Abstract
Background:
Critical care nurses experiencing high levels of emotional exhaustion (EE). However, limited studies explored the association between generational differences and nurses’ perceived EE. The objectives of the current study were to: (1) assess generational differences in EE among critical care nurses and (2) examine the link between nurses’ EE and the generational differences, occupational stress, structural empowerment, and nurses’ perceived work environment.
Methods:
A proportional stratified clustered sampling technique was utilized. The hospitals were stratified according to their location. Data were collected from nurses working at 19 hospitals in Oman. The emotional exhaustion sub-scale of the Maslach Burnout Inventory was used to assess the level of EE among nurses working in critical care units.
Results:
A total of 714 staff nurses participated. The majority (78%) were from generation Y and 22% were from generation X. Regression analysis showed that generation Y critical care nurses experienced higher EE levels than generation X nurses. Increased psychological stress among nurses was associated with increased EE. Higher levels of access to support, resources, and information, as well as supportive managerial leadership and sufficient staffing and resources, were associated with significant reductions in EE.
Conclusion:
To reduce job burnout among critical care nurses, healthcare leaders are required to ensure adequate staffing, provide managerial support, and monitor stress and EE levels frequently, particularly among generation Y nurses.
Introduction
Each generation possesses a distinctive blend of experiences, skills, perspectives, and expectations. 1 The belief is that similarities in terms of work values, attitudes, preferences, expectations, perceptions, and behaviors among individuals within a generation stem from shared historical, economic, and social experiences. 2 With a thorough understanding of these generational differences, organizations – including healthcare sector – can gain a stronger competitive advantage by harnessing and exchanging their unique experiences and expertise.
There are three main generations namely Baby Boomers (born between 1946 and 1964), Generation X (born between 1965 and 1980), and Generation Y (also known as Millennials and born between 1981 and 1996). 3 Baby boomers generally expect recognition for their efforts and contributions to the organization, value learning and training opportunities, encourage rapport building and teamwork, and tolerate management instruction.
Generation X stands out as one of the most highly educated generations in history, characterized by technological and media proficiency, as well as a sense of skepticism and pragmatism. 4 Nurses from Generation X are independent, self-directed, compliant with rules and regulations, and appreciate working environments that provide them with opportunities to develop their talents, creativity, and expertise. 5 Generation Y cohorts exhibit diverse experiences, values, attitudes, and preferences, all of which significantly impact their wellbeing, sensitivity to stress, and control of emotions.6,7 Generation Y nurses expect a high level of personal attention from their managers and leaders. 6
Occupational stress, structural empowerment, and perceived work environment
Nurses’ health and well-being can be negatively affected by factors like complex nursing practices, heavy workloads, time pressure, and challenging workplace conditions. These elements often lead to internal frustration and occupational stress resulting in EE.8 –10 Studies suggest a link between nurses’ EE and empowerment.11,12 Kanter’s theory supports the idea that structured work environments empower nurses, granting them significant rights and autonomy, resulting in enthusiasm and confidence, which all contribute to a reduction in their perceived EE. 13 Moreover, the evidence found that working in a healthy environment with less stress is associated with a reduction in the perceived EE. 14
Research has shown that differences between work engagement, occupational stress, and work environment exist among generational cohorts.5,6 However, limited evidence explored the level of these modifiable work-related factors across different generations and explored their links to EE among nurses working particularly in critical care units. Nurses working in critical care units reported high levels of EE.11,15 In critical care nurses, the frequency of moral distress situations – perceived as futile or nonbeneficial to patients – is associated with the occurrence of EE, a primary component of burnout Perceived EE has been linked to poor quality of care and unsafe practices. 16 Therefore, the aim of the present study was twofold: (1) to assess the generational differences in the level of EE, WE, SE, and OS among critical care nurses, and (2) to examine the association between generational differences, WE, SE, OS, and nurses’ EE level.
Theoretical framework
This study was based on the Job Demand-Resources model (JD-R). 17 Based on the JD-R model, high levels of job resources are associated with a reduction in emotional exhaustion (EE), whereas high levels of job demands are associated with an increase in EE. Work environment (WE) and structural empowerment (SE) components were considered job resources in the current study, while occupational stress (OS) was considered a reflection of perceived job demands.
Methods
Research objectives
To assess the generational differences in the level of EE, WE, SE, and OS among critical care nurses
To examine the association between nurses’ EE level and their generational differences, WE, SE, and OS.
Setting
In this study, a cross-sectional design was used. A proportional stratified clustered sampling technique was used to collect the data. The hospitals were stratified according to their location. The nurses were recruited from 19 different hospitals located in 11 governorates throughout Oman.
Ethical approval
An ethical approval was obtained from the Ministry of Health before data collection (MoH/CSR/18/10004).
Participants
The targeted sample was staff nurses working in ICUs. The eligibility criteria for participation in this study were that all participants must be registered nurses, currently assigned in ICUs, and hold a University Diploma or postgraduate degree. Nurses with less than 1 year of experience in their current unit were excluded from the survey as they might lack sufficient experience to form an informed opinion about the nurse practice environment, perceived empowerment, and perceived stress. Based on standard questions for estimating the sample size, an online calculator was used to estimate the required sample size. 18 With a statistical power of 80%, low effect size of 0.15, and 0.05 significance level, the calculation revealed that a sample of 874 nurses is required. After approaching the potential participants, a total of 714 staff nurses participated in the study, resulting in an 81.7% response rate.
Data collection
The data was collected over 5 months between November 2019 and April 2020. A written informed consent was obtained from participants, with no identifying information being collected. Participants were assured that their responses would be kept confidential. Participants were informed that they have the right to withdraw from the study at any time. Data was collected during their breaktime so as not to interrupt their work.
Five standardized instruments were used. The first instrument was a sociodemographic and work characteristics sheet that included information regarding participants’ age, gender, education, marital status, work status (full-time or part-time), and years of experience.
The Practice Environment Scale of the Nursing Work Index (PES-NWI) was used to assess nurses’ perceptions of their work environment. 19 It consists of 31 items rated on a Likert scale of 1–4, with 1 representing strongly disagreeing and 4 representing strongly agreeing. Higher composite scores indicate a more favorable practice environment. The scale assesses five features of practice, including nurse manager leadership and support, nursing foundation for quality, staffing and resources adequate, nurse-physician relationship, and nurse involvement in hospital affairs. Scores equal to or below 2.5 indicate discordance, while scores above 2.5 indicate the item is present in practice. It has been used and validated in a variety of countries and cultures, including Oman. 20 The Cronbach’s alpha was 0.84. 21 In this study, Cronbach’s alpha was 0.94.
Conditions of Work Effectiveness Questionnaire-II (CWQ-II) was used to assess structural empowerment. 22 This scale consists of 12 items that are rated on a Likert scale of 1–5, with 1 referring to “none” and 5 referring to “a lot.” The scale quantifies four features of empowerment: access to resources, information, support, and opportunity. The total scores were calculated by summing the four subscales. Higher scores indicate higher structural empowerment. In addition, the perceived empowerment of nurses was divided into three categories: low (scores between 4 and 9), moderate (scores between 10 and 14), and high (scores between 15 and 20). The instrument has been found to be valid and reliable with a Cronbach’s alpha of 0.82. 22 The Cronbach’s alpha in this study was 0.91.
The short version of the Perceived Stress Scale (PSS) 23 was used to measure OS among nurses. The scale consists of 4 items. The respondents were asked to indicate their agreement with each item on a 5-point Likert scale, with 0 referring to never and 4 referring to very often. The scale demonstrated good validity and reliability with Cronbach’s alpha = 0.79. 23 In the current study, the Cronbach’s alpha was 0.75.
The EE sub-scale of the Maslach Burnout Inventory 24 was used to assess the level of EE. Emotional exhaustion is a 9-item, 7-point Likert scale, wherein 0 referring to “never” and 6 referring to “every day.” Higher scores indicate higher levels of emotional exhaustion. The mean composite score is classified into three levels: low for scores less than 18; moderate for scores between 19 and 26; and high for scores of 27 or above. 24 The scale’s validity and reliability have been well-established; the Cronbach’s alpha was 0.85. 8 In the current study, Cronbach’s alpha was 0.80.
Data analysis
IBM SPSS Statistics software [version 23] was used to analyze the data. Descriptive statistics including means, standard deviations, frequencies, and percentages were utilized to describe nurses sociodemographic. Independent sample t-test and Pearson correlation were used to describe the relationship between different study variables. Multivariate regression analysis was conducted to examine the relationship between EE, WE, SE, and OS controlling for sample demographics and work characteristics.
Results
Sample demographics
The sample was predominately female (84.6%), expatriate (62.4%), full-time nurses (93.4%), with an average age of 35.34 (SD = 6.319), and an average work experience of 12.13 years (SD = 6.352) in nursing. The majority (78%) of the sample (n = 557) were from generation Y and 22% were from generation X. Table 1 presents the sample characteristics across the two generations.
Sample Characteristics (N = 714).
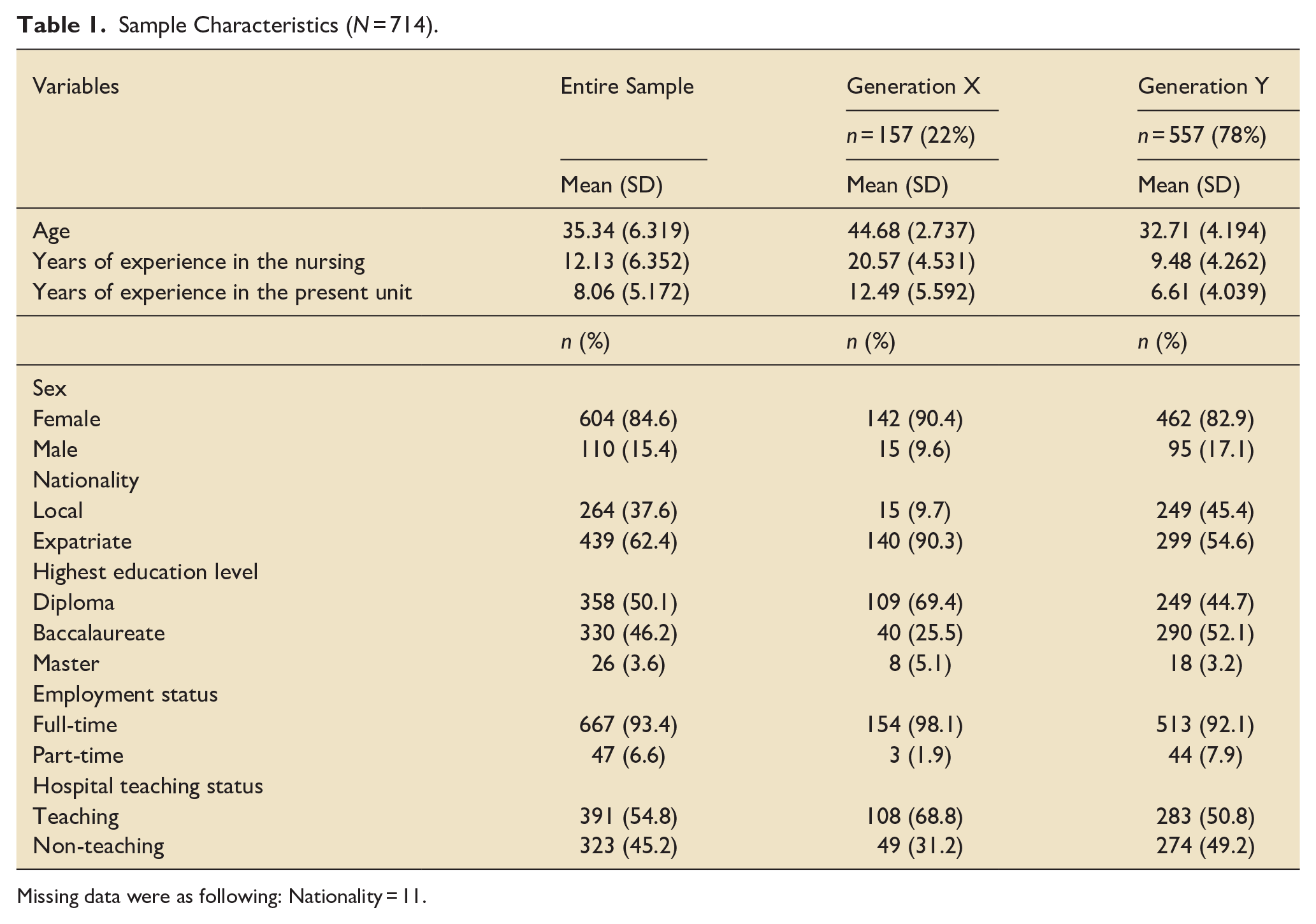
Missing data were as following: Nationality = 11.
Description of emotional exhaustion, practice environment, empowerment, and occupational stress
Table 2 presents a descriptive summary of EE, practice environment, structural empowerment, and psychological stress across X and Y generations. The mean score of EE was 22.23 (SD = 10.88) indicating a moderate level of job burnout. Out of the 714 participants, 13.3% reported having a low level of EE, 64.4% reported having a moderate level, and 22.3% reported having a high level. Generation Y nurses reported significantly higher levels of EE compared with generation X (t = −3.896, p < 0.001).
Descriptive summary of emotional exhaustion, work environment, structural empowerment, and psychological stress.
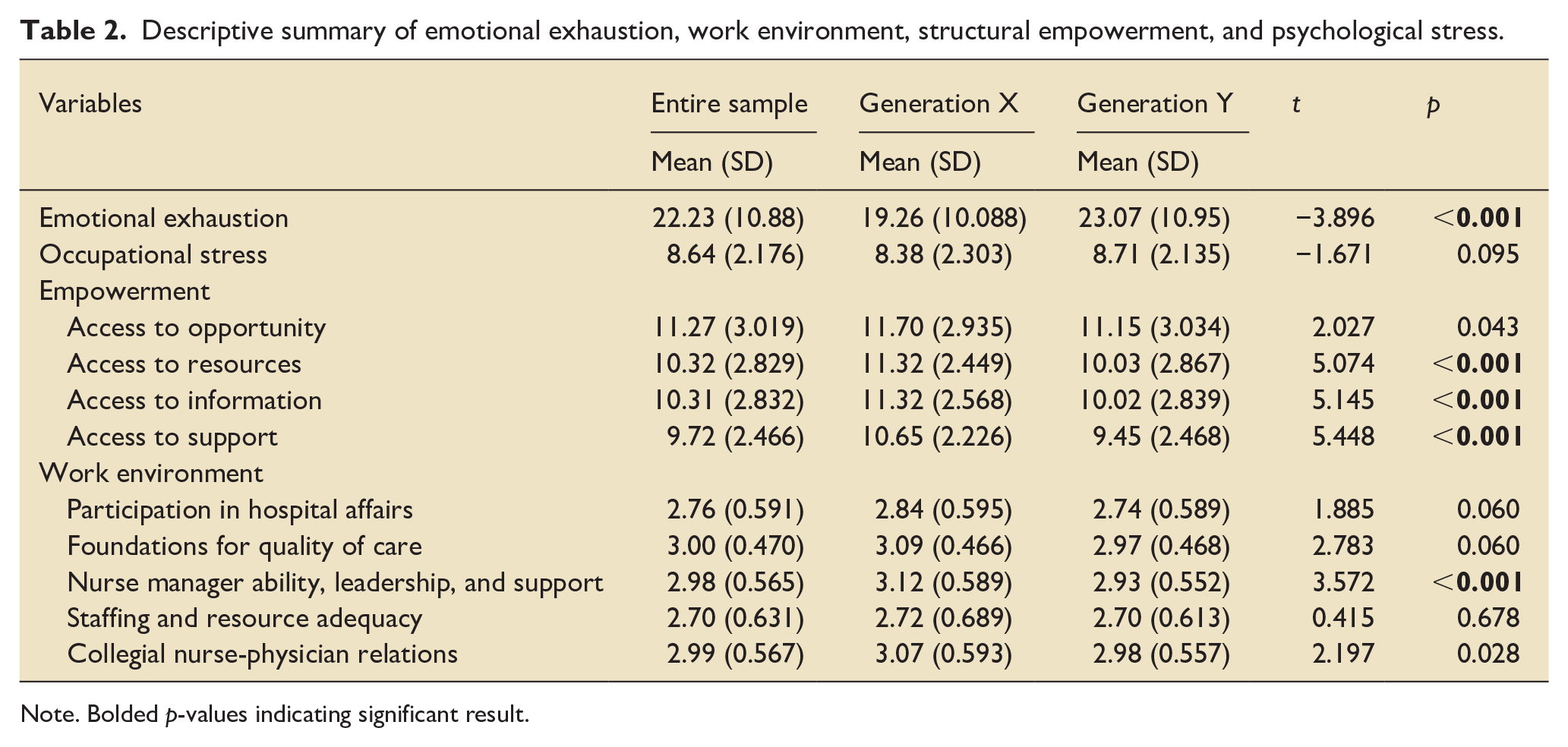
Note. Bolded p-values indicating significant result.
Nurses rated access to opportunity as the most empowering dimension and access to support as the least. Generation X reported better perception of access to opportunity (t = 2.027, p = 0.043), access to resources (t = 5.074, p < 0.001), access to information (t = 5.145, p < 0.001), and access to support (t = 5.448, p < 0.001) compared to generation Y nurses.
Nurses perceived their practice environment as “favorable” as all subscales were above the midpoint of 2.5. Generation X nurses rated the “nurse manager ability leadership and support” as the most favorable feature of their practice environment followed by the “foundations for quality of care,” while Generation Y nurses rated the “collegial relationship with physicians” as the highest. “Staffing and resources adequacy” was rated as the least favorable dimension of practice environment by nurses in both groups, Generation X and Y.
Emotional exhaustion was positively correlated with psychological stress (r = 0.093, p < 0.001) and negatively correlated with structural empowerment (r = −0.226, p < 0.001) and perceived work environment (r = −0.232, p < 0.001), see Table 3.
Correlations between main study variables.
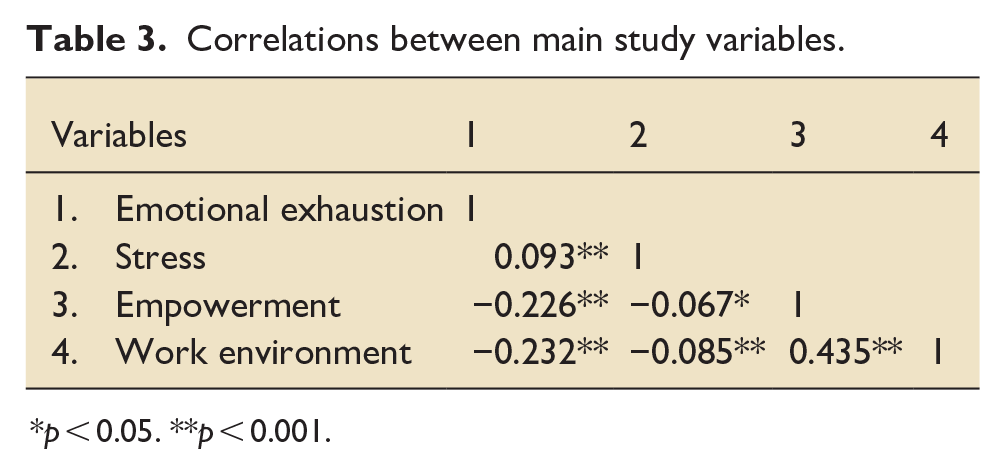
p < 0.05. **p < 0.001.
Factors influencing emotional exhaustion
Findings from the multivariate regression model showed that generations, psychological stress, empowerment, and work environment were significant predictors of emotional exhaustion controlling for other covariates (R2 = 0.170, F(18, 820) = 13.674, p < 0.001), see Table 4. Generation Y experienced higher levels of EE compared to their counterpart nurses from generation X. Each additional point in the psychological stress nurses experiencing was associated with a 0.62 increase in their EE. Among the structural empowerment such-scales, higher levels of access to support, access to resources, and access to information were associated with a significant reduction in perceived emotional exhaustion. Among the work environment characteristics, having manger leadership and support and sufficient staffing and resources were associated with a significant reduction in perceived emotional exhaustion. The regression model explained 17% of the variances in the perceived emotional exhaustion. No evidence of multicollinearity was observed (IVF = 2.836) and regression residuals were normally distributed.
Multiple regression of the influence of generational differences, occupational stress, structural empowerment, and perceived work environment on nurses’ emotional exhaustion.
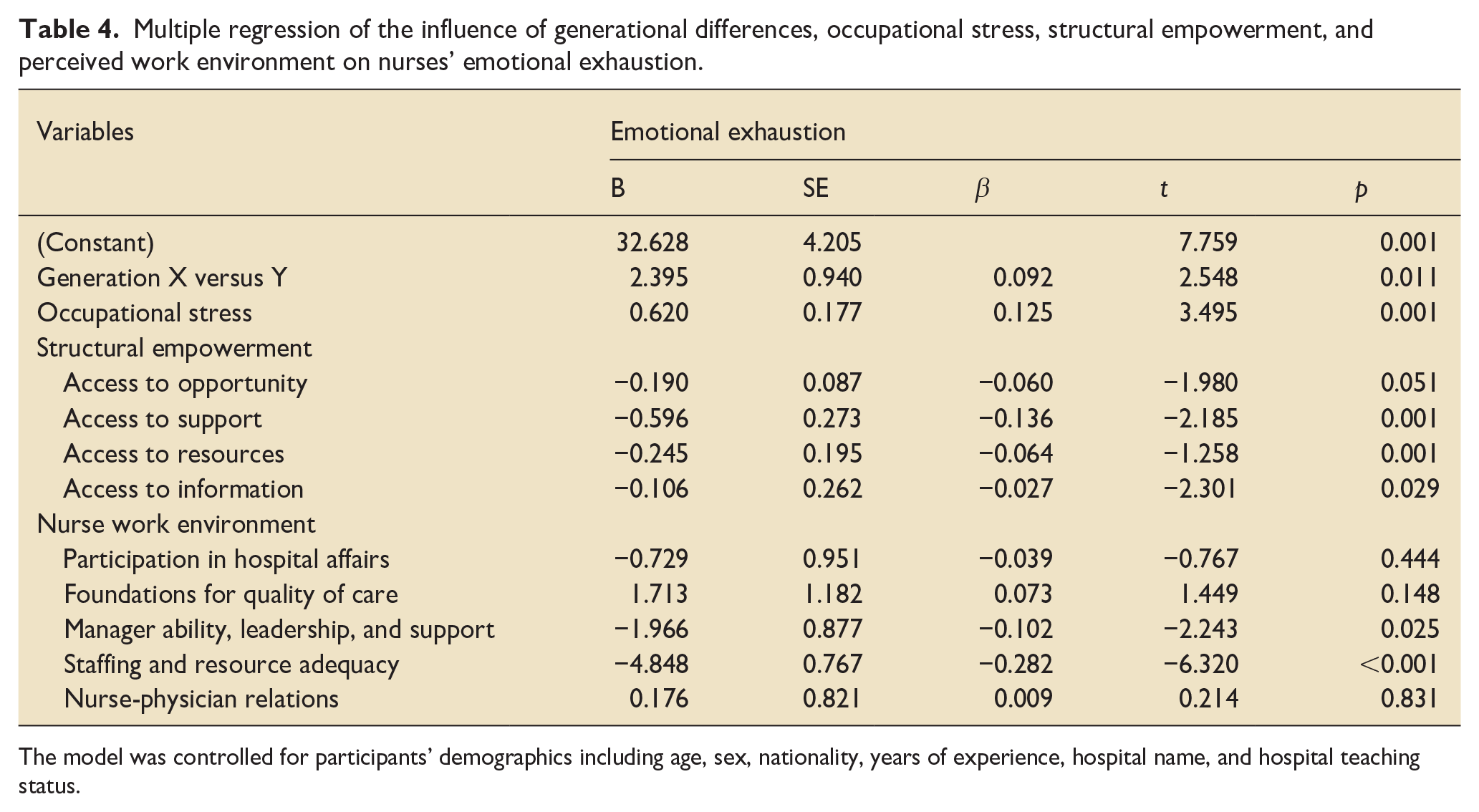
The model was controlled for participants’ demographics including age, sex, nationality, years of experience, hospital name, and hospital teaching status.
Discussion
This study examined the association between nurses EE, the generational differences, occupational stress (OS), structural empowerment (SE), and perceived work environment (WE).
Critical care units are vital in providing high acuity nursing care to patients. These settings have long been considered as challenging and stressful areas for healthcare workers including nurses. 25 It is not surprising that the sampled critical care nurses in this study reported a moderate EE level. More specifically, Generation Y nurses reported significantly higher levels of EE when compared to Generation X. This finding is particularly novel and requires attention, as Generation Y represents the majority of the nursing workforce today. This result is in support of previous research,26,27 indicating that Generation Y nurses experience higher stress and burnout levels in the clinical area than other cohorts of nurses. The moderate burnout levels in Gen Y nurses could be attributed to an inadequacy of positive coping skills in this generation of nurses, adversely affecting their capacity to adapt effectively to their work environment. 28 In addition, Gen Y nurses when compared to earlier cohorts of nurses have lower psychological resilience, which is essential when dealing with stressful events. 29
Given the higher levels of EE in Generation Y nurses, it is essential for nursing policy, management, and practice to address these generational differences through targeted interventions. Nursing policy should focus on creating a supportive work environment that encourages the development of positive coping skills, resilience, and well-being, particularly for younger nurses. 30 Policies promoting mental health support, such as access to counseling and stress management resources, should be prioritized to address these challenges. 31 Additionally, nursing management should consider tailored approaches to staffing, workload distribution, and leadership training to ensure Generation Y nurses receive the necessary support to manage stress effectively. 32 This may involve mentoring programs, debriefing sessions, and fostering an environment where open discussions about emotional well-being are encouraged. 35 In Oman, where Generation Y nurses represent the largest segment of the nursing workforce,33,34 it is crucial to prioritize these interventions to ensure their well-being and support their ability to cope with the challenges of critical care nursing.
Nursing practice should also evolve to incorporate strategies aimed at boosting resilience and coping mechanisms among Generation Y nurses. This could include incorporating mindfulness practices, time management skills, and self-care strategies into orientation and ongoing training programs. 35 Creating a culture that values work-life balance, flexible scheduling, peer support, leader or manager support can also significantly reduce burnout levels and enhance job satisfaction. 36 Moreover, regular assessments of the psychological well-being of Generation Y nurses should be integrated into nursing practice to ensure early intervention and continuous support. 30 By focusing on these implications, healthcare organizations can mitigate the adverse effects of EE, thereby improving retention, job satisfaction, and overall patient care outcomes among Generation Y nurses.
Critical care nurses in this study rated access to opportunity as the most empowering dimension and access to support as the least. Among these nurses, Generation X reported a better perception of access to opportunity, access to resources, access to information, and access to support compared to Generation Y nurses. Similar results, where Generation X had a better perception of structural empowerment, were found in the study by Cayaban et al. 37 Additionally, nurses from both cohorts perceived their practice environment favorably, with all subscales scoring above the midpoint of 2.5. In Generation X, nurse managers’ leadership and support were rated as the most favorable feature, followed by foundations for quality of care. Managers need to understand what nurses from different generations consider to be desirable managerial support in order to fulfill their expectations. For example, for generation X, scholars found that employees seek instant gratification and feedback for their work and contributions which directly affect their performance. 38 Therefore, nurse leaders are recommended to create a motivational environment that makes nurses feel supported and that their accomplishments were valued and acknowledged.
Generation Y nurses, on the other hand, rated their collegial relationship with physicians as the highest, which supports the notion that Generation Y nurses value group cohesion. 7 Similar findings were reported by Wieck et al. 39 who explored the perceived work environment among 1773 nurses working at different 22 hospitals in the USA. Findings showed that generation Y nurses perceived their relationship with physicians as the most satisfying aspect of the work environment. Hence, promoting respectful and positive teamwork among healthcare providers is necessary to build a healthy work environment for employees from different generations.
Findings from the multilevel regression analysis indicate that generations, OS, SE, and WE significantly predict EE, controlling for other covariates. First, occupational stress significantly predicted emotional exhaustion, suggesting that when critical care nurses experience higher stress levels, this may lead to higher levels of burnout. The demanding nature of nursing roles, coupled with the unique stressors inherent in patient care, creates a perfect storm for emotional exhaustion and burnout. Critical care nurses face high job demands characterized by long shifts, heavy workloads, and the need to multitask under time constraints. These demands not only strain physical endurance but also deplete emotional resources over time. Mounting evidence has shown that persistent exposure to stressful situations could gradually erodes nurses’ resilience and coping mechanisms, resulting in burnout—a state characterized by emotional exhaustion, depersonalization, and reduced personal accomplishment. This result highlights the importance of addressing stress in nursing to prevent burnout and sustain the well-being of critical care nurses who play a critical role in patient care.
Regression analysis identified structural elements including access to support, access to resources, and access to information to have a significant effect on critical care nurses’ emotional exhaustion. This result indicates that when critical care nurses feel adequately supported and equipped with resources and information, they are better able to cope with job stressors, reducing the risk of emotional exhaustion. Access to support systems within the workplace, including colleagues, supervisors, and organizational support structures, were seen to play a critical role in mitigating emotional exhaustion, 40 while access to adequate resources such as staffing adequacy, training opportunities, and organizational policies were seen to enhance nurses’ coping resources. 41 Access to information, including clear communication channels, feedback mechanisms, and decision-making transparency, fosters a sense of control and autonomy among nurses. This empowerment can mitigate feelings of helplessness and frustration often associated with high job demands, ultimately reducing emotional exhaustion. Hospital administrators should invest in these structural elements, to create a supportive work environment that enables critical care nurses to thrive professionally and emotionally, ultimately benefiting both staff and patient outcomes.
Previous studies strongly tied a favorable work condition to a variety of job outcomes and safety outcomes for patients.11,21 In this study, work environment features including adequate nurse manager leadership and support and sufficient staffing and resources were seen to significantly reduce emotional exhaustion in critical care nurses. This finding yielded support to previous research 8 which identified various organizational factors playing a critical role in nurses’ overall well-being. When provided with strong leadership and support, a supportive work environment is created and nurses feel valued and empowered, resulting to lower levels of EE. 42 In addition, adequate staffing and resources ensure that nurses can effectively carry out their work and provide quality patient care, resulting in reduced stress and burnout. These findings highlight the importance of organizational support and resources in promoting critical care nurses’ mental health and job satisfaction.
Overall, the study findings closely align with the Job Demand-Resources (JD-R) model, which highlights the pivotal role of job resources and demands in shaping critical care nurses’ well-being. Within this model’s framework, access to support, resources, and information is regarded as crucial job resources that assist individuals in managing job demands and alleviating emotional exhaustion. Higher levels of these resources provide critical care nurses with the necessary tools to effectively navigate their roles effectively, thereby reducing EE. Similarly, the presence of supportive nursing leadership, along with adequate nurse staffing and resources, contributes to creating a desirable work environment conducive to nurses’ well-being. This aligns with the JD-R model’s proposition that such elements could help buffer the adverse effects of job demands, ultimately resulting in lower level of EE among critical care nurses.
Limitation
Because the study utilized a cross-sectional design, establishing causal relationship between study variables was not possible. In addition, generalizability of study findings can be limited to nurses working in acute care hospitals.
Conclusion
Overall, critical care nurses experience higher levels of emotional exhaustion. Generation Y nurses exhibited higher levels of EE when compared to their counterparts in Generation X. Work environment characteristics, specifically having managerial leadership and support, as well as adequate staffing and resources, were associated with a significant reduction in perceived EE. Given these results, hospital administrators and clinical nurses can prioritize initiatives to establish supportive WEs, addressing workplace challenges. It is crucial for nurse managers to play a pivotal role in evaluating and formulating strategies aimed at addressing these modifiable factors with the goal of mitigating EE. The implementation of strategies that foster supportive work environments can contribute to overall well-being in critical care units.
Footnotes
Acknowledgements
The authors would like to acknowledge Sultan Qaboos University and The Research Council for their support and thank all nurses who contributed to this study.
Author contributions
(SA, OA, IB) designed the study. (SA) collected the data. (SA) analyzed the data. (SA, AC, LL, RA) prepared the manuscript. (SA, AC, OR, RA, LL, IB) provide critical revisions for important intellectual content. All authors approved the final version for submission.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by Sultan Qaboos University (RF/CON/FACN/19/01) and The Research Council, Sultanate of Oman (RC/RG-CON/FACN/18/01).
