Abstract
Background:
There are multiple stroke guidelines globally. To synthesize these and summarize what existing stroke guidelines recommend about the management of people with stroke, the World Stroke Organization (WSO) Guideline committee, under the auspices of the WSO, reviewed available guidelines.
Aims:
To systematically review the literature to identify stroke guidelines (excluding primary stroke prevention and subarachnoid hemorrhage) since 1 January 2011, evaluate quality (The international Appraisal of Guidelines, Research and Evaluation (AGREE II)), tabulate strong recommendations, and judge applicability according to stroke care available (minimal, essential, advanced).
Summary of review:
Searches identified 15,400 titles; 911 texts were retrieved, 200 publications scrutinized by the three subgroups (acute, secondary prevention, rehabilitation), and recommendations extracted from most recent version of relevant guidelines. For acute treatment, there were more guidelines about ischemic stroke than intracerebral hemorrhage; recommendations addressed pre-hospital, emergency, and acute hospital care. Strong recommendations were made for reperfusion therapies for acute ischemic stroke. For secondary prevention, strong recommendations included establishing etiological diagnosis; management of hypertension, weight, diabetes, lipids, and lifestyle modification; and for ischemic stroke, management of atrial fibrillation, valvular heart disease, left ventricular and atrial thrombi, patent foramen ovale, atherosclerotic extracranial large vessel disease, intracranial atherosclerotic disease, and antithrombotics in non-cardioembolic stroke. For rehabilitation, there were strong recommendations for organized stroke unit care, multidisciplinary rehabilitation, task-specific training, fitness training, and specific interventions for post-stroke impairments. Most recommendations were from high-income countries, and most did not consider comorbidity, resource implications, and implementation. Patient and public involvement was limited.
Conclusion:
The review identified a number of areas of stroke care where there was strong consensus. However, there was extensive repetition and redundancy in guideline recommendations. Future guideline groups should consider closer collaboration to improve efficiency, include more people with lived experience in the development process, consider comorbidity, and advise on implementation.
Background
The World Stroke Organization’s (WSO) mission is to reduce the global burden of stroke through prevention, treatment, and long-term care. In 2014, Lindsay et al. produced a Global Stroke Services Action plan, 1 based on recommendations from the 10 stroke guidelines which achieved scores of greater than 60% on two (Rigor and Editorial Independence) of the six domains from The international Appraisal of Guidelines, Research and Evaluation (AGREE II) tool. The authors judged the applicability of recommendations in minimal, essential, and advanced stroke services.
In 2021, the WSO Board tasked the existing Stroke Guidelines and Quality Committee (the Committee) to update the synthesis of global guidelines. The Committee included one lay member. With the approval from the WSO Board, additional co-opted members with expertise in systematic reviews and guideline production were added by open competition, balanced by gender, seniority, and location. All members provided conflict of interest statements prior to publication. No funding was provided for this work. It was agreed that the work would be published in International Journal of Stroke after peer review.
Aims
Our broad question was “What do existing stroke guidelines recommend about the management of people with stroke?” Our specific objectives are described in our PROSPERO protocol (CRD42021268434, 26 July 2022). Based on the recommendations, the group devised metrics for service audit.
Methods
Literature searches were devised and run by Joshua Cheyne, Information Specialist of Cochrane Stroke (Supplemental Appendix 1).
Participants/population
Collating guidelines, extracting data, and reviewing quality
There is no published methodology for collating recommendations from multiple guidelines. Thus, we used the same approach as Lindsay et al (2014), but evaluated all published guidelines since 2011. We drew heavily on our expertise in evidence syntheses.
We categorized guidelines into acute, and/or secondary prevention, and/or rehabilitation/life after stroke. Three subgroups were convened (rehabilitation: G.E.M., S.W., M.K., L.Y.; acute: A.A.R., G.S.S., T.S., V.C.U., D.S.L., P.N.S.; secondary prevention: L.A.S., K.W., K.H., V.K.S.) and each member was allocated approximately 15 guidelines each. Only “strong” recommendations were extracted. We relied on the evaluation of strength of recommendation by the authors of the individual guidelines; these recommendations were usually but not always supported by the highest grade of evidence. Sometimes, the individual guideline authors judged the recommendation to be “strong” and/or judged the evidence underpinning the recommendation to be of the highest grade, but if the writing group disagreed based on their knowledge of the literature, we noted these and did not include them in our recommendations. If a recommendation included the term “consider,” we retained the term “consider” as we did not wish to inadvertently change the meaning of the recommendation. We evaluated quality using the AGREE II tool (available at http://agreetrust.org) which has six domains (scope and purpose, stakeholder involvement, rigor of development, clarity of presentation, applicability, and editorial independence), 23 checklist items within these six domains; and some checklist items include multiple questions. Some guidelines were evaluated using AGREE II by only one reviewer due to the large number of guidelines.
“Strong” recommendations were collated into tables 1 to 3 and, where possible, very similar ones were combined to limit repetition. The group then judged applicability in advanced, essential, and minimal services (Box 1), acknowledging that these may vary between countries and within regions. We matched recommendations to level of service available—accepting that within the three categories we used, there is likely to be variation in specific interventions available (Box 1). If an intervention is indicated but not available, services should indicate this in patient’s records; which may help to drive forward service development.
Definition of stroke service delivery model. 1

CT: computed tomography.
A “service” may include several hospitals offering a range of stroke care.
Each group lead (G.E.M., A.A.R., L.A.S.) narratively reviewed the AGREE II forms and reported common areas of strengths and weaknesses. There is no published methodology for collating the findings of AGREE II—thus, we narratively reviewed them. These completed forms are available on request should other researchers wish to analyze the data in more detail.
Based on the recommendations, we created performance metrics for audit (Table 4). We did not use the minimal/essential/advanced categories for performance metrics because of the variation in service level within each category.
Following peer review, we removed the handful of recommendations about “what not to do.” The searches were performed in September 2021. While we could not systematically search the literature again in 2022, because this would have delayed publication of this article, we scrutinized newly published guidelines that were identified through our stakeholder consultation in November 2022. We listed the new guidelines in our reference list and checked that our recommendations were still valid. This also applied to guidelines published prior to September 2021 which had not been identified in our initial searches.
Stakeholder involvement
In November 2022, we asked the WSO Board, including Stroke Support Organisations (which have patients as core stakeholders) to comment. In December 2022, we held a meeting with people with lived experiences (PWLE) to review an updated version of the guidelines. PWLE provided feedback at the end of the meeting based on a structured interview, including the following questions: (1) Do you think these guidelines are thorough enough to capture the most relevant aspects of stroke care? (2) Are there any aspects of stroke care that these guidelines should address? (3) Please provide a short comment about potential areas of improvement. (4) Do you have any other comments?
Results
Search results are shown in Supplemental Appendix 2 and in Figure 1. Guidelines not relevant to respective subgroups are shown in Table 3 of Supplemental Appendix. From the initial 14,049 records screened from our searches, we extracted recommendations from 200 included guidelines.3–202 The great majority of guidelines were from high-income countries. Fewer than a 10th covered the entire stroke pathway. Following peer review, we included five additional references to clarify secondary prevention statements.203–207
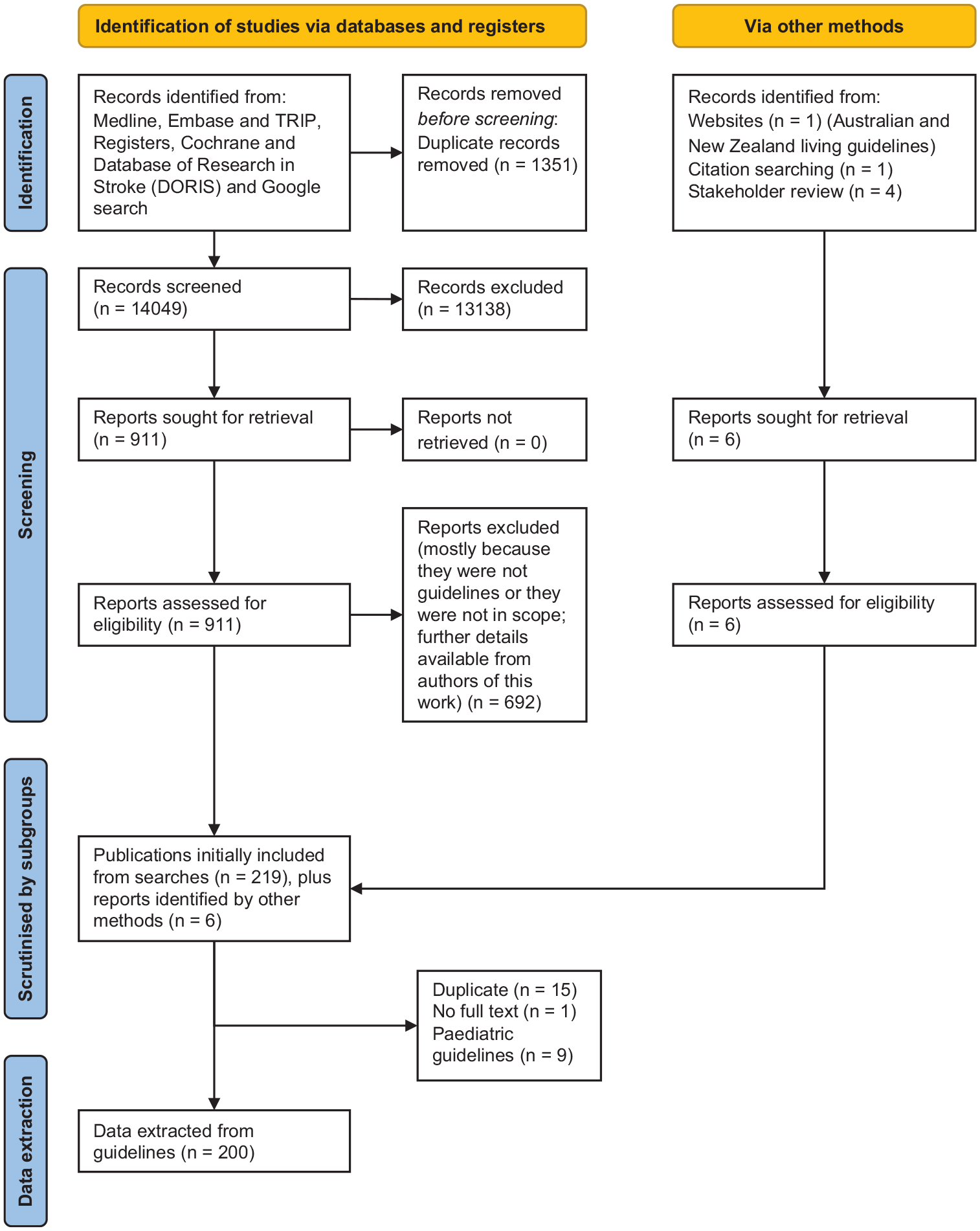
PRISMA flow diagram showing selection of guidelines.
Grading systems used
Different guideline groups used different grading systems. For instance, AHA used Classes I, II, and III, with associated levels of evidence A–C; Department of Veterans Affairs/Department of Defense (VA/DoD) used “strong/weak,” either for or against; European Stroke Organization (ESO) and Australia and New Zealand Guideline group uses strength of recommendations divided into four categories (strong or weak for or against) based PICO (patient, intervention, comparison, outcome) questions according to the GRADE approach); and Canadian guidelines used A or B or C for strength of recommendations. National Institute of Clinical Excellence (NICE) and Royal College of Physicians of London (RCPL) provide just the recommendations; in the absence of any grading, we assumed all recommendations were strong and included them.
Quality assessments by AGREE II
Our quality assessments showed that in general, the objectives, populations, questions (aspects 1–3 of AGREE II), group membership and target users were defined but the target population, preferences, and views were not so clearly described. There was a lack of patient, public and caregiver authorship of guidelines.
Very few guidelines set out to consider a priori the impact of comorbidity on recommendations, for example, interaction between treatment for hypertension and diabetes in the same person, interaction between atrial fibrillation, smoking, and diabetes; the impact of frailty and other conditions such as dementia; and how polypharmacy prior to stroke might influence treatment options. The guideline developers may have known in advance that the majority of primary research studies do not consider these interactions. Search methods and evidence selection criteria were generally well described, and strength and limitations of guidelines were satisfactory. Methods for external review were generally not well described, and most did not provide the date for a planned update.
Recommendations were generally specific and unambiguous, though the word “considered” was often used for “strong recommendations,” implying some uncertainty in the evidence. Future guidelines groups should clarify the meaning of “consider.” Management options were generally described well. Recommendations were listed either in a table (which were quick to extract) or in the text.
Facilitators and barriers to application were generally not discussed. Only some of the bigger groups provided implementation tools and advice. Resource implications were generally not discussed.
The funding body was generally recorded but some guidelines did not specifically state whether the funder had an influence on the guidelines. Competing interests were generally given for each author, but how these interests influenced the conclusions of the guidelines was not so well reported. Patient and public involvement (PPI) was limited, and stakeholder peer review was infrequently reported.
The detailed recommendations for each of the three subgroups (acute, rehabilitation, and secondary prevention) are shown in Tables 1 to 3. For acute treatment, recommendations addressed pre-hospital care, emergency care, and acute hospital care. There were more guidelines about ischemic stroke than spontaneous intracerebral hemorrhage (ICH). Strong recommendations were made for reperfusion therapies for acute ischemic stroke. For secondary prevention, strong recommendations included establishing etiological diagnosis, the management of hypertension, weight, diabetes, lipids, and lifestyle modification, and for ischemic stroke, management of atrial fibrillation, valvular heart disease, left ventricular and atrial thrombi, patent foramen ovale, atherosclerotic extracranial and intracranial disease, and antithrombotics in non-cardioembolic stroke. For ICH, strong recommendation was made for application of prothrombin complex concentrate (PCC) with addition of intravenous vitamin K over fresh frozen plasma (FFP) for reversal of vitamin-K-associated ICH, and for external ventricular drainage placement in case of intraventricular hemorrhage (IVH) and hydrocephalus that is contributing to decreased level of consciousness. For rehabilitation, there were strong recommendations for organized stroke unit care, multidisciplinary rehabilitation, task-specific training, fitness training, and specific interventions for post-stroke impairments.
Acute Management of Stroke—Recommendations, according to minimal, essential, and advance systems of care. See Box 1 for definition of levels of care.
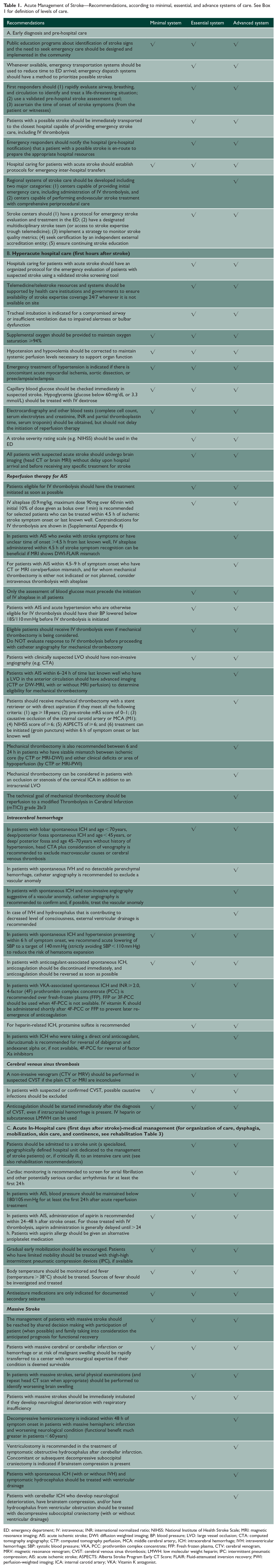
ED: emergency department; IV: intravenous; INR: international normalized ratio; NIHSS: National Institute of Health Stroke Scale; MRI: magnetic resonance imaging; AIS: acute ischemic stroke; DWI: diffusion weighted imaging; BP: blood pressure; LVO: large vessel occlusion; CTA: computed tomography angiography; CTP: computed tomography perfusion, MCA: middle cerebral artery;, ICH: intracerebral hemorrhage; IVH: intraventricular hemorrhage; SBP: systolic blood pressure; VKA, PCC: prothrombin complex concentrate; FFP: Fresh frozen plasma, CTV: cerebral venogram, MRV: magnetic resonance venogram; CVST: cerebral venous sinus thrombosis; LMWH: low molecular weight heparin; IPC: intermittent pneumatic compression; AIS: acute ischemic stroke; ASPECTS: Alberta Stroke Program Early CT Score; FLAIR: Fluid-attenuated inversion recovery; PWI: perfusion-weighted imaging; ICA: internal carotid artery; VKA: Vitamin K antagonist.
Secondary Prevention after Stroke—Recommendations.
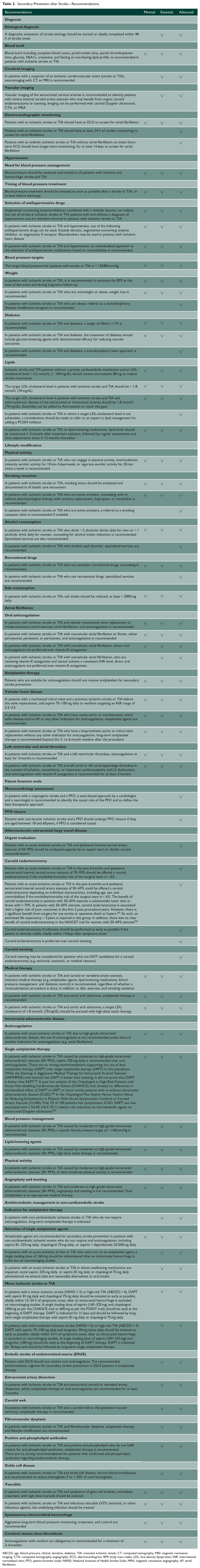
ABCD2: age, blood pressure, clinical, duration, diabetes; TIA: transient ischemic attack; CT: computed tomography; MRI: magnetic resonance imaging; CTA: computed tomography angiography; ECG: electrocardiogram; BMI: body mass index; LDL: low-density lipoprotein; INR: international normalized ratio; PFO: patent foramen ovale; NIHSS: National Institute of Health Stroke Scale; MRA: magnetic resonance angiography; AF: atrial fibrillation.
Rehabilitation after Stroke—Recommendations.
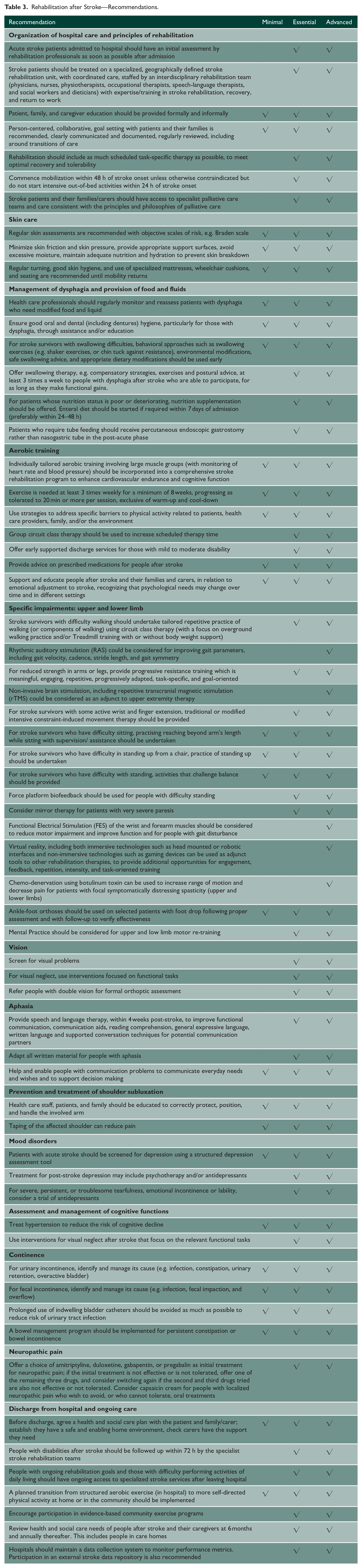
The performance metrics derivable from these recommendations are shown in Table 4.
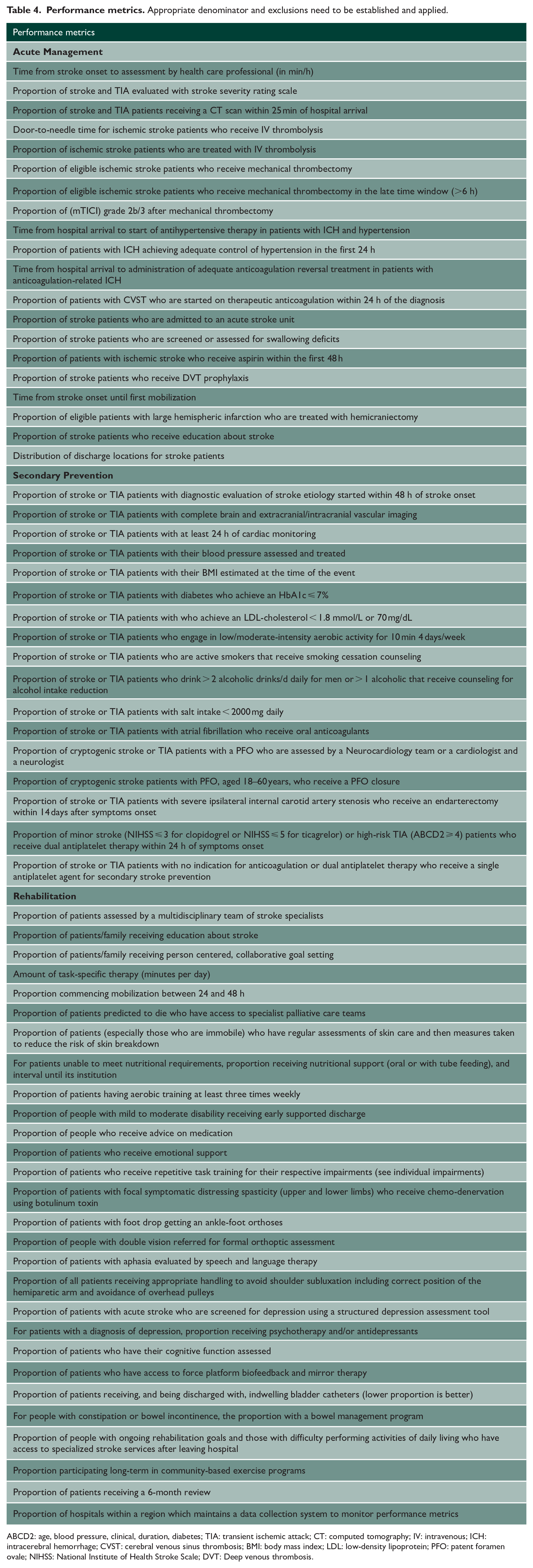
ABCD2: age, blood pressure, clinical, duration, diabetes; TIA: transient ischemic attack; CT: computed tomography; IV: intravenous; ICH: intracerebral hemorrhage; CVST: cerebral venous sinus thrombosis; BMI: body mass index; LDL: low-density lipoprotein; PFO: patent foramen ovale; NIHSS: National Institute of Health Stroke Scale; DVT: Deep venous thrombosis.
Stakeholder assessment
We received several responses from health care professional members of the WSO board in November 2022, which resulted in an updated version of the manuscript. This updated version was further reviewed by PWLE. The latter assessment determined that this document was thorough enough to address their most significant concerns. It also identified topics that were not covered in the present work because of the lack of strong recommendations in currently available guidelines (e.g. left atrial appendage for stroke prevention in patients with high-bleeding risk). PWLE also mentioned their concern about guidelines not consistently applying the same criteria for assessing the strength of recommendations, possibly resulting in disparities in stroke care across countries/regions (e.g. measuring troponin levels in the acute stroke setting). They recommended patients should be involved in the preparation of guidelines from the beginning, and guidelines should include sections with lay language for patients to understand what they mean. Clear timelines are very important for acute treatment, secondary prevention, and rehabilitation. Overall, they felt satisfied with the systematic approach and contents of the reviewed document. Comments from one more PWLE received in January 2023 were the need for single rooms in the acute phase, online support groups, and re-training for stroke survivors unable to return to their previous jobs.
Discussion
Main findings of our searches
To the best of our knowledge, this is the first systematic review and synthesis of all available stroke guidelines worldwide, published from 1 January 2011. The scope varied from specific issues to all aspects of the stroke pathway. The full list of publications we initially identified is displayed in our reference list3–202 and those excluded (e.g. because they superseded) are shown in Supplemental Appendix 3.
Main recommendations for acute stroke
Most guidelines for acute management of acute ischemic stroke were focused on acute reperfusion therapies, though some provided a more comprehensive discussion and broader management guidance. Unsurprisingly, there were more guidelines on acute ischemic stroke than on ICH, and only a couple dedicated to cerebral venous sinus thrombosis (CVST). Comprehensive acute stroke guidelines were organized into pre-hospital, emergency setting, and hospital care sections. We followed the same approach to summarize the key recommendations in this document.
Overall, the concepts of the key recommendations were consistent across guidelines. However, we noticed some disagreements regarding the evaluation of the strength of the evidence supporting those recommendations. Such disagreements may be explained by different methods used for the grading of the evidence, but in some cases, a comparison of individual discussions of some topics (e.g. extended-window intravenous thrombolysis guided by perfusion imaging) indicated differences in how strong the evidence itself was considered to be.
Important knowledge gaps persist, and they are manifested by the lack of recommendations for some practical questions.
Of note, some individual guidelines had recommendations that differed from the rest. A notable example is the lower dose of alteplase in the Japanese guidelines (0.6 mg/kg).
Main recommendations for secondary prevention
We identified 20 secondary stroke prevention topics for which there were strong recommendations, including the etiological diagnosis of ischemic stroke and TIA, lifestyle modification, management of specific risk factors, the use of antithrombotic agents for different cardioembolic sources, embolic stroke of undetermined source (ESUS), and extracranial/intracranial atherosclerotic disease, less frequent causes of ischemic stroke, and the prevention of recurrent spontaneous ICH. There were some differences between guidelines in their comprehensiveness and the strength and level of evidence assigned to specific recommendations. Strong recommendations for the secondary prevention of ICH were scarce.
Overall, the guidelines for the secondary prevention of ischemic stroke were comprehensive and covered all aspects of the continuum of care. However, there were no strong recommendations regarding some aspects of the secondary prevention of ICH because of the lack of robust evidence (e.g. specific blood pressure targets, the use of statins, and the management of antithrombotics post-ICH). Several ongoing randomized clinical trials will be concluded in the upcoming years and will likely contribute to address these knowledge gaps.
Main recommendations for rehabilitation
Rehabilitation recommendations were extracted from guidelines about one particular problem (e.g. aphasia), all of rehabilitation/life after stroke, or the entire stroke pathway. None of the rehabilitation guidelines differentiated between ICH and ischemic stroke, implying that rehabilitation needs and interventions are equally effective for both stroke types. Whether this is the case is unknown, and is an area where further research is needed.
There were strong recommendations (Table 3) for organized stroke unit care, task-specific training, strength training, aerobic training, early supported discharge, goal setting, and avoiding very early mobilization. For other interventions, there was variation in strength of recommendations, for example, the VA group did not grade antidepressants for post-stroke depression as “strong” and the NICE guidelines (UK) included strong recommendations for rehabilitation of cognitive deficits, while other guidelines did not rate this as strong. One guideline recommended psychological treatment for anxiety (as in the general population), and one recommended selective serotonin reuptake inhibitor (SSRI), but we decided not to include these as the group judged that the underpinning evidence was insufficient. The variation in strength of recommendations might have reflected differences in the grading criteria, evidence included, and interpretation of evidence.
There are no strong recommendations for dysarthria, fatigue, apathy, and neglect. The only recommendation for end-of-life care was that palliative care services should be accessed.
Quality of guidelines
The AGREE II tool demonstrated that guidelines generally did not consider resource implications or implementation. Thus, our subjective assessments of applicability had to be made based on own knowledge of resources in different health care settings. Ideally, services across the world should consider the cost-benefit of interventions based on local costs and resources available.
Strengths of our approach
We published our protocol on PROSPERO; we followed this protocol except for the exclusion of pediatric guidelines because we did not have sufficient resources to evaluate those documents. We performed comprehensive searches, we convened an international group of experts in topic areas and systematic reviews with a balance of gender, seniority, and location.
Weaknesses of our approach
To the best of our knowledge, there is no published methodology to synthesize the results of multiple guidelines. Although our approach was rigorous, some subjectivity, based on the judgment of the group members, was needed when guidelines differed in strength of recommendations for particular interventions.
There is no systematic way to our knowledge to investigate how the AGREE II tool can be used to identify which domain(s) influences recommendations. The previous WSO 2014 guidance took just two domains and selected 10 papers which had good scores in those two domains. Instead, we considered 200 publications identified in our searches. Further work is needed to develop ways to explore the influence of guideline quality on recommendations made. Researchers wishing to take this forward should contact us for access to the AGREE II assessments.
Although all the group was medically qualified and had broad range of experience from hyperacute care to rehabilitation and life after stroke, we did not have experts in other disciplines. We invited the WSO board members (which include stroke support organizations, with PWLE) to comment on our draft. We received several professional responses and lay responses. The next WSO guideline committee should seek to have more balanced professional/PWLE membership. This may require funding to enable PWLE to provide their time and expertise. Also, PWLE will be important in the dissemination stage of our work.
We did not search gray literature (i.e. literature that is not formally published in sources such as books or journal articles) or contact experts in the field to identify local/regional guidelines—due to insufficient resource. All the guidelines we reviewed were based on the same trials and systematic reviews, so it is unlikely that gray literature/regional guidelines would have come to different conclusions.
Ideally two authors would have extracted recommendations and reviewed quality for all guidelines, but this was not always feasible. It is unclear whether this would have improved the quality of our review process or changed our final recommendations.
Although we initially planned to exclude recommendation on TIA, we decided to modify the original PROSPERO protocol by including these recommendations. Reasons were that most recommendations for the prevention of ischemic stroke are also valid for TIAs and for specific recommendations, it would have resulted in reporting recommendations for stroke but not for TIA (e.g. dual antiplatelet therapy for minor stroke or TIA).
How to use this information
This is the most comprehensive systematic evaluation of all world guidelines in stroke; however, the existence of guideline recommendations is meaningless without efforts to implement them in clinical practice. Services will need to consider the cost-benefits of different interventions in their own settings. Implementation of evidence is often challenging particularly for complex interventions that require changes in service structure and processes, or interventions for which new funding is needed. It is sometimes easier when disinvestment is needed or when simple changes are needed to organization of care. The recommendations we found generally require additional resources or reorganization of care pathways, although some of the recommendations require disinvestment (e.g. avoid very early mobilization). Based on the recommendations from this review, we then developed performance metrics for services, which may be used in audits (Table 4). These are at service level, process level, or individual patient level. A review of practice in line with findings in this review should be undertaken at multiple levels: individual clinicians, hospital teams/services, and across whole health systems.
Implications for future guideline development and research
Guideline development is a resource-intensive process. Not only did we identify multiple superseded versions of guidelines, but there was duplication of work among different guideline groups, with the same trials and systematic reviews being cited in multiple guidelines. A central repository of stroke trials could be coordinated by WSO. Cochrane Stroke has maintained such a database for many years (Database of Research in Stroke (DORIS), www.askdoris.org/m), but with the disbanding of the UK Cochrane groups, DORIS will no longer be updated. However, with a modest investment, ongoing updates could be facilitated by the WSO. This will require further discussion.
Guideline groups should consider working more closely to avoid duplication such collaborative working could be coordinated by the WSO and focus on the evidence identification and data extraction stages. However, development and implementation of clinical recommendations must be contextualized for different health systems, and WSO should continue to support collaboration with guideline development groups.
To Guideline groups could also collaborate with a “living” guideline model. 208 Living clinical guidelines ensure that evidence is kept up to date, as produced by the Stroke Foundation. Where there are common topic areas, groups could collaborate in the data extraction and overall evidence summaries. An often-cited potential risk to the living guideline approach is the possibility to change a recommendation every time a new trial is published. However, the Australian experience to date suggests this is rarely a consideration, with robust methods and strong clinical expert input, including period of public consultation to ensure new evidence is taken in context including consideration of other major trials underway which may impact the overall body of evidence.
We noted that guideline developers use different methods to grade the strength of recommendations. Guideline developers could consider using a common method to establish the strength of recommendations, such as GRADE.
There were important gaps—some problems of importance to patients (e.g. fatigue) were not featured, largely due to the lack of primary research. For rehabilitation, there was an implicit assumption that the pathology of the stroke lesion is not relevant to choices about rehabilitation. Future guideline groups should define “consider.” Lay membership influences the conduct of guideline development, scope, inclusion of patient-relevant topics, outcome selection, and planned approaches to recommendation development, implementation, and dissemination with implications for both guideline developers and the guideline development process; therefore, lay members should be embedded within guideline development. 209 Also, a more robust assessment of resource implications and implementation is needed. Finally, the burden of comorbidity is increasing with population aging, and the majority of current guidelines did not specifically address the impact of comorbidity, frailty, and polypharmacy on recommendations. This needs to be addressed by researchers and guideline developers in the future to ensure that evidence is applicable to the patients we treat.
WSO guidelines committee membership
Co-chairs: Gillian E Mead and Alejandro Rabinstein
Leads of subgroups: Acute care: Alejandro Rabinstein and Gisele Sampaio Silva; Secondary prevention: Luciano Sposato and Kolawale Wahab; Rehabilitation and life after stroke: Gillian Mead and Laetitia Yperzeele
Members: Patrice Lindsay, PN Sylaja, Vijay Kumar Sharma, Gisele Sampaio Silver, Mansur Kutlubaev, Simiao Wu, Mary Kay Ballastiotes (PWLE), Kelvin Hill, Victor Urrutia, Pooja Khatri, Anil Yalaprada, David Liebeskind, Mayowa Owolabi.
Supplemental Material
sj-docx-1-wso-10.1177_17474930231156753 – Supplemental material for A systematic review and synthesis of global stroke guidelines on behalf of the World Stroke Organization
Supplemental material, sj-docx-1-wso-10.1177_17474930231156753 for A systematic review and synthesis of global stroke guidelines on behalf of the World Stroke Organization by Gillian E Mead, Luciano A Sposato, Gisele Sampaio Silva, Laetitia Yperzeele, Simiao Wu, Mansur Kutlubaev, Joshua Cheyne, Kolawole Wahab, Victor C Urrutia, Vijay K Sharma, PN Sylaja, Kelvin Hill, Thorsten Steiner, David S Liebeskind and Alejandro A Rabinstein in International Journal of Stroke
Footnotes
Acknowledgements
The authors are very grateful to Maureen Harding and Sharon Moncrieff (University of Edinburgh) for retrieving references and adding them to Covidence. Gergana Ralencova provided administrative support. The authors are very grateful to the WSO Board for providing regular feedback through Board meetings during the course of our work.
The following people (stakeholders) provided comments on the draft manuscript:
Mirjam R Heldner, Assoc. Prof., MD, Swiss Certificates of Neurology (FMH), Cerebrovascular diseases/neurosonography and EEG (SSCN)
Caleb Ademola Omuwa Gbiri. PT, PhD, FWSO, Neurophysiotherapist, Forensic Neurophysiotherapist, Neuroscientist and Clinical Ethics Philosopher.
Dr Candice Delcourt, MD, PhD, FRACP, Program Lead, Neurological Program, Clinical Associate Professor, Department of Clinical Medicine, Faculty of Medicine, Health and Human Sciences, Macquarie University, Conjoint Senior Lecturer, Faculty of Medicine, The University of New South Wales, Medical Fellow, Medical and Regulatory Services, George Clinical
Prof Timothy Kleinig PhD FRACP MBBS (Hons) BA, Head, Stroke Unit, Department of Neurology, Royal Adelaide Hospital, Department of Medicine, University of Adelaide
Cheryl Bushnell, MD, MHS, Professor of Neurology, Vice Chair of Research, Stroke Division Chief, Department of Neurology, Medical Center Blvd, Winston Salem, NC 27157
Isabelle Simler (PWLE)
Susan Wyatt (PWLE)
Nadica Shikoska (PWLE)
Kirk Patterson (PWLE)
Prof. Anita Arsovska, MD, PhD, FESO, University Clinic of Neurology, University “Ss Cyril and Methodius,” Faculty of Medicine-Skopje, Bul. Majka Tereza 17, 1000 Skopje, Republic of N. Macedonia, Macedonian Stroke Association President, SAFE Vice President, World Stroke Academy Associate Commissioning Editor
Mari Ramsey from Lawson Health research Institute
Declaration of conflicting interests
The author(s) declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: Mansur Kutlubaev, Honoraria for lectures from Pfizer, Abbot Laboratories, Merz. Supported by the Bashkir State Medical University Strategic Academic Leadership Program (PRIORITY-2030). Thorsten Steiner, honoraria for lectures from Bayer, Boehringer, Pfizer, Daiichy, Astra; participation in data monitoring committee or advisory board: Boehringer; leadership role in ESO and WSO. Alejandro Rabinstein, grant for investigator initiated project from Chiesi; CEC committee for Boston Scientific, Advisory boards for Astra Zeneca, Novo Nordisk, Shionogi, Brainomix; leadership role for Life Source (unpaid). Luciano A Sposato, Kathleen and Dr. Henry Barnett Chair in Stroke Research (Western University) Saraydar Neurosciences Fund (Western University); Honoraria from Pfizer Boehringer Ingelheim Gore. Victor C Urrutia, Research grant from Genentech, Inc. Gillian E Mead, honoraria from Imperative Care, Royalties from Elsevier for a book on exercise training after stroke, co-leads Cochrane Stroke which hosts DORIS, President of British and Irish Association of Stroke Physicians. Gisele Sampaio Silva, Medication donation for the Resilient Extend IV trial - to her Institution from Boehringer Ingelheim; personal payment for consulting from Boehringer Ingelheim; honoraria/lectures-personal payment from Boehringer Ingelheim Astra Zeneca and Pfizer; Advisory Board: personal payment from Astra Zeneca. Kolawale Wahab, funding for the Development of Algorithm for management of hypertension in Nigeria and Development of a Training Manual for the treatment of hypertension in Nigeria from Sanofi Pharmaceuticals; Secretary-General, Nigerian Hypertension Society. Laetitia Yperzeele, World Stroke Organisation: Future Stroke Leaders Program funded project on the needs of Young People with Stroke 20.000 USD; Vives Hogeschool and UCLL Genk: Payment for lectures in the course for stroke nurses (payment to her organization, not personal account; World Stroke Organisation: Attendance of WSC 2022 Singapore. Member of the Scientific Board of the Belgian Stroke Council-no funding received. The other authors do not have conflicts of interest.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
ORCID iDs
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
