Abstract

Difficult peripheral venous cannulation (PVC) is one of many factors that can lead to a delay in treatment for patients. 1 This is more important for some conditions, such as in the case of sepsis, where delays in antibiotics have been shown to increase morbidity and mortality. 2 In 2013, a systematic review and meta-analysis of ultrasound (US) guidance for difficult PVC concluded that US increases the likelihood of success. 3 Junior doctors can be trained to use US for PVC and are able to retain and apply this skill as part of their daily practice. 4
Foundation doctors attended two organised teaching sessions, each two hours in length and included: a short presentation introducing the theory; technique demonstration from anaesthetic trainees and supervised practice with US-guided access on simulated models. Homemade peripheral vein models were created using gelatine and plastic containers (Figure 1). Foundation doctors undertook anonymous surveys based on the Kirkpatrick evaluation model before and after each session. 5 These were used to evaluate the effectiveness of our teaching and included self-reported confidence scores (Likert scales 1–10). Unpaired T-tests analysed assessed mean score changes.
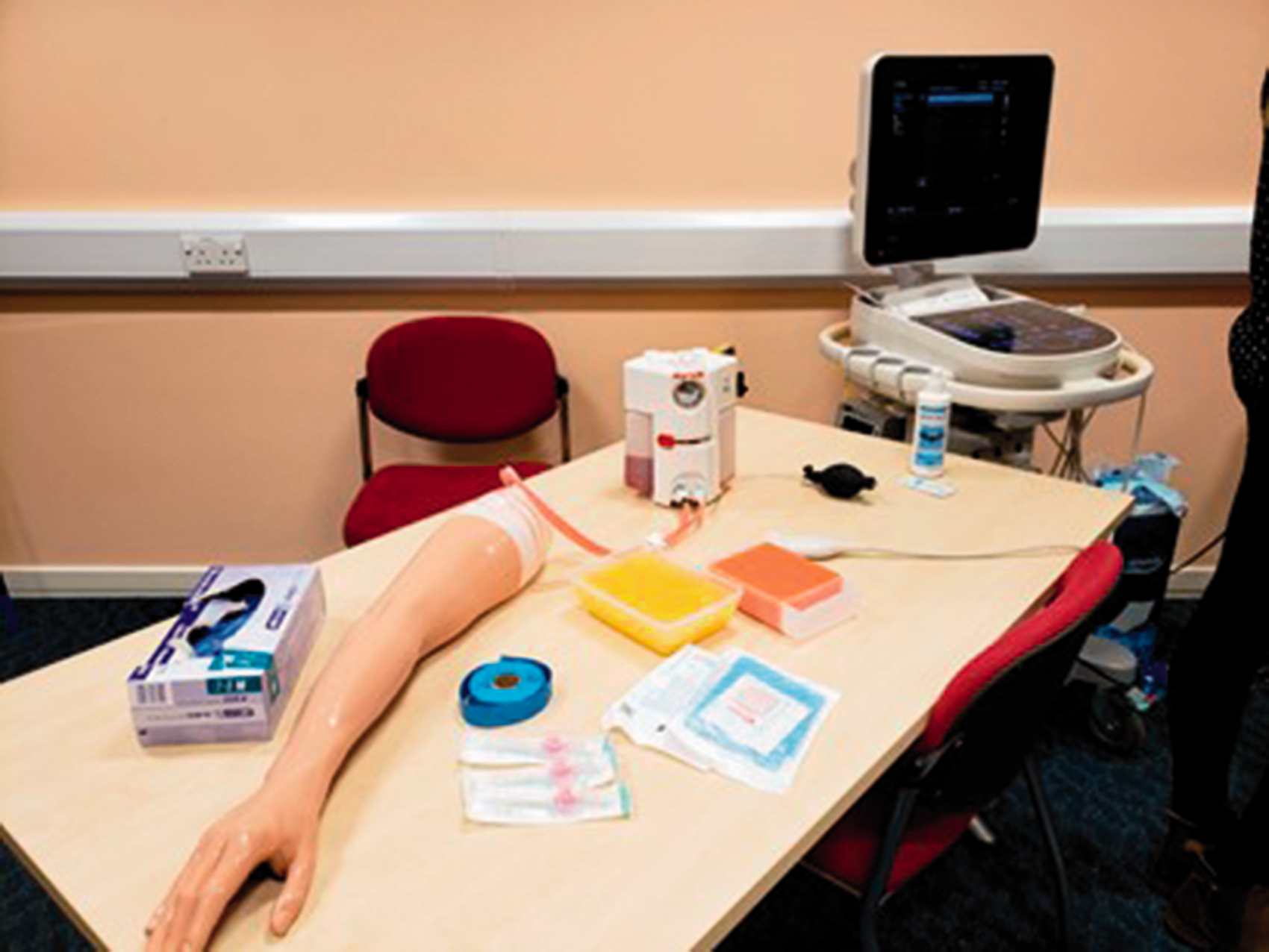
A selection of equipment used in teaching sessions.
In total, 20 foundation doctors attended. All found the session useful and rated the level and content of the teaching as just right. Prior to the teaching, foundation doctors reported they felt confident with performing PVC (Mean = 7.37, Likert 1–10) but were not confident with performing US-guided PVC (Mean = 2.47, Likert 1–10). A significant overall increase in mean scores was found post-teaching delivery (p < 0.0001), in confidence for performing both PVC (+1.53) and US-guided PVC (+4.53). High rates of foundation doctors (n = 19, 95%) reported contacting the on-call anaesthetist for PVC assistance, however, following the teaching, most (n = 15, 75%) stated they would now first attempt US-guided PVC.
Teaching sessions were limited by COVID-19 social distancing measures and the quality of our homemade peripheral vein models. Ongoing audit of anaesthetic referrals pre- and post-teaching delivery will help to further evaluate the effectiveness of teaching sessions. US-guided PVC is being integrated to form part the local foundation teaching programme at our NHS trust and will be made available to all foundation doctors.
In conclusion, despite the limited evidence base, US-guided PVC can be a useful skill for junior doctors to develop, especially in the management of the acutely unwell patient. Our near-peer teaching demonstrated an effective method for improving foundation doctors’ knowledge and confidence in performing PVC and US-guided PVC. We hope that in the future, expansion of US-guided PVC training may lead to a reduction in emergency PVC requests for anaesthetists and improvement in patient care.
Footnotes
Author contributions
All contributions have been completed by a single author as listed above, who agrees to be accountable for all aspects of the work.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
