Abstract

Question 1
The palmar cutaneous branch (PCB) of the median nerve

Question 2
High-pressure injection injuries

Question 3
Factitious disorders

Clinical case
This 39-year-old right-handed joiner has suffered a circular saw injury. The wound has been debrided and a metacarpal fracture K-wired by the admitting team. He now presents to you for consideration of soft tissue cover.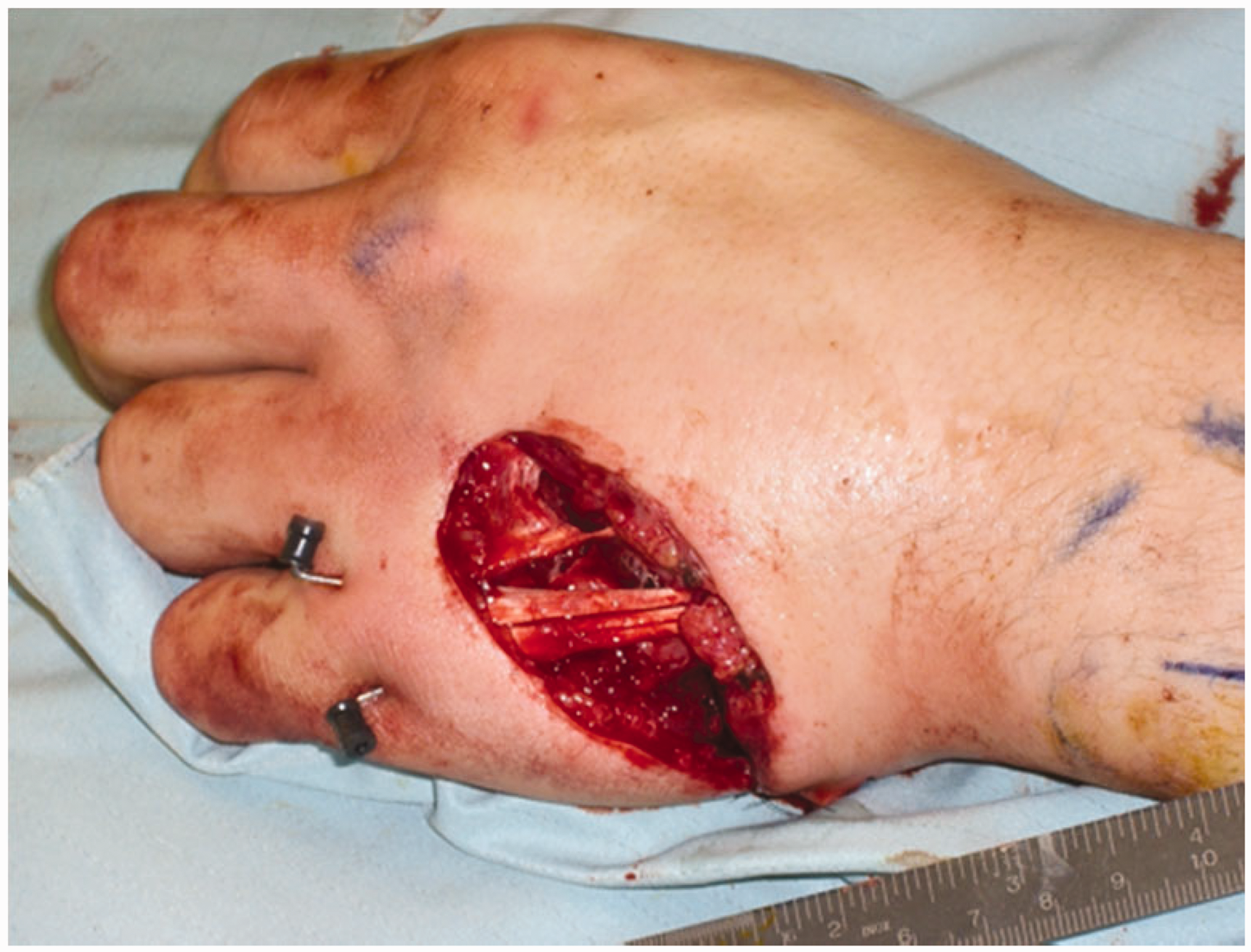
Please describe what you see.
How will you manage this patient? Please assume that the fracture is stable and will not need any further treatment other than to remove the K-wires.
Answers
Question 1
The palmar cutaneous branch (PCB) of the median nerve

The PCB arises from the radial border of the median nerve, 8.5 cm proximal to the wrist crease. It runs between the FCR and palmaris longus and pierces the antebrachial fascia 4.5 cm proximal to the wrist crease. At the wrist, it divides into multiple branches to supply the skin over the thenar eminence and over the central part of the palm (Yu and Chase, 2004).
Question 2
High-pressure injection injuries

High-pressure injection injuries may have a very innocuous looking entry point, usually on the non-dominant index finger. They do not have an exit wound. Oil-based paints and industrial solvents produce more necrosis than water-based paints and grease. Surgical delay of more than 10 hours in exploration and debridement increased the amputation rate. These injuries may be contaminated with Gram-positive and Gram-negative organisms. The prognosis is worse with greater time from injury to decompression, more irritant types of material injected, greater quantity of material injected, greater injection pressure of appliance, the presence of secondary infection and a more distal site of injection (Neal and Burke, 1991). Pinto et al. (1993) reported a salvage rate of 84% with early aggressive debridement. The series by Neal and Burke (1991) saw 3 of 11 fingers amputated.
Question 3
Factitious disorders

Patients with factitious disorders are not infrequent in the hand clinic. Recognizing the diagnosis will avoid extensive unnecessary investigations and treatment (Hobby et al., 2023). The problem usually follows a trivial injury. Wounds are frequently multiple and may be circular or linear. If the area is inaccessible under a plaster cast, the wounds will usually heal. Patients have characteristically attended multiple healthcare providers and had multiple investigations all without any diagnosis being made (Wolfe et al., 2022). Grunert et al. (1991) described stiff index finger, clenched fist posture and dysfunctional finger postures in their series. Burke (2008) categorizes the presentations into self-mutilation, Secretan’s syndrome, body integrity identity disorder, SHAFT syndrome, malingering, pain dysfunction syndrome, somatization and simulation of complex regional pain syndrome type I.
Clinical case answer
Minimal expected knowledge:
There is a large wound over the dorso-ulnar aspect of the hand.
The ring finger extensor tendon appears to be damaged.
You will need to have a strategy to cover this. A dermal substitute is an increasingly popular option, even for exposed structures and you may wish to discuss this.
In this case, a posterior interosseous flap was used, which is a reasonable option for the dorsum of the hand, without sacrificing a major artery.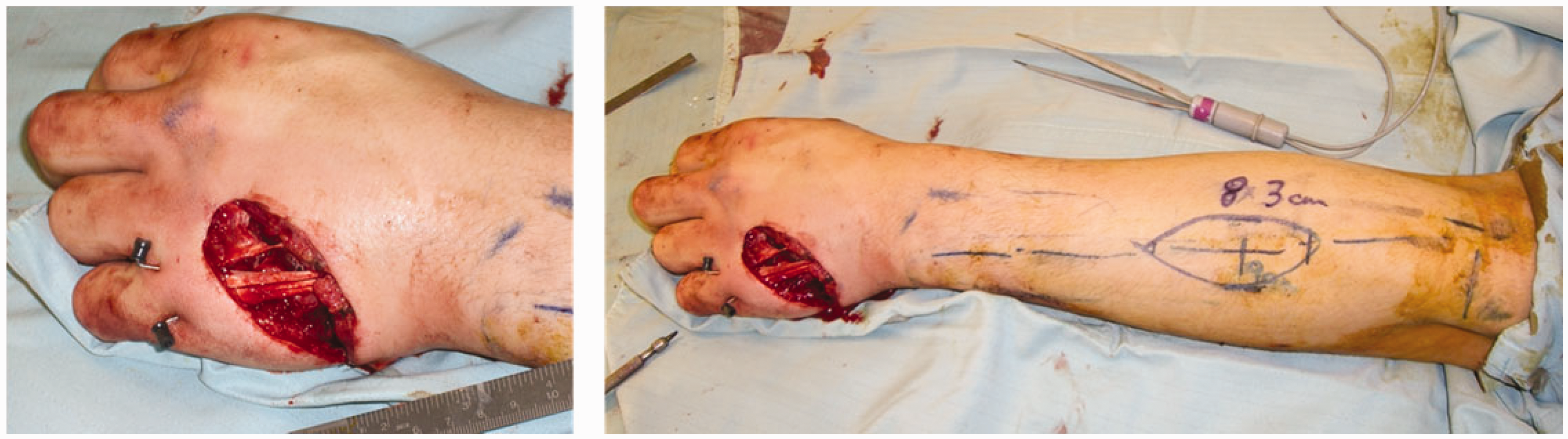
You will need to be able to describe the anatomy, indications and complications of the posterior interosseous artery (PIA) flap. You will need to be able to describe how to plan this.
The PIA flap is classically described as a reverse flow flap, although Angrigiani et al. (1993) and Hubmer (2004) postulate that it is based on the recurrent branch of the anterior interosseous artery. The surface markings of the PIA are drawn out with the elbow flexed to 90° (Hierner et al., 2014). A line is drawn from the lateral epicondyle to the distal radioulnar joint. The flap will be centred on the central third of this line, approximately 9 cm from the lateral epicondyle. The anastomosis between the anterior interosseous artery and PIA needs to be checked first – 5% of patients do not have this anastomosis and the flap will not then work. The rotation point of the flap will be based here, usually approximately 2–2.5 cm proximal to the distal radioulnar joint (Cheema et al., 2007). The artery perforates the intermuscular septum at an average of 7.9 cm (Costa et al., 2007) distal to the lateral epicondyle. It may arise from the common interosseous artery but in 18% of cases arises from the ulnar artery (Costa, 2001). The largest fasciocutaneous perforator arises just distal to the supinator muscle. Costa (2001) emphasizes the important anatomical consideration that the fascial septum between the extensor carpi ulnaris (ECU) and the extensor digiti minimi (EDM) in which the vessels lie is oriented sagittally. Care must be taken to protect the posterior interosseous nerve at the proximal extent of the dissection. In the middle third, the artery lies between the extensor digiti minimi on the radial side and the extensor carpi ulnaris on the ulnar side. At least a 5 mm cuff of fascia should be taken with the pedicle to protect it. Suturing the dermis to the fascia may help prevent shearing (Cheema et al., 2007).
Costa et al. (2007) recorded uneventful healing in 95% after using this flap to cover the dorsum of the hand. Out of 102 flaps, three had to abandoned because of unfavourable anatomy. Cheema et al. (2007) point out the learning curve associated with this flap and the importance of careful dissection proximally.
In this case, you may also be asked about your strategy for reconstructing the extensors. This may either be early, or you may place silastic rods and reconstruct the tendons at a second stage.
