Abstract
Background:
Almost half of acute ischemic stroke patients present with mild symptoms and there are large practice variations in their treatment globally. Individuals with an intracranial occlusion who present with minor stroke are at an increased risk of early neurological deterioration and poor outcomes. Individual patient data meta-analysis in the subgroup of patients with minor deficits showed benefit of alteplase in improving outcomes; however, this benefit has not been seen with intravenous alteplase in published randomized trials.
Design:
TEMPO-2 (A Randomized Controlled Trial of Tenecteplase Versus Standard of Care for Minor Ischemic Stroke With Proven Occlusion) is a prospective, open label with blinded outcome assessment, randomized controlled trial, designed to test the superiority of intravenous tenecteplase (0.25 mg/kg) over nonthrombolytic standard of care, with an estimated sample size of 1274 patients. Adult patients presenting with acute ischemic stroke with the National Institutes of Health Stroke Scale (NIHSS) ⩽ 5 and visible arterial occlusion or perfusion deficit within 12 h of onset are randomized to receive either tenecteplase (0.25 mg/kg) or standard of care. The primary outcome is return to baseline neurological functioning, measured by the modified Rankin scale (mRS) at 90 days. Safety outcomes include death and symptomatic hemorrhage (intra or extra-cranial). Other secondary outcomes include mRS 0–1, mRS 0–2, ordinal shift analysis of the mRS, partial, and full recanalization on follow-up computed tomography angiogram.
Conclusion:
Results of this trial will aid in determining whether there is benefit of using tenecteplase (0.25 mg/kg) in treating patients presenting with minor stroke who are at high risk of developing poor outcomes due to presence of an intracranial occlusion.
Data access statement:
Data will be available upon reasonable request.
Introduction and rationale
At least 50% of ischemic stroke is minor and initially nondisabling. 1 In the Get with the Guidelines Stroke registry in the United States, among all stroke patients presenting within 2 h of symptoms onset, 31% were not treated with thrombolytic due to specifically documented mild or improving symptoms. 2 The treatment of minor stroke with thrombolytic agent remains controversial, with much variation in practice. Most physicians do not treat all patients with minor deficits presenting within the standard thrombolytic window due to concerns that the risk of hemorrhage exceeds the potential reduction in disability with thrombolytic agents. However, a number of studies challenge the rationale for this cautious approach.
Most thrombolysis trials completed to date have included few or no minor stroke patients. However, data from a small subset of patients with minor deficits in an individual patient data meta-analysis of randomized trials of thrombolysis with intravenous alteplase suggest that thrombolytic agents improves outcome in these individuals (odds ratio (OR) = 1.48, adjusted for age and time from onset; 95% confidence interval (CI) = 1.07−2.06). 3 Within this subset of patients with minor stroke, patients with documented vessel occlusion are at the highest risk of early neurological deterioration and poor outcome when thrombolysis is withheld.4–7 Furthermore, several groups have reported that among patients considered too mild for thrombolysis, as many as a third are dead or disabled at the time of follow-up.2,5,6,8
However, randomized trials dedicated to examining thrombolysis exclusively in individuals with mild stroke have not demonstrated benefit over antiplatelet therapy. The PRISMS (The effect of Alteplase vs Aspirin on Functional Outcome for Patients with Acute Ischemic Stroke and Minor Nondisabling Neurological deficits) trial, alteplase against aspirin monotherapy, showed no significant difference in 90-day functional outcomes between the two groups and higher rates of symptomatic intracerebral hemorrhage (SICH) in the alteplase group. 9 The ARAMIS (Dual Antiplatelet Therapy vs Alteplase for Patients With Minor Nondisabling Acute Ischemic Stroke) noninferiority trial (−4.5% noninferiority margin) found that DAPT was noninferior to intravenous alteplase for excellent functional outcome at 90 days with no significant difference in the risk of SICH between the two groups. 10 Both trials used intravenous alteplase as the comparative thrombolytic agent and restricted enrollment to either 3 or 4.5 h from symptom onset. Furthermore, they did not specifically target patients with visible occlusion and/or perfusion deficit, who are the subset of individuals with minor stroke at particularly high risk for neurological deterioration. 11
Tenecteplase, a recombinant human tissue plasminogen activator similar to alteplase, has a longer half-life, is more fibrin-specific, produces less systemic depletion of circulating fibrinogen, and is more resistant to plasminogen activator inhibitor than alteplase. 12 These pharmacologic differences may potentially result in a superior safety profile and more rapid reperfusion. Recent tenecteplase trials, in particular the AcT (alteplase compared to tenecteplase) trial, 13 have shown that tenecteplase is noninferior to alteplase which has led to guideline changes, with intravenous tenecteplase (0.25 mg/kg) now recommended for use in ischemic stroke within 4.5 h of symptoms onset.14–16 The TIMELESS study 17 included patients with disabling stroke between 4.5 and 24 h from onset with potentially salvageable tissue defined by computed tomography perfusion (CTP) imaging and randomized patients to treatment with standard of care or intravenous tenecteplase. A large majority of these patients were also treated with endovascular thrombectomy. While there was no observable difference in the outcomes between groups, there was no evidence of harm when tenecteplase was given in this later time window.
The TEMPO-2 (Multicenter, prospective randomized open-label, blinded-endpoint (PROBE) controlled trial of thrombolysis with low-dose tenecteplase versus standard of care in the prevention of disability at 3 months in minor ischemic stroke with proven acute symptomatic occlusion) trial is designed to demonstrate superiority of intravenous tenecteplase (0.25 mg/kg) compared to standard of care in patients with minor stroke with visible intracranial occlusion or perfusion deficit presenting within 12 h from symptom onset, on 90-day functional outcomes assessed with the modified Rankin scale (mRS). The secondary objective of this study is to compare safety of intravenous tenecteplase with the standard of care.
Methods
The TEMPO-2 trial is a phase 3, prospective, randomized (1:1) controlled, open-label parallel group clinical trial with blinded end point assessment (PROBE design). A sample of 1274 patients with minor stroke (National Institutes of Health Stroke Scale (NIHSS) ⩽ 5) eligible for intravenous thrombolysis will be recruited to test whether intravenous tenecteplase (0.25 mg/kg body weight; maximum dose, 50 mg) is superior to standard of care (antiplatelet(s) and/or anticoagulation at the discretion of the treating physician). Given the treatment design of the trial, the time-sensitive nature of acute stroke, the nature of the investigative agent used, blinding the enrolling health personnel to treatment allocation is not practical, and therefore treatment allocation is open label.
Randomization will be 1:1 to intravenous tenecteplase (experimental) or nonthrombolytic standard of care (control). Randomization will be completed by a computer-generated minimization algorithm—minimal sufficient balance randomization to ensure balance on key variables (age, sex, baseline NIHSS score, time from onset to randomization). 18 This algorithm is developed centrally, and the details are not available to the treating sites. These are the key variables known to influence outcome in minor stroke.7,19,20 Randomization is dynamic and generated in the moment via a web-based system such that the sequence of allocation is fully masked. The system is enabled for smartphone, tablet, laptop, or desktop computer use.
Patient population
In brief, the inclusion criteria include:
Transient ischemic attack or minor stroke (NIHSS ⩽ 5) presenting within 12 h of onset or last seen well at presentation with a diagnosis of an ischemic stroke syndrome.
Direct imaging evidence of an intracranial occlusion or indirect evidence of occlusion as a perfusion abnormality relevant to the presenting symptoms.
No region of well-defined hypodensity on the NCCT (Non contrast computed tomography) consistent with the presenting symptoms or consistent with a well-evolved infarction concordant with the acute presenting syndrome.
No contraindication to intravenous thrombolysis (Supplemental Appendix 1).
The trial will recruit patients from 54 participating sites across 10 countries (Figure 1). All patients or legally authorized representative (LAR) will provide informed written consent, as approved by the relevant local Research Ethics Committee. The responsible treating physician will determine patient eligibility for the trial. This will be followed by informed consent, randomization, and treatment administration. Complete study inclusion and exclusion criteria are shown in Supplemental Appendix 2.
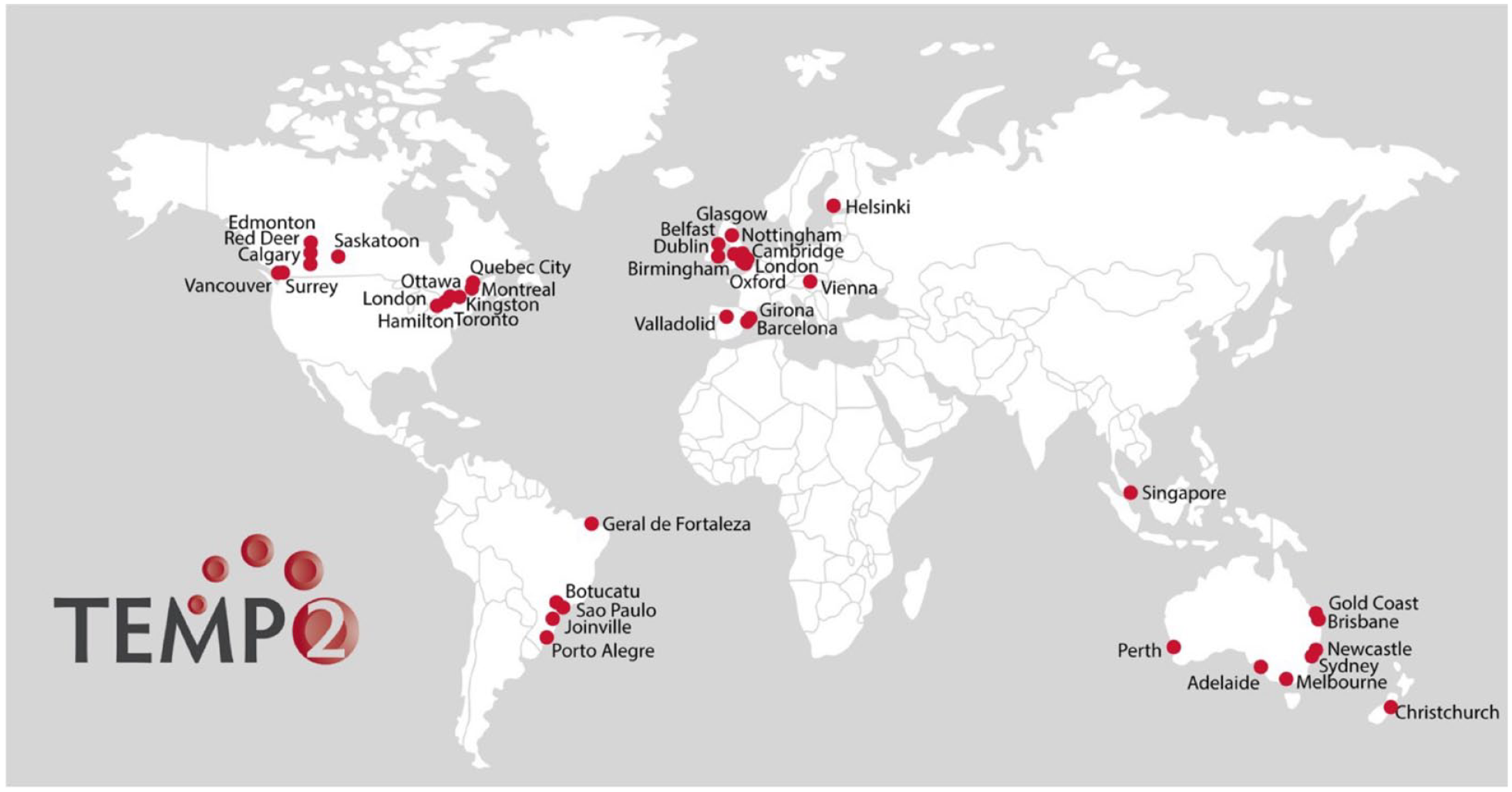
World map showing enrolling sites in TEMPO-2.
Treatment or intervention and study procedures
Experimental
Tenecteplase (0.25 mg/kg) is given as a single, intravenous bolus administered over 5–10 s immediately upon randomization.
Control
Patients will be treated with standard of care based nonthrombolytic treatment—choice at the discretion of the investigator. Per protocol, all patients will minimally receive single antiplatelet therapy. Guideline-based care is recommended. As this is a multicenter, international trial where local practices will vary, rather than mandating a specific antiplatelet agent, we will allow the local investigator to choose which antithrombotic regimen should be used. Standard of care medication(s) should be given immediately upon randomization.
All patients are expected to be provided standard stroke unit care, investigations for stroke mechanism, and stroke prevention care according to current guidelines. Patients with a demonstrated vessel occlusion at baseline will undergo a study computed tomography angiogram (CTA) of the intracranial circulation between 4 and 8 h after randomization in both arms to determine whether the occluded artery has recanalized or not. For those enrolled on the basis of CTP, a repeat CTP will not be undertaken to reduce contrast and radiation exposure. All patients will undergo routine follow-up imaging at 24 h with computed tomography (CT) or magnetic resonance imaging (MRI).
Study outcomes
Primary outcomes
The primary outcome is return to baseline neurological functioning as measured by the mRS, using a sliding dichotomy approach. A responder will be defined as follows:
If the pre-morbid mRS is 0–1, then mRS 0–1 at 90 days is a responder (good outcome).
If the pre-morbid mRS is 2, then mRS 0–2 is a responder (good outcome).
Pre-morbid mRS is assessed using the structured mRS prior to randomization (Supplemental Appendix 3). 21 Outcomes will be assessed by an individual blinded to the treatment assignment. The 90-day mRS will be rated using the structured mRS questionnaire (Supplemental Appendix 3). 21 The 90-day mRS will be completed in person where possible and by telephone otherwise. The structured questionnaire has been showed to improve reliability in assessing the mRS both in person and by telephone. 21 Secondary outcomes are listed in Supplemental Appendix 4.22–24
The main safety outcome is the proportion of patients with major bleeding: This will include an analysis of symptomatic intracranial hemorrhage (ICH) alone and then as a composite of symptomatic ICH OR major extracranial hemorrhage. Symptomatic intracranial hemorrhage is defined as new intracranial hemorrhage (includes intracerebral, subarachnoid, intraventricular, and subdural hemorrhage) associated with clinical evidence of neurological worsening, in which, the hemorrhage is judged to be the most important cause of the neurological worsening. Clinical worsening will be guided by the NIHSS score of a minimum of 2 or more points different from baseline. 25 Major extracranial hemorrhage defined as life-threatening, resulting in hemodynamic compromise or hypovolemic shock, requiring inotropic support or other means to maintain cardiac output, requiring blood transfusion of more than 2 units of packed red blood cells, or associated with a fall in hemoglobin greater than or equal to 5 g/L. Economic analysis will be conducted using Canadian hospital data and quality of life measures to estimate treatment utility.
Adverse events and safety
Adverse events will be collected through the first 5 days of trial participation. Serious adverse events (SAEs) will be collected for the full 90-day trial period. SAEs will be reviewed by the trial medical monitor. SAEs will be reported to the appropriate regulatory authority in accordance with the relevant regulations and legislation in that region and state/country. Because the adverse event profile of tenecteplase is well known due to the experience of its use for coronary thrombolysis, we do not predict that there will be unexpected adverse events.
The data safety and monitoring board (DSMB) is comprised of experts (including a biostatistician) who are independent of the study operations team and participating sites. There are safety analyses planned after 100 and 400 patients have been enrolled. A single interim analysis will occur after two-thirds (n = 850) of enrolled patients have completed 90-day follow-up. O’Brien-Fleming boundaries will be used to establish the alpha spending function for efficacy. The DSMB is entrusted with a decision to make recommendations about the continuation of the trial in the context of the data and the context of the current and known evidence about stroke treatment using their best judgment. This interim analysis will also include a futility analysis based upon conditional power.
Sample size estimates and statistical analyses
Prior literature show an effect size of 10% in the subset of minor stroke patients treated with thrombolytic agents. 3 Previous trials included in the meta-analysis of individuals with mild stroke did not require patients to have an intracranial occlusion. Many of these individuals likely did not have an intracranial occlusion. In turn, given that we expect that the effect size of thrombolysis would be higher in a population exclusively comprised of individuals with an intracranial occlusion, we conservatively estimate an overall 9% effect size. In TEMPO-1, 26 the incidence of primary outcome (mRS score = 0–1) 90 days was 66% in the combined 0.1 and 0.25 mg/kg tenecteplase-treated groups and 76% good outcome in the 0.25-mg treated group. Based on this, we estimated 60% good outcome in the control group and 69% in the tenecteplase-treated group. The sample size for each group is 614 (1228 total)—adding 4% loss to follow up and a gives a sample size estimate of 1274 patients (637 in each treatment group).
The primary efficacy population will follow the intention to treat principle and include all randomized patients. The safety population will be defined as all patients who receive any dose of tenecteplase and all patients in the control group. The per-protocol population will be defined as all patients who received any dose of study drug and met all the inclusion and exclusion criteria. It is possible that after central imaging review, some patients will be enrolled in violation of the protocol or the treatment protocol may be breached due to the dynamic nature of acute stroke. This may occur entirely in the best interests of patient care. The primary analysis will be an unadjusted comparison of proportions using Fisher’s exact test. This will be supported by a secondary analysis will use a multivariable model (generalized Poisson mixed-effects model with log link) adjusting for all the minimization variables included as co-variables. Site will be considered a random effect and not pooled. Only main effects will therefore be considered in this model. A formal Statistical Analysis Plan will be documented prior to breaking of the blind.
Study organization and funding
The Steering Committee is responsible for the development of the protocol and for the conduct and oversight of the study. The protocol was approved by the local ethics committee at all participating sites, and the trial is registered (NCT02398656). A total of 54 sites in 10 countries will be included in TEMPO-2. The Trial Management Committee runs the trial on a day-to-day basis and is based at the TEMPO-2 Trial Coordinating Centre. Funding for the trial is from grants from Heart and Stroke Foundation of Canada and Canadian Institutes of Health Research. Intravenous Tenecteplase is off-the-shelf and supported by Boehringer Ingelheim, who had no role in the trial design or conduct, data analysis, or manuscript preparation.
Discussion
The TEMPO-2 trial addresses a critical gap in the current treatment landscape for minor ischemic stroke, where controversies persist. The balance between the risk of hemorrhage and potential benefit in disability reduction is much finer with intravenous thrombolytic agents in minor stroke patients.
The PRISMS and ARAMIS trials have attempted to shed light on the use of intravenous alteplase in minor stroke, but both trials lacked specificity in patient inclusion criteria.10,27 By requiring a proven intracranial occlusion or demonstrated perfusion abnormality, the TEMPO-2 trial is enriched with a higher-risk patient group within the minor stroke population. 28 These patients are predicted to be the most likely to deteriorate if untreated and thus most likely to benefit from recanalization therapies. 11 In addition, the control group receives the current standard of care, which is dual antiplatelet therapy, while PRISMS compared alteplase with aspirin alone. 9 Notably, the trial extends the treatment window to 12 h, based on pilot data and recognizing evolving stroke pathophysiology. 29 The use of tenecteplase as a potential alternative to alteplase confers additional novelty over previous randomized trials of thrombolytics in minor stroke. The responder analysis, tailored to pre-morbid mRS, adds granularity to understand treatment effects relative to baseline functional status. Currently, there are no other ongoing trials examining this clinically relevant question.
Supplemental Material
sj-docx-1-wso-10.1177_17474930241253702 – Supplemental material for A Randomized Controlled Trial of Tenecteplase Versus Standard of Care for Minor Ischemic Stroke with Proven Occlusion (TEMPO-2): Rational and design of a multicenter, randomized open-label clinical trial
Supplemental material, sj-docx-1-wso-10.1177_17474930241253702 for A Randomized Controlled Trial of Tenecteplase Versus Standard of Care for Minor Ischemic Stroke with Proven Occlusion (TEMPO-2): Rational and design of a multicenter, randomized open-label clinical trial by Nishita Singh, Carol C Kenney, Ken S Butcher, Brian Buck, Philip A Barber, Thalia S Field, Philip M Choi, Amy YX Yu, Timothy Kleinig, Ramana Appireddy, Carlos A Molina, Keith W Muir, Michael D Hill and Shelagh B Coutts in International Journal of Stroke
Supplemental Material
sj-pdf-2-wso-10.1177_17474930241253702 – Supplemental material for A Randomized Controlled Trial of Tenecteplase Versus Standard of Care for Minor Ischemic Stroke with Proven Occlusion (TEMPO-2): Rational and design of a multicenter, randomized open-label clinical trial
Supplemental material, sj-pdf-2-wso-10.1177_17474930241253702 for A Randomized Controlled Trial of Tenecteplase Versus Standard of Care for Minor Ischemic Stroke with Proven Occlusion (TEMPO-2): Rational and design of a multicenter, randomized open-label clinical trial by Nishita Singh, Carol C Kenney, Ken S Butcher, Brian Buck, Philip A Barber, Thalia S Field, Philip M Choi, Amy YX Yu, Timothy Kleinig, Ramana Appireddy, Carlos A Molina, Keith W Muir, Michael D Hill and Shelagh B Coutts in International Journal of Stroke
Footnotes
Declaration of conflicting interests
The author(s) declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: T.S.F. was site PI for TEMPO-2 at my institution; payments from CIHR and HSFC went to my institution. Outside of the submitted work, he has received in-kind study medication from Bayer and honoraria for advisory board work with HLS Therapeutics, Bayer Canada, Roche, AstraZeneca, and Novartis. He has done expert witness work and is on the board of DESTINE Health. A.Y.Y. holds a National New Investigator Award from the Heart & Stroke Foundation of Canada. Others have none to declare.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study was supported by the Heart and Stroke Foundation of Canada, Canadian Institute for Health Research, Alberta Innovates and British Heart Foundation. Intravenous Tenecteplase is off-the-shelf and supported by Boehringer Ingelheim.
ORCID iDs
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
