Abstract
Eighteen patients with a proximal interphalangeal joint fracture-dislocation involving at least half of the palmar articular surface were treated with hemihamate arthroplasty, achieving a mean of 70° flexion at 14 months. This technique is an effective option for complex injuries.
Proximal interphalangeal joint (PIPJ) dorsal fracture-dislocations (DFD) are challenging injuries that can result in pain and stiffness. Treatment with internal fixation, dorsal blocking wire or external fixation may fail if the palmar articular deficit is significant and unreconstructable.
Hemihamate arthroplasty, described by Hastings et al. (1999), uses the contour of the dorsal distal hamate as an autologous osteochondral graft. This recreates the palmar articular surface of the middle phalanx, restoring congruity and enabling early mobilization. Despite encouraging functional outcomes, concerns remain about technical difficulty, donor site morbidity, graft incorporation and long-term degeneration.
We retrospectively reviewed a consecutive, single surgeon series of hemihamate arthroplasties performed for unstable PIPJ DFDs at our trauma unit. Ethical approval was not required as this study was a retrospective service evaluation. The operating surgeon assessed palmar articular surface loss from pre-operative radiographs and found the defect to be at least 50% in all cases. All patients had unstable injuries that subluxed despite reduction and immobilization attempts in the emergency department, and all were reviewed in a hand fracture clinic to discuss surgical treatment options. The decision to perform hemihamate arthroplasty as an early definitive solution was made where there was a very large joint defect of at least 50%, and where stable reconstruction could not be achieved using alternative techniques. Smaller defects would be acutely treated with reduction of the joint and transfixion with a K wire in our practice. Patients were identified from our operative database and their electronic records were reviewed for clinical and radiological follow up. No patients were excluded.
Eighteen patients were identified between 2010 and 2023 (14 male and four female; mean age, 38 years SD 11.8 years; range, 22–68). The series includes two index fingers, four middle fingers, nine ring fingers and three little fingers. Average time from injury to surgery was 3.5 weeks (range 1–16). Articular surface loss ranged from 50 to 70%. A well-described surgical technique was used (Williams et al., 2002). Median follow-up was 14 months (IQR 5 to 31 months, range 1–60).
At final review, the mean flexion arc was 70° (range 40–100°), excluding one patient who developed late fibrous ankylosis two years after an otherwise unremarkable recovery. Follow-up radiographs showed a preserved joint space and incorporated graft. Two other complications necessitated secondary procedures for stiffness. One at 9 months underwent a dorsal capsule and partial collateral release through a dorsal longitudinal approach which improved flexion from 35° to 95°. The other patient was managed with an external frame applied at 8 months following the index procedure; a Pennig MinifixatorTM distracted the PIPJ 1 mm daily up to 4.3mm, and was removed after 18 days. The patient attended hand therapy for 5 months achieving a 47–98° range of motion before discontinuing further follow-up. There was no record of graft non-union, collapse, infection, donor site pain or radiographic osteoarthritis at final follow up. Figure 1 shows pre- and postoperative lateral radiographs.
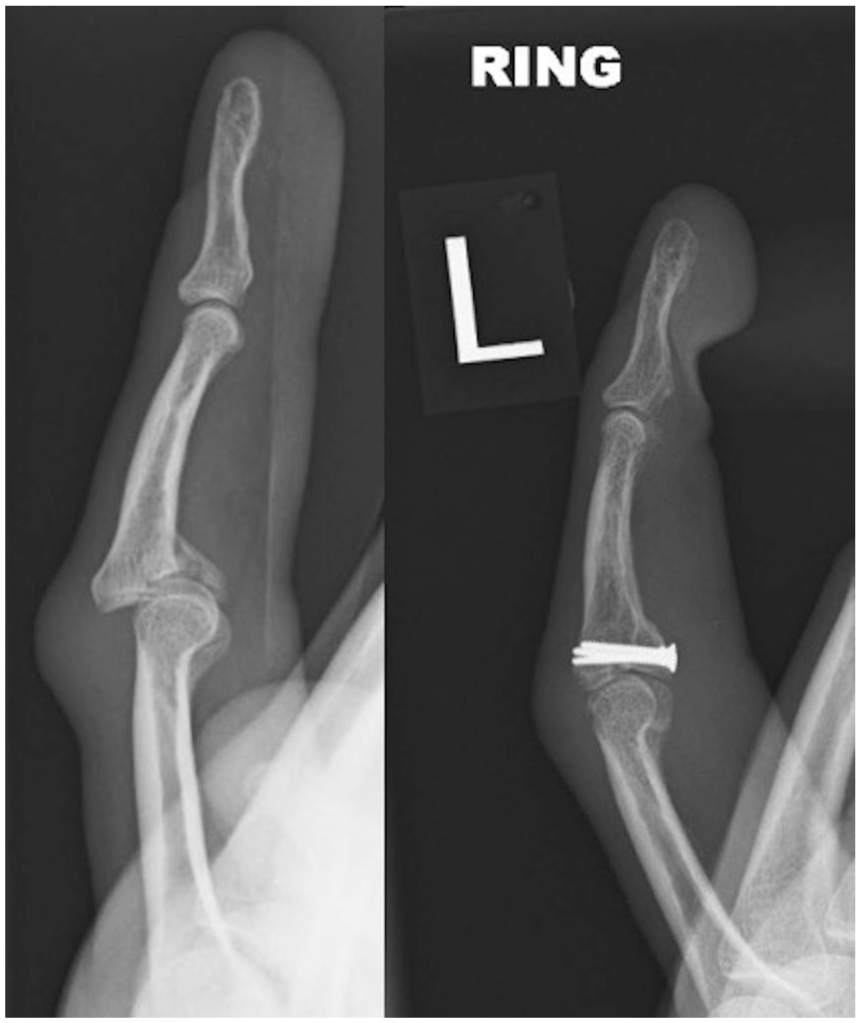
Preoperative and postoperative lateral radiograph of (a) a left ring finger proximal interphalangeal joint dorsal fracture dislocation (b) treated with hemihamate arthroplasty.
Our results align with existing literature. A recent review reported mean arc of 74° and low pain scores, although complications included secondary arthritis (18%) and donor site morbidity (3%) (Faulkner et al., 2023). Brennan et al. (2024) found that flush, rather than oversized, grafts yield better motion, challenging the notion that extra bulk improves stability. Donor site morbidity and persistent pain remain concerning in the literature; we performed careful donor site capsule closure and this complication was not identified in this study.
Although hemihamate arthroplasty is generally regarded as a salvage procedure for chronic injuries, we found it valuable in acute unstable DFDs with unreconstructable articular defects ⩾50% with an intact dorsal cortex.
This study is limited by its retrospective design, small sample size, variable duration of follow-up and subjective estimation of articular defect size from the radiographs. This series was performed by a single, highly experienced hand surgeon, which may limit generalizability but reflects the technical demands of the procedure.
In summary, hemihamate arthroplasty provided reasonable outcomes in PIPJ DFD patients with over 50% palmar articular loss. Our findings confirm that this procedure is safe and reliable for complex PIPJ reconstruction in DFD with large palmar defects in the acute setting.
Footnotes
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article. GH was supported by an NIHR Academic Clinical Fellowship in Trauma and Orthopaedics (ACF-2022-14-008).
Ethical approval
Ethics committee/ Institutional Review Board approval not required. Data was collected as part of routine audit practice.
Informed consent declaration
Not applicable since anonymized de-identified data were used.
