Abstract
Background:
Dysmenorrhea is one of the most common gynecological complaints among adolescent women. It has been associated with short-term absenteeism in school and has a negative impact on academic and daily activities. Therefore, the aim of the study was to show the evidence on the magnitude and correlates of dysmenorrhea in Ethiopia.
Method:
In this systematic review and meta-analysis, we searched the literature from different databases such as PubMed/Medline, Science Direct, PsycINFO, and Cochrane library. We also used unpublished literature from Google, Google Scholar. The quality of the included articles was assessed using the Newcastle-Ottawa Scale. Data were extracted using a Microsoft Excel data extraction format. STATA version 14 statistical software was used for data analysis. To assess the heterogeneity of the primary articles, the Cochrane Q test statistics and the I2 test were carried out. Publication bias was inspected by funnel plot, and Egger’s test was performed to confirm the presence of publication bias. A random-effects meta-analysis was used to estimate the pooled prevalence of dysmenorrhea and its associated factors.
Result:
A total of 12 studies were included in the final meta-analysis. The pooled prevalence estimate of dysmenorrhea among female students in Ethiopia is 71.69% (66.82%–76.56%). In our systematic review, among factors associated with dysmenorrhea, the family history of dysmenorrhea was frequently reported in included studies. Therefore, dysmenorrhea was significantly associated with a family history of dysmenorrhea (adjusted odds ratio = 4.69 (95% confidence interval: 2.80–7.85)).
Conclusion:
The pooled prevalence estimate of dysmenorrhea among students was much higher in Ethiopia. Health professionals and teachers should educate and support students to follow their menstrual cycle regularly in the event of irregular periods. There should be an awareness of the negative consequences of dysmenorrhea to reduce the physical and psychological stresses that affect women and their families.
Introduction
Dysmenorrhea refers to severe painful menstrual cramps in the lower abdomen. Commonly reported manifestations are sweating, loss of appetite, tachycardia, dizziness, headache, vomiting, and diarrhea just before the onset of menses.1,2 It can be primary, in the absence of identifiable pelvic pathologies, or secondary, with demonstrable organic pathologies like endometriosis and pelvic inflammatory disease.2,3 Dysmenorrhea is the most commonly reported gynecological complaint among women and occurs in 60%–93% of school girls from the studies conducted among women with different age groups and by using different assessment tools.1,3–7 Most women experience a certain degree of pain and distress during their menstruation. 8
Previous studies reported a different prevalence rate of dysmenorrhea. For example, epidemiological studies conducted in different countries have estimated that the prevalence of dysmenorrhea ranged between 43% and 91% among school girls.3,9 Dysmenorrhea is one of the leading causes of women’s health burden in the world.10,11 The result of the study showed that approximately more than 140 million hours are lost annually from school or work as a result of painful abdominal cramps. 12 It is the leading cause of recurrent work and absenteeism in school among young girls.10,13
Although dysmenorrhea is a common complaint among adolescent girls, it affects women of all reproductive ages and has a major impact on quality of life, work productivity, and healthcare utilization. 14 Approximately 10%–15% of women experience severe menstrual pain, which leads to stop of normal daily functions at work, home, or school. 15 Generally, dysmenorrhea has a negative impact on social, academic, and even psychological aspects of life among large numbers of female adolescents;16,17 suggesting that failure to address dysmenorrhea causes a major social and financial burden for families, neighbors, communities, and the globe at large. It causes a greater burden of disease, particularly in resource-limited settings such as Ethiopia.18,19
Although different pharmacological and non-pharmacological treatment approaches, such as taking nonsteroidal anti-inflammatory drugs (NSAIDS), dietary therapies, meditation, and acupuncture, have been used to reduce the effects of dysmenorrhea, 20 it causes great consequence among students. Younger age, early menarche, prolonged or aberrant menstrual flow, family history of dysmenorrhea, psychological disturbance, genetic influence, and history of sexual abuse are some of the reported factors associated with dysmenorrhea.6,21
Previous studies conducted to assess the prevalence and associated factors of dysmenorrhea among students in Ethiopia reported different findings ranging from 58.5% to 85.4%. Therefore, the aim of this systematic review and meta-analysis was to estimate the pooled prevalence and identify factors associated with dysmenorrhea among students in Ethiopia, and to our knowledge, this is the first study on systematic review and meta-analysis in our country. The result of this systematic review and meta-analysis will help policymakers and other concerned bodies to show appropriate strategies for early identification and intervention of dysmenorrhea and psychosocial-related problems among students.
Methods
Search strategy
We used the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) guideline to conduct this systematic review and meta-analysis. 22 We searched for articles using the following databases: PubMed/MEDLINE, PsycINFO, Google Scholar, AJOL, and Cochrane library. We have also searched for literature from websites that index Ethiopian journals and World Health Organization (WHO) reports. The search for these articles was carried out from 1 January 2020 to 30 March 2020. The key terms used to search for primary studies were prevalence OR magnitude OR incidence OR epidemiology) AND (associated factors OR correlates OR determinants OR risk factors) AND (dysmenorrhea OR menstrual cramp OR menstrual problem) AND (students OR adolescents OR females OR women) AND (Ethiopia). Data were extracted from articles, and we tried obtaining missing information from the primary author through email. Searching was performed from September 2019 to 30 March 2020, and studies are evaluated for their eligibility to be included in the meta-analysis using prepared eligibility assessment criteria.
Inclusion criteria
Exclusion criteria
Studies that were not fully accessed were excluded from the study because we were unable to assess the quality of each article in the absence of full texts. Reviews, editorials, letters to editors, short communications, conference presentations, and commentaries were excluded from the review.
Data extraction
Two authors (A.M. and B.M.) independently extracted all the necessary information from the articles using a standardized data extraction form. The extraction form included the following information: name of the first author, region of the country where the study was conducted, publication year, sample size included, response rate, and prevalence of dysmenorrhea. For the second objective (factors associated with dysmenorrhea), the data extraction format was prepared in the form of a two-by-two table. Contrasting results between the two authors during data extraction were solved through communication with other authors and by re-extracting the data together.
Outcome measurements
This review has two main objectives. The first objective was to determine the estimated pooled prevalence of dysmenorrhea among students in Ethiopia. The second objective was to estimate the pooled effects of factors associated with dysmenorrhea among students in Ethiopian. The pooled prevalence of dysmenorrhea was calculated by dividing the number of patients presented with dysmenorrhea to the total number of patients who have been included in the study and multiplied by hundred (100). For the second objective, odds ratio was used to measure the level of the association between dysmenorrhea and its predictor. The odds ratio was calculated from primary studies using two-by-two tables.
Quality assessment
The quality of the included articles was assessed using the Newcastle-Ottawa Scale (NOS). 23 This quality assessment tool has the following components: the methodological quality of the study, comparability of included studies, and quality of original articles with respect to statistical analysis. All authors independently evaluated the quality of the original articles using NOS. The tool has a total of 10 scores, and articles with medium and high quality (score of 6 and above) were included in this review. Any discrepancies between authors during the quality assessment of the included studies were solved by taking the average of each author.
Statistical procedure
The data were analyzed using STATA Version 14.0. The characteristics of the original studies were described using tables and a forest plot. The heterogeneity between the primary studies was checked using χ2 test and the I2 test. 24 These statistical tests showed that there was significant heterogeneity between primary studies, as evidenced by I2 = 94.2%, p value <0.001. We used a random-effects meta-analysis model to estimate the Der Simonian and Laird pooled effect of dysmenorrhea. Furthermore, we also employed a leave-one-out sensitivity analysis to identify the possible source of heterogeneity in the pooled meta-analysis of the prevalence of dysmenorrhea students in Ethiopia. Publication bias was also checked by performing Egger’s correlation and Begg’s regression intercept tests at a 5% significant level, respectively.25,26
Results
Search results
A total of 192 primary articles were retrieved during the literature search of Medline/PubMed, Google Scholar, AJOL, Cochrane Library, and Google Scholar. About 83 articles were excluded due to duplication and 75 studies were excluded after reviewing their titles and abstracts, since they were not conducted in Ethiopia. Then, we further evaluated 34 full-text articles. Of the 34 full-text articles, 22 articles are excluded due to their quality assessment result and not being conducted on students. Finally, 12 studies were included in meta-analysis (Figure 1).

Flow chart explaining the selection of primary studies for the systematic review and meta-analysis of the prevalence of dysmenorrhea among adolescents in Ethiopian, 2020.
Characteristics of the primary articles included
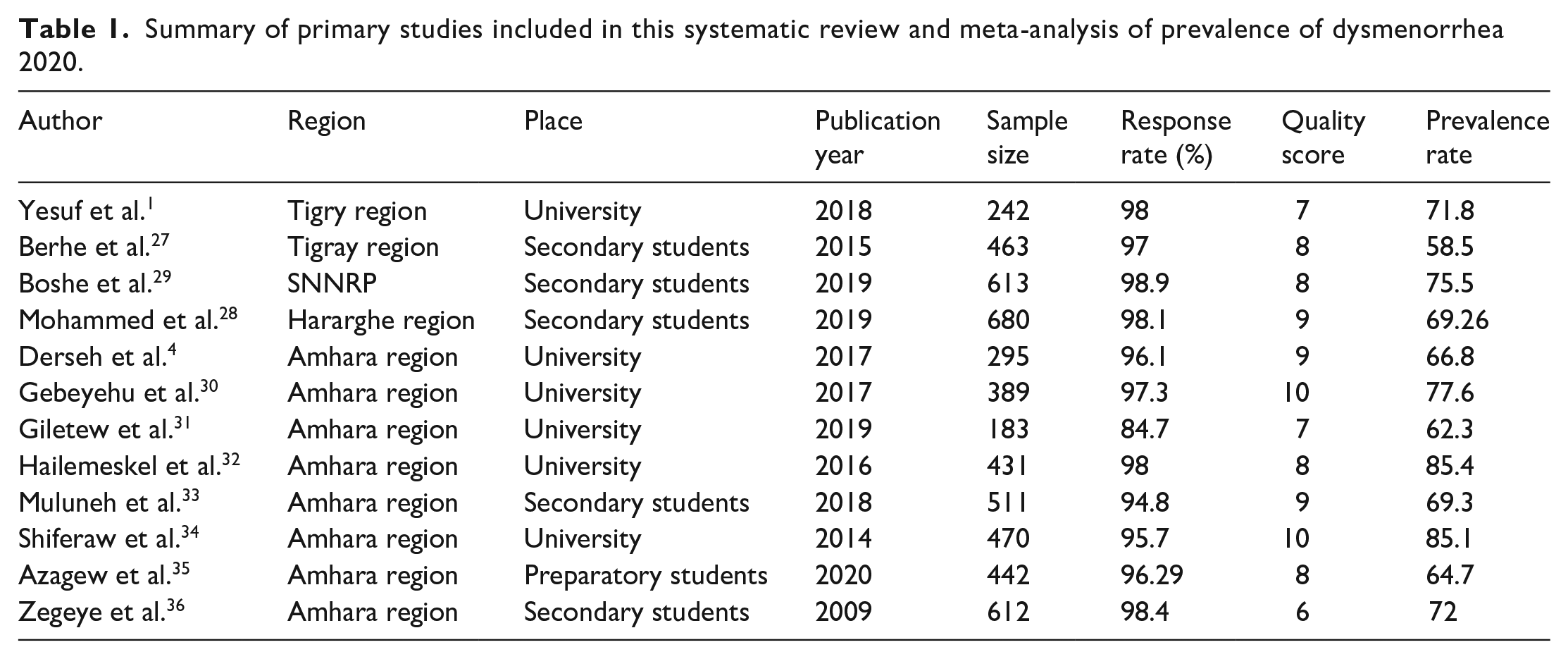
Table 1 shows the summary characteristics of the included studies. Studies were carried out from 2009 to 2020. Among the studies included in the Systematic Review and Meta-analyis (SRMA), two studies were from the Tigry region,1,27 one study from Hararghe 28 and a single study from southern nationalities and regions of peoples (SNNRP). 29 The majority of studies (eight) were conducted in the Amhara region.4,30–36 All studies included in this review were observational with sample size ranging from 183 to 680 participants as reported from studies carried out in Amhara 31 and Hararghe, 28 respectively (Table 1).
Summary of primary studies included in this systematic review and meta-analysis of prevalence of dysmenorrhea 2020.
Meta-analysis
Prevalence of dysmenorrhea among students
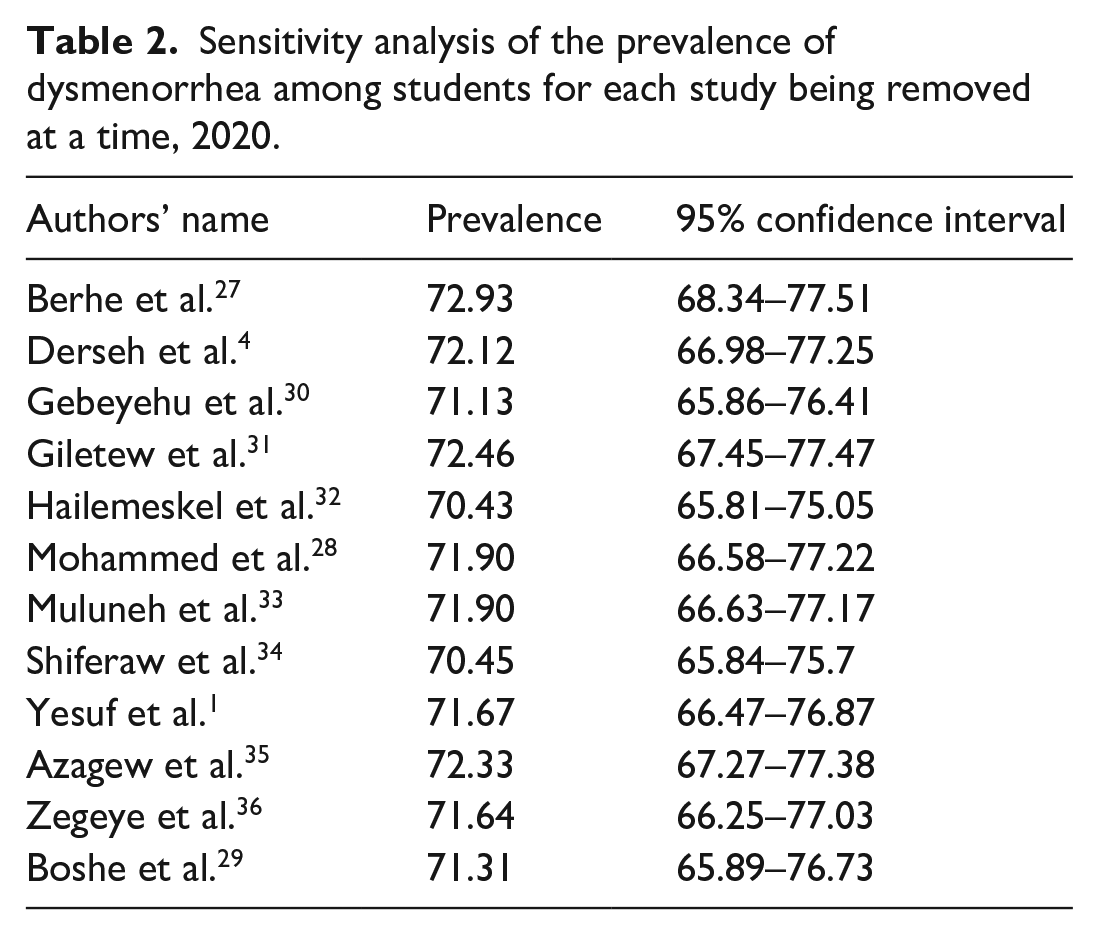
The highest and lowest prevalence of dysmenorrhea were reported from independent studies conducted at Debre Tabor University in the Amhara region 32 and in the Tigray region among secondary school students. 27 This systematic review meta-analysis showed that the pooled prevalence estimate of dysmenorrhea among students in Ethiopia was 71.69 %: 95% confidence interval (CI) = 66.82–76.56 (Figure 2). Significant heterogeneity was reported (I2 = 94.2% and p < 0.001); as a result, a random-effects model was conducted to estimate the pooled prevalence of dysmenorrhea among school-age students. Subgroup analysis by region was performed and higher prevalence was found among studies conducted in the Amhara region: 73.13 with 95% CI = 66.92–79.33 (Figure 3). We also performed a leave-one-out sensitivity analysis to identify the possible source of heterogeneity in the pooled meta-analysis of the prevalence of dysmenorrhea among students in Ethiopia. Therefore, the pooled prevalence of dysmenorrhea among students ranged between 70.43% (65.81–75.05) and 72.93% (68.34–77.51) in a leave-one-out sensitivity analysis (Table 2).

Forest plot for the pooled prevalence of dysmenorrhea among students in Ethiopia, 2020.

The results of subgroup analysis by region on dysmenorrhea among students in Ethiopia, 2020.
Sensitivity analysis of the prevalence of dysmenorrhea among students for each study being removed at a time, 2020.
Publication bias
We found publication bias in included studies (Egger’s test, p = 0.038, as well as asymmetric funnel plot). As a result, a Duval and Tweedie trim-and-fill analysis was applied to recalculate the pooled effect size after removing a single study which introduced publication bias. 37 Finally, the pooled prevalence of current is almost similar to previous, but we observed the absence of publication bias in this case as evidenced by Egger’s test (p = 0.07). Publication bias was also inspected using a funnel plot, and there is no evidence to confirm publication bias (Figure 4).

Funnel plot showing symmetric distribution of articles of dysmenorrhea among students in Ethiopia, 2020.
Predictors of dysmenorrhea among students in Ethiopia
There are many factors associated with dysmenorrhea among students in primary studies, but variables reported as a significant predictor of dysmenorrhea in at least three primary studies were included in this meta-analysis. As a result, a family history of dysmenorrhea, age at onset of menarche, and menstrual regularity were variables frequently reported in the included studies.
Family history of dysmenorrhea
Eight of 12 included studies showed that a family history of dysmenorrhea was a strong predictor of dysmenorrhea among students in Ethiopia.4,28,30,32–35 A total of 3218 samples were included to analyze the association of family history and dysmenorrhea among students in Ethiopia. The pooled estimated odds ratios showed that participants with a family history of dysmenorrhea were 4.69 times more likely to have dysmenorrhea compared to their counterparts (adjsusted odds ratio (AOR) = 4.69 (95% CI: 2.80–7.85)) (Figure 5).

Association of family history with dysmenorrhea among students in Ethiopia, 2020.
Age at onset of Menarche
Three of the included studies reported that the early onset of menarche was strongly associated with dysmenorrhea among students in Ethiopia.27,28,33 The odds of having dysmenorrhea were 2.7 times higher among students with a history of early menstrual onset before age 12, but the CI showed an absence of statistical association between age at the onset of menstruation and dysmenorrhea (AOR = 2.7, (95% CI 0.63–11.64)) (Figure 6).

Association of age at onset of menstruation with dysmenorrhea among students in Ethiopia, 2020.
Menstrual irregularity
Another frequently reported factor was menstrual irregularity,34–36 but there is no scientifically significant association between menstrual irregularity and dysmenorrhea (AOR = 1.33, (95% CI: 0.66–2.73)) (Figure 7).

Association of menstrual irregularity with dysmenorrhea among students in Ethiopia, 2020.
Discussion
Dysmenorrhea is a common problem among women of reproductive ages and is also very common among adolescents of school age. There is a wide variation in the prevalence of dysmenorrhea in different studies around the world.38–40 Different independent studies conducted in our country also showed various estimates of dysmenorrhea among students, ranging from 58.5% to 85.5%. 27 Although there are different primary studies conducted on the prevalence of dysmenorrhea among students, there is no summarized evidence on the problem. The current review aimed to show the pooled prevalence of dysmenorrhea and to identify its associated factors among students in Ethiopia. According to the knowledge of the authors, this is the first systematic review and meta-analysis in the country.
The result of this systematic review and meta-analysis showed that there is a high magnitude of dysmenorrhea among students in Ethiopia (71.69; 95% CI: 66.82–76.56). The finding of this review was consistent with a review study conducted in Iran where the prevalence of dysmenorrhea among students was reported as 73.27%, 41 another systematic review study conducted among university students in different countries (71.1%), 42 and a study conducted in Turkey (72.7%). 43 It was also similar to others studies conducted in Iran 71% 44 and India 75%. 45 However, the pooled prevalence of dysmenorrhea in this study was higher than the studies conducted in Saudi Arabia (61%), 46 Jordan (56%), 47 Canada 20%, 48 and the review study conducted among students in Iran in which 18% of the students had secondary dysmenorrhea. 44 It was also higher than another review study conducted on menstrual disorder in a developing country (5%–20%). 49 whereas the finding of the current study was lower than previous studies conducted in Oman (94%) 50 and Australia (80%). 51
The possible explanation for these highly discrepant reports of dysmenorrhea could be due to the different definitions of dysmenorrhea between primary and secondary dysmenorrhea and the scales used to determine dysmenorrhea.17,46,52,53 Most of the studies included in our study are conducted on primary dysmenorrhea, in fact resulting in a greater variation compared to other studies that included secondary dysmenorrhea. In fact, secondary dysmenorrhea is rare among adolescents. Another reason for variation might be the difference in study subjects; we included secondary school students along with university students; but in the rest of the studies focused on university students, we expect, most of the time, that the age of onset of menarche is commonly among secondary students and is more stressful and might lead to manifest the symptoms of dysmenorrhea. The assessment tool variations could be another possible reason for the differences, in which studies conducted in Ethiopia used culturally adapted tools, and difference in the timing of the study period (night) also has an effect on the differences in dysmenorrhea in our study and previously conducted studies. Sociocultural differences could be another possible reason for this discrepancy, as studies have shown that dysmenorrhea is more prevalent in stressful situations. 54 The stressful situations among school-age students are also common in developing countries, including Ethiopia. Most of the students in developing countries also did not seek medical advice, despite the high prevalence of dysmenorrhea leading to absenteeism in school and other functional impairments. 44
Regarding factors associated with dysmenorrhea among students, the family history of dysmenorrhea was strongly associated with dysmenorrhea among students in Ethiopia. Students with a family history of dysmenorrhea were 4.69 times more likely to have dysmenorrhea compared to their counterparts. This is supported by the studies conducted in Iran, 55 Turkey, 56 Australia, 14 and Serbia. 57 The possible reason could be that daughters of mothers with dysmenorrhea might experience the same behaviors from their mothers, 58 and evidently, family history is basically associated with gynecological problems. Studies showed that apart from genetic factors involved in the pathogenesis of dysmenorrhea, 59 learned behaviors are also important indicators to share similar symptoms of dysmenorrhea among family members.60,61
Limitation of the study
The limitations of this study are that only full-text articles were included; conference presentation and commentaries were excluded due to quality assessment. The presence of probable publication bias could be another limitation of this systematic review and meta-analysis.
Conclusion
This review revealed that the pooled prevalence of dysmenorrhea was high in Ethiopia and the family history of dysmenorrhea was also a strongly associated factor among students in this review and meta-analysis. Health professionals and teachers should educate and support students to follow their menstrual cycle regularly in the event of irregular periods. Awareness of the negative consequences of dysmenorrhea should be given to reduce the physical and psychological stresses that affect women and their families. The result of this systematic review and meta-analysis will help policymakers and other concerned bodies to show appropriate strategies for early identification and intervention of dysmenorrhea and related psychosocial problems among students.
Footnotes
Acknowledgements
We acknowledge the authors and participants of the original included studies.
Author contribution(s)
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Availability of data and materials
Data will be available upon reasonable request from the corresponding author (
