Abstract
Obtaining patient feedback for personal reflection, development and GMC revalidation as an ICU consultant is complex. Various options for alternative evidence for revalidation have been suggested by FICM guidance. Communication with families at a time of crisis is core to the role of an ICU consultant and is something we should endeavour to seek feedback on to enable reflection and personal development, and which may also be useful evidence for GMC revalidation. In this article we propose a method for obtaining third party feedback on key communication events which we have demonstrated to be workable and useful.
Introduction
GMC guidance requires doctors to obtain patient feedback in each revalidation cycle. 1 FICM has issued guidance 2 for intensive care consultants especially those whose practice is soley intensive care, suggesting various alternatives: team feedback, unsolicited feedback, and broader colleague/teams/network feedback. These are important in triangulating performance, but rarely cite an individual and are not systematic to enable personal reflection on overall approach and communication skills.
Patient and family communication is a vital part of the role of senior ICU doctors and the skill with which this is done contributes to the well being of patients and their families. It can be especially important as the first stage in a bereavement process. 3 It is incumbent on ICU consultants to continue to reflect upon and obtain feedback on their communication skills to ensure they are maintaining and improving these skills throughout their careers. There is likely a cost implication in saved litigation when ICU consultants communicate well early during an unexpected deterioration.
This article presents a solution we have developed in our unit that has enhanced and formalised this feedback.
Methods
The issue of responding to the GMC requirements for patient feedback was discussed over several ICU consultant meetings. It was felt that asking relatives at times of crisis and high stress for their feedback on a consultant’s communication skills is inappropriate and overly burdensome. The majority of significant communication events occur in the presence of a member of the nursing staff. A review of available patient feedback questionnaires was conducted and adapted to be relevant for a third party to answer the questions. The form was reviewed by the consultant body and senior ICU nurses and further modified.
The team discussed making this mandatory and routine or opt in, and electronic versus paper. An opt in, voluntary, paper based system was developed.
The trust responsible officer and appraisal lead were consulted for approval to pilot (and then continue) this process as an appropriate surrogate for patient feedback.
The blank forms are available in the nurses’ offices on the unit, alongside a locked box for completed forms. The forms are collected monthly and analysed by one consultant who is an experienced trust appraiser and trained in counselling 360 feedback. The fully anonymised data is transcribed to a spreadsheet and individual consultants receive a report every 6 months for their reflection and appraisal, with the option for 1:1 meeting if required.
Results
The form developed is shown in Figure 1.
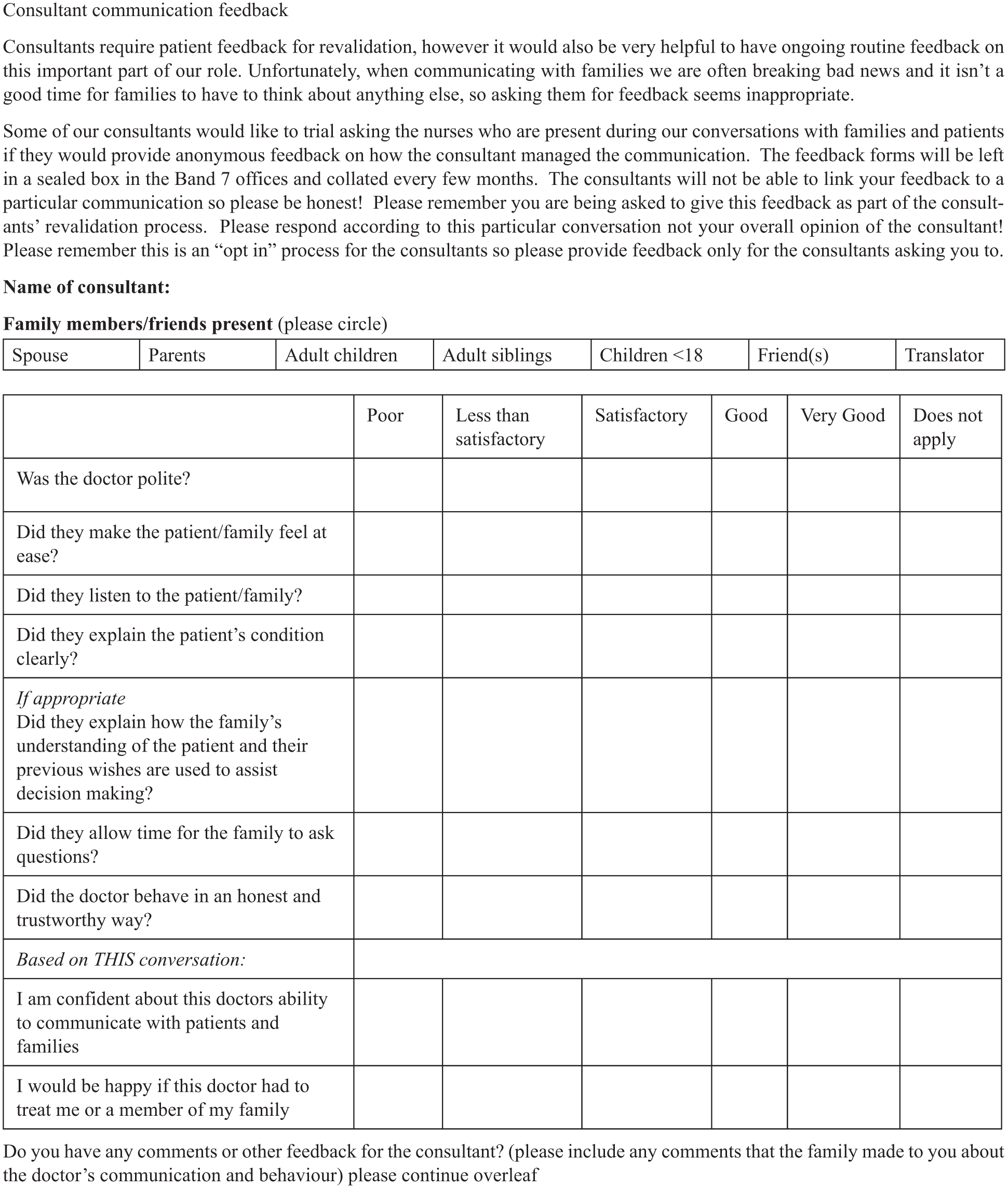
The form developed and used during the pilot period.
Fifteen senior ICU doctors (consultants and advanced trainees) have participated in the feedback scheme over 3 years. The number of nurses contributing feedback is unknown because the forms are fully anonymous. One hundred thirteen feedback forms have been submitted, mean 7.5 per doctor, range 1–29.
Some ICU consultants have opted out, where they have significant areas of practice outside of ICU, and obtain patient feedback relevant to their practice using the trust multi-source feedback.
Participation is by asking the nurse accompanying the doctor for the communication event to complete the form and return it to the letterbox. Sometimes they complete the form with the family if appropriate.
Whilst the vast majority of feedback is very positive there have been some developmental opportunities and the free comments have been useful, we postulate that the nursing respondents would not have been candid without the full anonymity offered by our method.
Feedback from individual consultants has been extremely positive, for example “thank you [this has] supported my personal professional development in a productive way.”
Informal feedback from nursing staff has indicated that they feel their contribution is valuable and important and the process is not burdensome.
Discussion
Communication with patients’ families at times of crisis is complex and a key part of the role of ICU consultants. Most of these events occur in the presence of an ICU nurse who is often an expert third party. Asking nurses for anonymous feedback we aim to capture their objective view on the communication at times where it would be overly burdensome to ask a family.
Whilst this is not patient feedback, it is feedback on a vital area of practice that is, in effect, our face to face interaction with those accessing our service, and aligns to the GMC principle of obtaining feedback from patients to reflect on and improve practice.
It enables colleagues to discuss communication skills with their appraisers with individual feedback, paralleling the expectation of appraisers from outside of ICU to see patient feedback results as part of the MSF. This provides a more granular opportunity to reflect than departmental or team feedback.
Footnotes
Acknowledgements
ICU nursing staff, University Hospitals Plymouth; Consultants and advanced trainees, University Hospitals Plymouth.
Funding
The author received no financial support for the research, authorship, and/or publication of this article.
Declaration of conflicting interests
The author declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
