Abstract
Cancer is one of the most common causes of mortality among disabled people, and population-based screening is an effective method to identify some cancers early; however, its uptake is lower among the disabled population. There is a lack of evidence regarding why they access less, and their need to access population-based screening programmes. To synthesise evidence of the experience of accessing population-based screening programmes for disabled people. A qualitative evidence synthesis (QES) was carried out by searching electronic databases including Medline, CINAHL, Web of Science Core Collection, and Scopus. Grey literature was also searched for. The search yielded 32 relevant publications. The findings are based on Levesque’s conceptual framework. Several factors affect the accessibility of screening services, including people’s perceptions, family support, affordability, literacy, and accessibility.
Conclusion
Screening services need to acknowledge the needs of disabled people and integrate reasonable accommodations to facilitate their needs.
Keywords
Introduction
The number of cancer deaths worldwide in 2022 was 10 million, making it the second leading cause of mortality (World Health Organization, 2022). It is projected that 28.4 million people worldwide will be diagnosed with cancer in 2040, leading to a worsening of the global burden of cancer (Sung et al., 2021). Disabled people, who represent 1.3 billion people worldwide (World Health Organization, 2023), have a disparate risk of certain forms of cancer compared to non-disabled people (Hughes et al., 2022; Iezzoni et al., 2021). Cuypers et al. (2022) found that individuals with intellectual disabilities experience higher mortality rates from colon, breast, and cervical cancer than the general population. Colon cancer accounted for the highest number of deaths among people with intellectual disabilities, while cervical cancer, despite having a lower absolute number of deaths, showed the largest difference in mortality risk compared to the general population, indicating substantial disparity in outcomes, potentially due to differences in access to or effectiveness of cancer screening and treatment (Stirling et al., 2021). Similarly, people with physical impairments (Iezzoni, Rao, and Agaronnik, 2020), and members of the Deaf community (Druel et al., 2018) have a higher risk of mortality due to cancer.
The causes of this heightened risk are multifactorial, with a higher prevalence of cancer-related risk factors, including higher rates of smoking, obesity, and sedentariness (Iezzoni et al., 2022). Disparities in cancer-related mortality among disabled people are also attributable to lower rates of participation in cancer screening (Kellen et al., 2019; Shin et al., 2020). Despite having a higher risk of acquiring cancer, disabled people report poor access to population-based screening services such as cervical cancer screening (Bennett et al., 2016; Bussiere et al., 2015; Bussiere et al. 2014; Lofters et al., 2014), breast (Floud et al., 2017; Horner-Johnson et al. 2015; Horner-Johnson et al., 2014), and colorectal screening (Gofine et al., 2018; Deroche et al., 2017). Kellen et al. (2019) reported that breast screening uptake is lower among disabled people compared to the general population. Similarly, cervical screening uptake is also lower among disabled people than those without disabilities (Horner-Johnson et al., 2015; Steele et al., 2017; Wei et al., 2006). Iezzoni et al. (2020) found that complex disability remained significantly associated with reduced access to colorectal cancer screening.
Multiple factors may underpin the lack of population-based screening uptake among disabled people, as evidenced by an amassing body of literature. Research points to a lack of accurate and precise cancer screening information specific to this population, a lack of assistance from screening staff, poor communication, fear, poor access to transportation (Merten et al., 2015), difficulty in arranging appointments, and professional attitudes (Fang et al., 2016; Watts, 2008), negatively affecting screening access. In addition, a lack of transportation to screening centres (Yankaskas et al., 2010) and inappropriate environments and equipment, such as too high/narrow examination tables (Wu et al., 2012), have been identified as barriers. Therefore, understanding and addressing these barriers are critical for making screening more accessible to disabled people.
Researchers are beginning to conduct systematic reviews to synthesise the available data on screening behaviour among disabled people and their attitudes and perceptions of disabled people regarding screening services. For example, literature on the screening behaviour of people with intellectual disabilities (Chan et al., 2022), attitudes and perceptions of people with intellectual disabilities and carers (Byrnes et al., 2020), and barriers to physical impairments (Edwards et al., 2020) have been systematically reviewed. However, to the best of our knowledge, no previous review has provided a comprehensive synthesis of the qualitative literature documenting the views and experiences of screening from the perspective of disabled people, their caregivers, and professionals. Therefore, this systematic literature review sought to synthesise the qualitative literature describing the experience of population-based screening programmes from the perspective of disabled people, caregivers of disabled people, and professionals involved in screening programmes.
Method
This review adopted a qualitative evidence synthesis (QES) approach, a type of systematic review synthesising evidence from qualitative research that can be conducted as a standalone approach or by reviewing complex interventions (Flemming et al., 2019). Qualitative evidence synthesis collates findings from qualitative research, often primary studies, to gain insight into issues or problems which may be sensitive (Downe et al., 2019). This approach will provide a greater understanding of how such issues or problems impact individuals, communities, or organisations. Therefore, the QES is suitable for this review to explore the needs of disabled people in accessing population-based screening.
Search strategy
In this review, we define disabled people as those with intellectual disabilities, autism, physical impairment, visual impairment, and deafness. The reason for including these disabilities is that many individuals with intellectual disabilities have one or more additional disabilities such as autism, physical impairment, visual impairment, and Deafness. The terminology used in this review is in agreement with Disabled People’s Organisations (DPO).
Inclusion and exclusion criteria.
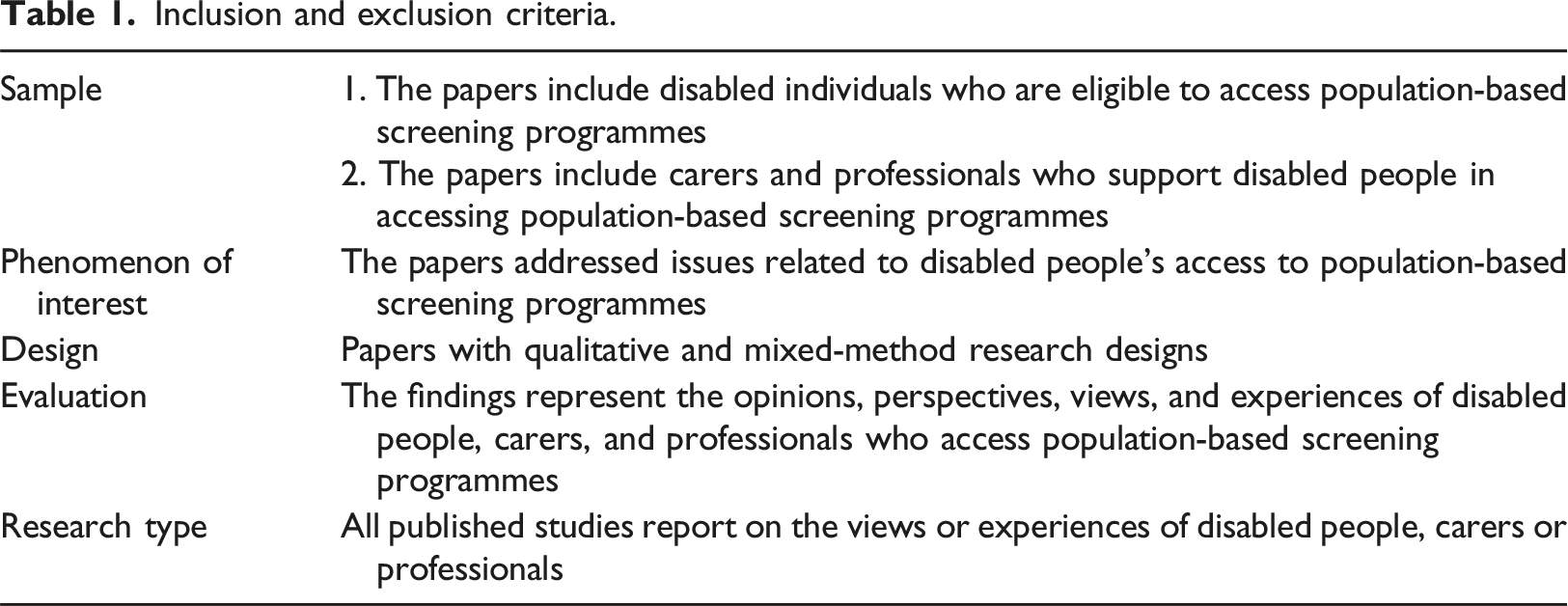

Search terms.
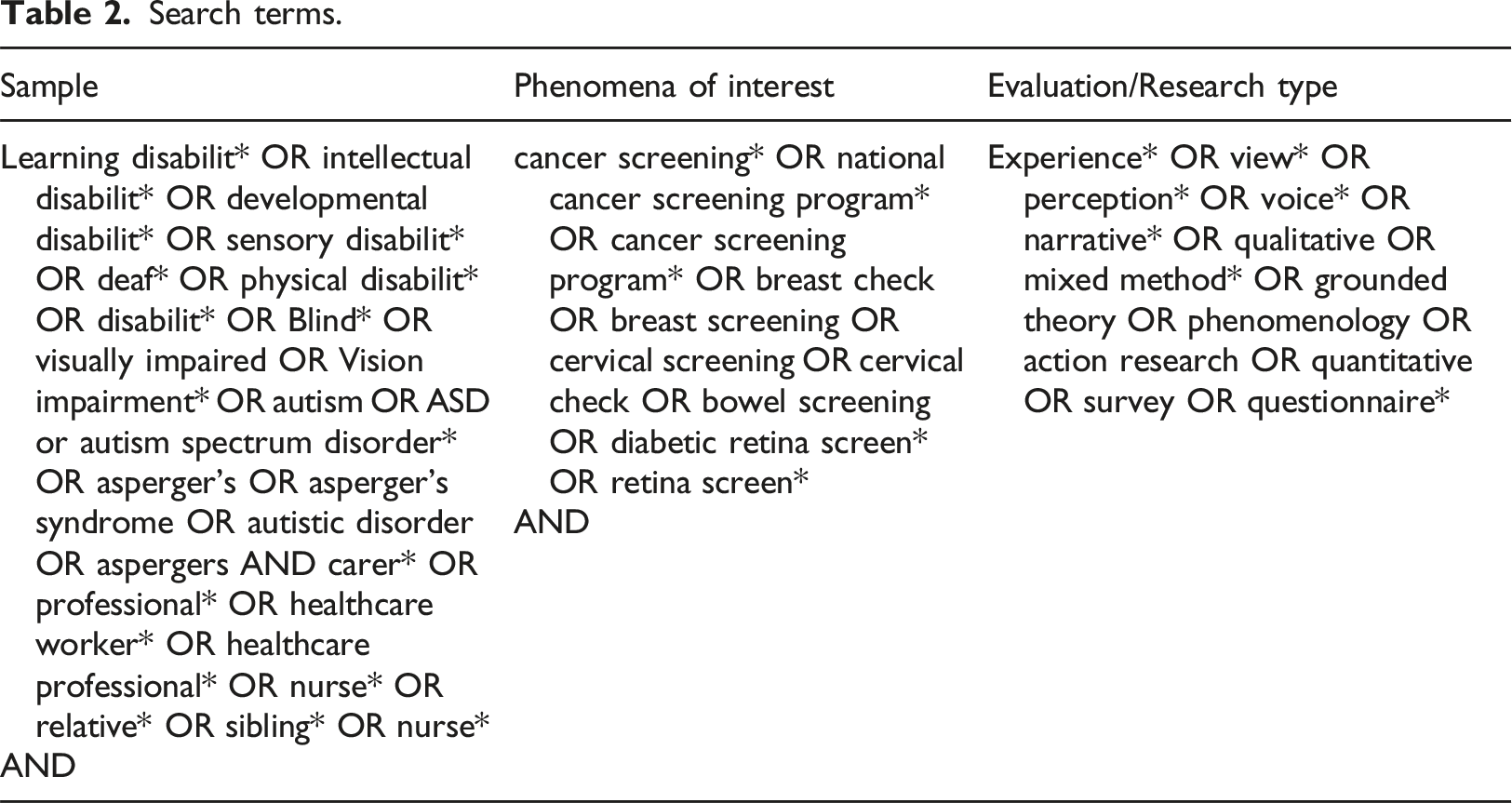
Screening and selection
After retrieving the articles, we imported all records into Zotero, a reference management software package. Subsequently, the relevant articles were uploaded to the Covidence software for eligibility screening (www.covidence.org). Two authors independently screened articles. Initially, the titles and abstracts of the included papers were screened for relevance. After the initial screening, articles that appeared to be eligible were included for full-text review. The full-text review was conducted based on the established inclusion and exclusion criteria, and articles that met these criteria were retained for review. Any disagreement or uncertainty regarding the inclusion or exclusion of records was resolved through a discussion between the reviewers. To broaden the scope of the review, we also searched the reference lists of the studies identified for inclusion in the review. This helped to ensure that we did not miss any relevant studies that may have been cited within the articles we had already found.
In total, 588 records were retrieved from the database searches. Additionally, we sourced one record through a reference search of the studies and two reports through a manual search on the web, which were included in the review. Of these, 157 papers were duplicates and subsequently removed from further consideration. The titles and abstracts of the remaining 434 records were screened, and 357 were judged to be ineligible for review and thus excluded. The eligibility of the remaining 77 records was assessed based on the full text. After a full-text review, 45 papers were deemed ineligible and excluded. Thus, 32 records were included in this review (Figure 1). PRISMA flow diagram showing the systematic screening process.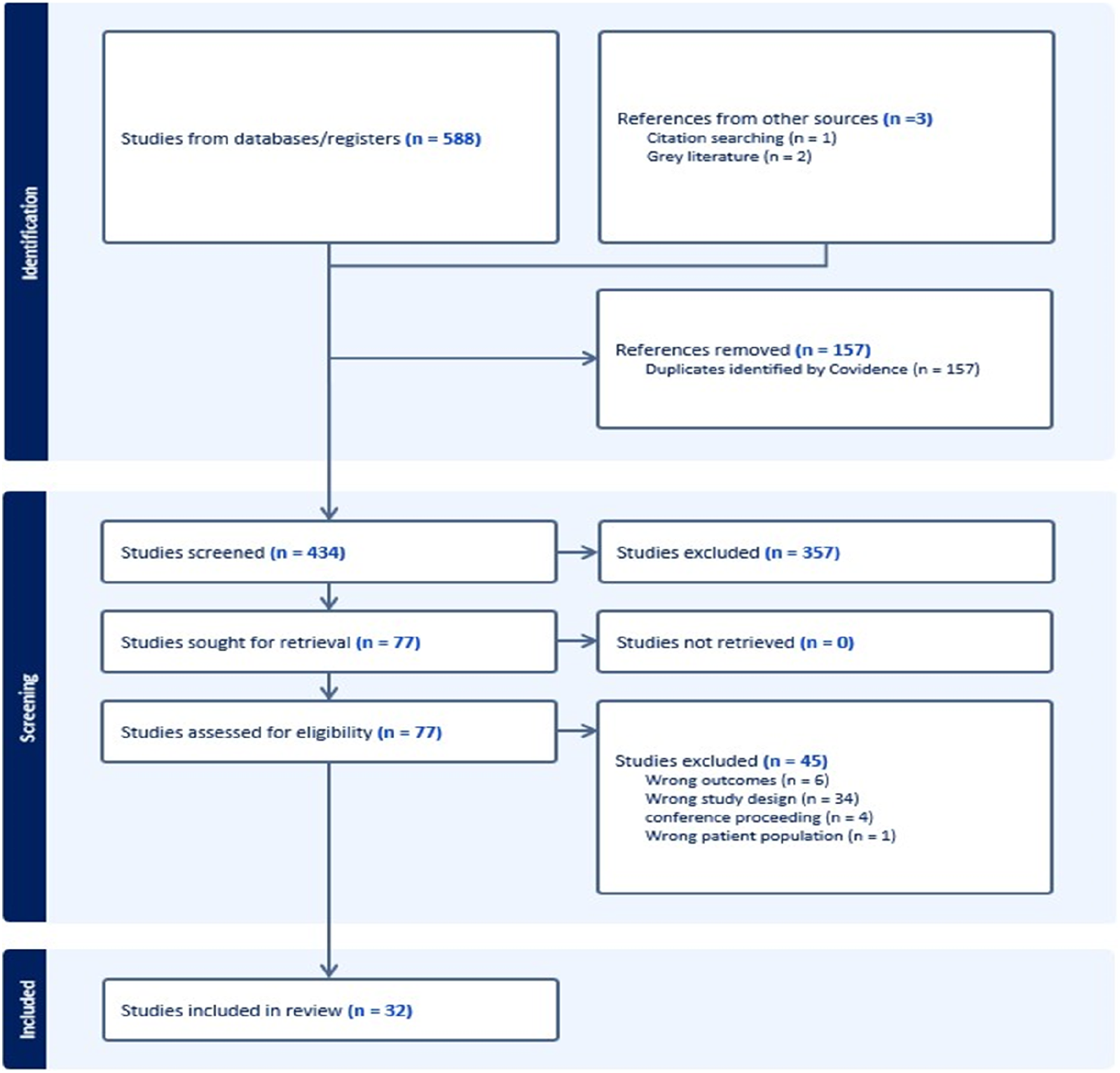
Results
Quality appraisal of the included studies
An essential aspect of the review process is the evaluation of the quality of the evidence included in the study. To accomplish this, two authors carried out an independent assessment of the included articles. A tool developed by the Evidence for Policy and Practice Information and Coordinating (EPPI) Centre was used to perform the quality appraisal (Thomas et al., 2003). This tool comprises 12 criteria that can be applied to evaluate the quality of the study design and execution, reliability and validity of data collection and analysis, and quality of the methods.
Two authors comprehensively evaluated the included studies and assessed the various aspects of their quality. This involved examining whether the aims and objectives of the studies were clearly articulated, whether the articles provided a thorough description of the research context, whether the sample and sampling methods were adequately explained, if the data analysis method was sufficiently described, and assessing the reliability and validity of the data collection tools and analysis procedures employed in each study. Additionally, they evaluated whether the data collection methods effectively captured the participants’ perspectives, whether the findings reflected the data, and whether the participants were actively involved in the study design and implementation (Thomas et al., 2003). None of the 32 studies met all the 12 assessment quality criteria. The majority of the studies, specifically 18, met 11 of the 12 quality criteria (Willis et al., 2015; Willis, 2016; Truesdale-Kennedy et al., 2011; O'Farrell et al., 2013; Magasi et al., 2019; Agaronnik et al., 2021; Arana-Chicas et al., 2020; Kilic et al., 2019; McIlfatrick et al., 2011; Mele et al., 2005; Peters and Cotton, 2016; Seaton et al., 2018; Shah et al., 2022; Sonalkar et al., 2020; Todd and Stuifbergen, 2012; Wilkinson et al., 2011; Sullivan et al., 2004; Taggart et al., 2011). Four studies (Angus et al., 2012; Breau et al., 2022; Peters and Cotton, 2014; Solenberg et al., 2021) met ten criteria - and two studies partially met two of the quality criteria (Barr et al., 2008; Swaine et al., 2013), whereas Wood and Douglas (2007), Poulos et al. (2011) and Greenwood et al. (2014) met eight quality criteria. Wollin and Elder (2003) met seven quality criteria. Finally, Hanlon and Payne (2017), Breakthrough (2020), and Monteith (2015) met only four criteria and partially met three criteria.
Most studies included had a well-defined research aim and were achieved through qualitative approaches. These studies also collected data aligned with their research questions and offered comprehensive insights into their data-analysis methodologies. Nevertheless, few studies have provided a lack of discussion about the inclusion criteria. Further details regarding the assessment of the methodological quality of each study are included in Supplemental File 1.
Description of the included studies
Studies contributed to each theme.

Data extraction and synthesis
Initially, relevant information was extracted from each study, including the purpose of the study, year of publication, funding information, details on recruiting participants, the method used to select participants, the characteristics of the participants, the length of the study, how data were collected, how it was analysed, and the findings regarding access to screening programmes for disabled people using a standardised form by the two authors, and then the relevant information was compared for accuracy. The data were analysed using the five-step framework analysis outlined by Goldsmith (2021). This approach provides a systematic and structured way to analyse qualitative data. Initially, key ideas and concepts in the data were independently coded by two authors, and the sub-themes were charted into the existing healthcare access framework systematically (Levesque et al., 2013). The Levesque model conceptualises five dimensions of healthcare access which are approachability, acceptability, availability, accommodation, affordability and appropriateness. It also identifies the corresponding abilities of people who utilise healthcare: the ability to perceive (recognise health needs), ability to seek (actively pursue care), ability to reach (physically access service), ability to pay (financial ability to pay) and ability to engage (Participate in healthcare) (Levesque et al., 2013). The review team extensively deliberated on mapping codes and sub-themes into the healthcare access framework until a consensus was reached on the placement of sub-themes within the framework (Gale et al., 2013; Srivastava and Thompson, 2009). This step ensured that the analysis was conducted rigorously and systematically and that any discrepancies or differences in interpretation were resolved through discussion (Goldsmith, 2021). Table 3 shows the studies that contributed to each finding.
Synthesis of findings
The presentation of findings in this review is guided by Levesque, Harris and Russell’s (2013) conceptual framework of access to health care. As such, barriers and facilitators of population-based screening are presented within the dimensions of (i) Ability to perceive vs approachability, (ii) Ability to seek vs acceptability, (iii) Ability to reach vs availability and accommodation, (iv) Ability to pay vs affordability; and (v) Ability to engage vs appropriateness. To illustrate findings, quotes are included to accompany the literature synthesis. Each framework domain is discussed and interpreted in relation to relevant literature.
Ability to perceive vs approachability
It is important for individuals to understand the importance and benefits of population-based screening in order to participate in it. When people perceive screening as a necessary and worthwhile activity, they are more likely to engage in it. Many studies in this review found that disabled people’s uptake of cancer screening services was influenced by their ability to view such screening as necessary. Data from included studies indicate that an individual’s perception of the need for cancer screening is influenced by several factors, with literacy skills being the most prominent (and the resultant dependency on family and caregivers) and their ability to communicate effectively with healthcare providers.
First, this review revealed that people with intellectual disabilities, mobility disability and sensory disabilities have difficulty reading screening information, which leads to family members having to communicate screening information to the individual and facilitate accessing the screening services (Llewellyn et al., 2011; McIlfatrick et al., 2011; Mele et al., 2005). Lower screening access was attributed to reading literacy issues and communication with professionals. In addition, professionals face difficulties in communicating the importance of screening programmes for those with intellectual disabilities and sensory disabilities. This often results in a lack of participation in such programmes (Arana-Chicas et al., 2020; Llewellyn et al., 2011): “Participants who were severely impaired appeared not to have knowledge of mammograms, even after a mammogram picture was shown to them” (Arana-Chicas et al., 2020, p. 6).
The ability of individuals with intellectual disabilities and physical impairments to communicate effectively can influence their uptake of available screening services (Greenwood et al., 2014; Magasi et al., 2019; Seaton et al., 2018; Willis et al., 2015). People with intellectual disabilities may face difficulties retaining the information provided, which can influence their decision to register for screening (Willis 2016). Professionals may sometimes face challenges in communicating effectively, which can negatively impact the decision of people with intellectual disabilities to participate in screening programmes (Wood and Douglas, 2007): “Particularly complex issues involved in explaining screening as opposed to therapeutic procedures, the need to enquire about sexual experience, and literacy issues in relation to invitation letters were seen as specific communication issues“ (Wood and Douglas, 2007, p. 88).
Levesque, Harris, and Russell’s framework suggests that the approachability of healthcare access depends on how service providers make their services more visible and accessible to the target populations. This is often linked to the transparency of screening services, their ability to reach the appropriate audience, and the provision of relevant and accessible information (Levesque et al., 2013). The review highlighted three factors shaping the approachability of population-based screening for disabled people. First, healthcare professionals in disability services are important, trusted sources of information for disabled people. Health education and promotional activities conducted by these professionals have the potential to increase awareness among people with intellectual disabilities and physical impairments about the importance of screening services (Arana-Chicas et al., 2020; Hanlon and Payne, 2017; Taggart et al., 2011). On the other hand, conflicting information from healthcare professionals regarding screening services for physical impairments can have a negative impact on the uptake of these services (Llewellyn et al., 2011).
Second, in addition to healthcare professionals, people with intellectual disabilities and physical impairments frequently rely on the information they receive from other sources, such as carers, friends, media, and the internet (Angus et al., 2012; Arana-Chicas et al., 2020; Llewellyn et al., 2011). In certain instances, this information from alternative sources was often favoured and trusted over healthcare professionals (Angus et al., 2012). In contrast, individuals with intellectual disabilities tend to rely on day service programmes to gain information and awareness about screening (Arana-Chicas et al., 2020): “I don’t rely on my doctors for up-to-date information. I very much rely on what I hear from others, and the radio and internet” (Angus et al., 2012, p. 69).
Third, this review emphasised the significance of providing accessible information in screening services to ensure that people with intellectual disabilities understand the nature and importance of cancer screening. Simple and easy-to-read information, using plain language with images, is often necessary to communicate screening information effectively. Furthermore, the invitation to screening services that people with intellectual disabilities receive should be tailored to meet their specific requirements (Wood and Douglas, 2007): “There was also agreement among the women that user-friendly leaflets or posters would be helpful in explaining breast awareness, breast screening and prevention albeit the information should be accessible with the writing ’big’ and 'easy to understand” (Truesdale-Kennedy et al., 2011).
Ability to seek vs acceptability
According to Levesque et al. (2013), seeking service refers to an individual’s ability to identify and access appropriate services when needed. Findings from 26 out of 32 included studies were related to seeking screening services and the acceptability of screening services. The review found that the dependency of some disabled people on others and the attitudes of screening professionals were the primary factors determining disabled people’s decision to seek cancer screening or not. There were multiple examples in the reviewed literature of disabled people depending on others to decide whether to engage with, register, and attend screening services. For example, people with intellectual disabilities and physical impairments frequently rely on others, such as primary carers or family members, to make an appointment and travel to the screening service (Angus et al., 2012; Arana-Chicas et al., 2020; Kilic et al., 2019). Family members are also frequently in a position where they must make decisions regarding screening for their disabled family members, especially those with intellectual disabilities. In some instances, family members were reported to judge that their family member with intellectual disabilities and physical impairments did not require screening services due to assumptions about their sexual activity or that screening was not a priority for the individual (Angus et al., 2012; Arana-Chicas et al., 2020; Greenwood et al., 2014; McIlfatrick et al., 2011; Swaine et al., 2013; Taggart et al., 2011): “[my daughter] wasn’t sexually active, not dating, nothing like that, and having sex. It wasn’t really necessary to put her through it.” (Swaine et al., 2013, p. 68).
Some family members consider screening an important preventive measure and act proactively by making an appointment, facilitating the screening visit, and supporting their loved ones during the screening process (Arana-Chicas et al., 2020). Acceptability of service also influenced the attendance of disabled people at screening services. Acceptability is how the service provision is aligned with the cultural, personal and social expectations of the individuals seeking or utilising the service. Research by Angus et al. (2012) and Peters and Cotton (2016), for example, found that assumptions of normalcy and a lack of sensitivity to people with intellectual disabilities and physical impairments impeded screening utilisation (Kilic et al., 2019; Swaine et al., 2013): “Assumptions of normalcy need to be replaced with an understanding of the nature of various disabilities and a focus on individualised care and reflective practice to combat oppression. The oppressive nature of both the machinery and the perceived uncaring environment led to participants feeling ‘put down’ and ‘powerless'” (Peters and Cotton, 2016, p. 188).
The studies reported instances of disabled people recounting how physical handling caused pain and humiliation, which influenced their decision to seek future screening services (Angus et al., 2012; Arana-Chicas et al., 2016, 2020; Peters and Cotton, 2014; Sullivan et al., 2004; Swaine et al., 2013). In addition, the specific needs of people with intellectual disabilities and physical impairments were often reported to be ignored, and observed that disabled people are more reluctant to seek help due to fear and anxiety (Peters and Cotton, 2014; Poulos et al., 2011; Truesdale-Kennedy et al., 2011): “Some participants felt health care professionals saw them as dehumanised, depersonalised, voiceless bodies, almost like robots, that could be manipulated and moved in any way they saw fit to meet the needs of the breast cancer screening procedure, without regard for the participant’s dignity or physical, emotional, psychological and communicative needs.” (Peters and Cotton, 2014, p. 567).
Comorbidities and complex needs of people with intellectual disabilities were also reported to be important factors affecting how screening professionals perceived and responded within their services (Angus et al., 2012; Arana-Chicas et al., 2020; Taggart et al., 2011; Willis, 2016): “Many women had complex medical conditions, requiring attention to multiple issues during health appointments, additional time and assistance to move about and communicate. Participants’ anecdotes suggested that providers might assign low priority to health promotion or screening under these circumstances. For example, one woman was refused a colonoscopy because of her history of respiratory illness.” (Angus et al., 2012, p.78).
On the contrary, there are positive experiences reported by disabled people regarding some screening professionals. For example, professionals were praised for helping disabled people to relax and assisting in making appointments, making an effort to accommodate their unique needs, providing reassurance, and allocating extra time (Arana-Chicas et al., 2020; Mele et al., 2005; Peters and Cotton 2016; Taggart et al., 2011).
Ability to reach vs accommodation
According to Levesque et al. (2013), the ability to reach pertains to the physical availability and accessibility of healthcare services when needed. Data from 25 studies indicate that the ability of disabled people to access screening services can significantly impact their uptake of these services. the ability of people to access screening services is determined by their ability to travel, mobility issues, and the accessibility of the service (Angus et al., 2012; Kilic et al., 2019; McIlfatrick et al., 2011; Mele et al., 2005). “Transport and timing of the appointment were noted, which were seen to preclude women with intellectual disabilities access breast screening services: . . . access to the screening unit or mobile unit where the mammogram is going to take place. So a transport practicality may prevent them from coming.” (McIlfatrick et al., 2011, p. 416).
People with physical impairments also described how their physical mobility, location, and distance impacted their ability to attend screening services (Peters and Cotton, 2014). Some people with intellectual disabilities and physical impairments feel they lack stamina and have difficulty remaining in a similar position for a short period, as is sometimes required for a mammogram (Greenwood et al., 2014; Peters and Cotton, 2014; Poulos et al., 2011). Further, having short stature and using a wheelchair was reported to impede an individual’s ability to access screening services (Llewellyn et al., 2011; Sullivan et al., 2004).
The studies reported various accommodation issues encountered by disabled people during screening procedures, such as a lack of strategies or facilities to address their specific needs. Appropriate accommodation is essential to ensure the effective completion of the screening procedure for people with intellectual disabilities and physical impairments (Agaronnik et al., 2021; Arana-Chicas et al., 2020): “Appropriate patient positioning is critical for ensuring image quality—inability to accommodate mobility disability can interfere with diagnosis. Furthermore, attitudes of clinical staff about providing accommodations can be just as important as physical accessibility ” (Agaronnik et al., 2021, p. 1254).
With appropriate accommodations and assistance, disabled people feel comfortable and safe. For example, the availability of healthcare attendants during screening can provide support to individuals with intellectual disabilities and physical impairments in various ways, such as assisting with wheelchair navigation, use of restroom facilities, bodily preparation, and handling of stool specimens (Angus et al., 2012; Arana-Chicas et al., 2020; Peters and Cotton, 2014): “Accessible rooms and equipment, as well as attendant care enhanced comfort: Joining [accessible health centre] was very good for me… I feel very comfortable going there. The doctors I’ve dealt with, and the nurses are amazing. One lady comes to help you dress… This takes the stress off me for going to the doctor” (Angus et al., 2012, p. 80).
Disabled people also worry about the absence of flexible appointments when attending screening services. This lack of flexibility often leads to frustration. They feel the set timeframe is insufficient for proper communication and physical preparation. As a result, the healthcare professionals might rush the procedure and miss out on sharing critical information that should be conveyed before the procedure (Angus et al., 2012; Greenwood et al., 2014; Llewellyn et al., 2011; Peters and Cotton, 2014; Willis, 2016). Long wait times can also create frustration and sometimes force the individuals with physical impairments to use additional facilities, such as bathrooms, that are inaccessible (Kilic et al., 2019): “For us, staying in the hospital for a long time means using the toilet there. It is really difficult to go to the toilet in the hospital. We need to finish our business and return as soon as possible.” (Kilic et al., 2019, p. 1982).
Also, the appointment time is crucial because some people with intellectual disabilities require more time to complete their morning routine and hygiene, making early morning appointments unsuitable (McIlfatrick et al., 2011): “Maybe timing of appointments because a lot of these women need care in the morning. By the time you get them washed, their hygiene and get them fed, . . .and you know again with the distance and maybe having to be there for 9 am, you know, to allow an appropriate time in the afternoon to suit them.” (McIlfatrick et al., 2011, p. 416).
Several disabled people in the included studies shared their experiences of some positive accommodations when they attended screening services. When the staff attempted to accommodate their needs, they felt they were treated equally humanely (Llewellyn et al., 2011; Seaton et al., 2018; Sullivan et al., 2004): “Many women praised the facility staff for their helpfulness and support, unfortunately this praise was not universal” (Llewellyn et al., 2011, p. 1764).
Disabled people often identified that the breast cancer screening procedure was inappropriate due to unsuitable mammographic machines. For example, the machine could not be adapted for people in a recliner wheelchair, the device is too high, and breast squeezing by the machine was reported as uncomfortable and painful for some (Angus et al., 2012; Peters and Cotton, 2014; Greenwood et al., 2014; Poulos et al., 2011; Sonalkar et al., 2020; Todd and Stuifbergen, 2012; Willis, 2016): “The requirements of the mammography machine dictated breast screening staff procedures and practices. Women’s bodies were required to meet the machine’s needs, rather than the other way around. Their bodies had to contort and be contorted to accommodate its requirements” (Peters and Cotton, 2015, p. 186).
During cervical screenings, people with physical impairments have experienced discomfort due to inaccessible or inappropriate examination tables which need to be physically manoeuvring to access the table (Hanlon and Payne, 2017; Kilic et al., 2019; Mele et al., 2005; Solenberg et al., 2021): “Having difficulty getting onto the table due to its height. She is reliant on others (a security guard) to lift her on and off the treatment table for the procedure. “The inability to be independent made her feel “manhandled” and caused a loss of personal dignity” (Hanlon and Payne, 2017, p. 22).
Some people with physical impairments have reported inadequate physical facilities that do not cater to their specific needs, leading to discomfort and discouragement in returning to screening services. For example, A small room space can make it challenging to move around, especially when using motorised wheelchairs in mobile clinics. Therefore, it was suggested to have bigger rooms that can accommodate these needs (Kilic et al., 2019; Solenberg et al., 2021; Sonalkar et al., 2020). In addition, others were frustrated with the inadequate facilities to mobilise within the screening centres, such as the lack of provision of lifts and ramps and the presence of revolved doors and heavily locked doors (Mele et al., 2005; Solenberg et al. 2021; Peters and Cotton, 2014): “Needing better access. Participants who used wheelchairs had difficulties with access to BCS [Breast Cancer Screening] facilities. Using caravan facilities was generally prohibitive, and many clinic and hospital venues also posed access barriers in terms of lack of lifts and ramps.” (Peters and Cotton, 2015, p. 186).
There were concerns about inadequate and inaccessible changing and toilet facilities that lacked privacy (Peters and Cotton, 2014; Mele et al., 2005). In addition, the changing rooms are small and do not have enough space for mobility devices, making it difficult and unsafe to transfer in and out of them. (Angus et al., 2012; Mele et al., 2005): “The bathrooms in their providers’ offices were not accessible. When they were, the doors did not lock automatically, increasing anxiety about privacy in those without the manual dexterity to lock the door. Toilets were also too close to the wall, making transfer difficult or unsafe” (Mele et al., 2005, p. 460).
Ability to pay vs affordability
Financial ability to pay influences the uptake of screening services and the affordability of healthcare costs by individuals seeking healthcare, including direct and indirect costs of services (Levesque et al., 2013). Participants in four of the included studies discussed how screening service utilisation is influenced by disabled people’s ability to pay. Some disabled people are deterred from attending screening services when they are not provided free of charge, but many countries consider screening services a fundamental right for their citizens (Llewellyn et al., 2011; Barr et al., 2008): “Women in four groups mentioned economic access barriers: problems paying for mammograms (e.g., inadequate insurance coverage, co-payments” (Barr et al., 2008, p.382).
Indirect costs such as transportation and other additional needs were also identified as barriers to access screening (Mele et al., 2005; Barr et al., 2008). For example, a Deaf woman (Barr et al., 2008) was required to pay for an interpreter service, which caused financial implications while attending the screening service.
Ability to engage vs appropriateness
Levesque et al. (2013) define the ability to engage as the individual’s capacity to participate in healthcare decision-making and engage effectively with healthcare professionals and health services. The ability of professionals and disabled people to engage with each other while attending screening services is essential. When professionals engage with disabled people, it fosters a sense of ownership and allows them to remain involved with services in the future. However, the lack of knowledge about disabled people’s specific needs can sometimes hinder professionals from effectively engaging with them. In addition, they often struggle to engage with professionals due to professionals’ lack of knowledge and negative perceptions of screening services. (Solenberg et al. ,2021; Sullivan et al., 2004; Taggart et al., 2011).
The interaction and engagement between disabled people and professionals and the suitability of screening services significantly influence the access and uptake of screening services. In addition, a lack of awareness persists among Deaf women about the age at which specific screening services must be undertaken (Wollin and Elder, 2003). Further, fear concerning the procedure and outcome often deters people with intellectual disabilities from attending screening services (Wilkinson et al., 2011; Willis, 2016). However, a good level of knowledge is demonstrated among some people with physical impairments about bowel screening (Solenberg et al., 2021): “A 72-year old female with degenerative disc disease and agoraphobia, first stated she knew nothing about CRC screening but eventually described two methods: Nothing…I know they go up your rectum…[there’s] a thing you can use at home to test for cancer in your poop” (Solenberg et al., 2021, 5).
Discussion
The findings from this qualitative evidence synthesis (QES) highlight the crucial role of individuals’ perceptions in shaping the uptake of cancer screening services, particularly within the context of disabilities. The review findings highlight substantial challenges for disabled people in accessing screening, including communication challenges, reliance on family support, socioeconomic factors, cultural expectations, and negative past experiences, all of which collectively impact their access to and engagement in population-based screening programmes. Notably, individuals with intellectual disabilities encountered obstacles in accessing screening due to challenges in reading information and reliance on family members for communication. A further barrier was communication issues with healthcare professionals, highlighting the significance of trusted sources. Levesque, Harris, and Russell’s (2013) framework accentuate healthcare professionals as crucial in health education, underlining the potential for raising awareness among disabled people, which would increase participation (Esmeray and Yanikkerem, 2022; Steinberg et al., 2002; Yankaskas et al., 2010). However, Orsi et al. (2007) argue that there is no relationship between awareness and uptake of the screening programme; instead, the uptake is hugely influenced by the attitude regarding cancer screening needs. Further, Kung et al. (2012) highlighted the influence of socioeconomic factors such as education levels and income status on screening uptake.
Family members play a pivotal role, sometimes deeming screening unnecessary based on assumptions about the individual’s sexual activity or prioritisation. However, proactive family members recognise the importance of screening as a preventive measure and actively facilitate the process. Breau et al. (2020) have highlighted the significance of family members or caregivers accompanying individuals with intellectual disabilities, serving as both emotional companions and valuable sources of information and support during the screening journey. The acceptability of services, aligned with cultural, personal, and social expectations, emerges as a key determinant of attendance, with barriers such as assumptions of normalcy and insensitivity impeding uptake (Vanderpool et al., 2014). Instances of physical discomfort, humiliation, and neglect of specific needs contribute to negative experiences, impacting individuals’ decisions to seek future screening (Filippi et al., 2013; Lo et al., 2013; Shaw et al., 2011; Streu, 2016). Additionally, the comorbidities and complex needs of disabled people influence how screening professionals perceive and respond to them (Edwards et al., 2020; Byrnes et al., 2019).
Kett et al. (2020) supported the review’s findings and asserted that challenges profoundly influence the ability of disabled people to access cancer screening services in terms of transportation, mobility issues, and overall accessibility. Further, difficulties in finding accessible transport and limitations in physical mobility impact attendance, with some individuals facing obstacles during procedures like mammograms due to their specific physical conditions (Ross et al., 2019). Accommodation issues, including professional, mechanical, and environmental factors, further highlight the necessity for tailored strategies to address the unique needs of disabled people attending screening services (Andiwijaya et al., 2022). Positive experiences are associated with appropriate accommodations, such as attendant services, while frustrations arise from inflexible appointment scheduling, long wait times, and inconvenient timings. Inappropriate mammographic machines and inaccessible examination tables during cervical screening contribute to discomfort and dissatisfaction (Ross et al., 2019).
Similar to this review, Amenuke-Edusei and Birore (2021) and Courtney-Long et al. (2011) found that problems affording screening due to inadequate insurance coverage or co-payments threaten access to screening services. However, Fayanju et al. (2014) argued that perceiving fear of mammogram-related pain and receiving bad news is a more substantial barrier than the perceived cost. In addition, the challenges in the engagement between professionals and disabled people arise from the professionals’ lack of awareness and knowledge about specific needs, hindering effective communication, which significantly acts as a barrier to accessing screening services (Fang et al., 2016).
Strengths and limitations
This qualitative evidence synthesis (QES) explores the experiences of disabled people, their families, and professionals when accessing population-based screening services. The review highlights the factors that facilitate or hinder access to these services. The studies also come from jurisdictions with different public health policies which set out the screening recommendations for specific populations and whether screening is provided free or the person is required to pay. The search strategy employed in this QES was carefully designed and supervised by an independent subject Librarian, explicitly focusing on qualitative research. However, this approach may unintentionally exclude quantitative studies that incorporate qualitative components. Furthermore, most studies included in this review primarily address physical and intellectual disabilities, with limited representation from individuals with visual impairments, Deaf and autistic people. As a result, the generalisability of the findings to other disability groups may be affected.
Implications of the findings: practice and research
The insights gained from this QES review can guide future decisions on implementing strategies or interventions to improve population-based screening access for disabled people. Additionally, this research provides valuable perspectives to policymakers, guideline developers, and practitioners involved in screening services regarding the experiences of disabled people and their caregivers concerning the need for screening procedures. It is worth noting that providing disability awareness training to professionals could significantly enhance their knowledge, confidence, and skills in meeting the requirements of disabled people. In addition, promoting screening information through accessible formats can significantly improve attendance at screening services by disabled people. Furthermore, developing supporting roles within screening services and creating communication channels between disabled people and professionals who carry out screening can contribute to the safe and efficient implementation of screening procedures while maintaining a person-centred approach. The review also highlights the lack of evidence on the experiences of certain groups, such as individuals with autism, Deaf or those who are visually impaired. Therefore, further research is required to explore these populations’ needs and those of people with physical impairments at specific points of the screening pathway.
Conclusion
This review highlights the critical role of individual perceptions in shaping the uptake of cancer screening services, particularly among disabled people. The review reveals barriers such as challenges in information access, lack of health literacy, reliance on family members, poor accessibility, affordability and communication issues with healthcare professionals. Family dynamics play a significant role, with proactive members facilitating screening while others may hinder it based on assumptions about their caree’s needs and preferences. Cultural and personal expectations, physical discomfort, and neglect of specific needs contribute to negative screening experiences. Moreover, the complex needs of disabled people impact how screening professionals perceive and respond to them, and challenges in transportation and accessibility further impede access. Tailored strategies addressing these multifaceted barriers are essential for improving the cancer screening experiences of disabled people.
Supplemental Material
Supplemental Material - Population-based cancer screening access needs of disabled people: A qualitative evidence synthesis
Supplemental Material for Population-based cancer screening access needs of disabled people: A qualitative evidence synthesis by Kumar Cithambaram, Deirdre Corby, Liz Hartnett and David Joyce, Lynn Swineburne, Kristi Egere, Sean Healy in Journal of Intellectual Disabilities
Supplemental Material
Supplemental Material - Population-based cancer screening access needs of disabled people: A qualitative evidence synthesis
Supplemental Material for Population-based cancer screening access needs of disabled people: A qualitative evidence synthesis by Kumar Cithambaram, Deirdre Corby, Liz Hartnett and David Joyce, Lynn Swineburne, Kristi Egere, Sean Healy in Journal of Intellectual Disabilities
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by the Health Service Executive, National Screening Service, Ireland.
Supplemental Material
Supplemental material for this article is available online.
