivo were performed.
Results:
DT-0111 acted as a selective and effective antagonist at P2X2/3R, that is, it did not activate or block P2YR; markedly inhibited the activation by ATP of nodose pulmonary vagal afferents in vitro; and, given as an aerosol, inhibited aerosolized ATP-induced bronchoconstriction and cough in vivo.
Conclusions:
These results indicate that DT-0111 is an attractive drug-candidate for the treatment of COPD and chronic cough, both of which still constitute major unmet clinical needs.
The reviews of this paper are available via the supplementary material section.
Introduction
Adenosine 5′-triphosphate (ATP) is found in every cell of the human body, where it plays a major role in cellular metabolism and energetics. ATP is released from cells under physiologic and pathophysiologic conditions. 1 Extracellular ATP acts as an autocrine and paracrine agent before it is rapidly degraded to adenosine 5′-diphosphate (ADP) and adenosine by ecto-enzymes (mainly, CD39 and CD73).2,3 The effects of extracellular ATP are mediated by P2 cell surface receptors (P2R), which are divided into two families: P2YR, seven trans-cell membrane domain G protein coupled receptors; and P2XR, trans-cell membrane cationic channels. 4 Various cell types in the airways express P2R. 5
In 1996, Pelleg and Hurt demonstrated for the first time that extracellular ATP is a potent activator of the canine pulmonary vagal sensory nerve fibers in vivo. 6 This action was mediated by bimodal P2XR, which respond to both mechanical (stretch) and chemical (e.g. capsaicin) stimuli. 6 In the same year, Pellegrino and colleagues showed that aerosolized ATP is a potent bronchoconstrictor in human subjects. 7 Based on these and additional early studies, Pelleg and Schulman hypothesized that extracellular ATP plays an important mechanistic role in pulmonary pathophysiology in general, and chronic obstructive pulmonary disease (COPD) in particular. 8 Since then, numerous studies have generated voluminous data supporting this hypothesis. 9 Regarding the effects of ATP on vagal sensory nerve terminals in the lungs, it was subsequently shown that, in addition to vagal C fibers, ATP stimulates also the vagal Aδ fibers by activating P2X2/3R. 10 This is in agreement with the documented expression of P2X3 in rat 11 and human nodose ganglion. 12 The stimulation of C fibers by ATP results in pronounced bronchoconstriction, and it can also trigger cough as both C and Aδ fibers mediate cough.13,14 The stimulation of vagal sensory nerve terminals could also have pro-inflammatory effects mediated by axon reflex and localized release of neuropeptides. 15 Taken together, the aforementioned data constitute a strong rationale for targeting P2X2/3R in the lungs as a novel therapeutic pathway in the treatment of COPD and chronic cough. Indeed, a recent phase II clinical trial has shown that a P2X2/3R antagonist, Gefapixant® (other names: AF-219; MK-7264) could be an effective antitussive drug in patients with chronic cough. 16
Here, we report on in vitro and in vivo proof-of-concept studies with DT-0111, a novel small water-soluble molecule that acts as a selective antagonist at P2X2/3R sites being developed as a drug-candidate for the treatment of COPD and chronic cough. The present data show that DT-0111 neither activated nor blocked P2YR, and it markedly attenuated ATP-induced current in nodose ganglionic cells, ATP-triggered neural action potentials in nodose ganglionic fibers, and aerosolized ATP-induced bronchoconstriction in both anesthetized and conscious guinea pig models.
Materials and methods
All studies, which were approved by the relevant Institutional Review Boards, followed the National Institutes of Health guide for the care and use of Laboratory animals (NIH Publications No. 8023, revised 1978).
Does DT-0111 affect P2YR signal transductions?
Functional assays in vitro were carried out by the Department of Pharmacology of the University of North Carolina [National Institute of Mental Health Psychoactive Drug Screening Program (NIMH-PDSP)] utilizing previously described methods. 17
Effect of DT-0111 on ATP-induced current in nodose ganglionic cells
Nodose ganglia from 17-day-old rats were dissected, treated with collagenase and trypsin and dissociated into single cells. 18 The cells were maintained in tissue culture for ~36 h. For electrophysiological recording, cells were bathed in a HEPES buffered physiological saline solution at room temperature. Whole cell patch-clamp recordings were made using Cs+-based pipette solution. Neurons were voltage-clamped at −60 mV. Drugs were applied by localized microperfusion. ATP (agonist) was applied for 1 s at 3-min intervals. DT-0111 (10 µM) was allowed to equilibrate for 2 min prior to application of agonist.
Effect of DT-0111 on ATP-induced neural action potentials in a guinea pig lung-vagus preparation ex vivo
The innervated guinea pig lung preparation was prepared as was described previously.19,20 The response to ATP (10 µM; 1 ml, slowly infused into trachea and pulmonary artery) was assessed as the number of action potentials it elicited. Two control responses 15 min apart were recorded. There were no differences in the number of action potentials evoked between the first and second response (p > 0.1). Subsequently, the lung was superfused and perfused via both trachea and pulmonary artery for 15 min with increasing concentrations of DT-0111 and the ATP challenge was repeated. The data were quantified as the total number of action potentials evoked and the peak frequency (Hz) as measured by the most action potentials evoked in any 1 s bin. DT-0111 was prepared in distilled water as a 10 mM solution, and aliquots were stored frozen at −20°C (1–5 days).
Effect of aerosolized DT-0111 on aerosolized ATP-induced bronchoconstriction in anesthetized guinea pig
Male Dunkin-Hartley guinea pigs (220–250 g, Charles River) were quarantined for 14 days. The housing room was constantly ventilated, and the temperature kept at 23°C. The mean body weight of the guinea pigs on the day of the experiment was 336.0 + 9.9 g. Anesthesia was induced by using a mixture of ketamine + xylazine (40–80 mg/kg + 5–10 mg/kg; IM) as published previously. 21 Supplementary anesthetic doses (one-quarter to one-half of the original dose) were administered as needed if an ear pinch changed the respiratory rate or upon manifestation of an accelerated heart rate. Body temperature was monitored continuously with a rectal thermometer and maintained at approximately 36.5°C using a heating pad and lamp. The trachea was cannulated below the larynx and connected to a pneumotachograph to measure the airflow via a differential pressure transducer (ML141, AD Instruments, Castle Hill, NSW, Australia). Animals were exposed to a gas mixture of 30% oxygen in nitrogen throughout the experiment and ventilated at a constant frequency (fR) of 70–75 breaths/min with a tidal volume at 2.5 ml, which was adjusted to keep an end tidal pressure of CO2 (PETCO2) at ~40 torr. Solutions of ATP (Sigma-Aldrich) used for aerosol challenge were freshly made just prior to use by dissolving the powder in 0.9% saline (NaCl) solution. DT-0111 solutions used for aerosol administration were freshly made by dissolving the powder in 0.9% saline (NaCl) solution. Control (saline) and test solutions were aerosolized by a vibrating mesh nebulizer (Ireland Ltd., Galway Ireland, AG-AL1100). The volume of the nebulizer’s reservoir is ~10 ml. The output rate of delivered aerosol was 0.5 ml/min with an aerodynamic mass median diameter of 3.7 µm (manufacture’s indications). The aerosol generated by the nebulizer was mixed with the airflow (1000 ml/min) to flow into a plastic cylinder (16 mm diameter). The latter loosely jacketed the inspiration inlet (4.5 mm diameter) of the ventilator, by which the guinea pig was ventilated with the aerosol delivered from the ventilator.
The side branch of the tracheal cannulation was connected to a pressure transducer (Statham Instruments Inc., Hato Rey, Puerto Rico). The pressure signal was preamplified by a bridge amplifier (AD Instruments Inc., Colorado Springs, CO, USA) and then digitized and recorded. The pressure signal was precalibrated with known water pressure (cm H2O). The pressure signal and animal rectal temperature were monitored and digitally recorded continuously in computer files throughout the experiment using the PowerLab/8sp data acquisition system (AD Instruments) with Dell XPS 8700 computer equipped with Microsoft Windows 7 and LabChart Pro 7 software (ADInstruments).
After adequate anesthesia was established, the animal in supine position was placed in a standard chemical fume hood (size: 3 × 6 ft) where the ventilator and nebulizer were also located. After stabilization of signals (body temperature, airflow, and tracheal pressure) for 3–5 min (baseline conditions), the animal was exposed to a given dose of aerosolized ATP [0.5, 1.5 or 4.5 mg/ml; low (L), middle (M) and high (H), respectively] for 2 min. Following recovery, the animal was exposed to either another dose of ATP or the same dose of ATP ~10 min after inhalation of DT-0111 aerosol administered for 2 min. The interval between the first and second aerosol exposure was approximately 30–45 min. Tracheal pressure values were obtained 10 s before (baseline, BL) and at the largest response value (peak) during or after ATP exposure. The data was expressed as either the absolute number or percent change from the baseline value (∆%) (after versus before aerosol inhalation). All group data were expressed as the means and compared before versus after aerosol.
Estimated amount of DT-0111 inhaled into the airways and lungs
The aerosol exposure lasted 2 min, during which 6 mg DT-0111 was mixed with 2000 ml airflow (1000 ml/min). The animal ventilation was 300 ml/2 min. Therefore, 6 mg × (300 ÷ 2000) = 0.9 mg, which is the approximate amount of DT-0111 inhaled into the airways and lungs during 2 min exposure. Based on the average body weight (336.0 g), the inhaled DT-0111 was 2.6 mg/kg.
Effects of aerosolized DT-0111 on aerosolized ATP-induced bronchoconstriction and cough in conscious free-moving guinea pigs
After adaptation, the first group of animals was placed in a standard double-chamber apparatus (PLY3355, Buxco Electronics Inc., Troy, NY) and exposed to six solutions of escalating ATP concentrations (0, 1.5, 3.0, 6.0, 12.0, and 24.0 mg/ml) to measure the specific airway resistance (sRaw) (PMID: 29187212). Each challenge consisted of 1 min aerosol exposure followed by a 1 min postexposure period such that the whole set of six challenges lasted 12 min. Approximately 2 h later, the animal was exposed to aerosolized DT-0111 (DT; 12 mg/ml) for 2 min and, 3 min later, the same set of aerosolized ATP challenges was repeated. The second group of animals was placed in a whole body plethysmograph chamber (model PLY3215, Buxco Electronics Inc., Troy, NY) for recording coughs. Figure 1 is a diagram of the experimental set-up used for studying conscious animals. As shown in Figure 1, the plethysmograph chamber was continuously flushed with normoxic (21% O2 and 79% N2) room air at a rate of 2.0 l/min. The same amount of air was drawn from the chamber through its base outlets using a Buxco bias flow regulator to keep the chamber bias flow balanced. Solutions of ATP or DT-0111 were aerosolized by using a vibrating mesh nebulizer (Ireland Ltd., Galway Ireland, AG-AL1100). The output rate of delivered aerosol was ~0.5 ml/min with droplet size (volume median diameter) of 2.5–4.0 µm (manufacture’s indications). The aerosol was mixed with airflow and delivered directly into the chamber. Following stabilization, guinea pig #1 was exposed to aerosolized ATP at 6 mg/ml, 24 mg/ml, and then 48 mg/ml for 5 min with an interval of 30 min between consecutive challenges. The remaining guinea pigs (#2–6) were exposed to 48 mg/ml aerosolized ATP for 5 min. After a recovery period of approximately 140 min, the same dose of ATP was administered again immediately after the administration of aerosolized DT-0111 (12 mg/ml for 5 min). This dose of DT was based on the results of a previous study in which DT-0111 significantly blunted aerosolized ATP-induced bronchoconstriction in guinea pigs. The cough audio signal and visual behavioral activities of the guinea pigs were monitored continuously, and recorded before (for 3 min) and during aerosol delivery (5 min), and for 20 min after cessation of the delivery of ATP.
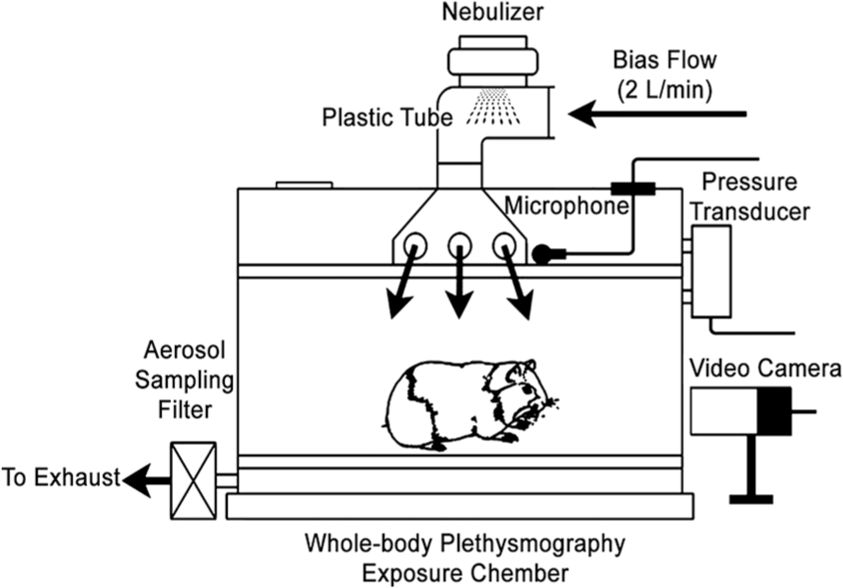
Diagram showing the exposure chamber and setup of cough recording system. Arrows indicate flow direction. The signals generated by video camera, microphone, and pressure transducer were amplified, digitized, and recorded continuously through a PowerLab system (ADInstruments Inc.) and LabChart Pro software (ADInstruments).
Setup of the cough recording system
The setup of the recording system was similar to that used in previous studies and is presented in Figure 1.22,23 The top of the plethysmograph chamber was connected to the nebulizer with a plastic tube. Normoxic air driven by the nebulizer controller was delivered into, and sucked out of, the chamber by the bias flow regulator with the in and out flow volume balanced (2.0 l/min). For cough detection using audio signal, a microphone system was mounted in the roof of the chamber; also, a video camera was placed outside of the chamber to monitor animal behavioral activity. A Buxco pneumotachograph (differential pressure transducer) was attached to the chamber to record airflow. All signals generated by video camera, microphone, and pressure transducer were amplified and recorded continuously by PowerLab/8sp (model ML 785; ADInstruments Inc., Colorado Springs, CO) and a computer with the LabChart Pro 7 software.
Cough count
A typical cough response, as reported before,22–24 was defined by the simultaneous appearance of a transient and great change in the airflow (a rapid inspiration followed by rapid expiration), a typical cough sound with the peak power density at 1–2 kHz in frequency spectrum (sneeze at 3.5–6.5 kHz), and animal body (head) posture and movement.
Aerosolized ATP-induced coughs were counted before and after the administration of aerosolized DT-0111, and the relevant data were compared using paired t test. All group data were expressed as mean ± standard error of the mean (SEM) in the text, tables, and figures. A p value less than 0.05 was considered statistically significant.
Results
Does DT-0111 affect P2YR signal transductions?
In in vitro functional assays (generously provided by the National Institute of Mental Health’s Psychoactive Drug Screening Program, Contract # HHSN-271-2018-00023-C (NIMH PDSP), DT-0111 did not act as an agonist or antagonist at the following receptor sites: P2Y2R, P2Y4R, P2Y6R, P2Y11R, P2Y12R, P2Y13R, and P2Y14R (data not shown).
Effect of DT-0111 on ATP-induced current in nodose ganglionic cells
As can be seen in Figure 2, ATP-induced inward current in rat nodose ganglionic cells was markedly attenuated by DT-0111. This action was dose-dependent and reversed upon washout. The IC50 of DT-0111 inhibition of ATP action was 0.3 µM.

DT-0111 (1.5 µM) abolished ATP-induced inward current in isolated rat nodose ganglionic cells. Upper panel tracings: Left, control effect of ATP; Middle, lack of effect of ATP in the presence of DT-0111; Right, recovery of ATP effect upon washout. Lower panel: Dose response of the attenuation of ATP effect to increasing doses of DT-0111. IC50 = 0.3 µM, n = 3.
Effect of DT-0111 on ATP-induced neural action potentials in a guinea pig ex vivo isolated, perfused lung-nerve preparation
In 3 of 10 preparations studied, the total numbers of action potentials were markedly reduced from 98, 96, and 87 before to 31, 17, and 15 after DT-0111, respectively. This action was reversible upon washout (Figure 3). Like its action on isolated rat nodose ganglionic cells, in all 10 preparations, DT-0111 markedly inhibited the peak frequency (Hz) of ATP-induced action potentials discharge, which averaged 13.4 ± 4.7 Hz and 7.4 ± 1.7 Hz in the absence and presence of drug, respectively (mean ± SEM, p < 0.03) (Figure 4).

DT-0111 antagonized the effect of ATP (10 µM) on nodose ganglion vagal sensory nerve terminals in the innervated guinea pig lung preparation in vitro. Upper panel: a typical example of neural AP recordings: Left, a burst of APs induced by ATP (Control); Middle, DT-0111 markedly suppressed the effect of ATP; Right, recovery of ATP effect after 30 min of DT-0111 washout. Lower panel: Number of APs recorded in the absence (ATP), presence of DT-0111 (1 mM) (ATP + DT), and after washout (ATP + washout). Blue arrows mark the administration of ATP, n = 3.

The peak AP discharge HZ in response to ATP in the absence (black bar) and presence (white bar) of DT-0111 (1 mM).
Effect of DT-0111 on ATP-induced bronchoconstriction in anesthetized guinea pigs
Aerosolized ATP alone caused bronchoconstriction in a dose dependent manner (Figure 5). Figure 6 summarizes the data obtained with DT-0111 in anesthetized guinea pigs in vivo. As can be seen in Figure 6, aerosolized DT-0111 alone did not affect the guinea pigs’ airways. In contrast, DT-0111 markedly attenuated the effect of low, middle, and high doses of ATP on the airways (Figure 6). The percent inhibition of the ATP effect is given in Figure 6..

Aerosolized ATP generally induced elevation of Ptr in a dose-dependent manner. (a) Effect of ATP on Ptr in eight individual guinea pigs. (b) Correlation between Ptr response and ATP concentration using linear and dose response (curved) models, with adjusted R2 0.85 and 0.71, respectively (both p < 0.001), n = 8.
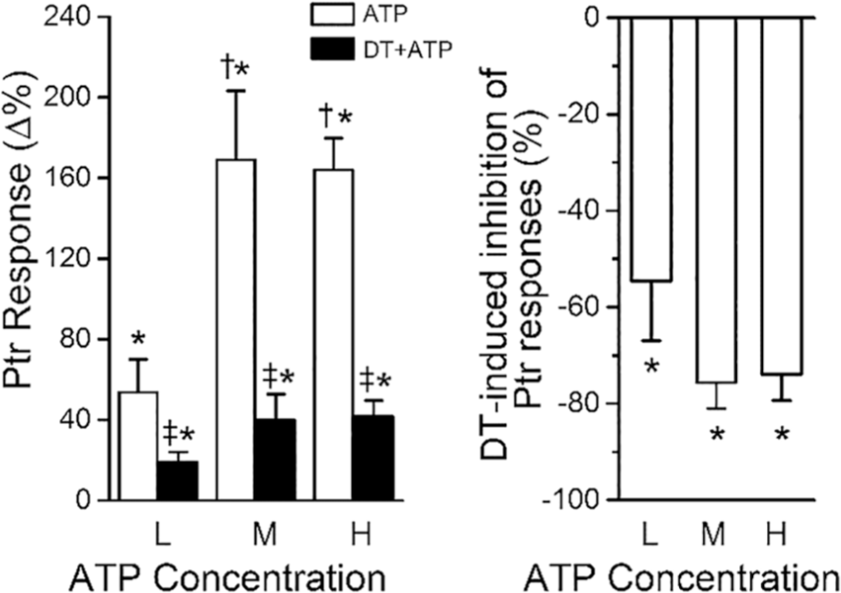
DT-0111 effects on tracheal pressure (Ptr). Left panel: Ptr responses to different ATP doses were significantly suppressed by pretreatment of aerosolized DT-0111. Ptr responses to middle and high ATP concentration were higher than those induced by low ATP dose. Right panel: The averaged percentage of the inhibition of Ptr responses to the three groups of ATP doses by aerosolized DT-0111 are similar in individual guinea pigs. n = 7 for L, M, and H ATP dose, respectively.
The effect of aerosolized DT-0111 on aerosolized ATP-induced bronchoconstriction and cough in conscious free-moving guinea pigs
Figure 7 summarizes the effect of aerosolized DT-0111 on bronchoconstriction induced by increase doses of aerosolized ATP. As can be seen in the figure, DT-0111 effectively abolished the constrictive effect of ATP.

Bronchoconstrictive effect of inhaled increasing doses of aerosolized ATP before and after aerosolized DT-0111 inhalation (DT-0111) in conscious guinea pigs expressed as % change in airways pressure (sRaw).
In all animals tested, aerosolized ATP evoked multiple coughs; a typical example of cough recordings is given in Figure 8, upper panel, and data across all animals are shown in the lower panel. The coughs were characterized by a mixture of bout(s) of coughs and individual coughs (Table 1). Four of six guinea pigs tested presented two bouts and the remaining two showed one bout of coughs.

Effects of DT aerosol inhalation on aerosolized ATP-induced cough response in guinea pigs. Upper panel: typical burst of coughs occurred during exposure to aerosolized ATP (48 mg/ml) for 5 min (left panel), and immediately after the administration of aerosolized DT-0111 (DT, 12 mg/ml; right). The dashed line under the sound trace indicates a bout of coughs, while arrow heads point to individual coughs. In most cases, the sound signal of a cough in bouts of coughs is mainly composed of low audio frequency component (100 Hz or lower) resulting from the body-movement or deep breathing and hardly heard. Lower panel: Number of coughing bouts and number of coughs induced by aerosolized ATP before and after aerosolized DT-0111, n = 5, 6 (ATP and ATP+DT, respectively).
Effects of aerosolized DT-0111 on aerosolized ATP-induced coughs.

ATP, adenosine 5′-triphosphate; BW, body weight; DT, aerosolized DT-0111; SEM, standard error of the mean.
In these cases, the individual coughs (1–3 coughs) occurred after the bout of coughs, with louder cough sound compared with the bout of coughs. In the remaining two of six guinea pigs, individual coughs without bout(s) of cough were observed.
Discussion
The present study indicates that DT-0111, a novel, water-soluble small molecule is a selective antagonist of P2X2/3R, an inhibitor of ATP-induced action potentials in rat and guinea pig nodose ganglionic cells, and, given as an aerosol, a potent inhibitor of aerosolized-ATP induced bronchoconstriction and cough in anesthetized and nonanesthetized guinea pigs, respectively. These results constitute a strong rationale for the development of DT-0111 as a drug-candidate for the treatment of COPD and chronic cough.
Sensory input to the central nervous system from the lungs is mediated by P2X2/3R. 25 In the rat nodose ganglionic neurons, which express almost exclusively heteromeric P2X2/3R, 26 ATP induces inward Ca2+ current by activating slowly desensitizing α,β-methylene-ATP-sensitive P2X2/3R. 18 DT-0111 effectively and reversibly inhibited this action of ATP, indicating that it is a P2X2/3R antagonist (IC50 = 0.3 µM). Functional assays have shown that DT-0111 does not act as an agonist or antagonist at P2YRs. Thus, it can be concluded that DT-0111 acts as a selective antagonist at P2X2/3R sites. Indeed, the activation of the guinea pig pulmonary C and Aδ fibers was markedly attenuated by the P2X2/3R selective antagonist A-317491. 27 In concert with these findings, DT-0111 reduced the number of ATP-induced action potentials in the innervated guinea pig lung preparation (–78%, n = 3), and it reduced the peak frequency (Hz) of ATP-induced action potential from 13.4 ± 1.5 to 7.4 ± 1.7 (mean ± SEM, n = 10, p < 0.03). Importantly, Canning and Mori found in a guinea pig model that cough initiation requires sustained, high-frequency (⩾8-Hz) afferent nerve activation. 28 They also found that a process of summation is involved in cough initiation, 28 which is in congruence with the findings that ATP lowers the threshold for citric-acid-induced cough in the guinea pig.29,30 Interestingly, the guinea pig nodose ganglion C fibers are stimulated also by adenosine (Ado) via the activation of A1AdoR and A2aAdoR. 31 In contrast to ATP. however, Ado does not directly induce bronchoconstriction in either human or canine lungs.13,32,33 This difference between the guinea pig and human lungs is explained by the fact that ATP is a potent trigger of cough in humans, 34 but much less so in guinea pigs, where high doses are required to trigger cough in conscious guinea pigs; in anesthetized guinea pigs it just lowered the threshold for the induction of cough by other tussigenic agents.29,30
The mechanism of cough is not fully delineated; however, it is well established that neural reflexes, the vagus nerve and ionic channels play a critical role in the mechanism of cough. 35 Since ATP stimulates vagal sensory terminals in the lungs by activating P2X2/3R, it is not surprising that ATP is a potent tussigenic agent and a blocker of P2X3R is potentially an effective antitussive agent. 16
The effect of ATP on the guinea pig airways in vivo is the first demonstration of ATP-induced bronchoconstriction in this species; this is in congruence with observations in humans and dogs in vivo,7,13,34,36 and the finding that perfused ATP-induced bronchoconstriction in the guinea pig ex vivo isolated perfused lung-nerve preparation via the stimulation of the nodose ganglion C fibers. 20
COPD is a progressive incurable disease, which still constitutes a critical unmet clinical need. It is the fourth and third leading cause of death worldwide and in the United States (US), respectively. In the US, more than 15 million people are affected by the disease and more than 135,000 people die from the disease each year (www.nhlbi.nih.gov/health/educational/copd/what-is-copd/index.htm). Most current drugs aimed at bronchodilation are long-acting β2-adrenergic receptor agonists (LABA), long-acting muscarinic antagonists (LAMA), or a combination of both. In addition, corticosteroids and other agents that target lung inflammation are used together with bronchodilators, although their benefits in this setting is controversial.37,38 It is now well established that extracellular ATP plays a major mechanistic role in obstructive pulmonary disorders in general and COPD, asthma and chronic cough in particular.9,39 Indeed, the levels of ATP in the lungs of COPD patients is abnormally high (see Pelleg and colleagues). 9 The detrimental effects of ATP are mediated to a large extent by the P2X2/3R localized on vagal afferent terminals, 10 the activation of which causes bronchoconstriction, cough, and the localized release of pro-inflammatory agents. 8 Thus, the blockade of P2X2/3R by selective antagonists has been recognized as an important target for drug development aimed at novel therapeutic approaches for the treatment of COPD and chronic cough.9,16 The present data indicates that DT-0111 is an attractive drug-candidates that could constitute a new therapeutic modality in the management of COPD and chronic cough. Aerosolized DT-0111 effectively inhibited aerosolized ATP-induced bronchoconstriction in anesthetized and conscious guinea pigs in vivo. Extrapolation of the inhaled dose used in the present study indicates that a relatively small amount of DT-0111, that is, 2.9 mg/kg is effective in antagonizing the effects of ATP in the lungs. Importantly, this suggests that use of DT-0111 would not be associated with the side effect (loss of taste sensation) observed with a similar drug-candidate Gefapixant® (other names: AF-219; MK-7264). 16
Study limitations
All present data were obtained using guinea pig models; there is no guarantee that DT-0111 would act effectively and safely in human patients. Also, the number of animals in each of the preparation studied (ranged from 5 to 10) is relatively small. Larger ‘n’ would have provided better support of our conclusions; however, objective difficulties in carrying out the present experiments in particular, those in free moving conscious animals as well as the high costs of the de novo synthesis of DT-0111, limited the number of experiments. Thus, considering that DT-0111 exert its effects by antagonizing ATP at the P2X2/3R, we look at the results in toto to reach our main conclusion that DT-0111 merits its development as a drug-candidate for the treatment of COPD and chronic cough. In addition, although similar P2X2/3R were found to be effective antitussive agents in human patients, they were delivered as oral medications while DT-0111 was delivered as an aerosol in all in vivo studies. Accordingly, it is expected that the pharmacodynamics and pharmacokinetics of DT-0111 would be different from the above-mentioned drug-candidates. Finally, the present studies were carried out using several established models; however, none was either a specific model of COPD or cough (i.e. the animals were healthy). That notwithstanding, two other drug-candidates that are currently in phase II and III clinical trials have used a similar experimental approach in their proof-of-concept studies. Specifically, these drug-candidates were tested for their ability to attenuate the tussigenic activity of ATP. The efficacy demonstrated in these clinical trials validate both the relevance of this experimental approach and our original basic hypothesis that extracellular ATP released from cells during inflammation is mechanistically involved in bronchoconstriction and cough. That notwithstanding, it remains to be determined whether DT-0111 would be as effective bronchodilator and anti-tussive agent in human subjects.
Conclusion
The efficacy of aerosolized DT-0111 in inhibiting neurogenic bronchoconstriction constitute a strong rationale for the continued development of this novel molecule as a drug-candidate for the treatment of COPD and chronic cough.
Supplemental Material
Author_response – Supplemental material for DT-0111: a novel drug-candidate for the treatment of COPD and chronic cough
Supplemental material, Author_response for DT-0111: a novel drug-candidate for the treatment of COPD and chronic cough by Amir Pelleg, Fadi Xu, Jianguo Zhuang, Bradley Undem and Geoffrey Burnstock in Therapeutic Advances in Respiratory Disease
Supplemental Material
DT_paper_suppl_2 – Supplemental material for DT-0111: a novel drug-candidate for the treatment of COPD and chronic cough
Supplemental material, DT_paper_suppl_2 for DT-0111: a novel drug-candidate for the treatment of COPD and chronic cough by Amir Pelleg, Fadi Xu, Jianguo Zhuang, Bradley Undem and Geoffrey Burnstock in Therapeutic Advances in Respiratory Disease
Supplemental Material
Reviewer_1_v.1 – Supplemental material for DT-0111: a novel drug-candidate for the treatment of COPD and chronic cough
Supplemental material, Reviewer_1_v.1 for DT-0111: a novel drug-candidate for the treatment of COPD and chronic cough by Amir Pelleg, Fadi Xu, Jianguo Zhuang, Bradley Undem and Geoffrey Burnstock in Therapeutic Advances in Respiratory Disease
Supplemental Material
Reviewer_1_v.2 – Supplemental material for DT-0111: a novel drug-candidate for the treatment of COPD and chronic cough
Supplemental material, Reviewer_1_v.2 for DT-0111: a novel drug-candidate for the treatment of COPD and chronic cough by Amir Pelleg, Fadi Xu, Jianguo Zhuang, Bradley Undem and Geoffrey Burnstock in Therapeutic Advances in Respiratory Disease
Supplemental Material
Reviewer_2_v.1 – Supplemental material for DT-0111: a novel drug-candidate for the treatment of COPD and chronic cough
Supplemental material, Reviewer_2_v.1 for DT-0111: a novel drug-candidate for the treatment of COPD and chronic cough by Amir Pelleg, Fadi Xu, Jianguo Zhuang, Bradley Undem and Geoffrey Burnstock in Therapeutic Advances in Respiratory Disease
Footnotes
Acknowledgements
We thank Philip M. Dunn, of the Autonomic Neuroscience Institute, Royal Free and University College Medical School, London, United Kingdom for carrying out the experiments with nodose ganglionic cells in vitro.
Funding
The authors received no financial support for the research, authorship, and publication of this article.
Conflict of interest statement
The present studies were supported by Danmir Therapeutics, LLC of Haverford, Pennsylvania, USA (Danmir), which also supplied DT-0111 to all investigators. Other than AP, none of the authors holds any commercial interest in Danmir. AP is a co-inventor of DT-0111; he conceptualized the present studies and wrote the first draft of the manuscript. GB supervised the cellular studies, BU performed the ex vivo guinea pig innervated-lung studies and FX and JZ performed the in vivo guinea pig studies. All authors read the manuscript contributed to its content and approved its submission.
Supplemental material
The reviews of this paper are available via the supplementary material section.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
