Abstract
Objectives
Increased psychological support is required to assist the long-term well-being of the adult Cystic Fibrosis (CF) population. This research aimed to identify relationships between mindfulness, psychological flexibility, and wellbeing, as well as potential mediating effects of mindfulness to increase wellbeing in adults with CF.
Methods
In a cross-sectional study, 114 (56 female, 58 male) adults with CF completed and returned a series of validated questionnaires that assessed mindfulness, psychological flexibility, and wellbeing.
Results
Participants who demonstrated better psychological flexibility also had higher levels of mindfulness and wellbeing, and similarly, those who reported higher levels of mindfulness had better wellbeing. Mindfulness subscale scores indicated additional associations. Mindfulness partially mediated the relationship between psychological flexibility and wellbeing. A second mediation model suggested that specifically ‘acting with awareness’ (i.e., a mindfulness subscale) also partially mediated the relationship between psychological flexibility and wellbeing, highlighting the significance of mindfulness within promoting wellbeing through psychological flexibility.
Discussion
This research demonstrates the importance of mindfulness in the relationship between psychological flexibility and wellbeing. The findings provide promising preliminary evidence to suggest that Acceptance and Commitment Therapy (ACT), a therapy enhancing psychological flexibility through mindfulness, to be beneficial for enhancing the wellbeing of adults with CF.
Introduction
Cystic Fibrosis (CF) is the most common life-limiting genetic disease affecting approximately 10,837 individuals in the United Kingdom (UK). 1 Following the scientific advances of cystic fibrosis transmembrane conductance regulator (CFTR) modulator therapies in recent years, many people with CF are now surviving into adulthood. The median predicted survival age for an individual with CF is 50.6 years, and 60.6% of the population are aged 16 or over. 1 As a consequence of the CF demography evolving, attention to long-term well-being and quality of life has become increasingly important. An expansion to the CF psychosocial care guidelines based on the notion of “growing older with CF” recognises the need to promote positive coping strategies to support emotional adjustment. 2
While there is much to be celebrated in the progress of CFTR modulator therapies, there remains several psychosocial challenges present for the adult CF community. These include components of wellbeing that are important to functioning and quality of life, such as: education, employment, social support, reproductive health concerns, and mental health.3,4 CFTR modulator therapies provide hope for improving physical health outcomes, yet several individuals demonstrated worsening depression or anxiety upon commencement of CFTR modulators. 5 Data suggests a global prevalence of anxiety (26.22%) and depression (12.66%) among CF patients. 6 Furthermore, the psychological implications and health risks of CF post-modulator therapies highlight the complex changes in identity that impact health behaviours and psychological wellbeing, 7 suggesting there is a need for increased and effective psychological support. Despite the physical health improvements that some will have experienced following commencement of CFTR modulator therapies, a focus needs to be placed on wellbeing and mental health with this being an emotionally challenging time for the CF community.
Promoting positive wellbeing for adults with CF is important and has been recognised in a growing body of research.8–10 Higher levels of positive mental health and wellbeing were previously associated with better physical health and health-related quality of life in adults with CF, demonstrating potential benefits for future assessment and promotion of positive wellbeing. 8 A possible approach to support positive wellbeing for the adult CF population may be through the development of mindfulness training into CF care. Mindfulness promotes wellbeing by enhancing present-moment awareness, acceptance, and non-judgmental attention, which in turn reduce rumination and emotional reactivity, promote adaptive coping, and facilitate psychological flexibility. 10 Increased mindfulness enables individuals to experience thoughts and emotions without avoidance, fostering resilience and value-driven behaviour that underpins long-term wellbeing. 11 Mindfulness-based interventions such as Mindfulness-based Stress Reduction (MBSR), Mindfulness-based Cognitive Therapy (MBCT) and Acceptance and Commitment Therapy (ACT) appear beneficial to the betterment of psychological wellbeing and quality of life in populations with chronic conditions.12,13 Additionally, informal and brief mindfulness practices are also suggested to achieve the formation of habitual mindfulness practicing, particularly for novices, and to promote a lifestyle adaptation and change through mindfulness. 14 Prior research on mindfulness within CF populations indicate that mindfulness showed significant positive associations with the quality-of-life subscales (social functioning, emotional functioning, and interpersonal relationships), and significant negative correlations with depression, anxiety, and stress. 15 Additionally, qualitative research demonstrates the emotional, physical, and psychological wellbeing benefits of formal and informal mindfulness practices, alongside a demonstrable interest for increased accessibility, education and integration of these practices into CF care.3,16 Furthermore, mindful eating moderated the relationship between emotional eating and body mass index (BMI), thus psychological interventions around mindful eating and weight regulation have been proposed to support improvement of BMI, physiological outcomes of weight, and psychological wellbeing.17,18
Mindfulness interventions, specifically ACT-based practices, have gained considerable attention in recent years when considered alongside positive wellbeing. The ACT model is constructed around the concept of psychological flexibility (i.e., the ability to seek contact with one's present experiences, including thoughts, feelings, and behaviours, alongside the likelihood of taking value-based actions 19 ). This model is established by two overarching areas: mindfulness and acceptance processes (for example, contact with the present moment and acceptance), as well as commitment and behaviour change processes (for example, committed action). Thus, ACT-based practices aim to increase psychological flexibility. Previous research outside of CF shows that psychological flexibility is significantly associated with quality of life, mindfulness, wellbeing, and psychosomatic functioning.19–21 Additionally, psychological flexibility and mindfulness may mediate the development of psychological disorders and facilitate achieving overall wellbeing. 21 Developments of internet-guided self-help interventions based on ACT show promising benefits for chronic condition populations, regarding improvements in depression, pain intensity, psychological inflexibility, mindfulness, and pain catastrophising three months after intervention. 22 While limited research has been conducted in CF, in a sample of adolescents and young adults with CF, more acceptance was related to better emotional and social functioning, and less depressive symptoms. 23 The authors concluded that accepting one's limitations imposed by CF, alongside a refinement of life goals, may positively impact wellbeing in adolescents and young adults with CF. More recently a pilot study of ACT in people with CF demonstrated statistically significant reductions in psychological distress from pre to post treatment, and reductions in cognitive fusion (i.e., rigid attachment to thoughts as truth 19 ) were associated to improvements in psychosocial functioning. 24 Significantly, the developments of CFTR modulators, the limited age samples, and the restricted effect size postulate caution on positive past data, and the continuation of research in the field.
Mindfulness-based approaches to improving wellbeing are growing, yet limited research has been conducted in a growing population of adults with CF. The present research aims to initially explore associations, and then indirect effects between psychological flexibility, mindfulness, and wellbeing in an adult CF population. We hypothesised that higher levels of wellbeing would be related to higher levels of mindfulness and psychological flexibility. Also, that higher levels of mindfulness would be associated with higher levels of psychological flexibility. Additionally, we predicted that mindfulness would mediate the relationship between psychological flexibility and wellbeing.
Methodology
Participants
One hundred and sixty, English-speaking adults living in the UK who had a confirmed diagnosis of CF were recruited into the study. One hundred and fourteen (56 female, 58 male) participants completed and returned the questionnaires. Participant demographic and medical data are presented in Table 1. Participants were recruited using a purposeful sampling method through two regional adult CF Centres in the Midlands over eight months. Recruitment occurred during routine outpatient appointments or inpatient admissions. Eligible participants were approached initially by a clinician following the “consent to contact” ethical procedure. Those interested were provided with an information sheet by the researcher, and written informed consent was obtained prior to completing the study measures. Ethical approval was granted by the University's Ethical Committee, the Health Research Authority (HRA) via an NRES Committee (REC reference: 19/NE/0183), and by each NHS Research & Development department. Data collected for REC: 19/NE/0183 had two themes, one of which focused on self-compassion 15 and the second theme focusing on mindfulness and ACT as potential interventions toward wellbeing.
Participant demographic and medical data.
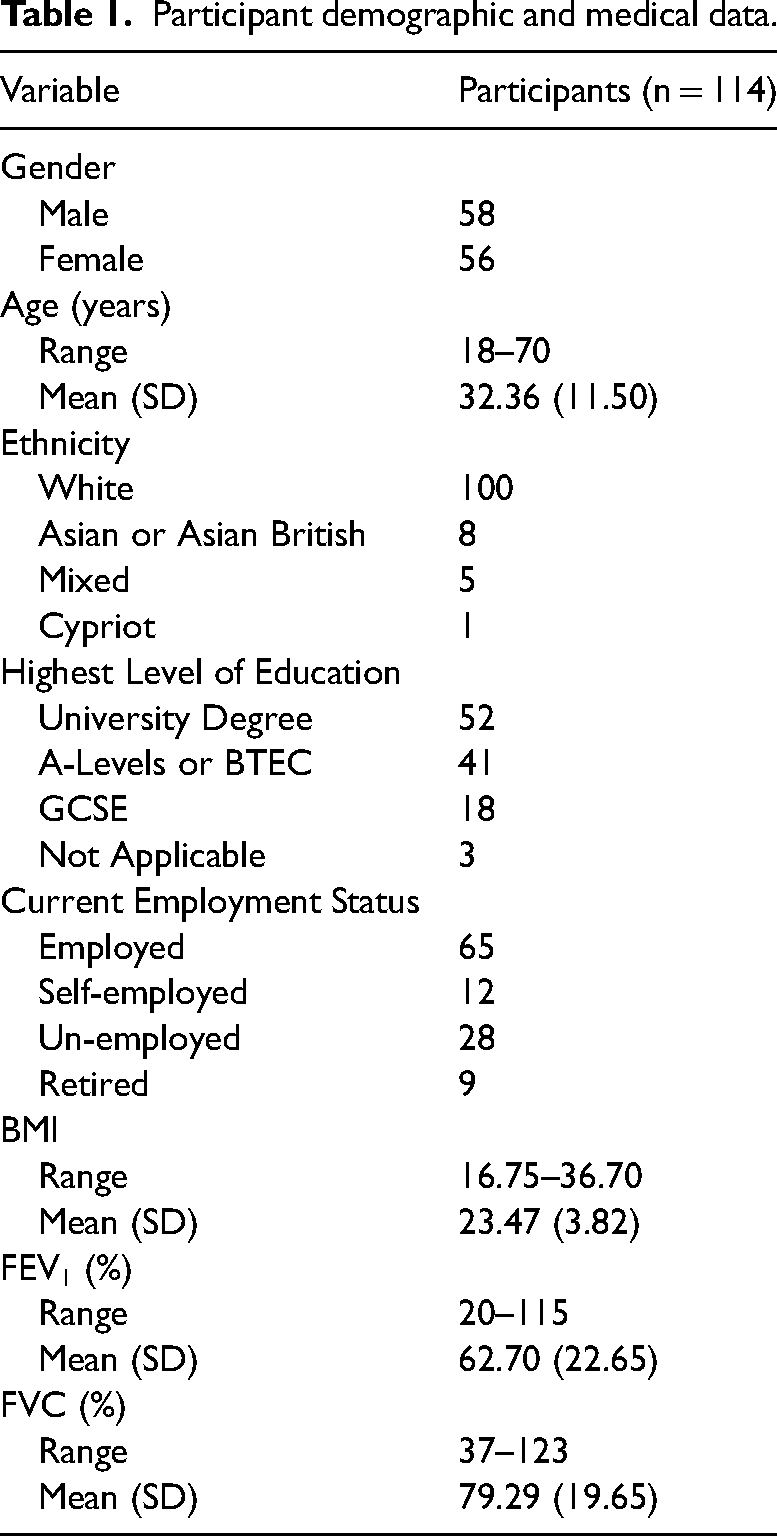
Measures
Demographic information form
Participants reported their date of birth, gender, ethnicity, highest level of education, and employment status.
Medical information form
The following information from participants’ medical records was collected: forced expiratory volume in 1 s (FEV1), forced vital capacity (FVC) and BMI.F
The Acceptance and Action Questionnaire-2 (AAQ-2) 25
The AAQ-2 is a seven-item, holistic measure of psychological flexibility (example item: “I’m afraid of my feelings”). Each item is followed by a seven-category response scale, ranging from 1 (Never true) to 7 (Always true). Total scores were calculated as the sum of the item responses, with lower scores indicating greater psychological flexibility, and higher scores indicating greater psychological inflexibility. The AAQ-2 demonstrated appropriate internal consistency, test-retest reliability, factorial validity, and discriminant validity. 25 In the present sample, Cronbach's alpha for the total score was .94.
The Five Facet Mindfulness Questionnaire: Short Form (FFMQ-SF). 26
The FFMQ-SF is a 24-item measure composed of five subscales: observe, describe, acting with awareness, non-judging, and non-reactivity (example item: “I’m good at finding the words to describe my feelings”). Each item is followed by a five-category response scale, ranging from 1 (Never or very rarely true) to 5 (Very often or always true). Total scores were calculated as the sum of the item responses, with higher scores indicating greater mindfulness. The FFMQ-SF demonstrated sufficient internal consistency, convergent and divergent validity, thus the content validity and the psychometric properties were sufficiently preserved in the short form. 26 In the present sample, Cronbach's alpha for the overall total score was .83. Cronbach's lpha for subscale total scores were: observe .75, describe .81, acting with awareness .84, non-judging .82, and non-reactivity .74.
The World Health Organization Well-Being Index (WHO-5)
The WHO-5 is a 5-item measure designed to assess wellbeing (example item: “I have felt calm and relaxed.”). Each item is followed by a six-category response scale, ranging from 0 (At no time) to 5 (All of the time). Total scores were calculated following the sum of the item responses, multiplied by 4 to obtain a percentage score, with higher scores indicating better wellbeing. The WHO-5 demonstrated very high clinical validity. 27 In the present sample, Cronbach's alpha for the total score was .90.
Procedure
The research study was initially introduced to the potential participant by a clinician at the CF centre, following the “consent to contact” ethical procedure. If agreed, the researcher provided potential participants with a verbal overview of the study procedure, followed by a participant information form. Once verbally agreed, participants provided written informed consent, completed a demographics form, that was followed by a series of questionnaires. On average, the questionnaires took 20 min to complete. The researcher subsequently collected information of participants’ medical records (FEV1, FVC, BMI) with prior participant consent, and alongside a clinician. This medical data was collected for all participants and based on the most recent recording of this data. Following completion, the participants were given a debrief form by the researcher with an overview of the study, and researchers contact details should participants decide to withdraw their data later.
Analysis
We used IBM SPSS v25 to analyse the data. Preliminary analyses examined for outliers and met assumptions of normality, linearity, and multicollinearity. 28 We computed bivariate correlations to explore associations between psychological flexibility, mindfulness, and wellbeing. The PROCESS macro (Model 4) was used to examine the direct and indirect effects of psychological flexibility on wellbeing, via mindfulness. 29 All models used a 95% bias-corrected confidence interval based on 5000 bootstrap samples, an effective method for smaller samples that is least susceptible to Type 1 errors. 30
Results
Pearson's bivariate correlations between psychological flexibility, wellbeing, and mindfulness total scores are presented in Table 2. Large significant and negative associations were observed between psychological flexibility and mindfulness (r = −.687, p < .001), as well as psychological flexibility and wellbeing (r = −.592, p < .001). Additionally, large significant and positive associations were observed between mindfulness and wellbeing (r = .526, p < .0005).
Means, standard deviations, and bivariate correlations between psychological flexibility, wellbeing, and mindfulness total scores.
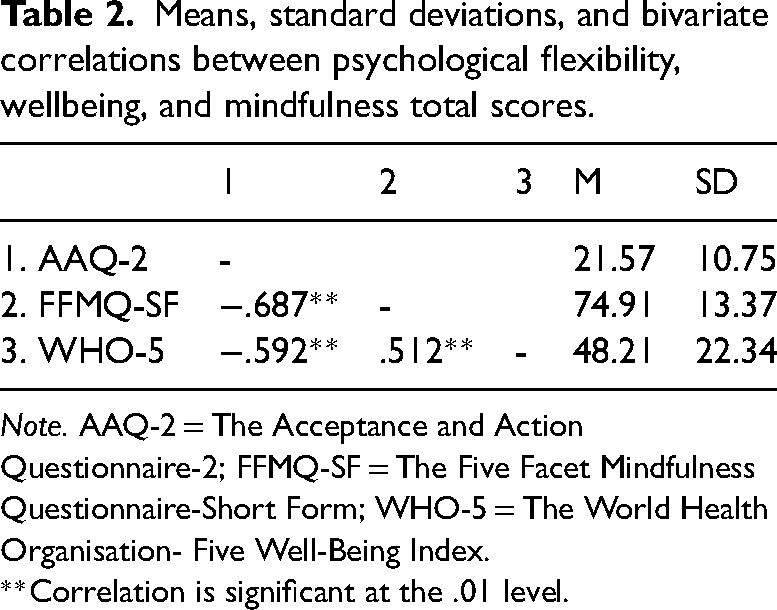

Note. AAQ-2 = The Acceptance and Action Questionnaire-2; FFMQ-SF = The Five Facet Mindfulness Questionnaire-Short Form; WHO-5 = The World Health Organisation- Five Well-Being Index.
**Correlation is significant at the .01 level.
Pearson's bivariate correlations between psychological flexibility (total scores), wellbeing (total scores), and mindfulness (subscale scores) are presented in Table 3. Findings showed significant negative associations between four mindfulness subscales (non-react, act aware, describe, and non-judge) and psychological flexibility. With significant positive associations observed between three mindfulness subscales (act aware, describe, and non-judge) and wellbeing. Mindfulness subscale intercorrelations also presented five significant positive associations between the following facets: observe and non-react, describe and observe, act aware and describe, non-judge and act aware, describe and non-judge.
Means, standard deviations, and bivariate correlations between psychological flexibility (total scores), wellbeing (total scores), and mindfulness (subscale scores).

Note. AAQ-2 = The Acceptance and Action Questionnaire-2; WHO-5 = The World Health Organisation- Five Well-Being Index; Act aware = acting with awareness; Non-judge = Non-judging of inner experience; Non-react = non-reactivity to inner experience.
**Correlation is significant at the .01 level.
*Correlation is significant at the .05 level.
In the first mediation model, psychological flexibility (AAQ-2) was entered as the predictor variable, mindfulness (FFMQ-SF) was entered as a potential mediating variable, and wellbeing (WHO-5) was entered as the outcome variable. In modern methods, mediation may still exist if one of the paths (a or b) are non-significant. 29 Total scores were used for all variables in this model. As seen in Figure 1, the c pathway indicated a significant and negative relationship between psychological flexibility on wellbeing b = −1.23, p < .001, 95%CI [−1.54, −.91], highlighting that lower psychological flexibility was associated with reduced wellbeing. This analysis confirmed that the indirect effect of psychological flexibility on wellbeing via mindfulness was significant ab = −.28, 95%CI [−.63, −.002], suggesting that mindfulness partially explains how flexibility relates to wellbeing. Path a showed that greater psychological flexibility predicted higher levels of mindfulness b = −.85, p < .001, 95%CI [−1.02, −.68], and for path b mindfulness did not significantly predict wellbeing (p = .064). Finally, pathway C’ however, remained significant b = −.94, p < .001, 95%CI [−1.38, −.51], suggesting that the relationship between psychological flexibility and wellbeing is partially mediated by mindfulness. This pattern suggests that adults with CF who are more open and accepting toward their internal experiences tend to report higher mindfulness, which in turn contributes to greater wellbeing, highlighting mindfulness as one pathway through which psychological flexibility fosters wellbeing.
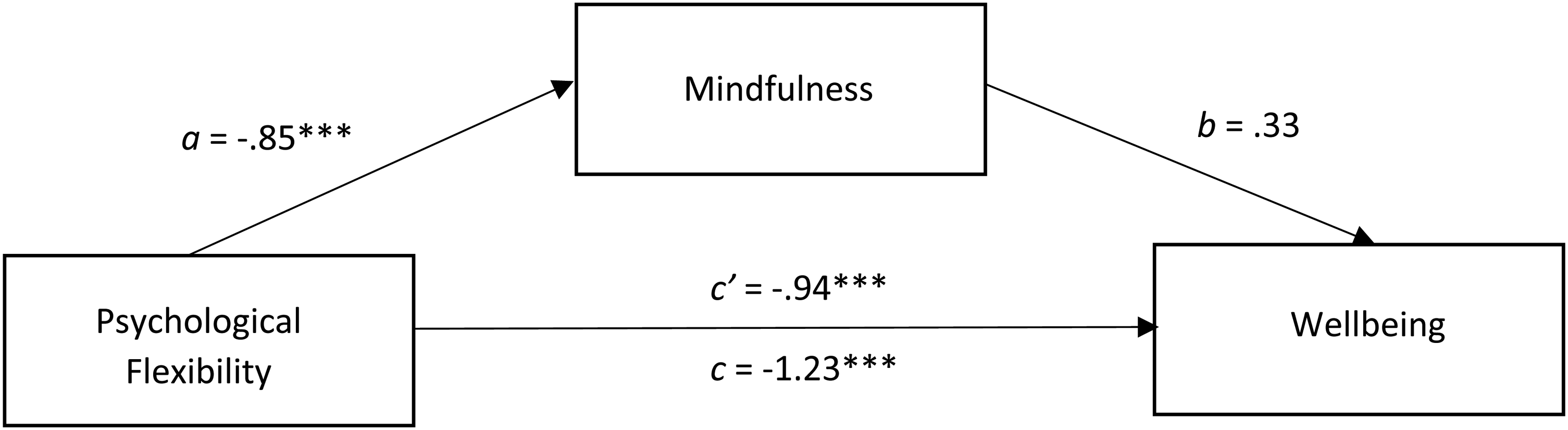
The mediating effect of mindfulness in the relationship between psychological flexibility and wellbeing. All presented effects are unstandardised; a is the effect of psychological flexibility on mindfulness; b is the effect of mindfulness on wellbeing; c’ is the direct effect of psychological flexibility on wellbeing; c is the total effect of psychological flexibility on wellbeing. * = p < .05, ** = p < .01, *** = p < .001.
In the second mediation model, psychological flexibility (AAQ-2) was entered as the predictor variable, acting with awareness (FFMQ-SF subscale) was entered as a potential mediating variable, and wellbeing (WHO-5) was entered as the outcome variable. As seen in Figure 2, the c pathway indicated a significant and negative relationship between psychological flexibility on wellbeing b = −1.23, p < .001, 95%CI [−1.55, −.91], highlighting that lower psychological flexibility was associated with poorer wellbeing. This analysis confirmed that the indirect effect of psychological flexibility on wellbeing via acting with awareness was significant ab = −.22, 95%CI [−.44, −.002]. Path a showed that greater psychological flexibility predicted higher levels of acting with awareness b = −.24, p < .001, 95%CI [−.30, −.17], and path b showed that acting with awareness predicted higher wellbeing b = −.91, p < .05, 95%CI [.01, 1.80]. Finally, pathway C’ however, remained significant b = −1.02, p < .001, 95%CI [−1.39, −.64], suggesting that the relationship between psychological flexibility and wellbeing is partially mediated by acting with awareness. This pattern implies that adults with CF who demonstrate greater awareness of their actions tend to experience higher wellbeing, partly because such awareness supports the flexible regulation of thoughts and emotions in daily life.
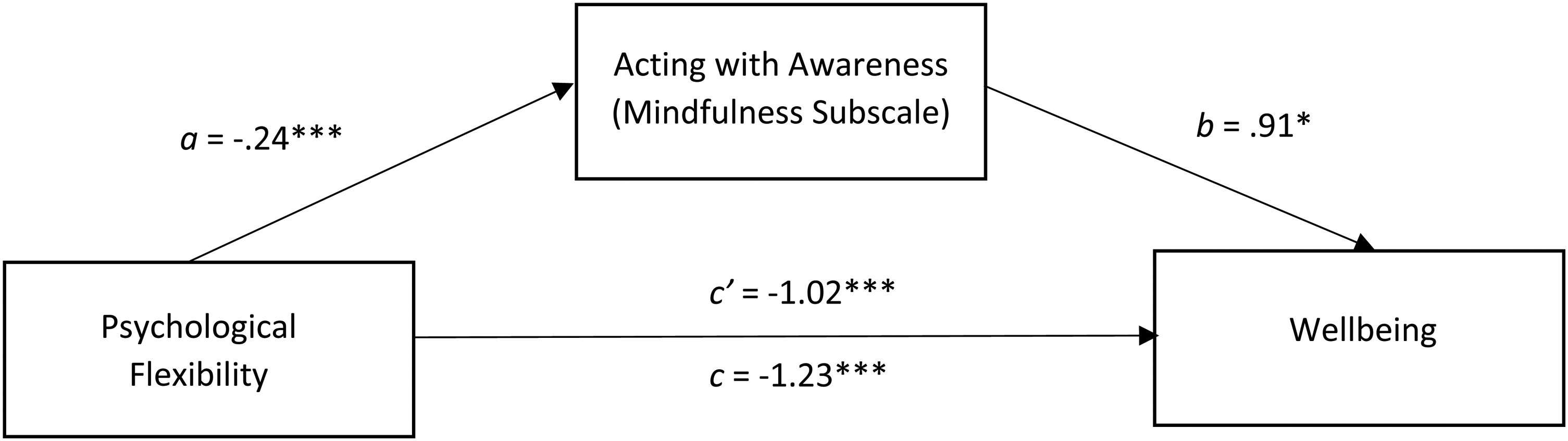
The mediating effect of acting with awareness (mindfulness facet) in the relationship between psychological flexibility and wellbeing. All presented effects are unstandardised; a is the effect of psychological flexibility on acting with awareness; b is the effect of acting with awareness on wellbeing; c’ is the direct effect of psychological flexibility on wellbeing; c is the total effect of psychological flexibility on wellbeing. * = p < .05, ** = p < .01, *** = p < .001.
In the third mediation model, psychological flexibility (AAQ-2) was entered as the predictor variable, describe (FFMQ-SF subscale) was entered as a potential mediating variable, and wellbeing (WHO-5) was entered as the outcome variable. Similarly, in the fourth mediation model, psychological flexibility (AAQ-2) was entered as the predictor variable, non-judging of inner experience (FFMQ-SF subscale) was entered as a potential mediating variable, and wellbeing (WHO-5) was entered as the outcome variable. Only significant direct effects were observed in both models, indirect effects were not identified, resulting in direct-only non-mediations as described by Zhao and colleagues. 31 These results indicate that, although psychological flexibility remains a strong predictor of wellbeing, the specific mindfulness components of describing and non-judging of inner experience do not appear to account for this relationship in adults with CF. This suggests that not all mindfulness facets contribute equally to wellbeing within this population, highlighting the potential importance of acting with awareness as a more influential mindfulness process.
The final two subscales of the FFMQ-SF (observe, and non-reactivity to inner experience) were not used as potential mediators due to individual insignificant correlations with the outcome variable WHO-5.
Discussion
The present study explored associations and indirect effects between psychological flexibility, mindfulness, and wellbeing in adults with CF. The findings indicate that adults who demonstrated greater psychological flexibility and mindfulness also reported higher wellbeing, and that mindfulness partially mediated the relationship between psychological flexibility and wellbeing. Specifically, the “acting with awareness” facet of mindfulness played a significant mediating role.
This study is the first to provide insight into the relationships and indirect effects between psychological flexibility, mindfulness, and well-being in adults with CF. Outside of CF research, and in line with the present findings, psychological flexibility was also significantly associated with mindfulness and wellbeing.19–21 Prior literature further supported associations found between mindfulness and wellbeing. 16 Extending this evidence to adults with CF provides novel empirical support for mindfulness and acceptance-based approaches within this population. The mediation effects observed suggest that mindfulness contributes to wellbeing partly by enhancing psychological flexibility, helping individuals to remain present and act in accordance with personal values despite physical and emotional challenges. This reinforces the theoretical assumption that psychological flexibility serves as a central mechanism linking mindfulness to positive mental health outcomes. 32 Furthermore, within CF research, findings from the current study aligned with research that explored related concepts to psychological flexibility and wellbeing,22–24 explained through the impact of mindfulness.
With increasing psychological complexities prevalent in CF adulthood years,3,7 it is imperative to explore possible approaches and inform future psychological interventions that could strengthen and improve the psychological resilience, health, and wellbeing of the adult CF population. Therefore, based on the present study results we propose that psychological interventions based on ACT and mindfulness practices may be a way forward to support emotional adjustment in an era of increasing life expectancy for CF populations. Internet-based self-help tools based on ACT and mindfulness approaches as previously researched by Trompetter et al. 22 in chronic populations may also provide a feasible and effective method to promoting positive wellbeing in people with CF due to infection prevention and control guidelines.
Three limitations were identified within this study. The first limitation is that the study did not account for previous, or current, engagement in mindfulness-based interventions. Knowledge of this would have allowed for stronger conclusions to be drawn. Secondly, the study presents cross-sectional data, which makes it difficult for identified associations to be interpreted in any greater detail. Although this was needed as a first step to identify the relationships between psychological flexibility, mindfulness, and wellbeing, as well as the mediating role of mindfulness in adults with CF, future research could emphasise the role of acting with awareness in ACT-based interventions. Finally, the study did not confirm how many individuals were using CFTR therapies. It is important to consider that data collection was conducted prior to the availability of the newest CFTR therapy (Kaftrio) via the NHS, it would therefore be interesting to replicate this study today with 90% of the UK CF population eligible for CFTR therapies.
In combination with the present findings demonstrating the importance of mindfulness in the relationship between psychological flexibility and wellbeing, and prior research highlighting the benefits of brief and accessible mindfulness interventions. 14 These findings could be used to inform, create, and trial brief mindfulness interventions to be used within a holistic self-care practice for adults with CF, and to support CF clinical teams with flexible psychological practices that could be easily suggested to patients.
Overall, this study makes a unique contribution by being among the first to quantitatively examine the interrelationships between mindfulness, psychological flexibility, and wellbeing in an adult CF population. The findings highlight mindfulness, particularly acting with awareness, as a potential mechanism through which psychological flexibility influences wellbeing, providing a theoretical and empirical foundation for developing ACT- and mindfulness-based interventions tailored to CF care. In an era of CFTR modulator therapies, the current findings provide promising preliminary evidence to suggest that mindfulness-based interventions may be beneficial for supporting the positive wellbeing for adults with CF.
Footnotes
Availability of data and material
The data that support the findings of this study are available on request from the corresponding author.
Consent to participate and publish
Informed written consent was obtained from all individual participants prior to participation. The authors affirm that participants provided informed consent for publication.
Contributorship
SK, HE, MM, RK researched literature, conceived the study and were involved in protocol development and gaining ethical approval. SK conducted patient recruitment, data analysis, and wrote the initial manuscript. HE, MM, RK critically reviewed and edited the manuscript. All authors reviewed and edited the manuscript and approved the final version of the manuscript.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethics approval
The study was approved by the Ethical Review Board of the University (3123 /R(C) /2019 /Mar /BLSS FAEC), and the Health Research Authority (HRA: REC reference: 19/NE/0183), and with the 1964 Helsinki Declaration and its later amendments. This manuscript does not contain any studies with animals.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
