Abstract
Dear Editor,
Midcarpal instability (MCI) is a poorly understood condition in terms of aetiology and treatment. The typical patients with intrinsic MCI are young women who experience nontraumatic, chronic wrist pain with instability and/or a locking sensation. These patients present with pain mainly located at the triquetro-hamate joint. The wrist is usually lax and a painful clunk is often provoked during the midcarpal shift test. At our hospital, osseous pathologies are ruled out by conventional radiography, and cineradiography is performed to confirm the diagnosis of dynamic midcarpal instability (Sulkers et al., 2018). The primary treatment is hand therapy. Surgery is considered only in case of failed conservative treatment. There is no consensus concerning the best soft-tissue stabilization. The third author (S.D.S) developed and performs a flexor carpi radialis tendon transfer that stabilizes the palmar–radial and dorsal–ulnar sides of the wrist by augmenting the stability of the scaphotrapeziotrapezoidal joint and reefing the radiotriquetral and dorsal intercarpal ligaments (Figure 1). At surgery, the dorsal capsule is opened parallel to the distal part of the radiotriquetral ligament. The radiocarpal and midcarpal joints and the scapholunate ligament are inspected. Volar incisions are made over the distal pole of the scaphoid and on the forearm 8 cm more proximally. Through these incisions, a radial strip of one-third of the flexor carpi radialis tendon is harvested. A K-wire (1.1 mm) is drilled through the scaphoid from proximal–dorsal to distal–palmar emerging just proximally to the distal pole of the scaphoid. A 2.7 mm cannulated drill is then used to create a tunnel. The tendon slip is passed through this tunnel from palmar to dorsal. The distally based slip is fixed on the palmar side at the periosteum of the distal pole of the scaphoid using a 2-0 absorbable suture to set the tension for the sling and to prevent the tendon slip from gliding back and losing tension. The sling then penetrates the radiotriquetral ligament and dorsal intercarpal ligament as a grasping loop and is sutured back to itself with 3-0 absorbable sutures after maximally tightening the tendon. While the wrist is still completely relaxed due to plexus anaesthesia, the carpus is tested for range of motion and anteroposterior translation. In case of too little tension, the anteroposterior translation of the carpus is possible, and this is corrected by further tensioning. The wrist is immobilized for 6 weeks, and then hand therapy begins.
Description of the operative technique in dorsal and lateral view.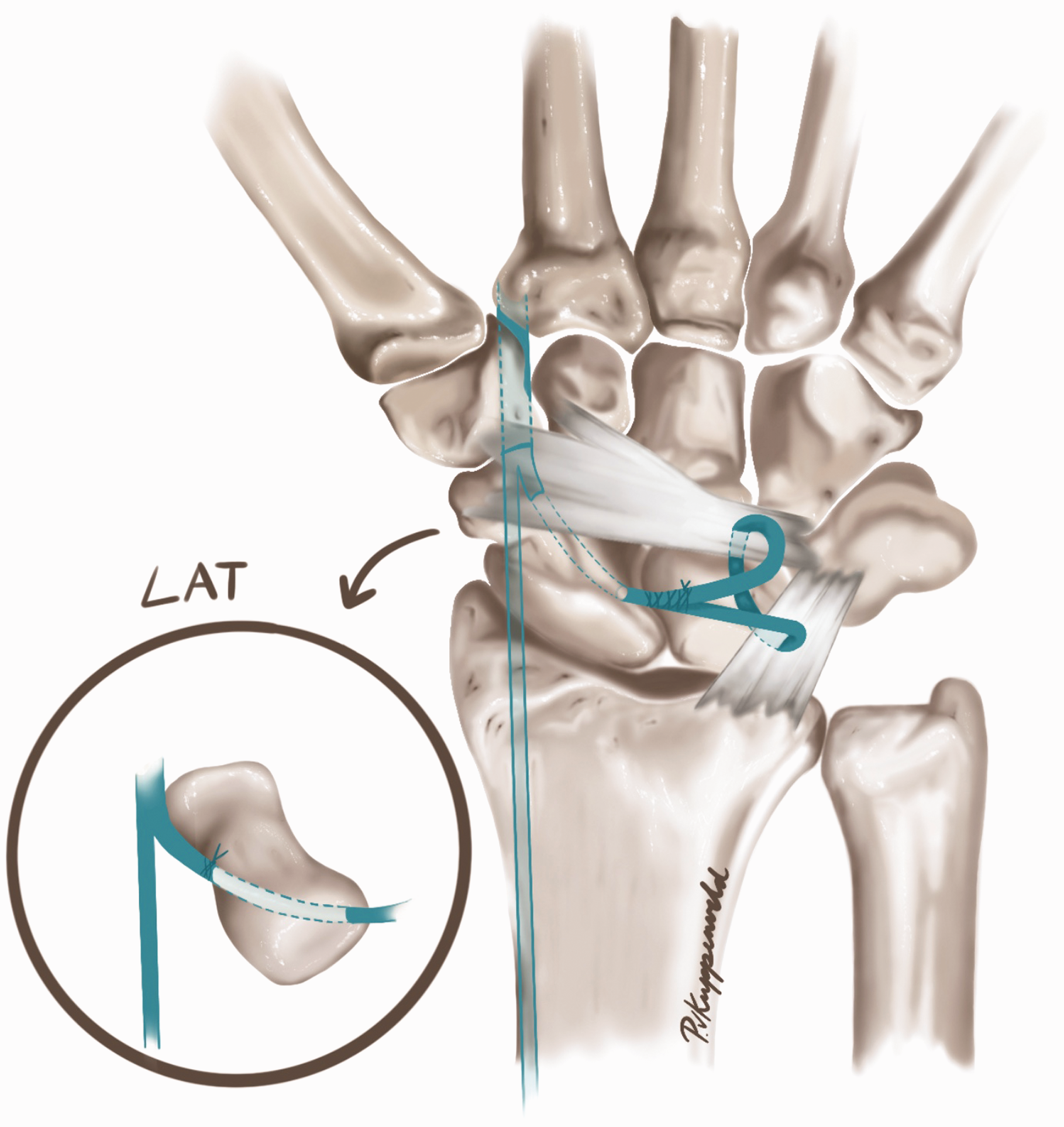
Twenty-one patients (24 wrists) were retrospectively identified and all completed the Patient-Rated Wrist and Hand Evaluation (MacDermid et al., 1998) and the Quick Disabilities of the Arm, Shoulder and Hand (Kennedy et al., 2011) and answered additional questions.
Characteristics and clinical outcomes of patients.
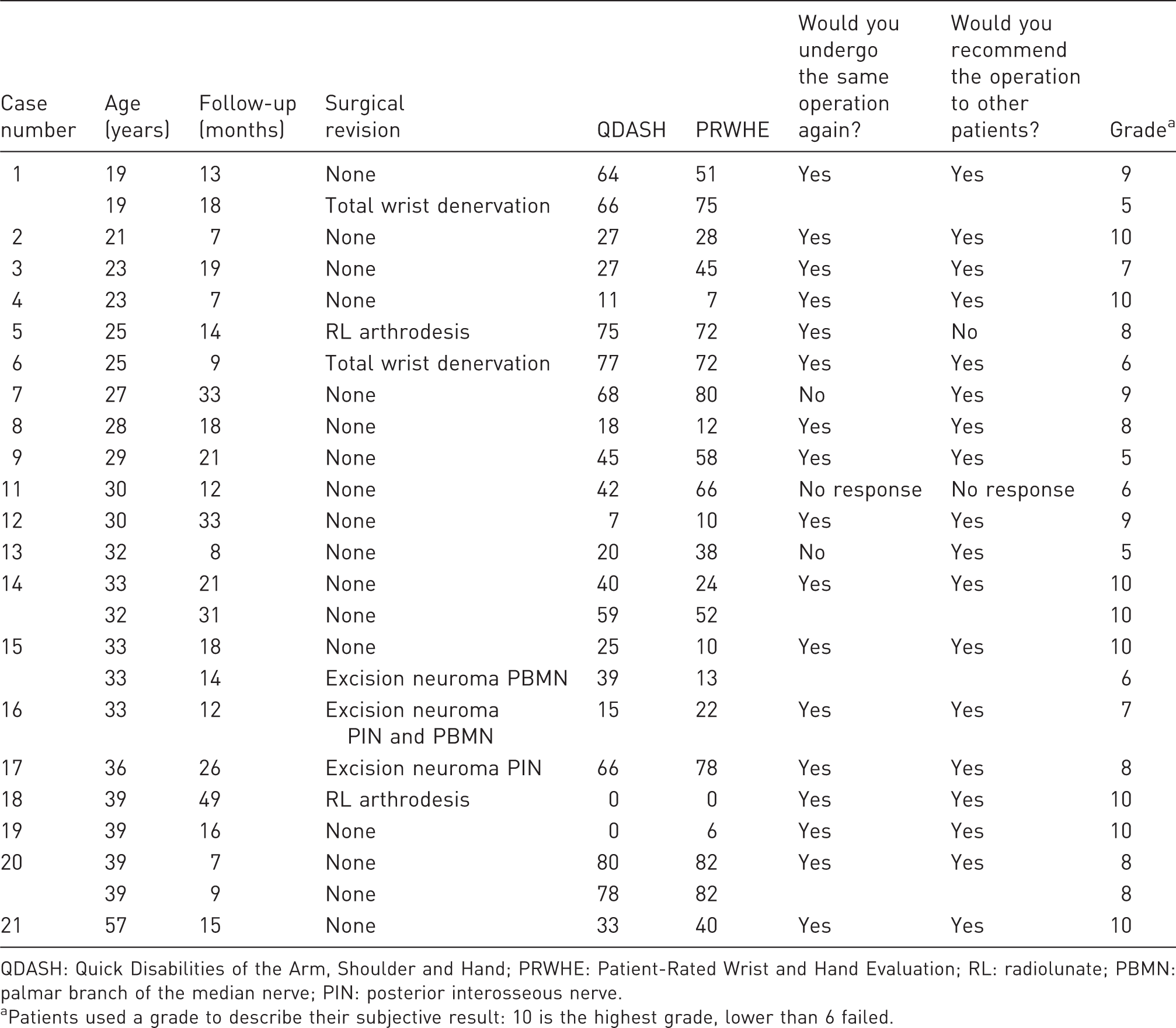
QDASH: Quick Disabilities of the Arm, Shoulder and Hand; PRWHE: Patient-Rated Wrist and Hand Evaluation; RL: radiolunate; PBMN: palmar branch of the median nerve; PIN: posterior interosseous nerve.
Patients used a grade to describe their subjective result: 10 is the highest grade, lower than 6 failed.
This report has limitations: no preoperative patient-rated outcomes measures are available, so it is impossible to prove improvement of wrist function, however, patient satisfaction, grip strength and return to work were high. Second, the follow-up was short; and third, there was no control group. Because most patients were satisfied with the operation, we will continue to use this technique.
Footnotes
Acknowledgements
We thank K. Cheriex for her assistance in the early stage of this study and P. Kuppenveld for creating the operative image.
Declaration of conflicting interests
The authors declare no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical approval
This study was approved by the Medical Ethical Committee at the Academic Medical Centre in Amsterdam, The Netherlands.
