Abstract
Background:
India is facing a growing burden of stroke due to population aging, lifestyle changes, and increased exposure to risk factors. However, longitudinal data on stroke patterns and outcomes in India are limited.
Objectives:
This study assessed stroke patterns, risk factors, management practices, and outcomes using data from the Hospital-Based Stroke Registries (HBSRs) in India.
Methods:
This prospective hospital-based registry included 34,792 stroke cases from 30 centers across India, recorded between 2020 and 2022. Data on demographics, clinical features, risk factors, diagnostics, treatments, and outcomes were collected, with follow-up at 28 days and 3 months. Functional outcome was assessed using the modified Rankin Scale (mRS), along with data on recurrence.
Results:
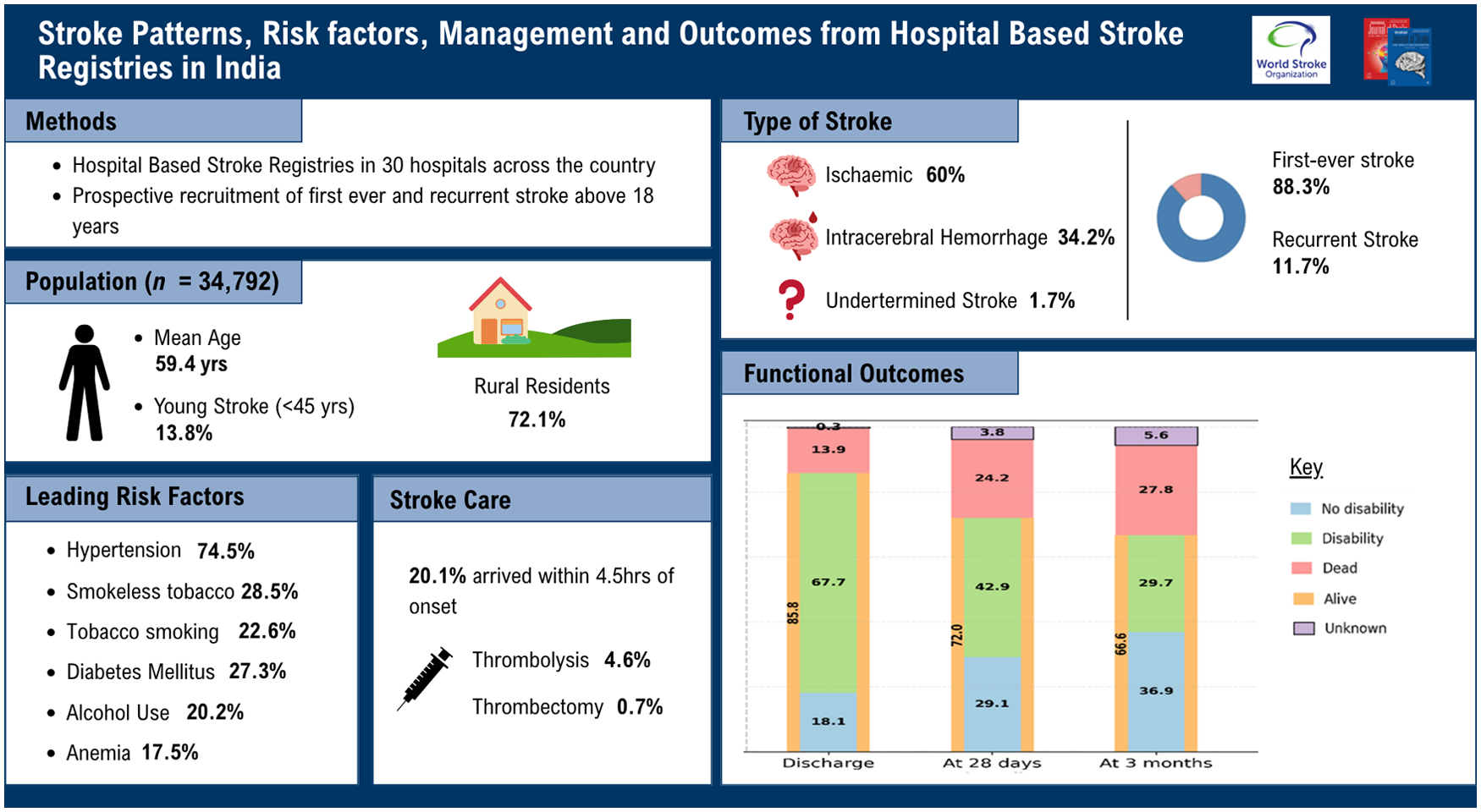
The mean age was 59.4 years; 13.8% were aged under 45, 63.4% were male, and 72.1% were from rural areas. Hypertension (74.5%) was the most common risk factor, followed by smokeless tobacco use (28.5%) and diabetes mellitus (27.3%). Ischemic stroke accounted for 60% of cases. Only 20.1% were presented within 4.5 h of symptom onset, while 37.8% of cases presented after 24 h. Motor impairment (74.8%) followed by speech disturbance (51.2%) were the commonest symptoms at onset. Thrombolysis was given in 4.6%, and thrombectomy in 0.7%, of ischemic strokes. At 3 months, 27.8% had died, 29.7% had significant disability (mRS 3-5), and 1.1% had a recurrent stroke.
Conclusion:
In this study, one in 7 stroke were in the young, 2 in 5 patients arrived after 24 h of symptom onset, and thrombolysis and mechanical thrombectomy were underutilized. Over half had poor 3-month outcomes, highlighting the need for improving comprehensive stroke care across India.
Introduction
Stroke remains one of the leading global health burdens, causing significant deaths and disability worldwide. 1 Hypertension, air pollution, tobacco smoking, high cholesterol, increased salt intake, and diabetes were the leading risk factors of stroke as per the Global Burden of Disease Study 2021. 2 Due to population growth, aging, and greater exposure to risk factors, the incidence of stroke is increasing significantly in low- and middle-income countries (LMICs), especially in India. 2 The estimated stroke incidence in India ranged from 108 to 172 per 100,000 population and 1-month case fatality varied from 18% to 42%. 3 The Population-Based Stroke Registries (PBSRs) established by the Indian Council of Medical Research—National Centre for Disease Informatics and Research (ICMR-NCDIR) reported a crude stroke incidence rate of 138.1 per 100,000 population and an age-standardized case fatality rate of 30 per 100,000 population. 4 When compared to disease patterns in the western countries, stroke tends to occur at a younger age and is associated with a higher case fatality rate in India.3,5
Stroke management in India faces multiple challenges including significant regional differences in stroke incidence and mortality across the country. Also, there are substantial disparities in stroke care services between urban and rural areas. 6 Poor public awareness, delay in seeking care, inadequately equipped acute stroke care facilities, and modest rehabilitation services are additional major challenges faced by stroke patients.7,8
Despite the growing burden of stroke and challenges in stroke care, data from India remain sparse and are largely limited to studies in single or small number of centers. The Hospital-Based Stroke Registries (HBSRs), under the ICMR-NCDIR National Stroke Registry Programme (NSRP) established across several hospitals providing stroke care in India, offer a systematic and standardized approach to collecting, analyzing, and disseminating stroke data. By capturing clinical, management, and outcome variables from diverse geographic and healthcare settings, HBSRs provide a unique, large-scale evidence base that can inform policy, guide resource allocation, and drive improvements in stroke care. This study utilizes data from these registries to address critical gaps in knowledge by analyzing stroke patterns, risk factors, management practices, and outcomes across India.
Methods
The NSRP, initiated by ICMR-NCDIR, aims to generate reliable data on the burden of stroke in defined populations through the PBSR and to capture information on the patterns and outcomes of stroke across various healthcare settings through the HBSR. 9 HBSR is a prospective collection of data from all the consecutive cases of stroke including both first-ever and recurrent stroke, aged 18 years and above, reporting at the registry hospitals within 28 days of onset of stroke. A first-ever stroke was defined as the initial stroke in a person’s lifetime, while a recurrent stroke was defined as any new stroke event occurring more than 21 days after the onset of the initial stroke, or if it occurs earlier, involving a different vascular territory. 10
The data included patients’ demographic information, clinical presentation, and risk factors, as well as diagnostic and treatment details. Cases were classified as ischemic stroke (IS), intracerebral hemorrhage (ICH), subarachnoid hemorrhage (SAH), or venous stroke based on clinical and imaging findings. Cases that could not be categorized due to unavailable imaging information were classified as undetermined stroke (UD). All the cases were followed up on day 28 and 3 months after the onset of stroke, during which information on patients’ disability status, measured by the modified Rankin Scale (mRS), and information on recurrent stroke during the follow-up period was collected. Detailed descriptions of the HBSR design, study tools, data collection procedures, and quality management processes are provided elsewhere. 9 For this study, data from 30 HBSRs including public, private, and non-governmental organizations (NGOs)/trusts, across the country registered between 2020 and 2022 were analyzed (Figure 1). These centers were registered in a phased manner, with 10 centers registered each year over the 3-year period.
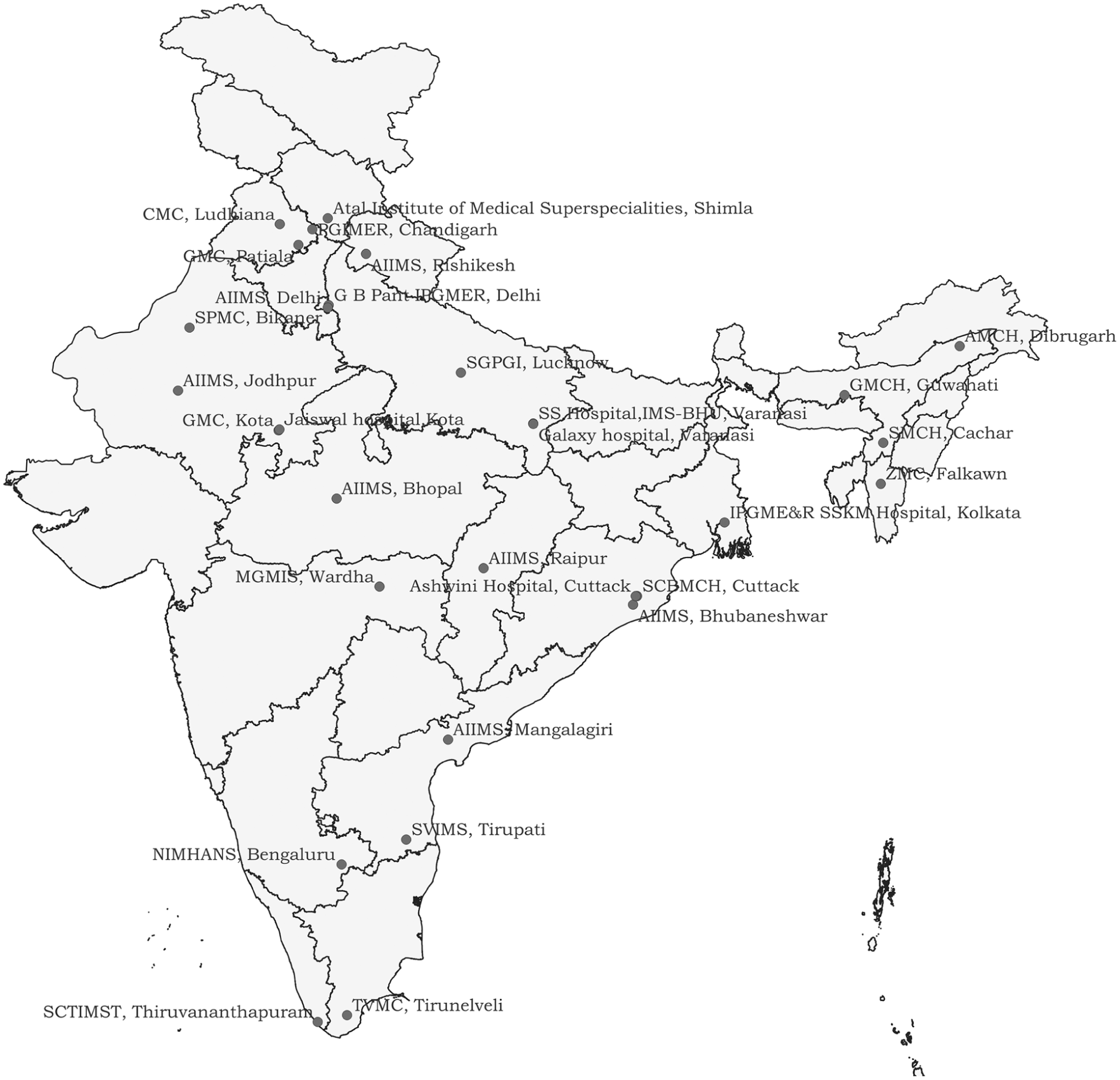
Participating centers in the hospital-based stroke registry 2020–2022.
Statistical analysis
Statistical analyses were performed using STATA version 14 (StataCorp. 2015, Stata Statistical Software: Release 14. College Station, TX, USA: StataCorp LLC). Descriptive statistics are presented as mean ± standard deviation (SD) and median with interquartile range (IQR) for continuous variables and as frequencies (percentages) for categorical variables. Patient functional outcomes were assessed using the modified Rankin Scale (mRS), with outcomes categorized as no disability (mRS score 0–2), disability (mRS score 3–5), and death (mRS score 6). The occurrence of recurrent stroke during hospitalization, on day 28, and at 3 months was analyzed separately for patients admitted with a first-ever stroke and those admitted with a recurrent stroke.
Results
A total of 34,792 stroke cases were registered between 1 January 2020 and 31 December 2022, with females accounting for 36.6% of the cases. The mean age of the participants was 59.4 ± 13.9 years, and the majority were in the 45- to 64-year age group. Stroke in the younger age group (aged < 45 years) constituted 13.8% of the total cases. Nearly three-fourths of the participants were residents from rural areas, and 90% of the patients were recruited as in-patients (Table 1).
Socio-demographic and clinical profile of the stroke cases registered in HBSRs.
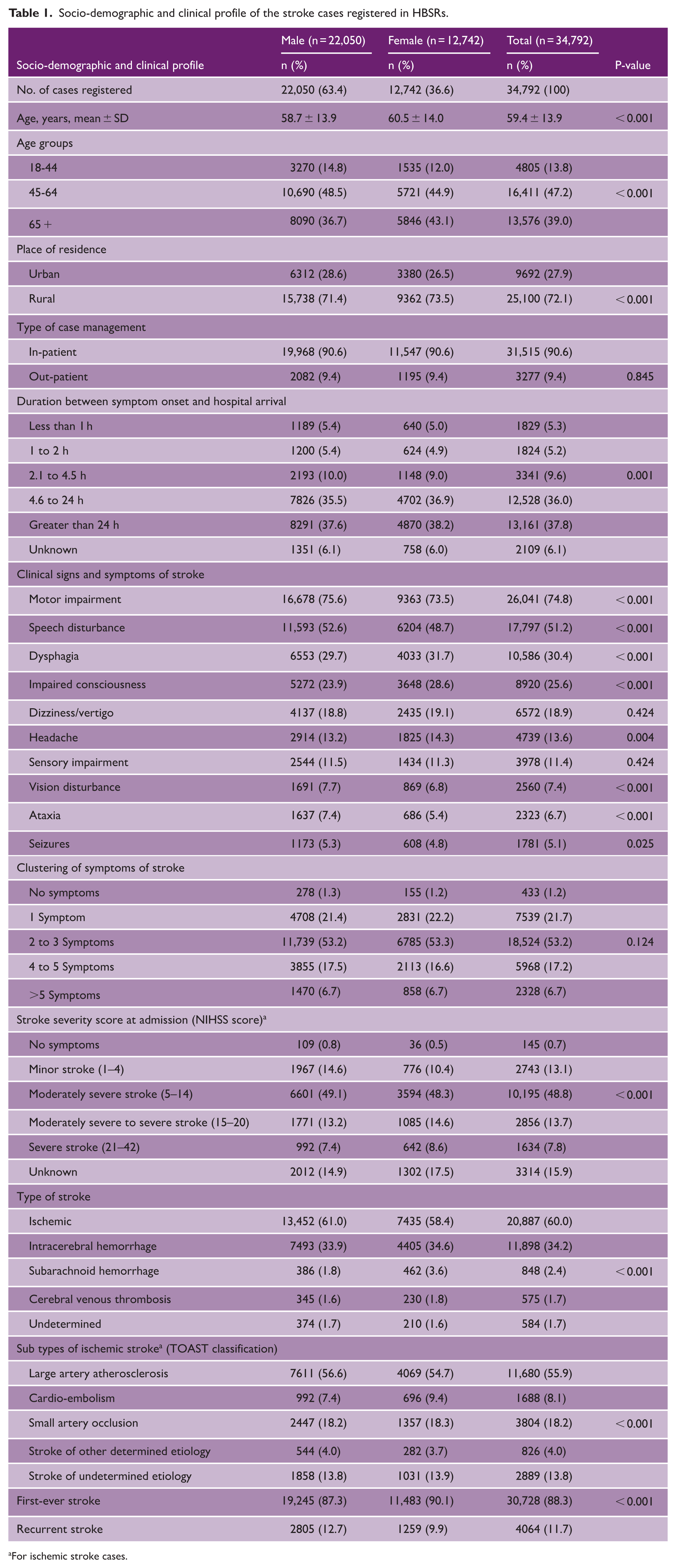
For ischemic stroke cases.
In total, 20.1% of participants arrived at the hospital within the first 4.5 h of onset of stroke symptoms, of which 5.3% arrived within the first hour (golden hour). Motor impairment was the most common clinical presentation (74.8%), followed by speech disturbance (51.2%), dysphagia (30.4%), and impaired consciousness (25.6%). About three-fourths of the cases presented with more than two symptoms at admission. Nearly 50% of participants presented with moderate stroke severity (National Institutes of Health Stroke Scale (NIHSS) = 5–14), and 7.8% had severe stroke (NIHSS = 21–42). IS was the most common type, accounting for 60% of cases, followed by ICH and SAH. Less than 2% of cases had venous strokes and UDs. Large artery atherosclerosis (55.9%) was the most common subtype of IS, followed by small artery occlusion (18.2%) and stroke of undetermined etiology (13.8%). In total, 8.1% of IS cases had cardioembolism which was higher among females (9.4%) compared to males (7.4%). Recurrent stroke was observed in 12.7% of men, compared to approximately 10% of women (Table 1).
At admission, hypertension was present in three-fourths of the stroke cases, making it the leading risk factor among both males and females. Among males, other major risk factors included tobacco smoking, smokeless tobacco use, alcohol consumption, diabetes mellitus, and anemia. In females, hypertension was followed by diabetes mellitus, smokeless tobacco use, and anemia (Table 2).
Risk factors of the stroke cases registered in HBSRs by gender.
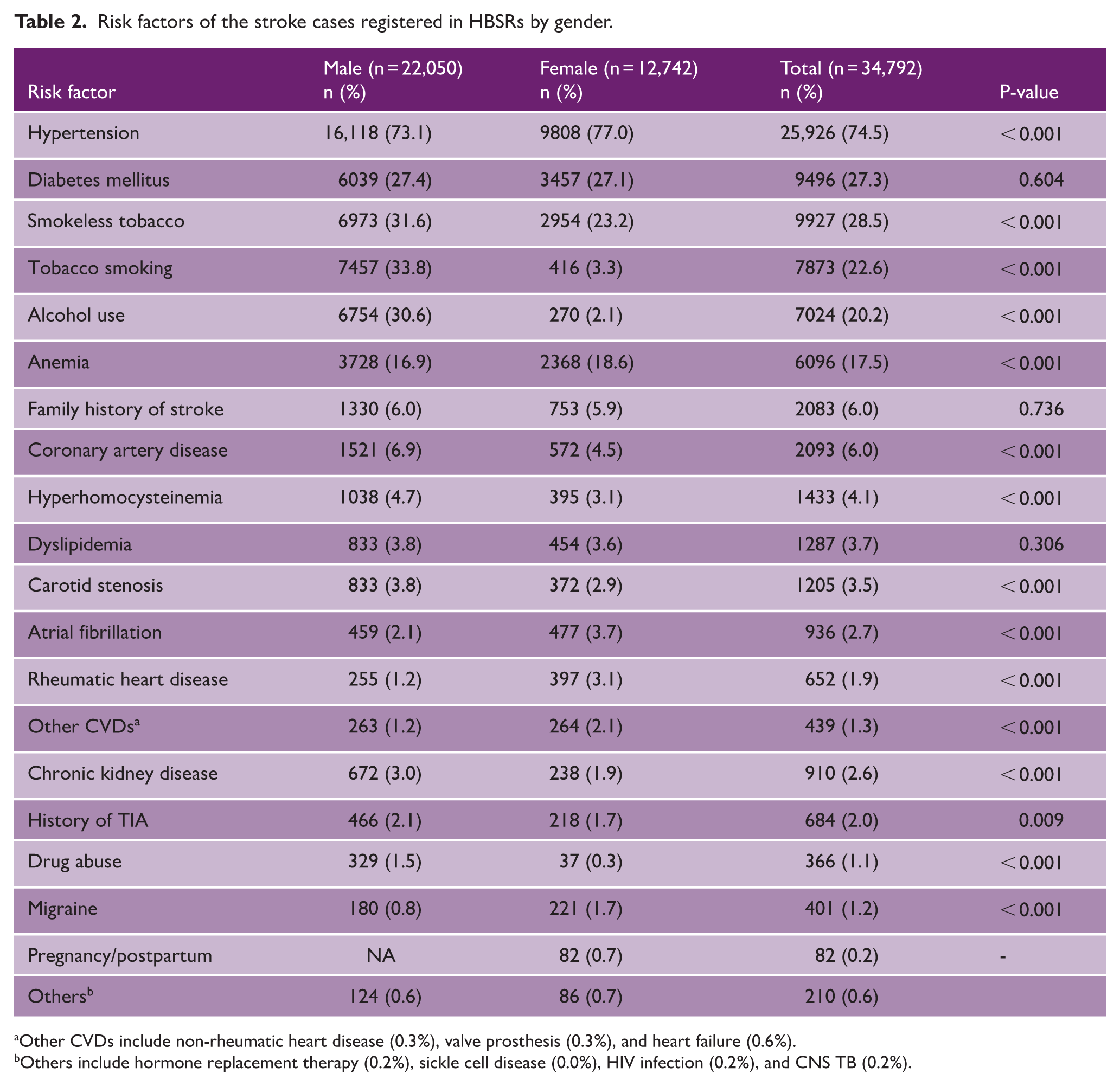
Other CVDs include non-rheumatic heart disease (0.3%), valve prosthesis (0.3%), and heart failure (0.6%).
Others include hormone replacement therapy (0.2%), sickle cell disease (0.0%), HIV infection (0.2%), and CNS TB (0.2%).
Diagnostic imaging was performed in 98.3% of patients, with the majority (64.5%) undergoing only computed tomography (CT) brain scans. Both CT and magnetic resonance imaging (MRI) were performed in 15.7% of cases, while 5.5% underwent MRI alone. CT/MR angiography was done in 15.9% of the cases, among which 13% was done for IS cases. Of the 20,887 IS cases, 860 (4.6%) received intravenous thrombolysis and 129 (0.7%) underwent mechanical thrombectomy (Table 3). The main reasons for not thrombolysing IS cases were delayed presentation (74.5%), in-hospital delay in imaging (12.6%), and non-availability of medicine (11%) (Supplemental Table 1). In total, 1.9% of IS cases who underwent thrombolysis had some serious complications after thrombolysis (Supplemental Table 2). The surgical procedures/interventions for stroke management were done in less than 2% of cases. Antiplatelets and anticoagulants were already administered by previous hospitals in 11.2% and 1.4% of IS cases, respectively, before arrival to the reporting hospital. During hospital stay, 87.4% of ischemic cases received antiplatelets, while 19.1% received anticoagulants. Both males and females had a median hospital stay of 6 days, and about half of the admitted cases stayed between 3 and 7 days (Table 3).
Diagnostic procedures and treatment of the stroke cases registered in HBSRs.
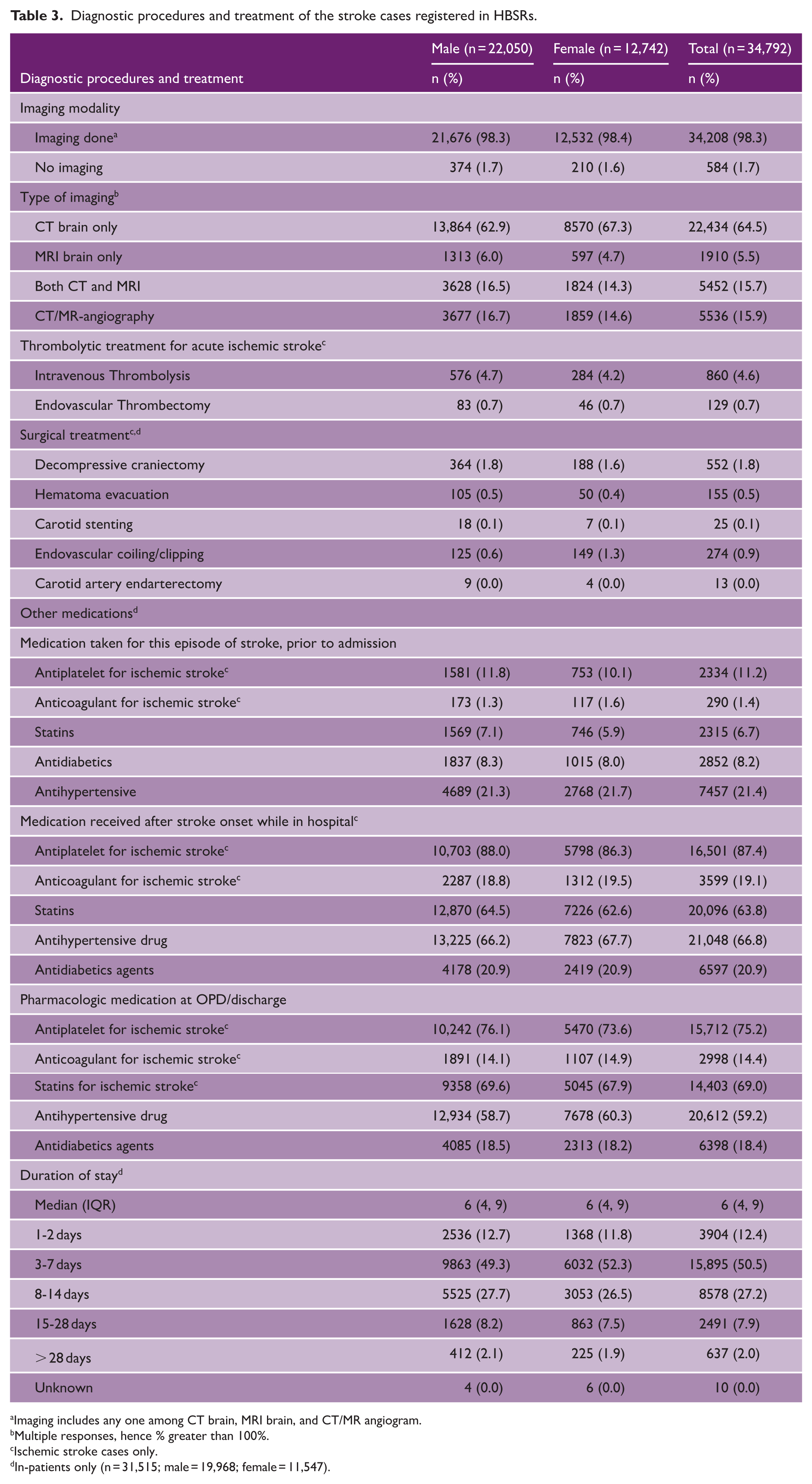
Imaging includes any one among CT brain, MRI brain, and CT/MR angiogram.
Multiple responses, hence % greater than 100%.
Ischemic stroke cases only.
In-patients only (n = 31,515; male = 19,968; female = 11,547).
The in-hospital mortality rate was 13.9%, and 67.7% of participants were discharged with some disability (mRS = 3–5). The mortality rate increased to 24.2% and 27.8% at 28 days and 3 months, respectively. At discharge, mortality rates were similar between males and females; however, a higher proportion of females (71.2%) experienced disability (mRS = 3–5) compared to males (65.9%). This trend persisted at both 28 days and 3 months, with only 32% of females showing no disability (mRS 0–2), compared to nearly 40% of males with no disability at 3 months. At 28 days, 43% of cases experienced disability, while nearly 30% had no disability. By 3 months, 37% of survivors were free of disability, whereas 29.7% continued to experience some disability (Figure 2).
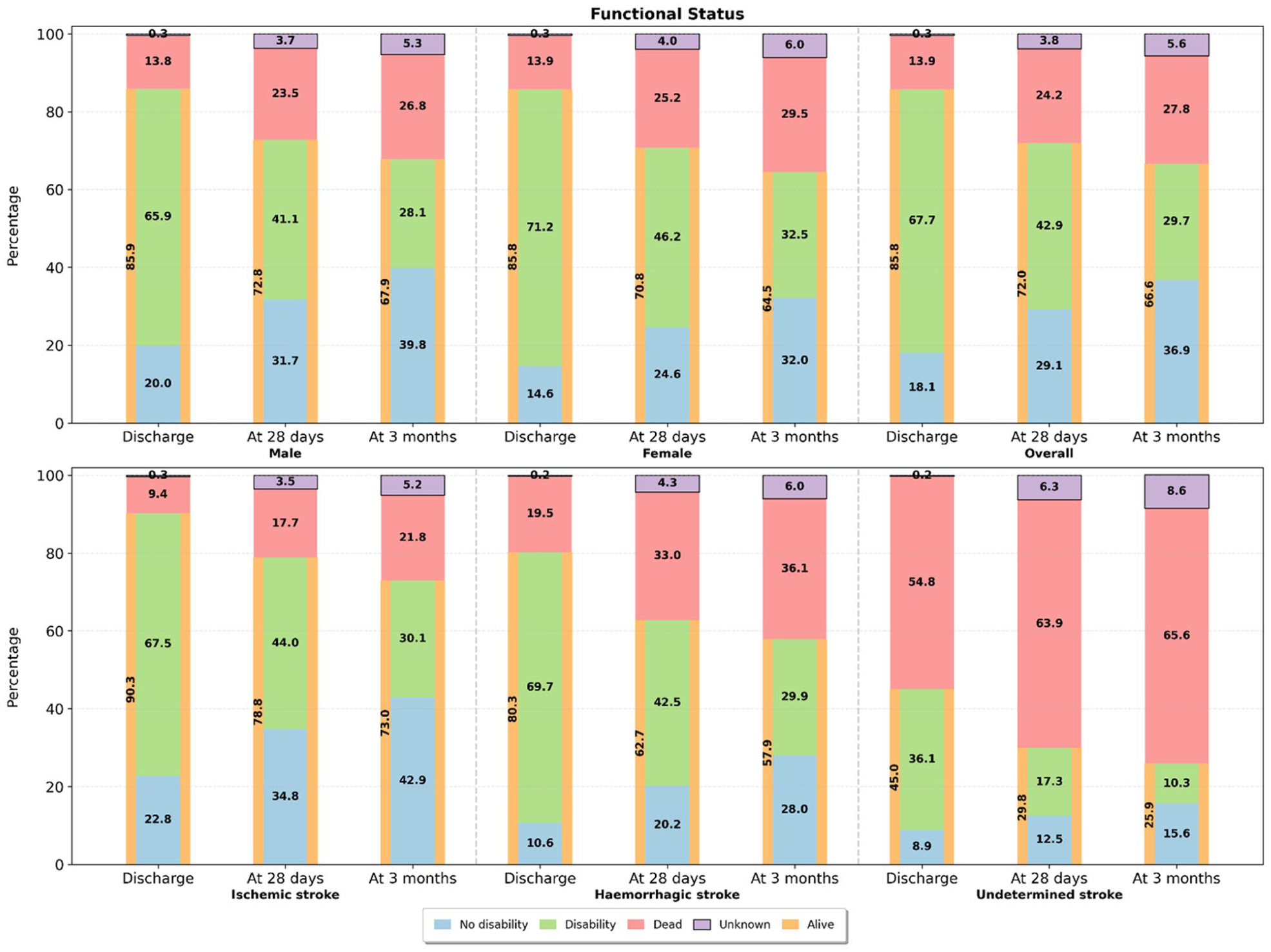
Functional status (mRS) of the stroke cases registered in HBSRs. No disability = mRS 0–2, disability = mRS 3–5, and dead = mRS 6.
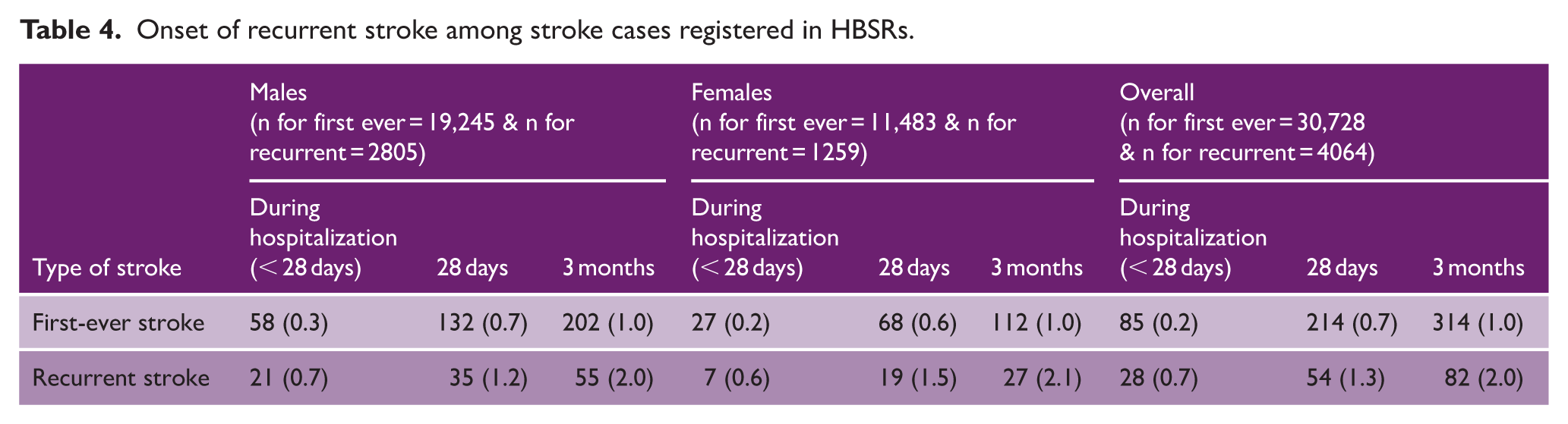
At 3 months, UD had the highest mortality rate (65.6%), followed by hemorrhagic stroke (36.1%) and IS (21.8%). IS showed the most favorable outcomes, with 42.9% of patients having no disability, compared to 28% of no disability among those with hemorrhagic stroke (Figure 2). Overall, 1.1% of cases experienced stroke recurrence within 3 months. Among patients admitted with a first-ever stroke, 1% had a recurrent stroke within this period. Whereas 2% of those admitted with a recurrent stroke experienced an additional stroke within 3 months (Table 4).
Onset of recurrent stroke among stroke cases registered in HBSRs.
Discussion
This study provides a comprehensive analysis of stroke cases from 30 hospitals across India, offering valuable insights into the stroke pattern, risk factor profiles, management practices, and outcomes. More than 50% of stroke cases experienced poor outcomes at 3 months, with 27.8% resulting in death and 29.7% in disability.
The mean age of stroke patients in our study was 59.4 years, with a substantial proportion of strokes in young cases (13.8%). This is consistent with earlier reports suggesting that stroke in India occurs at a younger age compared to western countries.5,11,12 A meta-analysis from the studies conducted in low- and lower-middle-income countries reported that 48% of cases reported to hospital within 24 h of onset of stroke. 13 Our study documented a slightly higher rate of 56.1% of cases reporting within the first 24 h of onset of stroke. A study from Kerala recorded 43.5% of cases of minor stroke with an NIHSS score of <4, 12 while our study observed only 11% of such cases. The higher proportion of severe stroke cases observed in our study might be attributed to the fact that most hospitals in our registry are tertiary care centers, which typically receive more critical cases. In addition, a majority of participants were from rural areas (72.1%), where limited awareness of stroke symptoms and delays in seeking medical care may have contributed to the severity at presentation.
The predominance of IS (60%) in our study is in line with findings from other studies across India11–13 and other south-east Asian countries,14,15 where IS is more common than hemorrhagic stroke. A higher frequency of ICH (34.2%) compared to high-income countries, consistent with previous studies from India,11,14 may be attributed to the high prevalence and suboptimal management of hypertension in India. 14 The most common subtype of IS in our study was large artery atherosclerosis (55.9%), which was higher than reported in other studies from India.16,17 Previous research has shown a high prevalence of intracranial stenosis in the Indian population,18,19 likely driven by risk factors such as hypertension, hyperlipidemia, diabetes, and tobacco use. However, our study did not collect information on intracranial or extracranial stenosis. Recurrent strokes accounted for 11.7% of admissions in our study, a proportion consistent with findings from other previous studies from India.11,12
The high prevalence of hypertension (74.5%), along with smokeless tobacco use (28.5%), diabetes mellitus (27.3%), tobacco smoking (22.6%), and alcohol use (20.2%) among stroke patients, underscores their significant role as major modifiable risk factors in the Indian population. Similar findings highlighting the high prevalence of these modifiable risk factors have been reported in other Indian studies.11,12 Our study also highlights gender differences in stroke risk factors. Among females, hypertension and diabetes mellitus were more prevalent, with smokeless tobacco use and anemia also emerging as significant factors. In contrast, the predominant risk factors in males included hypertension, tobacco smoking, smokeless tobacco use, and alcohol consumption. Similar trends were seen in other studies done in India 20 and other Asian countries like China 21 and Vietnam. 22 These gender disparities may be influenced by differences in lifestyle and healthcare access between men and women in India. These findings underscore the need for gender-specific prevention strategies, with a particular focus on tobacco control and the management of hypertension, diabetes, and anemia in women.
The low utilization of thrombolysis (4.6%) and mechanical thrombectomy (0.7%) and other surgical interventions is a concerning finding. Other studies done in India12,23 and Sri Lanka 15 also report similar results, highlighting the ongoing challenges in access to advanced stroke care, particularly for patients in rural and underserved areas where timely medical interventions are limited. In our study, among the 95% of IS cases that did not receive thrombolysis, the primary reasons were delayed hospital arrival, delays in imaging, and unavailability of the medication. Our study reported a higher in-hospital mortality rate of 13.9% compared to other studies from India11,12,20 but slightly lower than those reported from other LMICs. 13 This could be attributed to variations in healthcare infrastructure, stroke management practices, and the severity of cases included in the studies. At each follow-up, UD showed the highest mortality rate (54.8%, 63.9%, and 65.6% at discharge, 28 days, and 3 months, respectively). This may be attributable to critically ill patients who were clinically diagnosed as stroke but either succumbed before undergoing diagnostic investigations or were discharged against medical advice and subsequently died at home. While males and females had comparable outcomes at discharge, females showed poorer outcomes by the 3-month follow-up. This suggests gender disparities in post-discharge stroke care, particularly within our predominantly rural study population. Studies from countries such as Korea, Taiwan, and Germany24–26 report recurrent stroke rates of 3.4–3.9% within 3 months. In contrast, our study observed a lower recurrence rate of 1.1%, which may be attributed to attrition bias in the patients who experienced a recurrent stroke.
One of the key strengths of this study is its large sample size, with data collected from 30 HBSRs across India, providing a broad representation of stroke cases from different geographic regions. The prospective design and standardized data collection methods ensure high-quality and reliable findings. However, since the study is based on hospital registry data, it may exclude stroke cases that did not seek medical care in those hospitals, such as older patients or those with milder NIHSS, particularly in rural or resource-limited settings. This may limit the generalizability of the findings to the broader Indian population. Similar to research findings from both India and globally,27,28 stroke cases in the present study may be underrepresented due to disruptions in stroke care during the COVID-19 pandemic. In addition, the missing data due to poor follow-up information at 28 days and 3 months could lead to an underestimation of mortality, disability, and recurrence rates.
The findings from our study highlight the need for comprehensive stroke prevention and management strategies in India. Key priorities include raising awareness about modifiable risk factors, early recognition of stroke symptoms, reducing delays in seeking care, and the importance of pre-hospital, acute, and post-stroke care, particularly among females and rural populations. The National Programme for Prevention and Control of Non-Communicable Diseases (NP-NCD) plays a key role in promoting healthy lifestyles, raising public awareness, and supporting early detection to reduce stroke-related risk factors. Improving access to acute stroke care, including thrombolysis, and mechanical thrombectomy, especially in rural and underserved areas, remains a key challenge. In this context, healthcare initiatives like Ayushman Bharat Pradhan Mantri Jan Arogya Yojana (ABPM-JAY) are instrumental in enhancing financial access to advanced stroke interventions for economically vulnerable populations. In addition, enhancing the capacity of healthcare providers at the primary care level through training in timely stroke diagnosis and referral, along with ensuring the availability of follow-up and rehabilitation services, are critical steps toward improving stroke outcomes.
Conclusion
This multi-centric registry-based study provides important insights into the clinical characteristics, risk factors, management practices, and outcomes of stroke in India. The findings highlight the gaps in acute stroke care, including delayed hospital arrival, limited access to advanced treatments, and inadequate follow-up services. Stroke continues to pose a major public health burden, with poor outcomes. The findings of the study shall contribute to the development of evidence-based comprehensive strategies for stroke prevention, effective management, and improved treatment outcomes.
Supplemental Material
sj-docx-1-wso-10.1177_17474930251393187 – Supplemental material for Stroke patterns, risk factors, management, and outcomes from hospital-based stroke registries in India
Supplemental material, sj-docx-1-wso-10.1177_17474930251393187 for Stroke patterns, risk factors, management, and outcomes from hospital-based stroke registries in India by Prashant Mathur, Deepadarshan Huliyappa, Prathyusha PV, Vinay Urs, Rahul Rajendra Koli, Sureshkumar N and Kavyashree Seenappa in International Journal of Stroke
Footnotes
Acknowledgements
The authors acknowledge the registry staff involved in data abstraction and entry and project staff involved in data cleaning for their support during the conduct of the study.
National Stroke Registry Programme (NSRP) Investigators
Ashok Kumar Mallick,17474930251393187Nihar Ranjan Biswal, Vijay Sardana, S Saravanan, S Ravi, Ramachandiran Nandhagopal, B Vijayalakshmi Devi, Rameshwar Nath Chaurasia, Varun Kumar Singh, Sanjay Jaiswal, Hritvik Jaiswal, Paramita Roy, Bhaskar Debnath, Binod Sarmah, Kamal Rajkhowa, Dheeraj Khurana,17474930251393187 Sucharita Ray, Maya17474930251393187Gantayet, Soumya Ranjan Pradhan, Samhita Panda, Sarbesh Tiwari, P N Sylaja, Sapna Erat Sreedharan, Vishwesh Dutt Tiwari, Kumar Ashish, Marami Das, Anjanjyoti Talukdar, Mritunjai Singh, Kavya Bhatt, Priyanka V Kashyap, Debashish Chowdhury, Sanjeev Kumar Bhoi, Menka Jha, Biman Kanti Ray, Babuji Santra, Girish Baburao Kulkarni, R Subasree, Inder Puri, Divya Goswami,17474930251393187 Rohit Bhatia, M V Padma Srivastava, Sudheer Sharma, Rajeshwar Sahonta, Jeyaraj Durai Pandian, Raminder Sibia, Manjinder Singh Mann, Jyoti Jain, Madhura Joshi,17474930251393187Vinay R Pandit, Saravana Sukriya S, Rakesh Uppara Kadiyala, Sridhar A, Jayantee Kalita, Ruchika Tandon, Vanlalhruaii Vanlalhruaii, Rohmingmawia Rohmingmawia.
Author contributions
P.M., D.H., and P.P.V. contributed to the conceptualization and design. All authors contributed to the data acquisition. D.H., P.P.V., and R.R.K. contributed to the analysis and interpretation of data. D.H. contributed to drafting the manuscript. All contributed to critical review for important intellectual content.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The study received funding support from an intramural grant from the Indian Council of Medical Research-National Centre for Disease Informatics and Research.
Ethical approval
Ethics approval was obtained from the ICMR-NCDIR Institutional Ethics Committee (No: NCDIR/IEC/2018/5 dated 12 April 2018) and from the institutional ethics committees of the respective participating hospitals/medical colleges.
Data availability
HBSR data are not readily available. Data requests may be considered upon reasonable request and should be directed to the corresponding author.
Supplemental material
Supplemental material for this article is available online.
