Abstract
Background:
Within the UK, there is a goal that research is embedded into everyday healthcare practice. Currently education provided to students at pre-registration level is theoretical, with little focus on clinical research delivery.
Aims:
The paper’s aim is to report on the development and evaluation of a pre-registration clinical research resource for nursing and midwifery students with direct application to clinical settings and patient care outcomes.
Methods:
An initial survey assessed whether the learning resource was useful for nursing pre-registration students. Based on the findings, alongside expert stakeholder input, adaptations were made to the learning resources and a second survey re-evaluated the learning resources. Survey findings were analysed using descriptive statistics. Free text responses were thematically grouped.
Results:
Ninety-seven pre-registration nursing students responded. Most students agreed that they had enjoyed using the resources, had improved understanding of clinical research, anticipated being actively involved in research and would consider a future clinical research role.
Conclusions:
The learning resources can help overcome barriers to research engagement by nurses and midwives. The results demonstrate that research can be incorporated into clinical, educational and academic roles, highlighting their worth in supporting the clinical research workforce.
Keywords
Introduction
Globally, the World Health Organization (WHO) (WHO, 2020) identified that nurse education needs to emphasise and facilitate the development of ‘critical thinking skills’ to enable nurses to utilise advanced skills in clinical judgement; this can lead to improvements in patient safety. A recent WHO strategy document (WHO, 2021) emphasised that nurse graduates should meet or surpass health system demand and possess the requisite knowledge, competencies, and attitudes to meet national and international health priorities. For this to occur, pre-registration nurses and midwives need exposure to research so they can embed their critical thinking skills within their nursing and midwifery roles. Research career opportunities can tackle widespread recruitment and retention issues within nursing and midwifery through developing new and varied career progression pathways (Richardson et al., 2019).
In the United Kingdom (UK), the National Institute of Health and Care Research’s (NIHR) vision is to improve the health and wealth of the nation through embedding clinical research into everyday healthcare practice. This requires a research positive culture where all staff feel well equipped to support and participate in clinical research as part of day-to-day healthcare practice (Department of Health and Social Care (DHSC), 2021). The importance of a workforce who can think critically, apply up-to-date and relevant knowledge, and provide expert, evidence-based care is recognised by the UK Nursing and Midwifery Council’s (NMC) (2018a) proficiency standards for registered nurses and midwives. Recently, the Chief Nursing Officer for England’s National Health Service (NHS) stated that all nurses have a role to play in supporting, leading and delivering research and emphasised the role of research at the centre of nurses’ professional practice and integral to the delivery of high-quality patient care (National Health Service for England (NHSE), 2021).
Background/literature
Research capacity building and career planning for healthcare professionals to be research-trained and research-active is required at all career levels and stages (Carrick-Sen et al., 2019; NIHR, 2016), but should begin with pre-registration students (Council of Deans of Health, 2019). Pre-registration nurses and midwives need opportunities to practise their research knowledge and experience change and innovation in practice (Brooke et al., 2015). Pre-registration nursing and midwifery students who engage with research early can develop a comprehensive understanding of the role of research in assessing, evaluating and improving practice (Council of Deans of Health, 2019). However, much research education provided to students at pre-registration level is theoretical, with a heavy methodological focus and little applied understanding of how research works in real-life clinical settings (Menzies et al., 2021; Twycross and Shorten, 2014). Higher Education Institutions (HEIs) are required to provide a programme of education that includes preparing pre-registration nurses and midwives to understand and engage in research (Menzies et al., 2022). This usually involves research informed teaching, teaching on evidence-based practice modules and running compulsory research methods modules (Council of Deans of Health, 2019). Pre-registration nursing feedback on the teaching of research identified that students enjoyed learning about research, saw its relevance to their pre-registration programmes and understood the link between research and practice (Feeney, 2019). However, they highlighted that they would benefit from more opportunities for experiential learning about research (Feeney, 2019).
Despite an ever-increasing need for clinical research nurses and midwives across healthcare systems, career pathways in clinical research are rarely promoted by HEIs (Brand et al., 2022). This means many nursing and midwifery students have little understanding of what these roles involve (Capilli et al., 2022). Nursing and midwifery graduates who do have experience in conducting research are more likely to undertake further study and potentially embark on research roles throughout their careers (Menzies et al., 2021).
As a result of the challenges, the NIHR Clinical Research Network (CRN) identified a need to raise the profile of clinical research careers amongst pre-registration nursing students. As a result, in 2019 the CRN and other senior nursing colleagues developed a set of clinical research nursing resources for pre-registration nursing students which were piloted by members of the NIHR Workforce Learning and Organisational Development team with expert working groups. These resources were adopted by the NIHR Senior Nurse and Midwife Research Leader (SNMRL) programme (Henshall et al., 2020) and representatives from the NIHR Nursing and Midwifery Office and the NIHR Nursing and Midwifery Incubator (NIHR, 2022), with the intention of updating and piloting them with nursing students in HEIs and NHS organisations.
The overall aim of the paper is to report on the development and evaluation of these pre-registration clinical research resources for nursing and midwifery students to develop flexible, interactive teaching and learning materials with direct application to clinical settings and patient care outcomes.
The objectives included to:
increase pre-registration students’ awareness and understanding of clinical research delivery
develop learning resources for use in a wide variety of ways to support nursing and midwifery students’ learning experiences, styles and preferences
Methods
Study design
This quantitatively designed, longitudinal service evaluation involved the development of a co-produced learning resource that was evaluated at two separate time-points using online surveys (Figure 1). It was conducted between November 2020 and November 2022. From the 10 HEIs and NHS organisations who were contacted through networks stemming from the core working group, it led to participation from 4 HEIs and 1 NHS in both Phases I and 2, however the actual institutions taking part did vary in the phases.
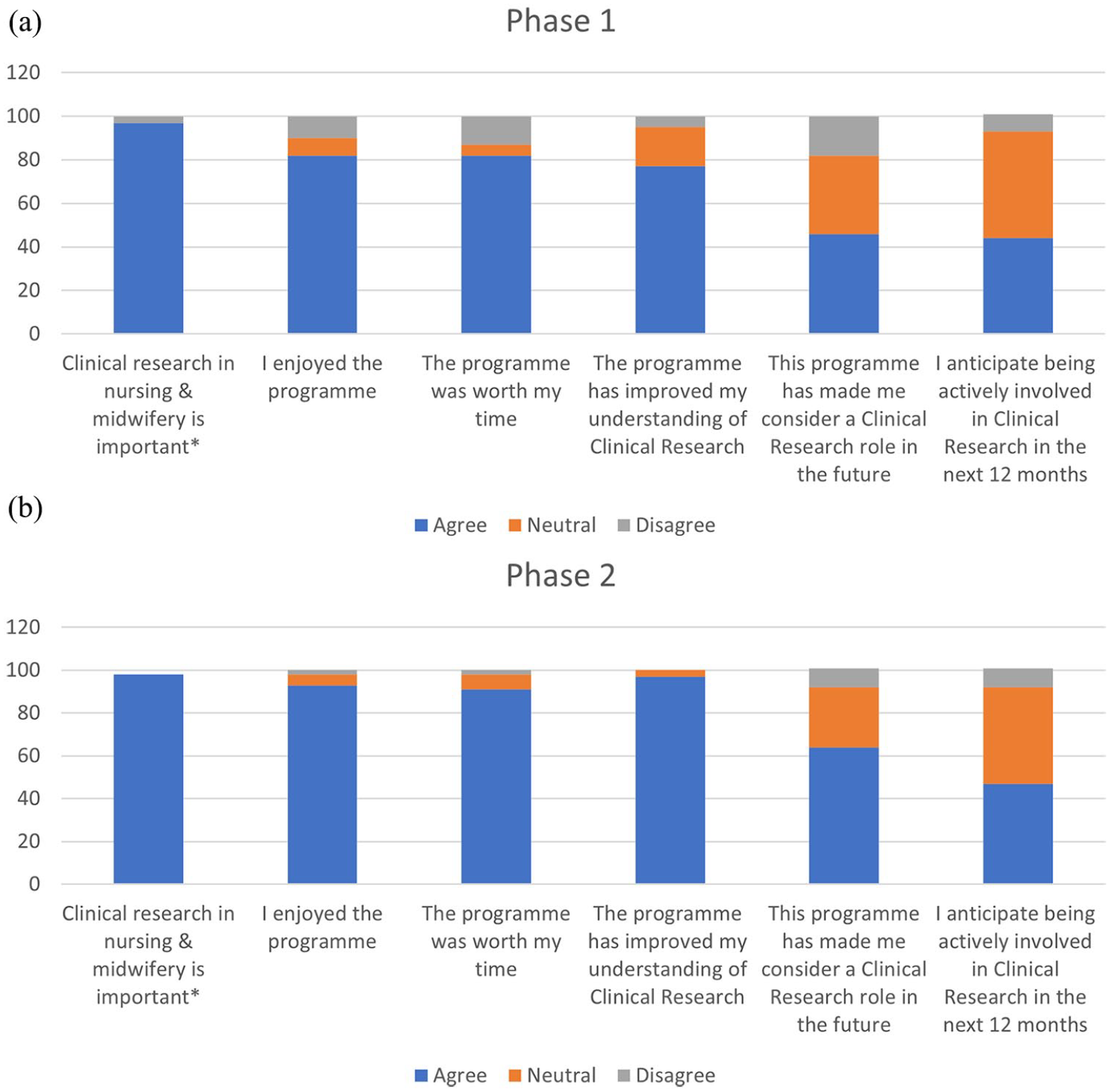
Phase 1 and 2 survey responses.
Learning resources
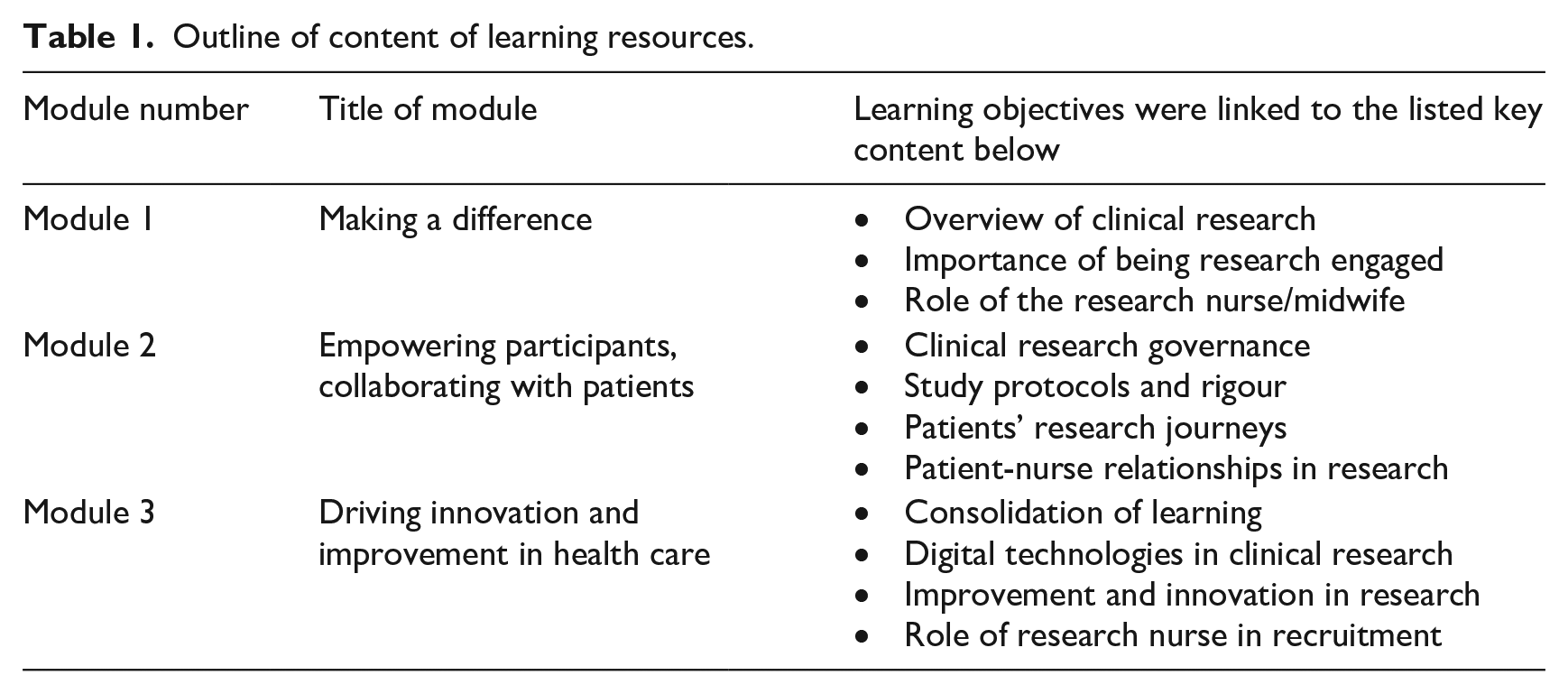
The learning resources developed consisted of three modules (Table 1). Each covered specific themes and topic areas; this enabled the modules to be delivered as stand-alone or collective resources, depending on the target audience, and learning environment. All three interactive modules were designed to be delivered either as self-taught online educational resources, as face-to-face or online traditional teaching materials, or as adjuncts for seminar/discussion forums. Each module was anticipated to take a minimum of 1 hour to complete, with a cumulative time of at least 3 hours to complete all three modules.
Outline of content of learning resources.
Phase 1 recruitment, data collection and analysis
This initial pilot phase aimed to assess whether the learning resources were useful for nursing pre-registration students. Between June 2021 and February 2022, the learning resources were shared with pre-registration nursing students based across five HEI and NHS organisations in England; most were in their second year of study. This was done by SNMRL’s sharing the resources with named contacts at the various HEIs and NHS organisations and asking them to share the resources with pre-registration nurses, as well as incorporating them into their teaching where appropriate. This time frame was sufficient for the learning materials to be used with students in various formats across a range of university semesters, modules and pathways, as well as allowing opportunities for students to use the resources whilst working in clinical research placement areas. The resources were delivered via different organisations either through face-to-face teaching sessions or as self-directed learning tools.
To evaluate the resources, the project team developed a short online survey (Appendix 1) via JiscMail to capture different elements of the learning experience, which were linked to the nine programme objectives. These were: (a) be able to explain what clinical research is, (b) understand why all clinical staff (including all nurses and midwives) need to be research aware, (c) understand what a research (delivery) nurse/midwife does, and how this differs from academic roles, (d) understand how clinical research regulations, guidelines and protocols protect patients and ensure robust conclusions inform evidence based clinical care, (e) understand a typical patient journey through a research project, (f) understand how patient interaction in research delivery compares with other clinical roles, (g) understand how digital technologies are transforming clinical research, (h) understand how clinical research design and delivery continues to evolve through a sustained focus on Improvement and Innovation and (i) understand how research nurses and midwives can have a major influence on improving patient recruitment.
The survey contained both structured Likert style questions and open-ended free text questions. Following the end of the phase 1 pilot, survey findings were analysed using descriptive statistics. Free text responses were grouped together thematically.
Stakeholder feedback
Based on the phase 1 survey findings, the project team made adaptations to the learning resources to increase their applicability and usefulness for pre-registration nursing students. To aid this process the project team also convened a national Stakeholder Advisory Group (SAG) in April 2022. The SAG consisted of individuals from HEI’s, healthcare organisations and local CRNs, all with expertise in clinical research delivery. SAG members reviewed the phase 1 survey findings and provided constructive feedback on how to improve resource content, language and deliverability. In addition, the SAG recommended that additional content and scenarios were included within the learning resources to ensure that they were relevant and applicable to pre-registration midwifery students, as well as to nursing students. Other recommended additions included captions and voice-overs to ensure inclusivity and flexibility of the resources for individuals with a range of learning needs and preferences and in a range of learning environments. Suggested changes and improvements to the learning resources were applied and the SAG subsequently re-reviewed and approved the updated resources.
Phase 2 recruitment, data collection and analysis
The phase 2 pilot took place in November 2022 and aimed to evaluate the use of the updated learning resources. Pre-registration nursing students studying from HEI and NHS organisations in Northwest England took part in the phase 2 evaluation. Contact was made with clinical academic nurse leads at these organisations who agreed to pilot the slides during teaching sessions with pre-registration nurses. Students who piloted the resources were mostly in their third year of study and had the option of engaging with the resources via self-directed learning or via face-to-face teaching. Following engagement with the slides, students were invited to attend an interactive workshop for further discussion on what they had read or been taught (a flipped classroom approach).
To evaluate the resources, the project team used the same online survey (Appendix 1) that had been used in phase 1 with the HEIs and NHS organisations, but with two additional questions added to capture data on the mode of delivery of the slides (face-to-face or self-directed) and the effectiveness of the delivery mode on meeting students’ learning requirements. The survey was shared with the HEI and NHS organisations, which were asked to share it with students who had engaged with the learning resources. Following the end of the phase 2 pilot period, survey findings were analysed using descriptive statistics. Free text responses were grouped together thematically.
Ethical considerations
This project involved the evaluation of a co-produced learning resource; therefore, ethical approvals were not required. However, the service evaluation was approved by the NIHR Governance team, and the data controllers were the Department of Health and Social Care. Survey completion implied consent to participate. In line with service evaluation standards, the work is reported with reference to the Standards for Quality Improvement Reporting Excellence (SQUIRE 2) checklist (Ogrinc et al., 2016).
Results
Characteristics of respondents
Characteristics of phase 1 and 2 respondents are detailed in Table 2. Most respondents were adult nursing students in their second or third year of study. A total of 97 students responded to the surveys, 39 in phase 1 and 58 in phase 2.
Characteristics of respondents.
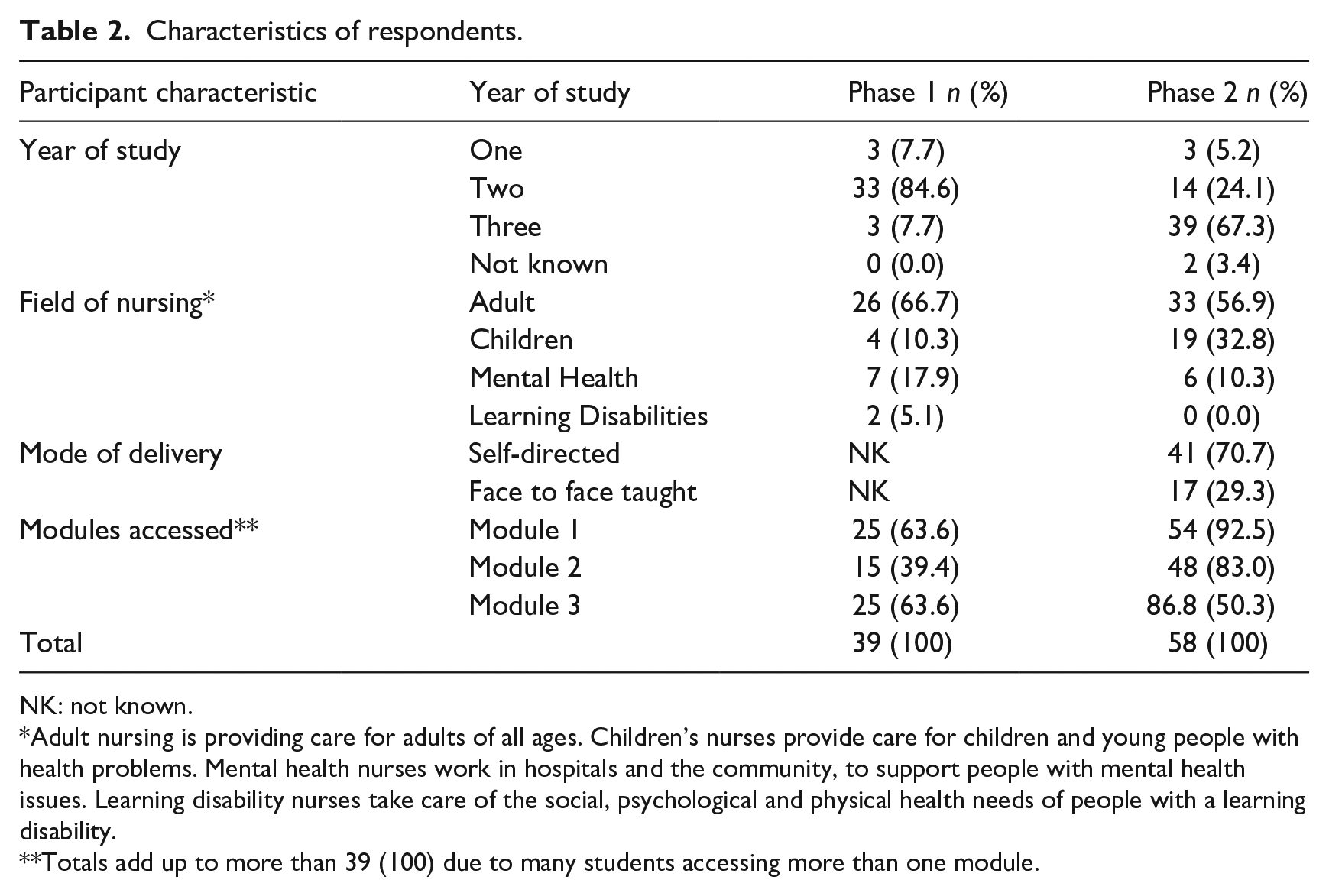
NK: not known.
Adult nursing is providing care for adults of all ages. Children’s nurses provide care for children and young people with health problems. Mental health nurses work in hospitals and the community, to support people with mental health issues. Learning disability nurses take care of the social, psychological and physical health needs of people with a learning disability.
Totals add up to more than 39 (100) due to many students accessing more than one module.
Survey findings
Some students in phase 1 suggested improvements to resource content, such as more ‘real life examples of research’. They also suggested that a range of delivery options including face-to-face teaching, in-person workshops and more interactive online breakout rooms would increase the versatility of the slides. Information technology issues were also reported; these centred around difficulties accessing HEI virtual platforms from NHS organisations. These comments were largely addressed and incorporated into the features of the learning resources prior to phase 2.
In phase 1, 64% of responders completed module 1, 39% completed module 2 and 64% completed module 3. During phase 2 this increased to 96% completing module 1, 83% completing module 2 and 87% completing module three 3. During phase 2, 71% of responders reported that they had utilised the slides via a self-directed learning approach, whilst 29% reported accessing the slides through face-to-face teaching. Ninety-one percent of students reported that the delivery mode they had accessed had been effective or quite effective in meeting their learning needs. No sub-analysis of any differences in responses for face to face versus online was undertaken.
There were increases in the proportion of students who ‘strongly agreed’ or ‘agreed’ with the survey statements between phases 1 and 2 (Figure 1). With regard to whether students had enjoyed the module, responses were very favourable, with strongly agree or agree being chosen by 82% of phase 1 respondents and 91% of phase 2 respondents. Seventy-seven percent of phase 1 respondents and 97% of phase 2 students agreed or strongly agreed that the learning resources had improved their understanding of clinical research and 82% and 91% of phase 1 and 2 respondents, respectively, agreed or strongly agreed that the time they spent reviewing the learning resources was worth it. When asked whether they considered clinical research in nursing and midwifery important, responses were consistent across the two pilot phases with 64% of phase 1 and 68% of phase 2 respondents strongly agreeing with this statement.
Forty-four percent of phase 1 respondents strongly agreed or agreed that they anticipated being actively involved in research in the coming year following use of the learning resources; this compared with 46% of phase 2 respondents. Forty-six percent of phase 1 respondents reported they would consider taking on a clinical research role in the future, compared to 63% in phase 2 respondents.
Respondents also commented on the nine programme learning objectives in terms of (a) whether they had been met and (b) which they considered the most useful (Figure 2). In both phases, responses were very similar regarding objectives being met, with answers ranging between 63–95% (phase 1) and 60–98% (phase 2). The learning objective that was considered most useful in both phases was ‘understanding why all clinical staff (including all nurses and midwives) need to be research aware’ (39% in phase 1 and 28% in phase 2), with 95% (phase 1) and 90% (phase 2) students reporting their learning needs around this objective had been met. This contrasted with the learning objective related to understanding how digital technologies are transforming clinical research being identified by only 8% of phase 1 students and none of the phase 2 students as the most useful learning objective. However, 68% (phase 1) and 60% (phase 2) students still reported that their learning needs around this objective had been met.
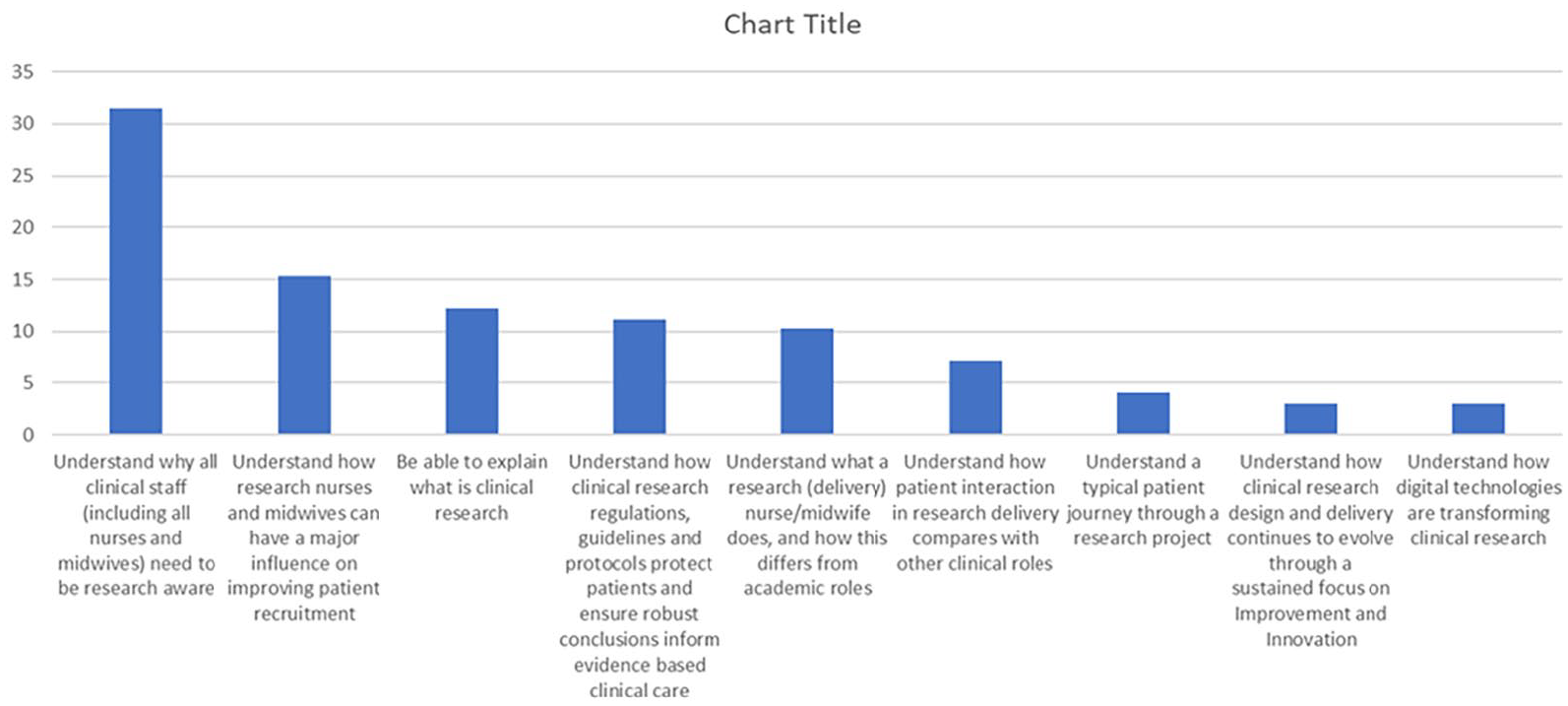
Combined phase 1 and 2 survey responses relating to students’ perceptions of whether programme learning objectives had been met.
Free text survey responses in phases 1 and 2 supported the findings that the learning resources were useful and well received by students. Students commented on the usefulness of the resources to aid their learning, as well as the interactive nature of the resources and how they helped them to engage with research. They also spoke of their enthusiasm for the topic and the way that the resources were delivered, making their learning experiences enjoyable and informative.
The slides are really informative and useful (phase 1 student) I loved the programme and how engaging it is (phase 2 student) It was all really well lead; I enjoyed my time (phase 2 student) I loved this session (phase 2 student)
Suggestions for improvement were also sought and these included improving the resource visuals to make them more appealing and allowing for greater interaction. As a result, the content has since been moved from the original PowerPoint slides to an interactive Articulate Rise 360 platform.
Discussion
The learning resources reported on in this paper have been found to substantially improve nursing students' understanding, engagement and enthusiasm for clinical research. This is crucial as during pre-registration nursing and midwifery programmes the opportunity to learn about research is relevant to every nurse and midwife, regardless of whether they wish to pursue a career in research (Council of Deans of Health 2019, 2021). Research underpins good clinical practice, and the NMC mandates that pre-registration courses should provide students with a level of research knowledge, skills and confidence that enables them to: (a) be research aware in their practice, (b) have an evidence-informed approach, (c) have knowledge of design, methods and ethics of research, (d) assess and evaluate evidence and (e) understand service evaluation and development (NMC, 2018b, 2018c).
A recent survey by the Council of Deans of Health (2019) to assess the current UK landscape of research education provision evidenced curriculum opportunities that included the use of evidence-based practice modules, research methods modules and dissertation modules. However, opportunities for students to be research aware in practice is limited and the ability for them to gain exposure to careers in research is rare (Council of Deans of Health, 2021). Some students complete pre-registration training without working alongside clinical research nurses and midwives or post-doctoral nurse/midwife researchers and many pre-registration nurses and midwives lack awareness that these roles exist (Council of Deans of Health, 2019). Our resources provide a solution to these challenges by exposing students to clinical research delivery roles prior to qualification. The Council of Deans of Health survey also demonstrated competing demands in a crowded curriculum, with variation in the extent to which research was integrated into it (Council of Deans of Health, 2019). A packed curriculum leaves little time for focused input on the applied side of research, such as clinical research delivery. Flexible and adaptable learning resources such as the ones reported in this paper, as well as innovative delivery methods, need to be developed and implemented to maximise the content of the pre-registration curriculum, to ensure that students gain the broadest possible professional research education and to increase awareness of career pathways in academia and clinical research delivery.
As emphasised by NHS England’s Chief Nursing Officer, all nurses and midwives have a role in supporting, leading and delivering research, regardless of their clinical roles (NHSE, 2021). Clinical research delivery roles, and clinical academic careers, are cornerstones of this research knowledge and understanding. In 2021/2022, the Academy of Medical Sciences convened a Working Group of experts from academia, industry, charities and the NHS to explore the actions needed to future-proof UK health research. The report recommended that people were placed at the heart of the UK health research system to reflect that research culture and career structures can be limited, undermining the ability of diverse individuals with broad expertise to fully explore their potential. It also recommended that talented people develop careers that span roles in public, private and charitable research sectors to maximise the research potential of the NHS (The Academy of Medical Sciences, 2023). Research led and delivered by nurses and midwives can drive sustainable change for the NHS, developing these healthcare professions in and beyond the UK (NHSE, 2021). The importance of exposure to health service researchers and research in pre-registration courses, including through our learning resources, is fundamental to this, as organisations that engage in clinical research have better outcomes than non-research active organisations (Jonker et al., 2020).
Nursing and midwifery curricula and learning environments need to be designed to facilitate the development of health professionals who can maximise their research potential and effectively integrate research activity across health and social care and academic settings, as well as inspiring a cohort of nurses and midwives to consider careers in clinical research. Newington et al. (2021) explored the perceived impact of being research-active from the perspectives of nurses, midwives, allied health professionals, healthcare scientists, psychologists, pharmacists and managers of these professions. They identified that most research-active clinicians reported that a key personal impact of their research engagement was the opportunity to establish and develop networks with other clinicians who were interested in research. We believe developing research networks should begin as a student and be sustained throughout nursing and midwifery professional careers. Our learning resources aim to raise awareness of nursing and midwifery research career opportunities to develop and maintain research activity throughout these professions.
The learning resources developed provide solutions to many barriers that limit nurses and midwives from engaging in research at the start of their professional careers and have been found to be engaging, informative and valuable, as well as generating an active interest and desire from students to remain involved in research going forward. The resource has been designed to be used flexibly in a range of different learning formats and can be adapted for a range of delivery modes, accommodating face-to-face and online learning. The versatility of the resources allows them to be delivered as standalone learning packages, used alongside other learning materials, or within university modules or programme content. This reduces the pressure to embed the resources within an already tightly packed nursing and midwifery curricula; instead, the resources can be used as an adjunct to complement and bring to life core learning that students have undertaken in research methods modules. This may be particularly effective if the resources are delivered by research delivery staff, rather than lecturers who have not had first-hand experience of clinical research settings. The learning resources can be delivered flexibly, which is important to meet individual and generational learning preferences (Joan, 2013; Jones et al., 2015). The resources can also be utilised at different times throughout nursing and midwifery pre-registration programmes, to ensure complementary learning and alignment with core curriculum elements. As such, the resources are responsive to the needs of both teachers and learners across HEI and NHS settings.
Strengths and limitations
The learning resources developed and piloted in this service evaluation were designed and developed with the input of key stakeholders with clinical research expertise. This collaborative approach enhances the credibility, usefulness and applicability of the resources, demonstrated by the increase in positive survey responses relating to clinical research between survey 1 and survey 2 (pre- and post-resource modifications). However, limitations included the fact that students who participated in this research might already be more likely to have a positive attitude to research which in turn could have biased the results. There were no students, or newly qualified nurses, as part of the steering group and this is something we would consider moving forward when reviewing future iterations of the resource. Whilst no midwifery students were included in the pilot evaluation, expert midwifery stakeholder feedback was incorporated when updating the resources prior to phase 2. In addition, phase 1 and 2 slides were piloted across different HEI and NHS organisations, which may have impacted on the responses received from students. As we were unable to monitor how many students were given access to the resources across HEI and NHS organisations, we were unable to ascertain a survey response rate. Furthermore, due to the limited time frame of the service evaluation we were unable to follow up nursing students who accessed the resources to see whether they went on to engage with research upon qualification. Future longitudinal work to explore this would help assess the long-term impact of the resources in shaping research career pathways for nurses and midwives.
Information technology difficulties during the pilot phases emphasised the need for the resources to be available on a platform that is easily and freely accessible from NHS and HEI locations. Plans to embed the tool on a suitable national platform aim to address this issue by maximising reach to teachers and learners alike. This will allow the resources to be accessed not only by pre-registration nurses and midwives but by other nurses and midwives who may be new to research or newly qualified, as well as those who have not had opportunities to engage in research or who want a research refresher. It will link to other research resources, meaning that users can gain exposure to a range of relevant research information and opportunities. Future work, supported by NIHR Nursing and Midwifery, will monitor usage of the resources to measure their long-term impact.
With regard to the questionnaire, we acknowledge that inclusion of the question ‘I anticipate being actively involved in clinical research in the next 12 months’ may have had confounders as year 1 and some year 2 students might not be in practice in 12 months. This has subsequently been changed for future iterations of the resource. It is also acknowledged that it will be valuable to include students, or newly qualified nurses when reviewing any future updated versions of the resource.
Conclusions
The learning resources piloted in this service evaluation have the potential to overcome many barriers to research engagement faced by nurses and midwives. By engaging nurses and midwives early in their professional careers, the resources can pique students’ interest in research, paving the way for further involvement. The resources demonstrate to students that research can be incorporated into a range of clinical, educational and academic nursing and midwifery roles, and there is no one size fits all approach to being research active. This aligns with national policy which stipulates the importance of creating diverse and varied opportunities to incorporate research into nursing and midwifery roles, regardless of setting, career stage or level of seniority (NHSE, 2021). Building and developing the clinical research workforce and integrating research across health and social care disciplines is a national and international priority (NIHR, 2021a, 2021b) and is integral to the health and the wealth of the nation. Though our learning resources have been designed primarily for use by nurses and midwives, their versatility means they could be adapted by a range of health professionals with an interest in clinical research, demonstrating their worth in supporting the clinical research workforce of the future.
Key points for policy, practice and/or research
A range of versatile learning resources are required to enable nurses and midwives to engage in clinical research.
Developmental research opportunities can help tackle widespread recruitment and retention issues within nursing and midwifery through creating new and varied career progression pathways.
Research is integral to the provision of optimal health outcomes, and all health and care staff need an awareness of how to implement research findings into practice.
All pre-registration students should have the opportunity to work alongside clinical research nurses and midwives or post-doctoral nurse/midwife researchers; this promotes awareness of these roles through role-modelling and profile raising.
Footnotes
Appendix
Undergraduate Slides feedback: Template.

|
|
| Which organisation has asked you to give feedback on these slides? |
| What year of your training are you in? |
| If you selected Other, please specify: |
| Please choose your branch: |
| Which module(s) of the training did you complete? (Select all that apply) |
| What was the mode of delivery? |
| How effective was this mode of delivery for your learning? |
|
|
| Please read the following statements and select the most appropriate response. |
| I enjoyed the programme |
| The programme has improved my understanding of Clinical Research |
| The learning objectives for the programme are listed below (a–i), please select those you feel were met, select all that apply: |
| Which of the learning objectives listed below (a–i), were most useful to you? |
| I felt that completing the programme was worth my time |
| I feel that Clinical Research in nursing and midwifery is important |
| I anticipate being actively involved in Clinical Research in the next 12 months |
| This programme has made me consider a Clinical Research role in the future |
| Please use this space to tell us anything that you think would improve the programme: |
| Would you recommend this programme to other nurses and midwives? |
| Protecting your data: |
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethical approval
This project involved the evaluation of a co-produced learning resource, therefore ethical approvals were not required. However, the service evaluation was approved by the NIHR Governance team, and the data controllers were the Department of Health and Social Care. Survey completion implied consent to participate. In line with service evaluation standards, the work is reported with reference to the Standards for Quality Improvement Reporting Excellence (SQUIRE 2) checklist (Ogrinc et al., 2016).
Trial registration
Not applicable.
