Abstract
Lebanon has faced a series of overlapping crises, including a severe financial collapse, the pandemic, the Beirut port explosion, the removal of subsidies, electricity shortages, and, most recently, the war in Lebanon. These events have disrupted supply chains, led to currency devaluation, damaged infrastructure, and generated market instability, ultimately resulting in critical medicine shortages, price volatility, and reduced availability of essential pharmaceuticals. These crises’ compounded effects have placed immense pressure on the healthcare system and heightened population reliance on generic medicines. This study maps the pathways linking multiple crises to medicine access challenges, highlighting both direct and indirect impacts on the pharmaceutical supply. Using a structured framework, we identify key vulnerabilities and the resulting adaptations in healthcare provision. Central to the response is the strategic promotion of generic medicines as a resilience mechanism to mitigate shortages and maintain treatment continuity. Findings underscore the importance of proactive, system-level strategies to buffer health systems against multifactorial shocks. By integrating crisis mapping with targeted interventions, policymakers and healthcare providers can enhance preparedness, ensure the availability of medicine, and strengthen resilience in the face of ongoing socio-political and economic instability. This approach offers a practical model for other regions facing compounded crises that impact healthcare access.
Keywords
Introduction
Prolonged conflict and crises have left Lebanon’s healthcare system strained to its limits, confronting challenges that threaten its very survival.1,2 Several overlapping challenges have recently emerged (Figure 1), overshadowing the nation’s once-shining reputation as a medical care leader in the Middle East, which has drawn patients from across the region for medical tourism.
2
During the 2019 financial crisis, access to foreign exchange was limited, and the currency began to devalue, resulting in a decline in purchasing power.
3
Institutions already facing difficulties were now faced with demands that were previously unheard of, as a result of the coronavirus outbreak.2,4 While neighboring conflicts further destabilized trade lines, the 2020 Beirut port explosion caused disruptions to supply systems. One of the most obvious consequences of this unstable storm was the disruption of the supply of medications. Patients frequently found themselves unable to continue treatment for chronic or life-threatening disorders, pharmacies were unable to fulfill all patients’ needs, and hospitals had to cut back on services.4,5 Impact of intersecting crises in Lebanon on generic reliance.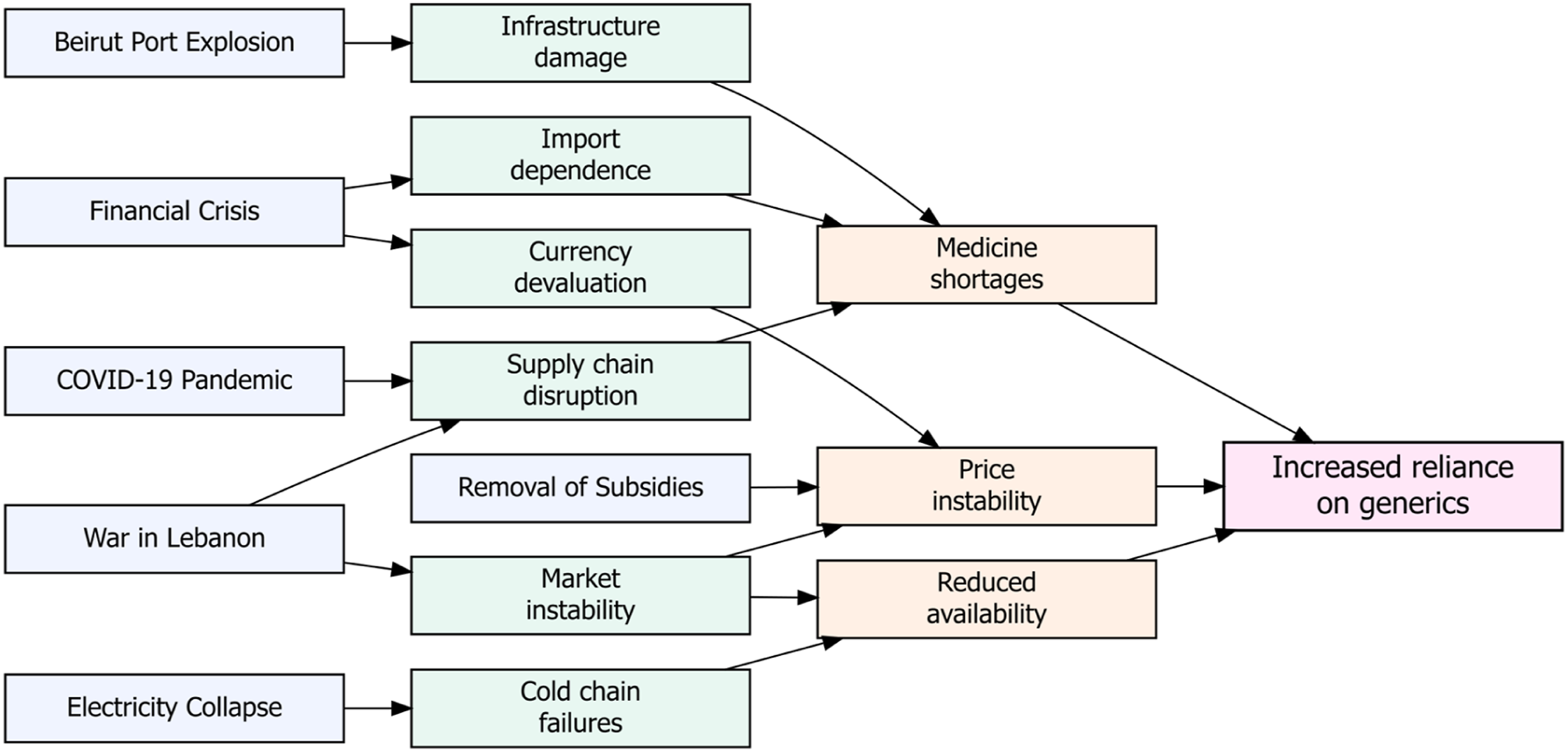
In light of this, generic medications become both a lifeline and a source of contention. When branded medications were unavailable, they were the sole accessible and reasonably priced option for many patients.6,7 In a market that was imploding, generics were the only way for local producers to survive. They served as a brittle stand-in for missing imports for wholesalers and pharmacies. Deep inconsistencies were also made clear by the Lebanese experience, though, as generics addressed pressing needs while simultaneously exposing flaws in the country’s production capacity, regulatory framework, and public confidence.8,9 Therefore, the implications of generics in Lebanon extend beyond medications; they also concern patients, companies, and institutions navigating one of the most precarious pharmaceutical environments in the world.
The Lebanese pharmaceutical system before the crises
Before 2019, Lebanon’s pharmaceutical sector appeared outwardly strong but was built on fragile foundations, relying on imports for around 95% of products. 10 As a result, multinational corporations dominated the Lebanese market. Branded products were the norm, physicians overwhelmingly prescribed them, patients equated them with quality, and marketing relationships reinforced the cycle.10,11 Branded generics accounted for 19% of the overall Lebanese drug market (10% locally produced and 9% imported). 12 Local manufacturers, such as Benta Pharma, Pharmaline, Pharmadex, and Algorithm, supplied only about 10% of the market in 2018 (rising to 30% in 2024), 13 focusing on lower-cost generics for common conditions. 14 Public confidence in these products was modest, and their role remained secondary.
This dependence on imports made Lebanon uniquely vulnerable. When the Lebanese pound collapsed, losing over 90% of its value, importers could no longer pay suppliers abroad.15,16 State subsidies, once critical for offsetting costs for patients, were withdrawn. By mid-2021, reports of shortages spanned the entire spectrum of care, including insulin, chemotherapy medications, antibiotics, and psychiatric medications for long-term treatment.4,17 Families lined up outside pharmacies for hours, often leaving empty-handed. Social media became a platform for desperate appeals, with patients asking friends abroad to send them essential drugs. 18
Generics between promise and distrust
In this vacuum, generics became the country’s fallback solution. The Ministry of Public Health promoted their use as substitutes for unavailable branded medicines. Pharmacies were granted more flexibility to substitute prescriptions, and new generic products were expedited for approval. 11 Local manufacturers attempted to scale up production despite enormous obstacles, including shortages of raw materials, electricity blackouts, and rising costs of imported packaging.10,14
Generics offered immediate relief, but they also carried baggage. For decades, Lebanese patients had associated generics with lower quality, and physician prescribing habits reflected this skepticism.11,19 A study conducted before the crisis showed that more than 70% of Lebanese doctors preferred to prescribe branded drugs, 19 citing doubts about efficacy and adherence. These attitudes did not vanish during the crisis. Even when faced with shortages, many patients resisted substitution, while others accepted generics reluctantly.
The rapid approval of generics during the crisis also raised questions. Fast-tracking increased availability, but some health professionals worried that regulatory shortcuts compromised quality. Rumors of counterfeit and substandard drugs circulated widely, sometimes amplified by media reports, further eroding public confidence. Thus, the very measures that allowed generics to gain ground also risked undermining their legitimacy.
Experiences on the ground
The contradictions surrounding generics played out in daily struggles. Insulin shortages, for example, forced many patients to ration their doses, cutting injections in half or skipping them altogether.7,20 Local producers explored the possibility of biosimilar insulin, but the lack of biotechnological capacity made this impossible. In oncology, dangerous interruptions in chemotherapy treatments were documented.17,21 Local generics filled only a fraction of the gap, leaving many cancer patients without viable options.
Other therapeutic areas, such as antibiotics, cardiovascular drugs, and psychiatric medications, saw a greater reliance on generics.7,10 Yet even in the aforementioned case, supply was inconsistent. Patients reported being able to find a generic for a period, only to face shortages the next. For chronic disease management, this inconsistency was devastating: blood pressure treatments, antidepressants, 22 and epilepsy medications cannot simply be taken sporadically without health consequences. Families often resorted to informal networks, smuggling, or donations from the diaspora to secure what the market could not provide. 23 Generics, then, were simultaneously indispensable and unreliable, reflecting Lebanon’s fractured local pharmaceutical ecosystem.
Local realities in global perspective
Lebanon’s case is part of a broader pattern. In fragile states around the world, generics often become the default solution when economic collapse or political conflict undermines access to branded medicines. In Syria, international sanctions and war have disrupted imports, leading to a reliance on local generics.24,25 In Venezuela, hyperinflation and the breakdown of supply chains created a similar dependence, with patients turning to generics in the absence of imports.26,27 Both cases mirrored Lebanon’s challenges, where generics offered continuity but were limited by capacity constraints and undermined by public distrust.
By contrast, neighboring countries like Jordan and Egypt highlight what Lebanon lacked, namely, resilient local industries capable of sustaining generics production at scale. Egypt’s large generics sector, supported by state investment and regional exports, allowed it to weather economic shocks while maintaining relatively steady access for its population.28,29 Jordan’s emphasis on pharmaceutical exports and regulatory rigor has helped position its generics industry as a source of national strength.30,31 These comparisons, among others, highlight that generics can stabilize fragile systems, but only when supported by robust manufacturing, effective regulation, and public trust.
Lessons for the future
Lebanon’s reliance on generics during crisis years offers sobering lessons. The country demonstrated that generics can indeed provide vital stopgaps when imports collapse. However, it also demonstrated that without trust, infrastructure, and stability, generics alone cannot ensure continuity of care. The Lebanese case highlights the danger of building a pharmaceutical system on import dependence, the difficulty of changing prescribing habits and patient perceptions under stress, and the risks of prioritizing speed over quality in regulation.
More broadly, Lebanon illustrates the blurred line between health and business in fragile contexts. For local manufacturers, pharmacies, and distributors, generics were not simply a matter of patient care; they were the foundation of survival in an economy where every sector was under siege. In such environments, business strategies and public health imperatives converge: resilient supply chains, transparent quality assurance, and patient trust become simultaneously commercial priorities and public goods. In the later stages of overlapping national crises, moving beyond emergency coping strategies toward structural resilience is essential. Our framework highlights five interconnected strategies (Figure 2). First, diversifying medicine import sources and supporting regional procurement mechanisms reduces dependence on a single currency or supply route. Second, strengthening local pharmaceutical production, particularly for essential generics, buffers against global supply shocks. Third, establishing a national strategic stockpile for chronic-disease medications mitigates risks associated with sudden port disruptions or changes in subsidy policy. Fourth, sustained investments in electricity and cold-chain infrastructure ensure the quality of drugs during prolonged outages. Fifth, implementing transparent pricing policies combined with digital monitoring of shortages can prevent panic buying, ensure fair distribution, and support long-term market recovery. Collectively, these measures transition the system from reactive crisis management to proactive resilience building. Proactive approach to pharmaceutical stability in overlapping crises.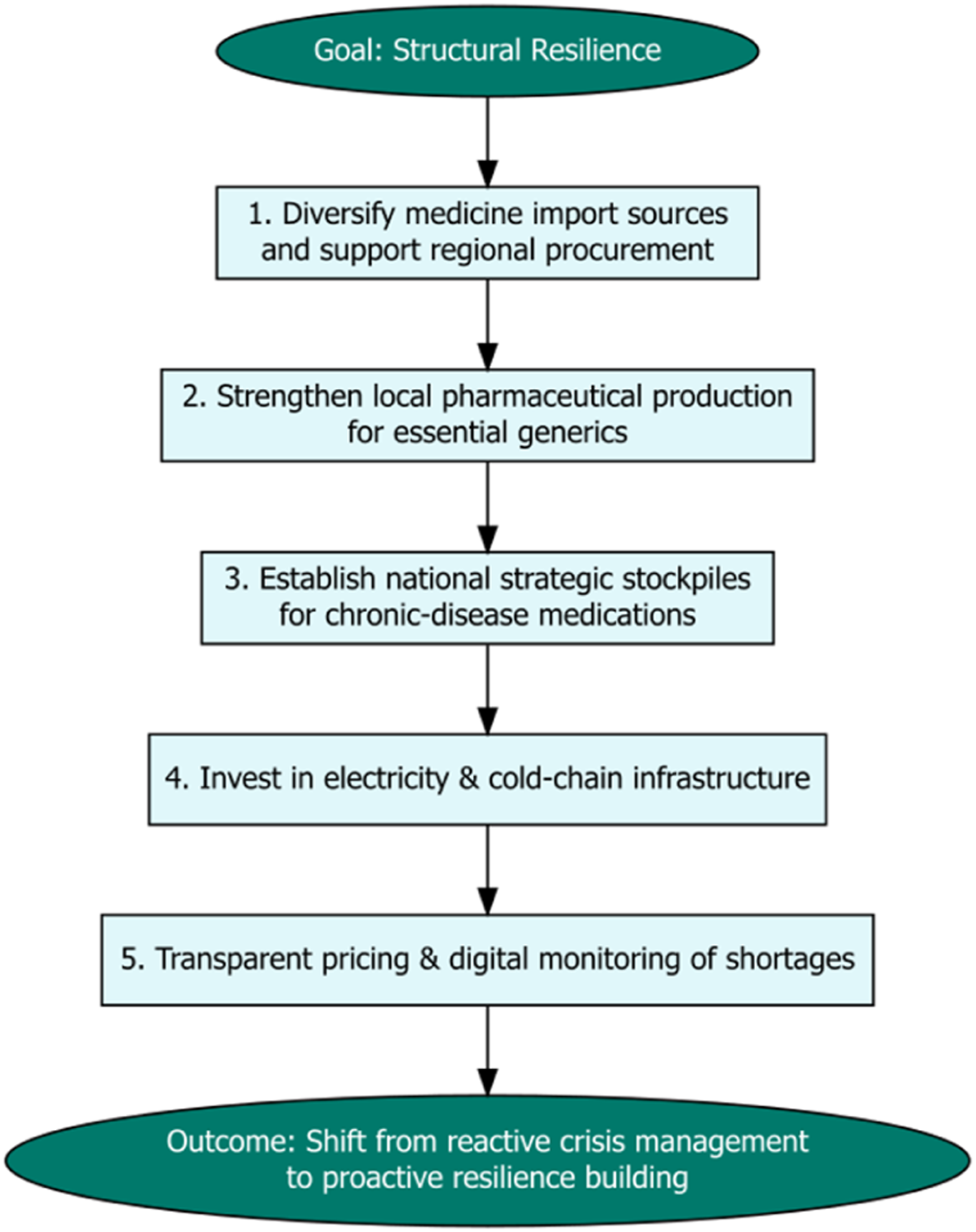
In Lebanon’s ongoing crises, ensuring access to generic medicines requires targeted strategies (Figure 3). First, diversifying import sources and engaging regional procurement networks reduces vulnerability to currency fluctuations and global supply shocks. Second, scaling up local production of essential generics strengthens self-sufficiency and mitigates reliance on imports. Third, establishing strategic stockpiles of high-demand chronic medications can buffer sudden shortages. Fourth, investments in storage infrastructure and cold chains ensure the quality of medicine during prolonged outages. Fifth, implementing transparent pricing policies and digital monitoring enables equitable distribution, discourages hoarding, and supports market stability. Together, these strategies create a system that is resilient to both economic and logistical shocks, while prioritizing patient access to essential generics. Strategies to secure generic medicine availability in crises.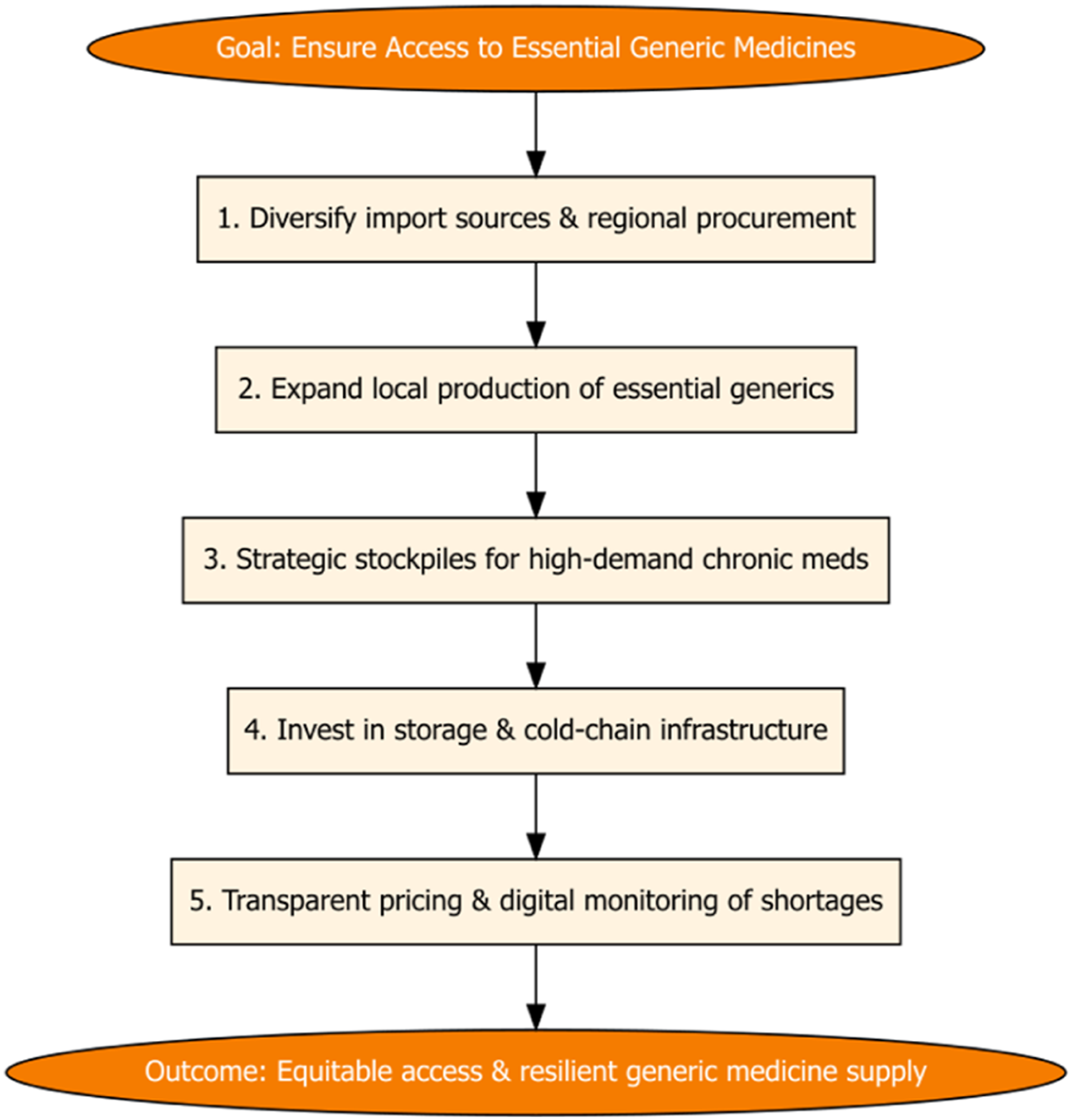
Conclusion and perspectives
Generic medicines played an imperative role during Lebanon’s struggle to preserve access to healthcare during the crisis. They offered immediate affordability when imports collapsed, yet they also exposed deep systemic weaknesses. For patients, they were a lifeline that was too often inconsistent. For providers, they were substitutes that sometimes came with skepticism. For manufacturers, they were both an opportunity and a near-impossible challenge. Lebanon’s experience, when placed in a regional and global perspective, reminds us that generics are never just cheaper alternatives. In fragile systems, they embody the intersection of health, trust, and economic survival. Their story in Lebanon is ultimately one of resilience under duress, and of the limits of substitution when institutions themselves are failing.
The role of generic medicines in Lebanon during periods of conflict and crisis embodies a paradox that deserves closer scrutiny. On the one hand, generics are promoted globally as a cornerstone of equitable healthcare: they lower treatment costs, expand access, and ensure continuity of care when branded drugs are unaffordable. Yet in Lebanon, where economic collapse, political instability, and supply chain disruptions intersect, the story is more complex. While generics often serve as the only viable option for patients who can no longer afford branded medications, their availability is not always guaranteed, and their acceptance among both patients and physicians remains uneven. This raises important scientific and societal questions. If generics are meant to be the “safety net” of pharmaceutical systems, why do shortages persist during crises in Lebanon? Are these shortages due to global supply chain fragilities, local manufacturing limitations, or deliberate policy gaps? And why, despite their proven bioequivalence, do patients in Lebanon frequently perceive generics as inferior, while in many European countries they are considered fully interchangeable?
Globally, evidence shows that generics account for more than 80% of prescriptions in the United States and between 17 and 83% the European Union. 32 By contrast, in Lebanon, their market penetration is significantly lower, hindered by skepticism, weak branding, and inconsistent regulatory enforcement. Should we therefore question whether the global model of generic adoption is truly transferable to fragile states under conflict? Or does Lebanon’s case highlight deeper issues of trust between institutions, in regulatory bodies, and in the healthcare system itself, that cannot be solved merely by offering cheaper alternatives?
Perhaps the contradiction lies in the dual identity of generics: globally celebrated as agents of survival and access, but locally entangled in doubts, shortages, and inequities. Can generics live up to their promise in environments where governance is weak and pharmaceutical dependence on imports is high? Or must we rethink how “generic policy” is designed for contexts of instability, moving from a cost-saving strategy to a resilience-building tool for health systems?
Footnotes
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
