Abstract
Background:
Mobile stroke units (MSUs) improve outcomes in acute ischemic stroke (AIS), but their effectiveness is constrained by limited service radii. Integrating a rendezvous strategy with emergency medical services (EMS) may extend the operational reach of MSUs in rural areas.
Aim:
We evaluated whether a novel rendezvous approach between MSUs and EMS could enhance thrombolysis efficiency for rural AIS patients in a larger service area.
Methods:
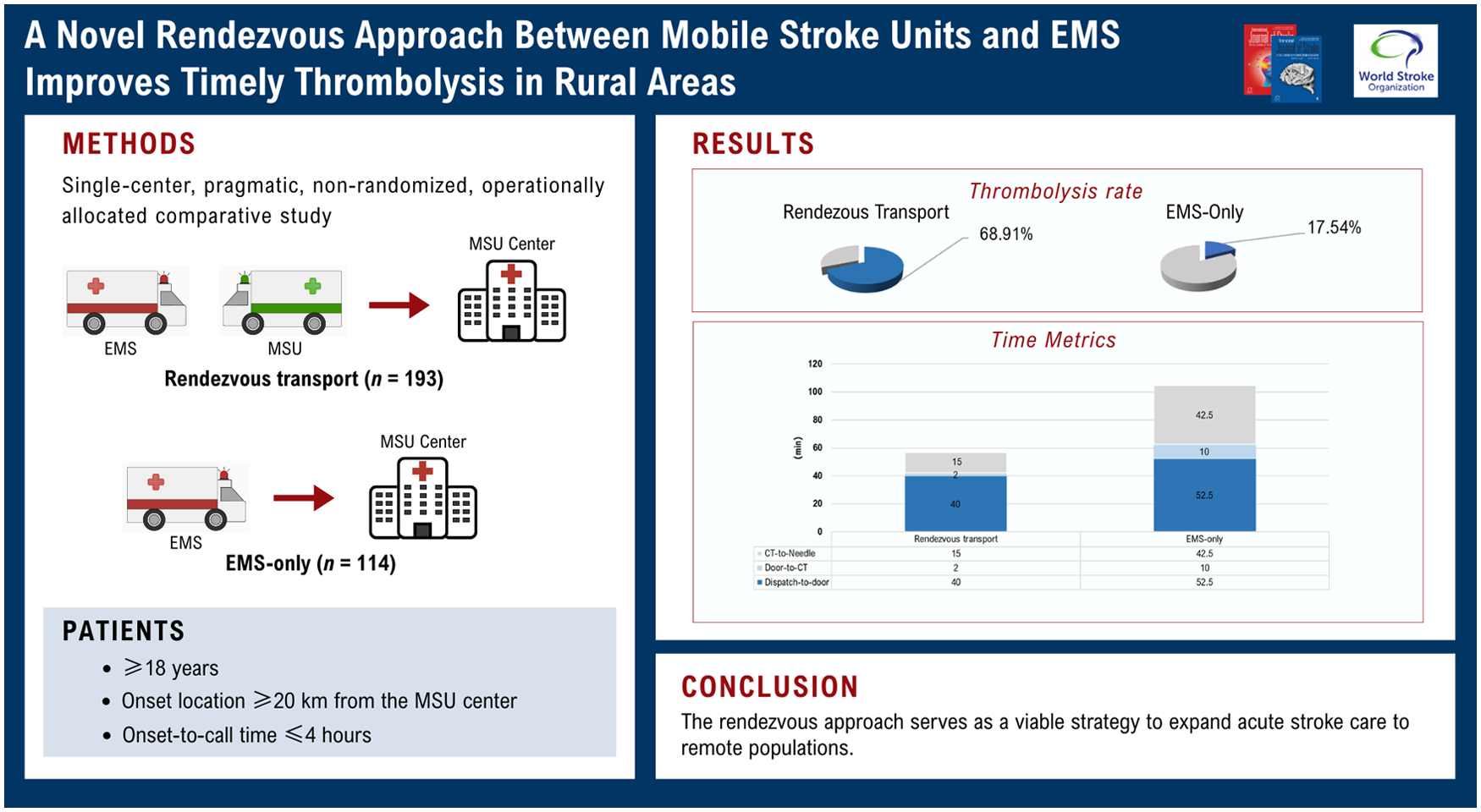
We conducted a single-center, pragmatic, non-randomized, operationally allocated comparative study in Suzhou, Anhui, from 1 January to 31 December 2024. When a suspected stroke call originated from a remote location, a nearby conventional ambulance was dispatched. Subsequently, the MSU was dispatched via an EMS call, met the EMS at a predetermined midway point en route to the stroke center, and treated the patient when MSU was available. Inclusion criteria were: age ⩾ 18 years; onset location ⩾ 20 km from the MSU center; and onset-to-call time ⩽ 4 h. Patients with a final diagnosis of cerebral ischemia were analyzed based on transport method (MSU rendezvous vs EMS only). The primary outcome was the thrombolysis rate; secondary outcomes included time metrics, 90-day functional prognosis, and incidence of symptomatic intracranial hemorrhage (sICH). Propensity score matching (PSM) was used to balance baseline characteristics.
Results:
A total of 307 patients with AIS were included; the median age was 72 years (IQR, 63–79), and 192 (62.50%) were male. One hundred ninety-three patients were transferred through rendezvous transport, and 114 patients were transferred through EMS-only. The median distance from onset location to hospital in the rendezvous transport group was 39.00 km (24.23 miles) (IQR 30.00–47.00 km), with a maximum of 68.00 km (42.25 miles). Compared with EMS-only transfers, patients transferred through rendezvous transport had a nearly 3-fold increase in thrombolysis rates (68.90% vs 17.50%, p < 0.001), reduced dispatch-to-door time by 12.5 min, door-to-needle time by 46 min, and onset-to-needle time by 60 min (all p < 0.001). In addition, in terms of clinical outcomes, patients in the rendezvous group had lower median 90-day modified Rankin Scale scores (2.0 (1.0–3.0) vs 3.0 (1.5–5.0), p < 0.001). These findings remained consistent after PSM.
Conclusion:
Our study demonstrates that the novel MSU-EMS rendezvous approach significantly improves thrombolysis rates and functional outcomes, serving as a viable strategy to expand acute stroke care to remote populations.
Data access statement:
Data collected for the study may be made available from the corresponding author to others upon reasonable request.
Keywords
Get full access to this article
View all access options for this article.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
