Abstract
Background
We assessed the impact of heparinised saline versus 0.9% normal saline on arterial line patency. Maintaining the patency of arterial lines is essential for obtaining accurate physiological measurements, enabling blood sampling and minimising line replacement. Use of heparinised saline is associated with risks such as thrombocytopenia, haemorrhage and mis-selection. Historical studies draw variable conclusions but suggest that normal saline is at least as effective at maintaining line patency, although recent evidence has questioned this.
Methods
We conducted a prospective analysis of the use of heparinised saline versus normal saline on unselected patients in the intensive care of our hospital. Data concerning duration of 471 lines insertion and reason for removal was collected.
Results
We found a higher risk of blockage for lines flushed with normal saline compared with heparinised saline (RR = 2.15, 95% CI 1.392–3.32, p ≤ 0.001). Of the 56 lines which blocked initially (19 heparinised saline and 37 normal saline lines), 16 were replaced with new lines; 5 heparinised saline lines and 11 normal saline lines were reinserted; 5 of these lines subsequently blocked again, 3 of which were flushed with normal saline.
Conclusions
Our study demonstrates a clinically important reduction in arterial line longevity due to blockages when flushed with normal saline compared to heparinised saline. We have determined that these excess blockages have a significant clinical impact with further lines being inserted after blockage, resulting in increased risks to patients, wasted time and cost of resources. Our findings suggest that the current UK guidance favouring normal saline flushes should be reviewed.
Introduction
Arterial lines are routinely inserted in the critically ill patient for continuous blood pressure monitoring, frequent blood sampling and assessment of arterial oxygenation. Biochemical and physiological measurements obtained from arterial lines affect clinical decision-making and assist in evaluating patient response to clinical intervention. Maintenance of arterial line patency is essential to reduce patient discomfort, time and financial expense incurred by blocked catheter replacement.1,2 Multiple factors including catheter flush solution have been shown to influence arterial line patency, with heparinised saline (HS) traditionally being used for its anticoagulant properties. 2
Current evidence regarding flush solution is conflicting, and uncertainty exists as to which solution is best. In 2008, the National Patient Safety Agency (NPSA) published a report recommending exclusive use of 0.9% normal saline (NS) as an arterial flush solution: subsequently use of HS in UK adult intensive care units has reduced to 4.6%.3,4 Despite this, serious errors involving administration of incorrect arterial flush solutions continue to occur. 5
In a recent publication, catheters flushed with HS had an increased lifespan and a significantly reduced likelihood of blockage. 6 This prompted suggestion that current debate should not only focus on patient safety but also on the implications of widespread use of NS flushes on patient morbidity.
At our university teaching hospital, HS is used as a flush solution. The aim of our study was to assess the impact of HS versus NS on arterial line patency and to perform a cost analysis of their use.
Methods
In 2014, our Intensive Care Unit decided to change its flush solution from HS to NS due to cost and pharmacy reasons. As such, this work was registered with our hospitals’ Audit Department, considered to be a service evaluation and ethics committee approval was not sought.
We conducted a prospective study analysing the use of HS and NS in maintaining invasive line patency. Over a four-month period in 2014, data were recorded on all elective and emergency admissions to the general adult ICU of our university teaching hospital. During the first and fourth months, data were collected on the use of HS to maintain arterial line patency. After a changeover period, HS was substituted for NS for the second and third months. Data concerning duration of line insertion and reason for line removal was collected from either our clinical information systems Innovian® or Phillips Intellispace Critical Care and Anesthesia® and details were clarified with bedside nursing staff where required.
Line insertion technique and site of insertion were unstandardised and lines were inserted in a variety of settings including intensive care, operating theatres and the Emergency Department. All lines were maintained and sampled using standard hospital protocols. Both NS and HS (2 units ml-1) were infused at a rate of 3 mls h−1 with 300 mmHg pressure applied to infuser bags.
Cost analysis was performed using the cost of all the equipment purchased in our department.
The demographic (sex and age) and clinical characteristics (admission type, nature of surgery, APACHE score, ICNARC score and where the first line was placed) of the two patient groups were compared using Fisher’s exact test for categorical variables and Mann–Whitney U test for continuous variables. The lifespans of the lines were compared using Mann–Whitney U test to compare all lines and to compare first lines only. Cox proportional hazards regression was used to compare the survival time for lines flushed with NS compared with HS. The following analyses were undertaken to test whether differences in length of insertion persisted when restricting the reason for line removal to blockages only (line blockage was defined as lines with a consistently unreliable arterial waveform or from which arterial blood samples could not be aspirated). The lines were further restricted to a comparison of the first lines inserted in patients to exclude the potential inflation of effect sizes due to patient-level influences on line survival.
Failure = Replacement of any line for any reason (lifespan of line considered censored if patient died); Failure = Replacement of any line due to blockage (all other reasons considered censoring). Assumed blockage = blocked (no trace)’ or blocked (no blood)’. As in second but restricted to first line received – sensitivity analysis in case patient-level factors affect the survival time of lines.
Risk ratios were derived to compare the risk of lines blocking when flushed with NS compared with HS. For reasons outlined above, we also undertook sensitivity analyses by restricting to the first lines inserted in patients.
Results
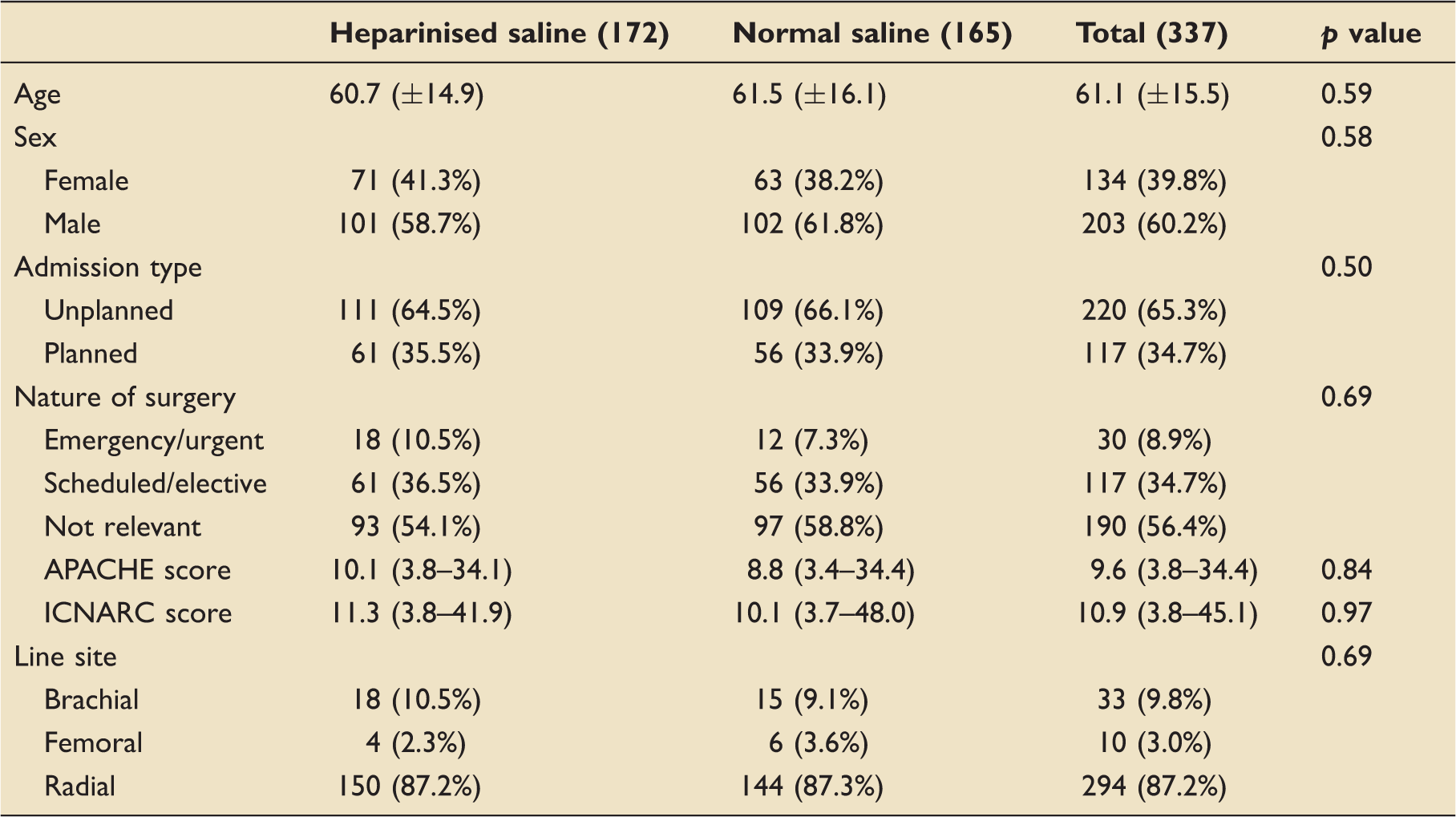
Demographics of patients with lines flushed with heparinised saline versus normal saline (first line inserted in each patient).
Reason for line removal.
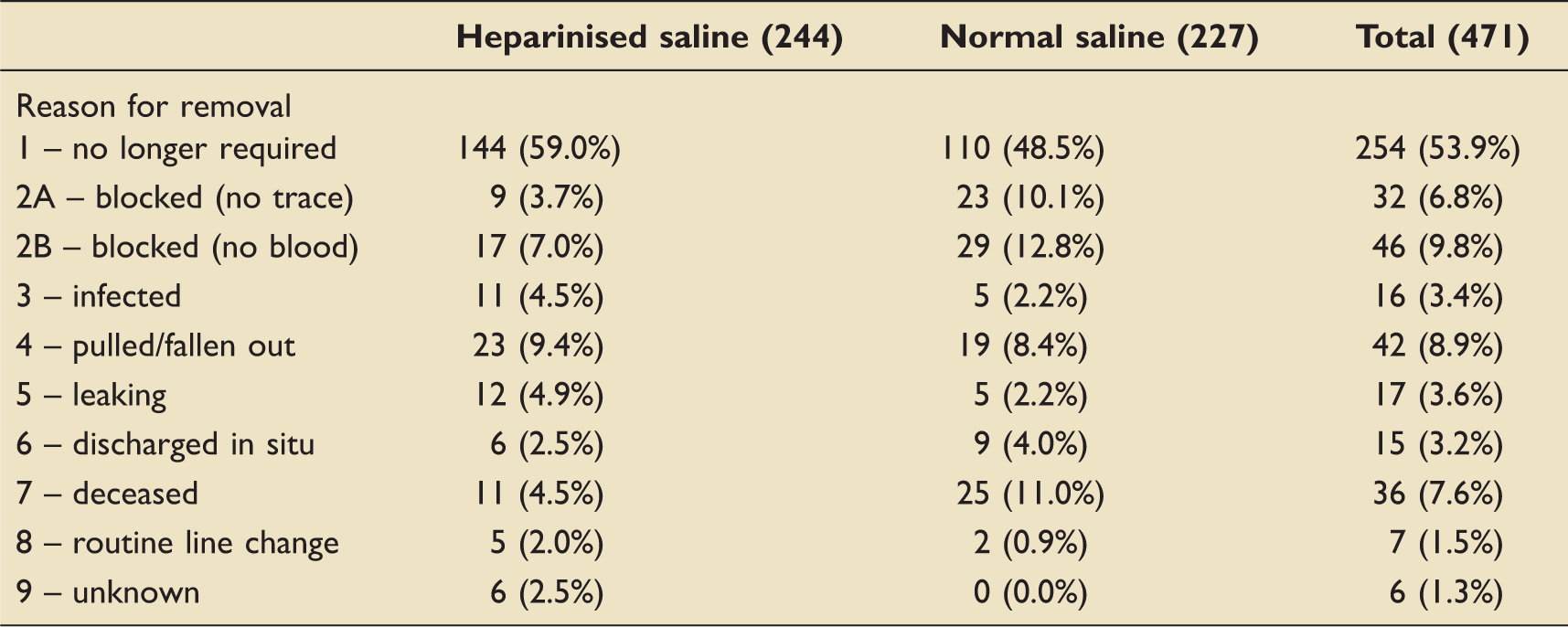
The median lifespan of all lines was two days (1–4). The median lifespan of lines flushed with HS and NS were comparable (median = two days, IQR = 1–4), but the Mann–Whitney U test found a slight difference in favour of HS lines (p = 0.035). This may be attributable to slight differences in the distribution of lifespans for the flush solutions, rather than a tendency towards overall longer lifespans in HS lines. However, restricting to the first line inserted in each patient the median lifespan was 2.5 days (IQR = 1–4) for lines flushed with HS compared with a median of two days (IQR = 1–3) for those flushed with NS (p = 0.004). The risk ratio showed a higher risk of blockage for lines flushed with NS compared with HS (RR = 2.15, 95% CI 1.392–3.32, p < 0.001), with a similar finding when data were restricted to only the first line inserted into each patient (RR = 2.03, 95% CI 1.219–3.381, p = 0.005).
Of the 56 lines which blocked initially (19 HS and 37 NS lines), 16 were replaced with new lines: 5 HS lines were replaced and 11 NS lines; 5 of these replaced lines subsequently blocked again, 3 of which had been flushed with NS, and one of these replaced lines which was flushed with NS blocked for a third time.
The hazard ratio for time to failure for any reason of lines flushed with NS compared with HS was 1.179 (95% CI 0.983–1.413, p = 0.076). When we restricted the reason for failure to blockages only the hazard ratio indicated that the time to failure for NS lines was less than for HS lines (HR = 2.471, 95% CI 1.542–3.960, p < 0.001, Plot 1), and further restricting to only the first line inserted into each patient (HR = 2.734, 95% CI 1.551–4.820, p < 0.001, Plot 2).
Kaplan–Meier survival curve for all lines placed, failure = line blocked. Kaplan–Meier survival curve for first lines placed only, failure = line blocked.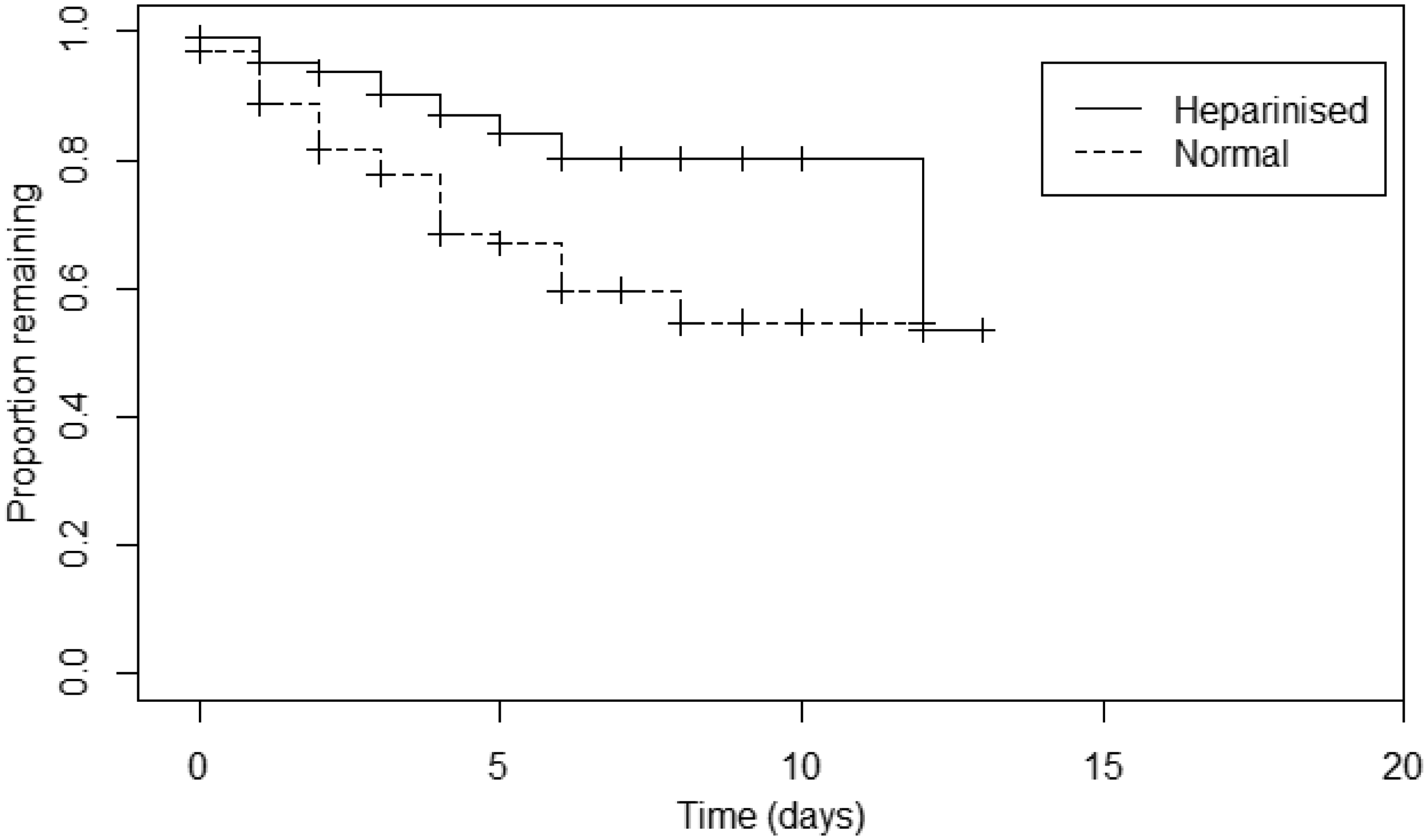
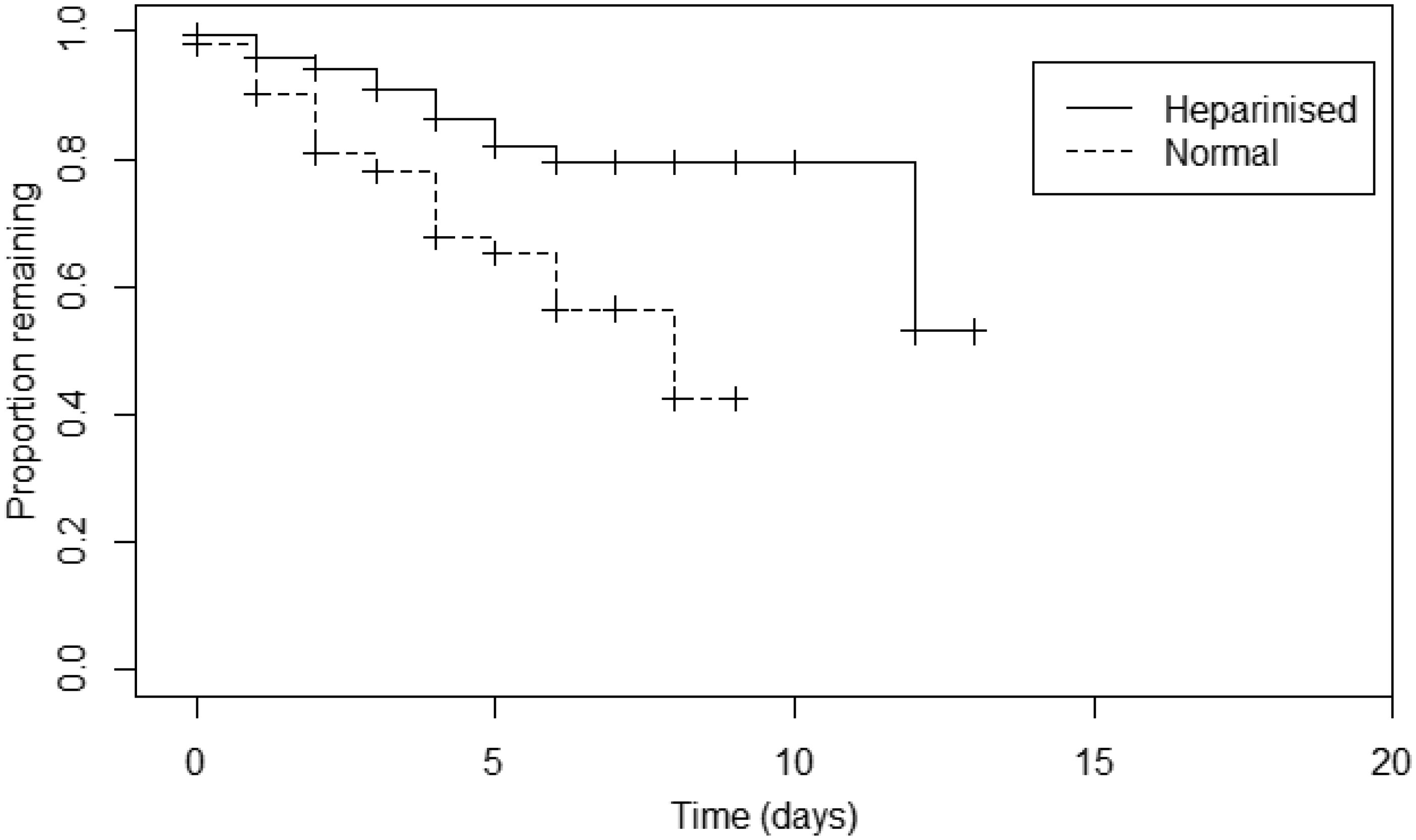
Despite small numbers for brachial and femoral versus radial lines, we found no difference between lifespan according to line site (p = 0.62). Subgroup analysis of radial line blockage showed HS flushed lines to survive longer (median for NS two days (IQR 1–3) versus HS two days (IQR 1–5), HR = 2.896 (p < 0.001)).
In using NS as a flush solution, our department saved £950 in one month, thus creating a projected saving of £11,400 per annum. An average of 100 lines is inserted per month on our ITU. If all of these lines were flushed with NS, with its associated increased rate of blockage, a further £547 would be incurred through catheter replacement, equating to £6564 per annum. Balancing this against the reduced cost of NS flush solution, an overall saving of approximately £403 per month would be made which equates to £4836 per year. This figure, however, has to be weighed against the increased patient morbidity with NS use. In addition, for the number of lines that were replaced, a greater proportion was not. The risk of harm as a result of this is unquantifiable.
Discussion
We have demonstrated a clinically significant increase in risk of line blockage when arterial lines are flushed with NS compared with HS, and these blockages occurred earlier in lines flushed with NS.
High quality evidence in this area is lacking. 2 One meta-analysis performed in 1998 demonstrated an increased longevity of lines flushed with HS. 7 This included one of the largest studies to date – a multicentre unblinded randomised control trial from the American Association of Critical Care Nurses. The study of 5139 subjects concluded that HS lines had a higher probability of remaining patent, compared to those flushed with NS. 8 Subsequent smaller studies have failed to demonstrate a difference between the two flush solutions.1,9,10,11 These studies are heterogeneous with variable HS flush concentrations, small sample sizes and inadequate statistical power. A recent Cochrane review summarised current evidence suggesting that NS is comparable to HS for maintaining catheter patency, whilst emphasising the poor quality of existing evidence. 2 A subsequent multicentre study demonstrated an increased lifespan and a significantly reduced likelihood of blockage in lines flushed with HS. 6 Whilst ours is a single-centred study, the strength of our results lies in our standardisation of equipment, procedures and data collection.
We demonstrated an overall cost saving with the use of NS. However, our economic evaluation did not include the increase in consumption of resources including clinicians’ time and additional line replacements causing potential morbidity to patients. During the period of replacement, inadequate non-invasive monitoring was undertaken. The potential misidentification of NS for a dextrose solution is an additional risk and cases of iatrogenic neuroglycopaenia are well documented. Inadvertent use of dextrose containing solution can lead to an artefactually raised glucose on sampling. Case reports have documented IV insulin administration in response to this, with subsequent hypoglycaemia.5,12 This led to the 2014 publication of an AAGBI guideline calling for stricter practical measures and changes in labelling to minimise risk. 13
Based on our findings and its distinctive labelling, we argue that HS may in fact be the superior and safest option despite the previously documented small risk of side effects (we recorded none), such as HIT, the risk of sampling contamination affecting clotting tests and despite its expense.
Our data were predominantly collected from documentation, and, therefore, this may limit the accuracy of our results; however, ambiguity was clarified with nursing staff in real time. Staff were not blinded to flush solution which could potentially bias how the lines were handled or data were recorded. Rewiring of lines was sometimes never recorded or was recorded as a new line insertion leading to some error in the data. Recording of line duration was made in whole days due to lack of accurate recording, especially when lines were inserted outside of the ITU. We did not investigate the use of concomitant anticoagulants as a confounding factor.
There is need for appropriately powered randomised-control trials to conclude if arterial lines flushed with HS have statistically lower blockage rates and increased longevity compared to NS, and the potential health economic impact of changing flush solution.
Conclusions
Our study demonstrates an increase in blockages in arterial lines when flushed with NS compared to HS. We have determined that these excess blockages have a significant clinical impact with further lines being inserted after blockage, resulting in increased risks to patients, wasted time and consumption of resources. Our findings suggest that the current UK guidance favouring NS flushes should be reviewed.
Footnotes
Acknowledgements
John Warburton – scientific advisor, Chris Sajdler – data collection, Catherine Stace – data collection.
Authors contribution
ME contributed for study design, patient recruitment, data collection, data analysis, writing up of the paper; LW for patient recruitment, data collection, data analysis, writing up of the paper; CP for data analysis, writing up of the paper; SS for study design, patient recruitment, writing up of the paper and DFT for study design, patient recruitment, data collection, data analysis, writing up of the paper.
Declaration of conflicting interests
The authors declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: The views expressed are those of the authors and not necessarily those of the National Health Service, the NIHR or the Department of Health.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: CP was financially supported by the NIHR Bristol Nutrition Biomedical Research Unit based at University Hospitals Bristol NHS Foundation Trust and the University of Bristol.
