Abstract
Background:
Moyamoya disease (MMD) is a rare cerebrovascular disorder for which nationwide epidemiological data on the pediatric population are limited. In Korea, the majority of published epidemiologic data on MMD entailed brief study periods and were published many years ago. Moreover, the majority of prior epidemiological studies on MMD have not examined the clinical outcomes associated with cerebral revascularization.
Aims:
To provide a comprehensive analysis of the recent epidemiological trends and cerebrovascular outcomes associated with pediatric moyamoya disease in the Republic of Korea.
Methods:
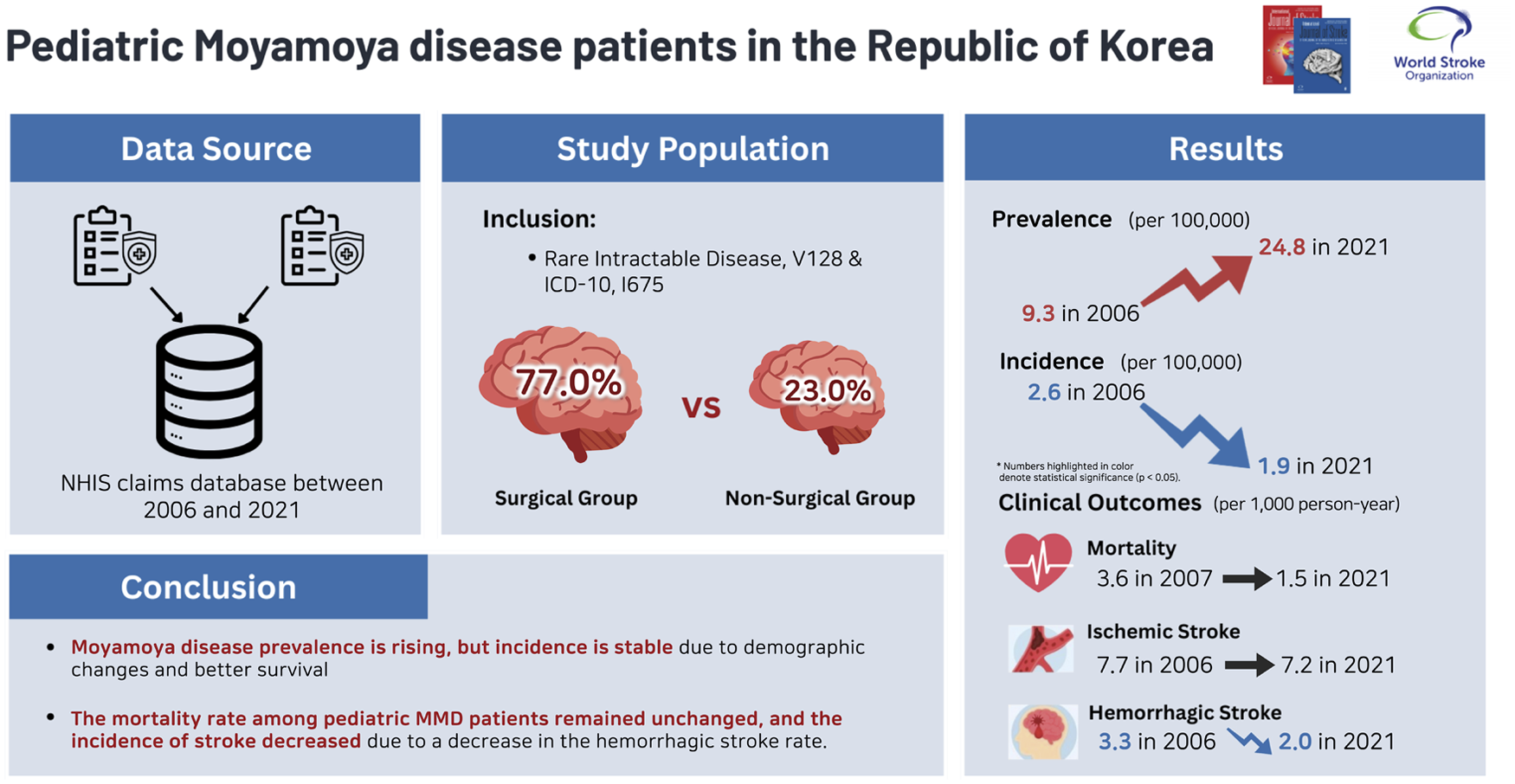
A retrospective cohort study was conducted using the Korean National Health Insurance Database, analyzing 4323 pediatric patients diagnosed with MMD between 2006 and 2021. Prevalence and incidence were assessed in all 4323 patients, and cerebrovascular outcomes were analyzed in 3656 of these patients. Patients were categorized into surgical and non-surgical groups, with surgical techniques including indirect bypass (IB), direct bypass (DB), and combined bypass (CB). To evaluate year-to-year variations, linear regression analyses were performed to identify and quantify temporal trends for all measured outcomes.
Results:
The mean observation period for the subjects was 10.3 years, with 12.1 years for the non-surgical group and 9.7 years for the surgical group. The prevalence of pediatric MMD increased from 9.3 to 24.8 per 100,000 between 2006 and 2021. Concurrently, the incidence rate has remained stable at approximately 2.0 per 100,000 since 2010. The surgical rate among prevalent cases has exhibited a gradual increase and has remained at approximately 88% since 2018. Furthermore, the case event rate for stroke has exhibited a downward trend over time, and a statistically significant reduction in hemorrhagic stroke was observed.
Conclusions:
In Korea, the prevalence rate of MMD continues to rise, while the incidence rate remains stable despite a reduction in absolute case numbers, reflecting demographic shifts and improved survival. The mortality rate among pediatric MMD patients remained unchanged; however, the incidence of hemorrhagic stroke was found to have decreased. Further multi-institution-based cohort studies are needed to clarify long-term cerebrovascular outcomes in this population.
Data access statement:
Researchers can access the NHIS database by submitting a request to the National Health Insurance Service Big Data Platforms (http://nhiss.nhis.or.kr).
Get full access to this article
View all access options for this article.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
