Abstract

Dear Editor,
In 40–80% of children with multiple hereditary exostosis (MHE)/multiple osteochondroma disease, forearm bowing develops owing to distal ulnar growth disturbance. This may be mild to severe depending on the amount of ulnar shortening and associated bowing of the radius. In severe cases, the radial head (RH) may dislocate and lead to marked functional impairment, pain and deformity (Ham et al., 2016). Early distal osteochondroma excision and ulnar tether release has been shown to be beneficial in a small group of six patients (Belyea et al., 2020). There is no clear consensus on when to intervene and which osteochondromas need to be resected to prevent ongoing deformity.
The frequently cited study of Masada et al. (1989) contains a classification of this disease that distinguishes between the location of the osteochondromas (radius/ulna), the length of the radius and ulna, and whether or not RH dislocation is present. Four types are described: Type I (distal ulnar osteochondroma/short ulna), IIa (distal ulna/short ulna and proximal radial osteochondroma with RH dislocation), IIb (distal ulnar osteochondroma/short ulna with RH dislocation) and III (distal radial osteochondroma/short radius). To the best of our knowledge this classification has not yet been formally validated. There are indications that this system is incomplete and does not capture the entire spectrum of possible variations in the forearm. Jo et al. (2017) reported that 65% of MHE cases could not be classified using it. Therefore, they proposed additional Types IVa (distal ulnar and distal radial osteochondromas) and IVb (distal ulnar and distal radial osteochondromas with RH dislocation).
The aim of this study was to compare the inter- and intrarater reliabilities of these two classifications in a group of 15 paediatric upper limb surgeons. A representative sample of 20 consecutive MHE forearm radiographs (anterioposterior and lateral) were selected and distributed via an online survey tool (surveymonkey.com). The radiographs were sent out in a random order to be rated a second time after a 2-week interval. All raters were asked to classify all images using one of the four Masada and six Jo types; alternatively, the image could be rated as ‘unclassifiable/not applicable’ (Figure 1). We calculated the interrater reliability of the two systems using Fleiss’ kappa and established any statistical difference between them using Hotelling’s T-squared test. The intrarater reliability was established using Cohen’s kappa. The statistical difference of unclassifiable cases between the classification systems was determined by a chi-squared test with Yates’ correction for continuity.
This example of multiple hereditary exostoses is difficult to classify. Surgeons rated this as IIa/b or ‘not applicable’ by the classification of Masada et al. (1989), whereas IIa/b, IVb or ‘not applicable’ were preferred using the categories of Jo et al. (2017). This case is prone to misinterpretation since raters may not notice a small osteochondroma. In this particular case, the osteochondromas were located in the mid-diaphysis and not distally.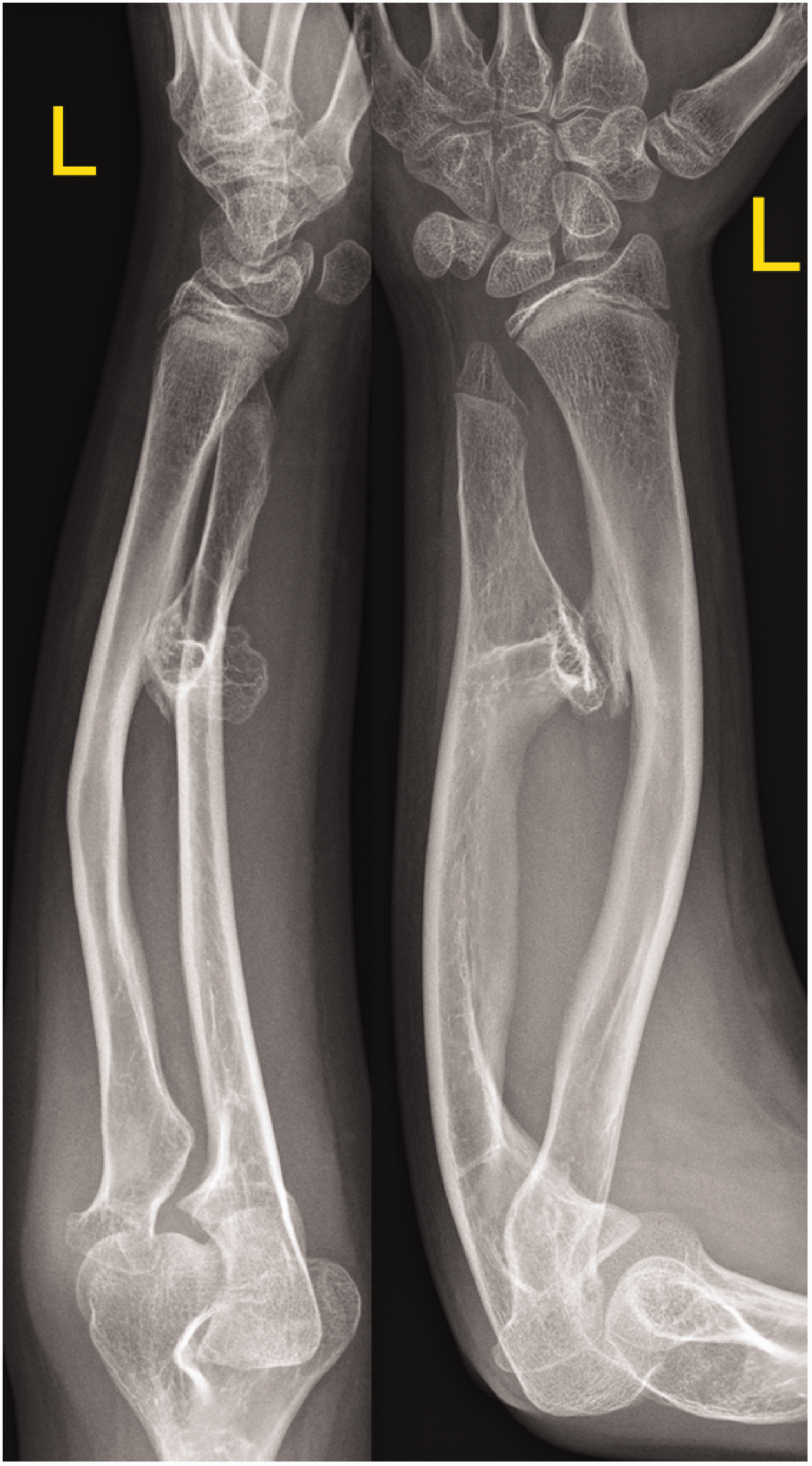
The Masada classification showed a significantly lower interrater reliability for the first and second measurement series (κ = 0.231 and κ = 0.230) compared with the Jo classification (κ = 0.357 and κ = 0.395; p = 0.022 and p = 0.011). While the agreement according to Masada can thus be considered as only fair overall, it was borderline moderate in Jo’s system. No statistically significant difference was found between the two-measurement series in both classifications (p = 0.939 and p = 0.316).
The median intrarater reliability among the group was κ = 0.54 (range 0.13–0.82) within Masada’s system, and κ = 0.60 (range 0.25–0.83) within Jo’s system. The ratings according to Jo showed a significantly lower proportion of unclassifiable cases (8–10% vs 49–52%; p < 0.001). The highest rate of unclassifiable cases in Masada’s system was found for those types that mainly resembled Jo Types IVa. However, Jo’s system was also unable to capture the entire range of existing tumour locations.
Treatment-oriented algorithms depend on a precise description of the pathology. For example, several studies have attempted to determine which factors may be responsible for RH dislocation and poorer outcomes. In our opinion, it may be important for the further clinical course to know whether there are any other osteochondromas besides the main ones described in the different Masada types. The classification of Jo et al. (2017) showed better but only moderate reliability among the experts. Although an excellent agreement overall could not be obtained with either classification, Jo’s system enabled the raters to adequately classify more cases, especially those with both distal radius and ulna osteochondromas. Therefore, we suggest that the system of Jo et al. (2017) should be preferred until a more reliable grading system has been developed.
Footnotes
Acknowledgements
European Paediatric Orthopaedic Society (EPOS) Upper Limb Study Group members are: Eva Pontén, Andrea Jester, Christina Steiger, Nunzio Catena, Francisco Soldado, Giovanni Luigi Di Gennaro, Sergio Martínez-Alvarez, and Sebastian Farr. The authors would like to thank the following collaborators for participation in this study: Rudolf Ganger, Florian Schachinger, Alexandra Stauffer, Marcos Fernandes Carvalho, Ignacio Sanpera, Ismat Ghanem and John Ham.
Declaration of conflicting interests
The authors declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: Sebastian Farr, MD, reports consulting fees from Orthofix Srl (Bussolengo, Italy) outside the submitted work. All other authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The Open Access funding was provided by the Medical University Vienna.
