Abstract
Severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) is still a global concern with high morbidity and mortality rates. The role of endothelial cells in the progress of COVID-19 is well established. Therefore, the current study aimed to measure the endothelial markers and their correlation with the hematological parameters in intensive care unit-admitted COVID-19 patients. This study involved 111 adult participants, including 55 ICU-admitted patients with COVID-19 and 56 healthy controls. Levels of E-selectin, ICAM-1, and VCAM-1 in the plasma of the study participants were measured and correlated with hematological parameters. The study demonstrates that COVID-19 patients admitted to the ICU have higher levels of E-selectin, ICAM-1, and VCAM-1 compared to healthy controls (p < .05). These elevated levels can serve as reliable indicators of endothelial dysfunction and early markers for the detection and prediction of endothelial cell involvement in COVID-19 complications. The findings of this study suggest that increased levels of E-selectin, VCAM-1, and ICAM-1 in patients with COVID-19 are indicative of the participation of endothelial cells in the pathogenesis of COVID-19 complications. Consequently, these endothelial markers are proposed as potential early indicators for predicting the severity of COVID-19.
Keywords
Introduction
The global impact of the COVID-19 pandemic caused by SARS-CoV-2 continues to be a significant concern, both in terms of public health and the economy, due to its high rates of morbidity and mortality.1,2 According the World Health Organization (WHO), as of December 28, 2022, there have been over 651 million confirmed cases of COVID-19 and more than 6.6 million deaths attributed to the disease. 3 Most COVID-19 patients either exhibit no symptoms or experience mild flu-like symptoms, resembling a common infection. However, approximately 20% of patients develop viral pneumonia, and around 5% progress to acute respiratory distress syndrome.1,4 Moreover, the pathophysiological mechanism of COVID-19 involves a diverse range of responses, including inflammatory and cytokine storms, as well as endothelial damage or activation. Additionally, patients may experience complications such as disseminated intravascular coagulopathy (DIC), thrombosis, and cardiovascular and cerebrovascular issues.4–6
The vascular endothelium plays a critical role in maintaining vascular homeostasis, which encompasses functions such as regulating vascular tone, hemostasis, and responding to injuries. Consequently, the activation and damage of the vascular endothelium are pivotal in the development of COVID-19, contributing to coagulopathy and an elevated risk of thrombotic events. 7 Multiple factors, including the SARS-CoV-2 virus, platelets, neutrophils, and hypoxemia, have been identified as important contributors to endothelial activation and inflammation. In order to assess the activation or damage of endothelial cells, specific markers expressed by activated endothelial cells, namely endothelial leukocyte adhesion molecule-1 (E-selectin), intercellular adhesion molecule-1 (ICAM-1), and vascular cell adhesion molecule-1 (VCAM-1), can be utilized.8–10 The levels of these endothelial markers (E-selectin, ICAM-1, and VCAM-1) have been linked to the severity of COVID.8,11–14
Complete blood count (CBC) parameters and CBC-calculated parameters, such as the neutrophil-to-lymphocyte ratio (NLR), platelet-to-lymphocyte ratio (PLR), platelet-to-neutrophil ratio (PNR), and mean platelet volume to platelet count ratio (MPR), are useful indicators for diagnosing and predicting the severity and prognosis of COVID-19.15–18 Furthermore, elevated NLR, PLR, and MPR values were observed in COVID-19 patients who passed away (PA) in the intensive care unit (ICU) compared to COVID-19 patients who were discharged (DC) from the ICU.18,19
Therefore, this study aims (i) to assess the levels of soluble endothelial markers, specifically E-selectin, ICAM, and VCAM, in the plasma of COVID-19 patients who were either DC from ICU or PA in the ICU and compare overall COVID-19 patients to healthy controls (ii) to correlate soluble endothelial markers levels with CBC parameters including neutrophils, platelets, D-dimer, and CBC-calculated parameters (iii) to investigate the association between the soluble endothelial markers, CBC parameters, CBC-calculated parameters, coagulation profiles, and the clinical outcome of COVID-19.
Materials and methods
Patient recruitment
A total of 111 adult participants were enrolled in this study. Among them, 55 individuals were COVID-19 patients who were admitted to ICU, while the remaining 56 participants served as healthy controls (23 male and 14 female). The COVID-19 patients (patient group) were admitted to Baish General Hospital in the Jazan region of Saudi Arabia and were diagnosed using real time-polymerase chain reaction (RT-PCR). Out of the 55 ICU-admitted COVID-19 patients, 28 were DC patients from the ICU, while 27 PA patients while in the ICU. The study collected samples were randomized, excluding all ICU-admitted patients who did not have COVID-19. The healthy controls (control group) were individuals who regularly donated blood, tested negative for COVID-19, exhibited normal hematological parameters, and had a negative status for transfusion-transmitted infections.
Sample collection
Venous blood samples were obtained from both patients and healthy controls using vacutainer tubes containing ethylenediaminetetraacetic acid (EDTA) and sodium citrate anticoagulants. The EDTA tubes were utilized for CBC analysis, while the sodium citrate tubes were used to assess soluble endothelial markers, coagulation profiles, and D-dimer levels. The blood samples from the patient group were collected upon their admission to the ICU based on the Saudi admission criteria. 20
Plasma preparation
The citrated tubes were subjected to centrifugation at 3000 r/min for 30 min at a temperature of 22°C to obtain platelet-free plasma (PFP). The PFP was divided into separate aliquots and promptly used for coagulation profiles and D-dimer measurements or stored −80°C for subsequent analysis of soluble endothelial cell markers.
Complete blood count
The CBC was assessed utilizing the Sysmex XN-550 Hematology Analyzer (manufactured by Sysmex, Kobe, Japan).
Coagulation profiles and D-dimer measurement
The coagulation profiles, which included measurements of prothrombin time (PT) and activated partial thromboplastin time (aPTT), as well as D-dimer levels, were determined using the Stago compact analyzer (manufactured by Diagnostica Stago, Asnieres sur Seine, France).
Complete blood count–calculated parameters
The CBC–calculated parameters were NLR, PLR, PNR, and MPR. These parameters were calculated as previously described.18,19,21
Measurement of endothelial cell markers
The plasma samples obtained were utilized to analyze the levels of soluble endothelial markers, namely E-selectin (using the Human E-selectin ELISA kit from MyBioSource), ICAM-1 (using the Human ICAM ELISA kit from MyBioSource), and VCAM-1 (using the Human VCAM ELISA kit from MyBioSource) in the PFP. These analyses were carried out following the manufacturer's instructions and procedures.
Ethical considerations
This study received approval from the Jazan Health Ethics Committee, Ministry of Health, Saudi Arabia, under the Reference number 2053. The committee granted permission to waive the requirement for informed consent. The study was conducted in accordance with the Declaration of Helsinki.
Statistical analysis
The statistical analysis was conducted utilizing GraphPad Prism software (version 8.0; San Diego, USA). For normally distributed data, the difference between the groups was assessed using an independent unpaired t test, while for non-normally distributed data, the Mann-Whitney test was employed. Spearman correlation analysis was used to investigate correlations. A significance level of p < .05 was considered statistically significant. The data are presented as median ± (IQR).
Results
Demographic data and comorbidities
Comparison of demographic characteristics, complete blood count (CBC) and CBC-calculated parameters between discharged ICU-COVID-19 patients and passed away ICU-COVID-19.

Abbreviations: DC: discharged; PA: passed away; WBC: white blood cells; RBC: red blood cells; Hb: hemoglobin; HCT: hematocrit; MCV: mean cell volume; MCH: mean cell hemoglobin; MCHC: mean cell hemoglobin concentration; RDW: red blood cell distribution width; MPV: mean platelet volume; ANC: absolute neutrophil count; ALC: absolute lymphocyte count; AMC: absolute monocyte count; AEC: absolute eosinophil count; EBC: absolute basophil count; NLR: neutrophil to lymphocyte ratio; PLR: platelet to lymphocyte ratio; PNR: platelet to neutrophil ratio; MPR: mean platelet ratio (mean platelet volume to platelet count ratio).
Comorbidities among patient group.

DM: diabetes mellitus, HTN: hypertension, *other clinical conditions than DM and HTN such as cardiovascular disease or liver or kidney disease.
Complete blood count
Comparison between patients and controls
The overall analysis of CBC showed statistically significant differences between the ICU-admitted COVID-19 patients and healthy controls (Supplementary Table 1). Specifically, in the patient group, the white blood cell (WBC) count, absolute neutrophil count (ANC), and red cell distribution width (RDW) were significantly higher compared to the control group (p < .0001). Conversely, the patient group exhibited significantly lower levels of red blood cell (RBC) count, hemoglobin (Hb), hematocrit (HCT), mean cell hemoglobin (MCH), mean cell hemoglobin concentration (MCHC), platelets, absolute eosinophil count (AEC) and absolute basophil count (ABC) as compared to the control group (p < .05) (supplementary Table 1).
Comparison between PA and DC patients with COVID-19
The results revealed that the PA patients had significantly higher WBC count, and ANC and significant low RBC count, Hb, HCT, platelet count, and absolute lymphocyte count (ALC) as compared to the DC patients (p < .05; Table 1).
Complete blood count–calculated parameters
The comparison between the control group and the patient group showed significantly higher NLR and PLR and significantly lower PNR in the patient group (p < .05; supplementary Table 1). On the other hand, comparing PA patients to DC patients, revealed significantly higher NLR and significantly lower PNR in PA patients (p < .05;Table 1).
Coagulation profile and D-dimer
Coagulation profile and D-dimer results of patients and control groups.

Soluble endothelial markers
Circulating endothelial markers patients and control groups.

Correlation study
Correlation of E-selectin with WBC, ANC group.
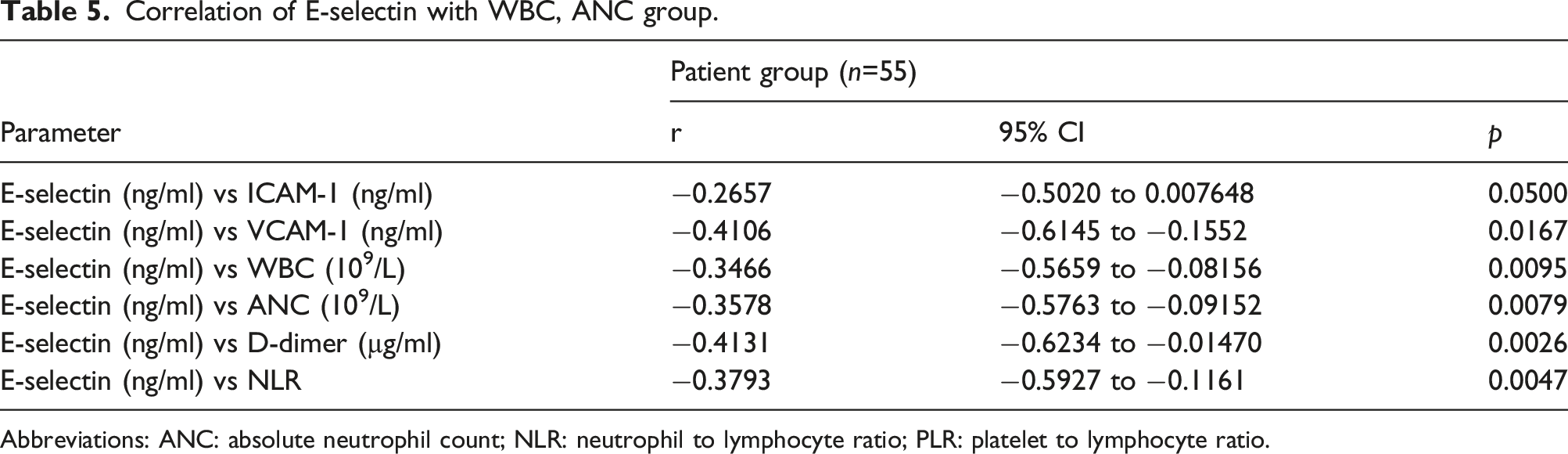
Abbreviations: ANC: absolute neutrophil count; NLR: neutrophil to lymphocyte ratio; PLR: platelet to lymphocyte ratio.

Correlation of E-selectin with ICAM-1, VCAM-1, white blood cells, absolute neutrophil count, D-dimer and neutrophil-to-lymphocyte ratio in the patient group. Abbreviation: ICAM-1: intercellular adhesion molecule-1, VCAM-1: vascular cell adhesion molecule-1, WBCs: white blood cells, ANL: absolute neutrophil count, D-dimer and NLR: neutrophil-to-lymp: ocyte ratio.
Association between baseline variables and COVID-19 mortality
Association between baseline variables and mortality among COVID-19 patients admitted to the intensive care unit.
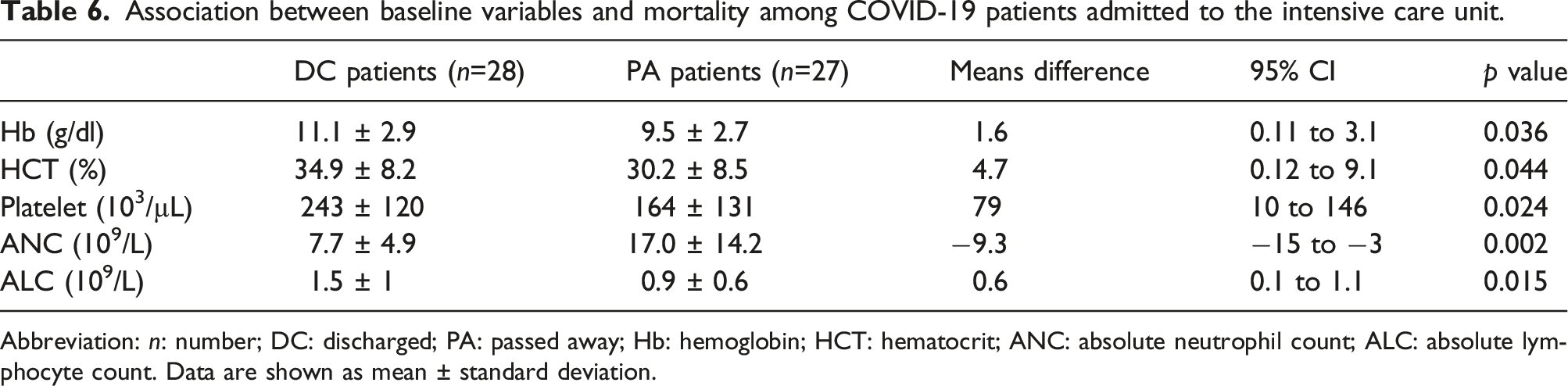
Abbreviation: n: number; DC: discharged; PA: passed away; Hb: hemoglobin; HCT: hematocrit; ANC: absolute neutrophil count; ALC: absolute lymphocyte count. Data are shown as mean ± standard deviation.
Discussion
This study reported elevated levels of soluble endothelial markers (E-selectin, ICAM-1 and VCAM-1) in severely ill patients with COVID-19, which is correlated with hematological parameters. The hematological parameters in this study revealed abnormal hemograms in ICU-admitted COVID-19 patients including elevated WBC count, neutrophilia, and lymphopenia, which is consistent with previous reports.18,22,23 The abnormality was more pronounced in PA COVID-19 patients as compared to DC COVID-19 patients.18,22 On the other hand, the CBC showed low hemoglobin (Hb) levels in COVID-19 patients,18,22,24,25 which further reduced in PA patients than DC patients. These findings have been found to be associated with severity, hospitalization, progression of the infection, inflammatory responses and mortality of COVID-19.18,26–30 Therefore, the current study suggests that a combination of WBC count, neutrophilia, lymphopenia, and low hemoglobin levels can serve as indicators of worsening condition in COVID-19 patients admitted to the ICU.
Platelet count is significantly reduced in COVID-19 patients. Platelet serves as an important indicator of disease severity, not only in COVID-19 but also in other diseases due to its diverse function. 31 It strongly correlates with COVID-19 severity, higher mortality rates, and hypoxemia, which is linked to endothelial dysfunction.23,32–34 The current study showed a significant reduction in platelet count in ICU-admitted COVID-19 patients compared to controls, with further reduction in PA COVID-19 patients compared to DC COVID-19 patients indicating a key role of platelets in COVID-19 infection, severity, and prognosis.
CBC-calculated parameters such as NLR, PLR, PNR, and MPR are increasingly recognized as valuable biomarkers for diagnosing, and predicting disease severity, inflammatory response, and mortality in various conditions, including COVID-1918,22,28,35–39 In this study, COVID-19 patients had increased NLR (p < .05), PLR (p < .05) and MPR (p > .05) compared to the control group. Similar findings have been reported of increased NLR, PLR, and MPR in both ICU and non-ICU COVID-19 patients and associated with adverse outcomes and mortality.28,35–38 The study highlights the importance of NLR, PLR, and MPR in predicting outcomes and mortality in COVID-19, as their levels were elevated in our cohort of PA COVID-19 patients as compared to DC patients. Additionally, COVID-19 patients had lower PNR compared to controls, consistent with other reports.18,22 Notably, DC COVID-19 patients had significantly higher PNR than PA COVID-19 patients, suggesting its potential role in predicting disease severity.
The coagulation profile, including PT and aPTT, in this study is consistent with previous reports, showing prolonged PT and aPTT in COVID-19 patients compared to controls.40–42 Additionally, D-dimer, a marker of fibrin clot breakdown, is significantly elevated in COVID-19 patients.40–42 Elevated D-dimer levels have been associated with mortality in COVID-19.41,43 The increased coagulation profiles and D-dimer, along with thrombocytopenia, are attributed to the impact of COVID-19 on the hemostatic system, leading to coagulopathy, including DIC.21,40 Hypercoagulability and thrombotic tendency, which are linked to endothelial damage, are well-established pathogenic factors in COVID-19.5,6,43
Endothelial damage is considered a significant contributor to the pathogenesis, severity, and poor outcomes of COVID-19. 44 The inflammatory response triggered by COVID-19, known as the “cytokine storm,” leads to endothelial damage. This damage releases adhesive and prothrombotic markers from the affected endothelial cells at the site of inflammation 8 and is associated with coagulopathy and thrombotic complications. 45 Endothelial markers such as E-selectin, ICAM-1, and VCAM-1 indicate endothelial damage. They are responsible for recruiting inflammatory cells (primarily leukocytes) to the site of inflammation (E-selectin) and facilitating their firm adhesion (ICAM-1 and VCAM-1).9,10 These along with others markers indicating endothelial damage, have been used as prognostic factors for outcome and mortality in non-COVID-19 acute respiratory distress syndrome.46,47 This study demonstrates elevated levels of E-selectin, ICAM-1, VCAM-1, in COVID-19 patients admitted to the ICU compared to healthy controls. E-selectin levels, typically low in healthy individuals, and increase during inflammation. 48 Furthermore, postmortem examination of lung tissue from COVID-19 patients reveals elevated levels of these markers compared to healthy controls. 8 Prior studies have reported elevated levels of E-selectin in ICU-admitted COVID-19 patients compared to non-ICU admitted COVID-19 patients.11,12,49 The elevation of E-selectin was observed in severe ill COVID-19 patients as compared to mild cases of COVID-19 infection, 50 and healthy controls.8,11,49,51 Furthermore, non-survivor COVID-19 patients admitted to the ICU had higher E-selectin levels than survivor patients admitted to the ICU. 52 However, previous study found lower E-selectin levels in COVID-19 patients (overall, outpatients, and inpatients) compared to controls, 9 while the current study showed comparable levels of E-selectin between DC and PA patients. These contrasting findings may be due to variations in the techniques used to evaluate soluble endothelial markers, including E-selectin, time of sample collection, and the presence of other comorbidities. Nevertheless, several studies have proposed E-selectin as a predictive marker for ICU admission in COVID-19 patients and for assessing disease severity and mortality in ICU-admitted COVID-19 patients11,12,51,53 and of thrombosis in hospitalized COVID-19 patients. 51
Leukocytes play a vital role in defending against infections by migrating across endothelial cells. 53 The adhesion of neutrophils to the endothelium is facilitated by ICAM-1 and VCAM-1, which are associated with mortality in severe infections.54,55 Our data and other studies have shown higher levels of ICAM-1 and VCAM-1 in COVID-19 patients compared to healthy controls.8,14 Additionally, ICAM-19,52 and VCAM-1 9 levels are elevated in non-survivor COVID-19 patients admitted to the ICU compared to survivor patients. Moreover, elevated levels of ICAM-1 are observed in COVID-19 patients admitted to the ICU, which suggest its potential as a predictor of ICU admission and mortality.49,52 However, previous study reported similar ICAM-1 levels between ICU survivors and non-survivors. 9 A study by Spadaro et al. (2021) indicated that ICAM-1 levels increased within 24 h of ICU admission in COVID-19 patients. 9 Additionally, ICAM-1 levels were found to decrease over time in COVID-19 patients admitted to the ICU, 9 supporting our findings as our samples were collected at the time of ICU admission and our hypothesis that time of collection can be contributed to results discrepancy.
VCAM-1 levels were significantly higher in COVID-19 patients (overall, outpatients, and inpatients) compared to controls. 13 However, no differences in ICAM-1 levels were observed between COVID-19 patients and patients with bacterial infection. 13 Bruni et al. (2022) found lower endothelial cell production in COVID-19, suggesting it as a specific feature of the disease. 13 The negative correlation between COVID-19 and other markers and laboratory parameters may be due to extensive treatment regimens received by the patients. VCAM-1 levels were elevated only in COVID-19 patients, while ICAM-1 and E-selectin levels were comparable between the two groups. 56 Some studies reported no differences in E-selectin, ICAM-1, and VCAM-1 levels between COVID-19 patients (mild and moderate cases) and healthy controls.50,57
It is important to note that the current study has several limitations, like any other study including the patients were recruited from a single study center and were limited to ICU admissions, without considering non-ICU COVID-19 patients, sample size and collection was randomized, and the study did not include other parameters such viral load and inflammatory markers such as C-reactive protein. In addition, other soluble endothelial markers were not considered.
Conclusion
This study found significantly elevated levels of soluble endothelial markers (E-selectin, ICAM-1, and VCAM-1) in COVID-19 patients, indicating endothelial dysfunction. These markers can serve as early indicators for detecting and predicting endothelial cell involvement in COVID-19 complications. E-selectin was significantly correlated with some hematological parameters, which might indicate a potential involvement with disease severity. Further comprehensive studies are needed to elucidate the exact and the potential role of endothelial cells with hematological parameters.
Supplemental Material
Supplemental Material - Correlation of circulating endothelial markers in COVID-19 patients admitted to the intensive care unit with laboratory data
Supplemental Material for Correlation of circulating endothelial markers in COVID-19 patients admitted to the ICU with laboratory data by Gasim Dobie, Abdullah A Mobarki, Aymen M Madkhali, Mohmmad S. Akhter, Abdulrahim R Hakami, Mohammed H Nahari, Yahya H Matari, Khaled Essawi, Waleed Hakami, Ali Hakamy, Mohammad Algahtani, Denise E Jackson, and Hassan A Hamali in European Journal of Inflammation
Footnotes
Author contributions
GD, HAH designed the study. MSA, KS, YHM, collected the samples. ARH, AZMHN WH prepared the samples. GD, MSA, ARH, MHN performed the analysis. HAH, GD wrote the manuscript, HAH, GD, AAM, AMM, DEJ reviewed and edited the manuscript.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by the authors extend their appreciation to the deanship of Scientific Research, Jazan University, for supporting the research work through the Research Unit support Program, (Grant Number RUP2-05).
Ethical statement
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
