Abstract
Background:
High-quality evidence comparing surgical strategies within 0–24 h and 24–72 h after aneurysmal subarachnoid hemorrhage (aSAH) remains limited. This study aimed to systematically evaluate surgical safety and long-term outcomes across these two critical time windows.
Methods:
Patients with aSAH undergoing aneurysm surgery within 72 h were consecutively enrolled from 12 tertiary centers in northern China between January 2017 and December 2020. A 1:1 propensity score matching (PSM) adjusted for intergroup differences, and a generalized estimating equation (GEE) model accounted for hospital-level clustering. Outcomes were compared between the 0–24 h and 24–72 h groups. Kaplan–Meier curves assessed survival, Cox models identified mortality risk factors, and logistic regression determined predictors of 2-year dependency.
Results:
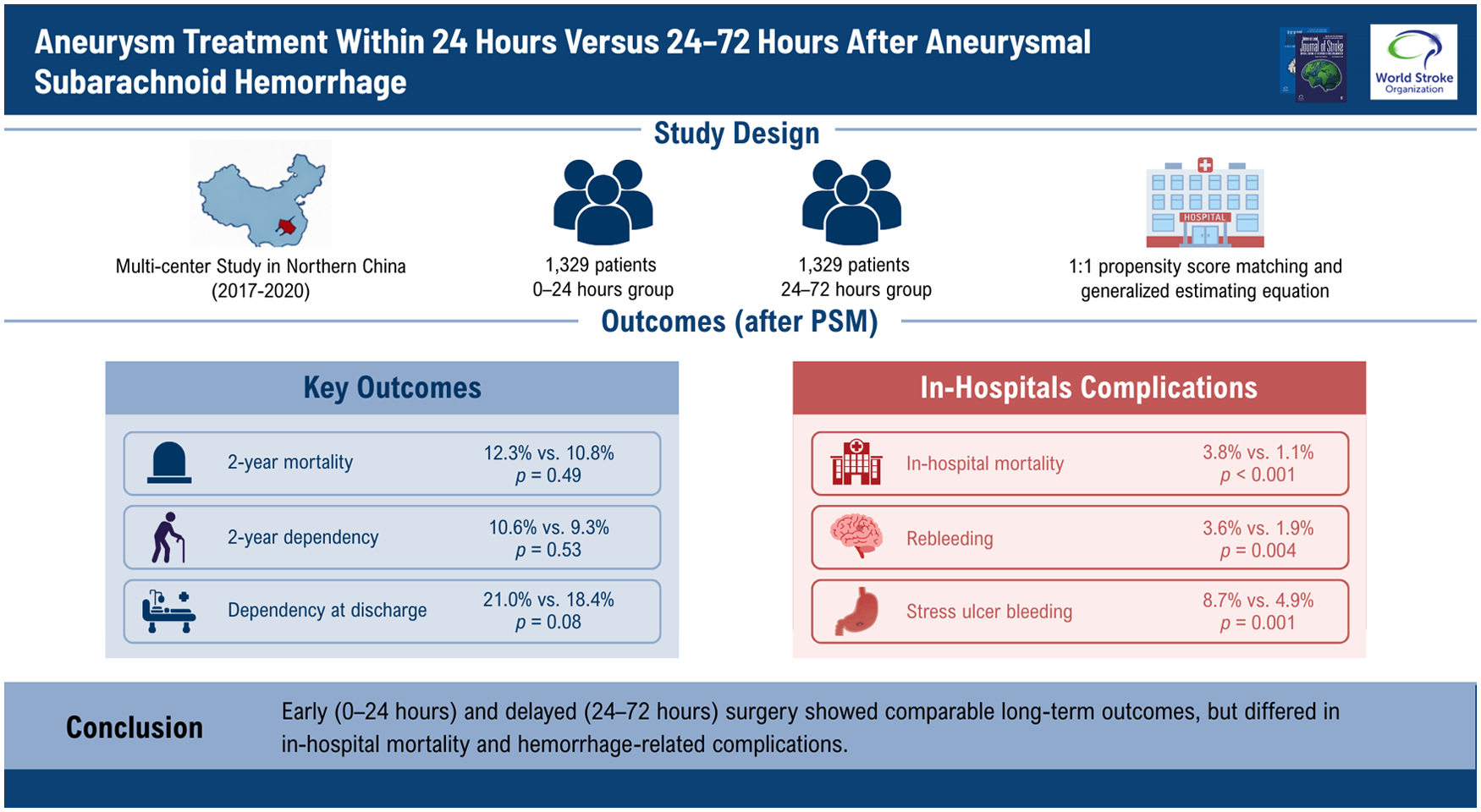
A total of 3560 patients were included. After PSM, 1329 patients in the 0–24 h group were matched with 1329 in the 24–72 h group. There were no significant differences in 2-year mortality (12.3% vs 10.8%, p = 0.49), dependency at discharge (21.0% vs 18.4%; adjusted odds ratio (OR) = 0.815, 95% confidence interval (CI) = 0.649–1.024, p = 0.079), or 2-year dependency (10.6% vs 9.3%; adjusted OR = 0.896, 95% CI = 0.636–1.264, p = 0.533). Compared with the 0–24 h group, the 24–72 h group had lower in-hospital mortality (3.8% vs 1.1%; adjusted OR = 0.503, 95% CI = 0.349–0.723, p < 0.001), rebleeding (3.6% vs 1.9%; adjusted OR = 0.489, 95% CI = 0.299–0.801, p = 0.004), and stress ulcer bleeding (8.7% vs 4.9%; adjusted OR = 0.811, 95% CI = 0.713–0.922, p = 0.001). Risk factors for mortality and 2-year dependency differed between groups.
Conclusion:
Surgery within 24 h of onset showed similar long-term outcomes compared with treatment at 24–72 h, but in-hospital mortality and some hemorrhage-related complications differed. Risk factor analysis may provide guidance for individualized treatment strategies.
Get full access to this article
View all access options for this article.
