Abstract
The Intensive Care Society and Faculty of Intensive Care Medicine are pleased to launch revised procedural checklists, Local Safety Standards for Invasive Procedures (LocSIPPs) that we hope will improve the safety of our intensive care units. First produced in 2017, the updates take into account learning from reported patient safety incidents, some of which have been associated with considerable morbidity and mortality. The publication of NatSIPPs 2 has been acknowledged during the update. We have focused on procedures which are commonly performed in Critical Care Units (intubation, bronchoscopy, intercostal drain insertion, tracheostomy insertion, central venous catheter insertion). The checklists have been designed to enable departments to use and adapt to make them unit specific. They will require relevant educational and clinical governance procedures to accompany them, to fit into local working practices.
NHS England published the original National Safety Standards for Invasive Procedures (NatSSIPs) in 2015, 1 to aid NHS organisations to provide safer care and help reduce the number of patient safety incidents related to invasive procedures. From this, in 2017, The Intensive Care Society and The Faculty of Intensive Care Medicine collaborated to create Local Safety Standards for Invasive Procedures (LocSSIPs), for those procedures commonly performed on critical care units, to reduce the associated morbidity and mortality. The aim was to aid each institution to create their own hospital specific checklists. These checklists should be used in real time when performing the procedures.

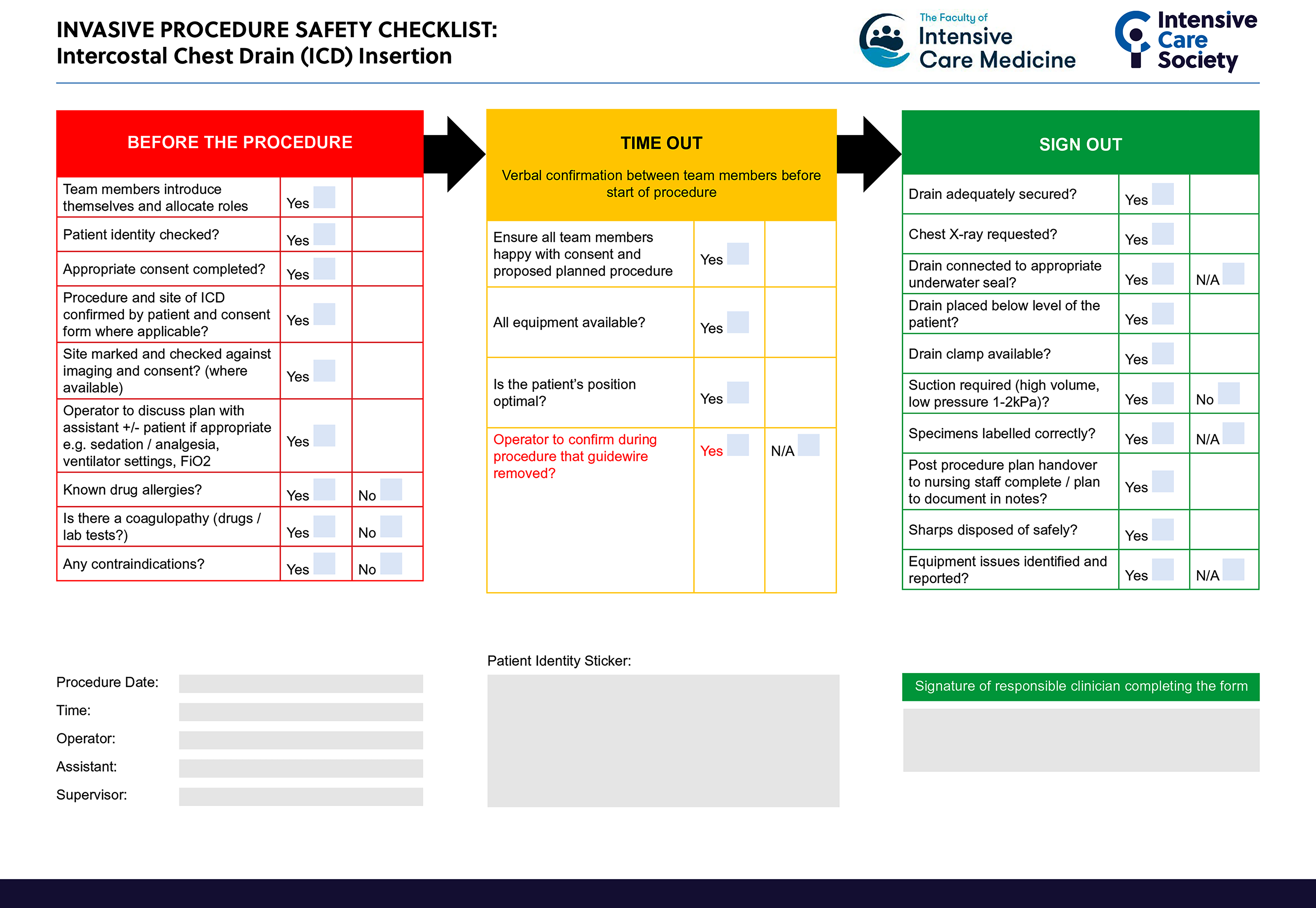

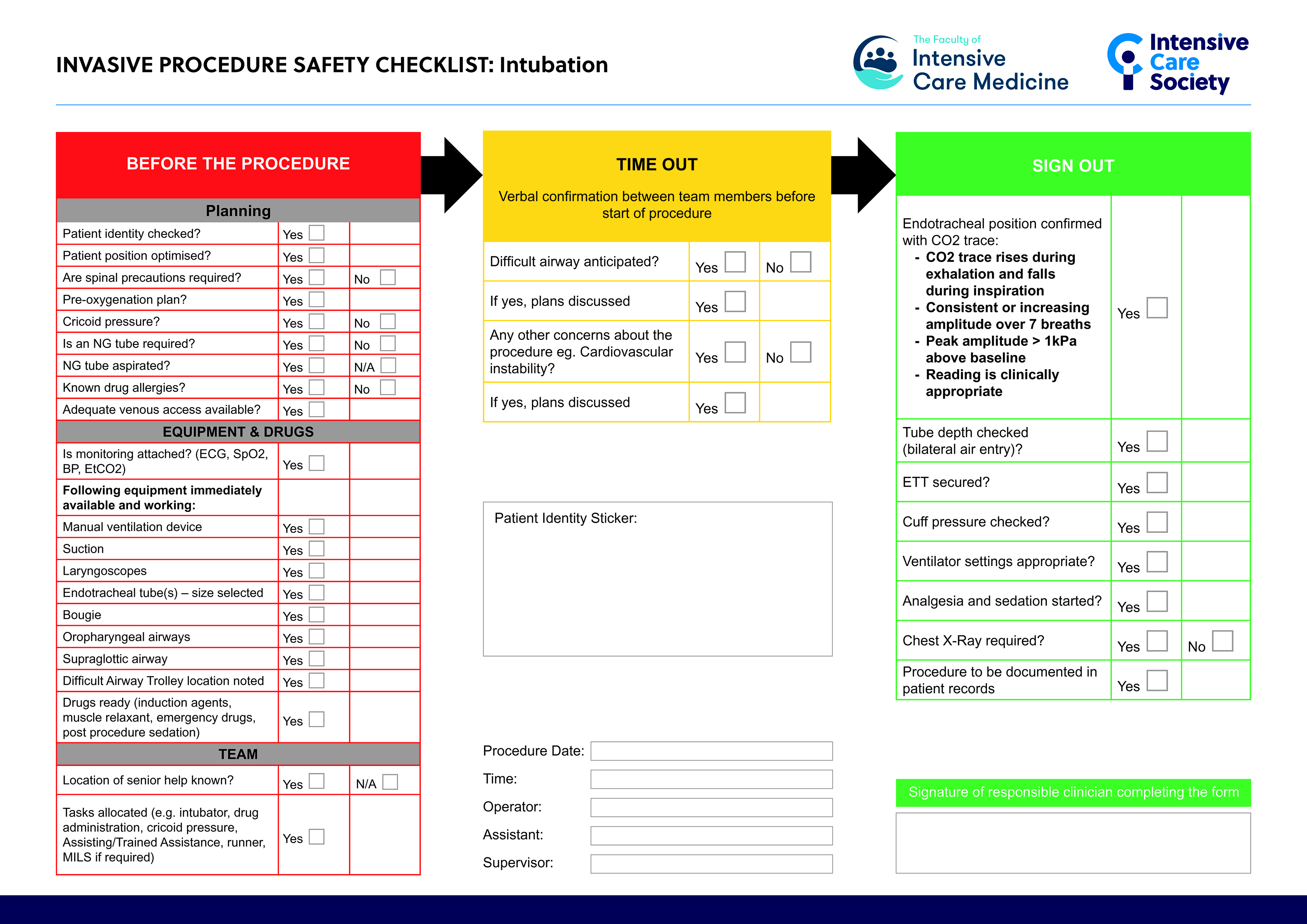
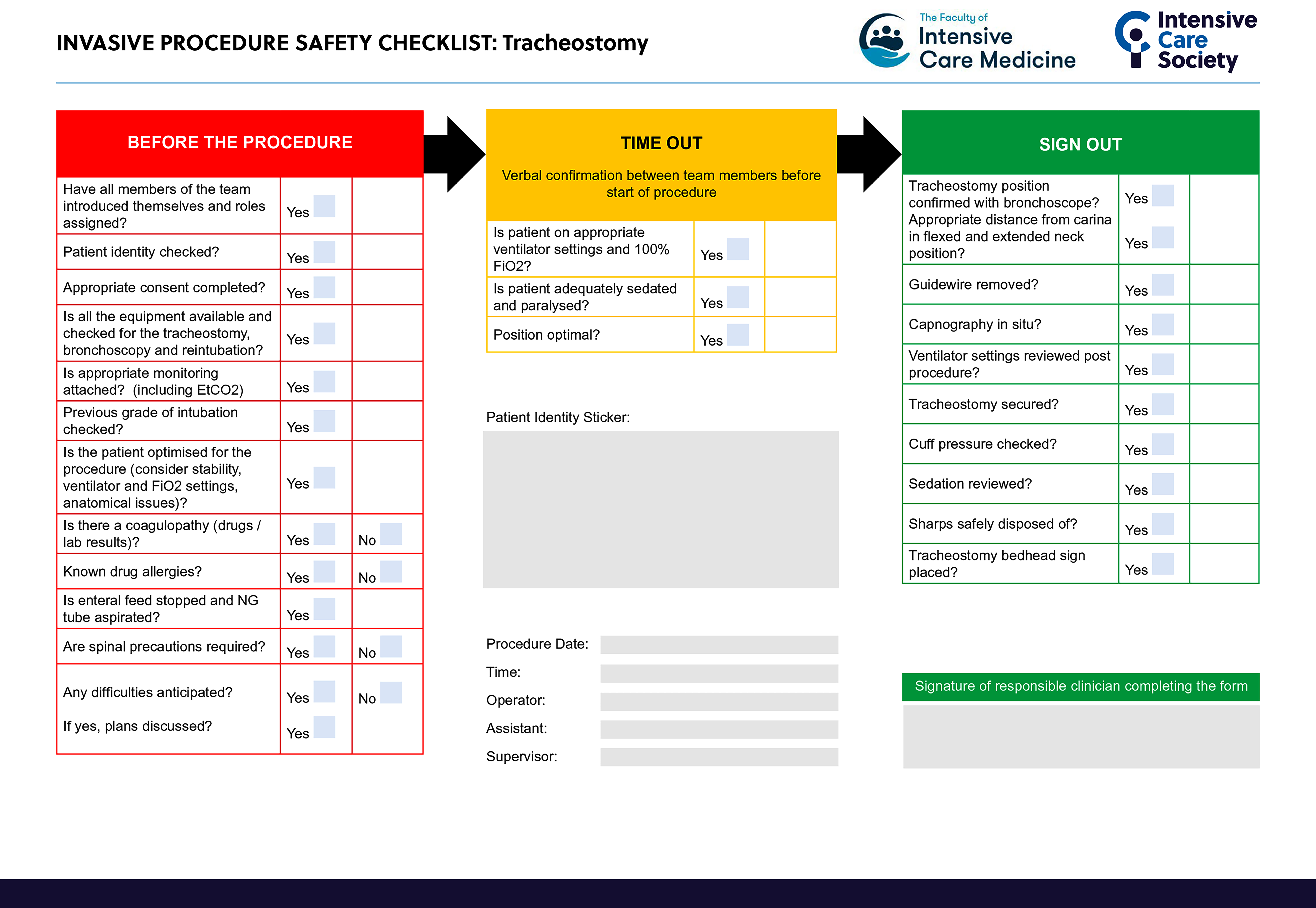
The publication of NatSSIPs 2 in 2023 has helped in the process of revising the original LocSSIPs. 2 They intend to utilise previous learning and current best practice to support organisations to deliver safer care.
It has been evident from reported safety incidents that the original LocSSIPs were needed, and that they required revision to encompass evolving evidence.
The overall aim is to support clinicians in the provision of safer care during commonly performed invasive procedures within the critical care setting. Examples of reported incidents, that the LocSSIPs help prevent, include unrecognised arterial puncture during central venous catheter insertion, unrecognised oesophageal intubation and wrong side intercostal drain insertion. All these have the potential to lead to serious harm.
We have focused on those procedures which are commonly performed in Critical Care Units (intubation, bronchoscopy, intercostal drain insertion, tracheostomy insertion, central venous catheter insertion), to help in the safety of these. A decision has been made to remove the nasogastric tube insertion LocSSIP as the information pertaining to all safety aspects of this procedure are contained within National Patient Safety Alerts, 3 and the risk we feel is more related to confirmation of position than insertion. The central venous catheter insertion checklist has been updated to bring it in line with layout of the others, and to acknowledge that two location confirmation techniques are required.
Our aim is that they will be adopted at local level and ingrained in the safety culture of all Critical Care Units. We hope you find them to be user friendly, but they have been written to be modifiable locally. No checklist can be effective if it isn’t used!
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
*
The checklists are available as downloadable and editable PDFs from the Society’s https://ics.ac.uk/guidance/checklists.html and Faculty’s ![]() websites.
websites.
