Abstract
Objective
No consensus exists regarding the association between pemphigus and thyroid disease. To explore the relationship between the two conditions by synthesizing the existing data.
Methods
We performed this review based on PubMed, Embase and Web of Science (from inception to 2022) and used the Newcastle-Ottawa scale for assessing the quality of studies. The outcome was represented by pooled odds ratios (ORs) with 95% confidence intervals (CI). And the publication bias and sensitivity analyses were developed.
Results
Our analyze finally included six studies containing 17,567 pemphigus patients. Overall, we revealed that pemphigus is significantly associated with hypothyroidism (OR 1.70, 95% CI 1.54–1.87), while not with thyroid cancer (OR 0.93, 95% CI 0.41–2.11) and autoimmune thyroid disease (AITD) (OR 1.64, 95% CI 0.91–2.95). In subgroup analyses, pemphigus was also not associated with Graves’ disease (OR 0.97, 95% CI 0.63–1.49) and Hashimoto’s thyroiditis (OR 1.32, 95% CI 0.88–1.97).
Conclusion
Our results reveal a significant association between pemphigus and hypothyroidism. Considering other relevant studies, we also speculate that the prevalence of AITD is higher in pemphigus patients than in the general population.
Introduction
Pemphigus is a chronic, recurrent and severe bullous skin disease with acantholysis in the epidermis. Flaccid vesicles appear on the skin or mucous membranes with a positive Nikolsky phenomenon. 1 This is primarily dominated by IgG autoantibodies against desmosomal adhesion molecules, including desmoglein 1 (Dsg1) expressed in the skin and desmoglein 3 (Dsg3) expressed in the skin and on mucous membranes. Then the autoantibodies will bind to desmosomal proteins, which will induce adjacent keratinocytes to separate, a process called acantholysis. 2
In some investigations, thyroid diseases have been found to be a comorbidity of several skin diseases, such as alopecia, vitiligo, chloasma and Sjogren’s syndrome. A recent study showed that the relatives of pemphigus patients seemed more prone to thyroid diseases. And about 34% of pemphigus vulgaris patients had hypothyroidism, Graves' disease, toxic multinodular goiter or follicular carcinoma. 3
It is speculated that pemphigus has a correlation with thyroid diseases, but there is no meta-analysis to systematically prove it. This article summarizes a series of epidemiological investigations on pemphigus to explore the relationship between them.
Methods
Literature search
We performed this review based on the recommended PRISMA guidelines 4 and searched PubMed, EMBASE and Web of Science from inception to 28 October 2022. We chose “pemphigus” combined with “hypothyroidism” or “thyroid cancer” or “autoimmune thyroid disease” as the MeSH terms or keywords.
Eligible studies must set groups recording thyroid disease cases in pemphigus versus controls. For inclusion, the studies must be published in English and contain enough data on the odds ratio between pemphigus and thyroid disease. And the study design can be cohort, case-control or cross-sectional. Studies were excluded by reading the title, abstract and full text.
Data extraction
Two investigators respectively recorded data from the included articles and settled the disagreements through discussion. They carefully reviewed each study and collected the following data: the period of investigation; study design; location; sample size; thyroid disease type; and the odds ratios (ORs) to have thyroid disease among pemphigus patients with 95% CI.
Methodological quality assessment
We used the Newcastle-Ottawa scale (NOS) for evaluating the quality of studies. 5
And high-quality research is defined as a score of at least 6 (9 in total). Sensitivity analysis and Egger’s test were used for assessing the stability of results and potential publication bias, respectively. 6
Statistical analysis
If the p value of Cochrane Q statistics is less than 0.05 or I2 statistics is greater than 50%, it means the included studies have significant heterogeneity. Then we will choose the random effects meta-analysis model, otherwise we will choose the fixed effect model. The overall pooled odds ratio with 95% CI was shown as the primary result. Analyses were performed using Stata 17.0.
Results
192 articles in total were retrieved, 46 of which were duplicates, and 32 were excluded according to the title and abstract. The remaining 114 articles were carefully reviewed in full text. Finally, six studies were included in this meta-analysis.7–12 The flow diagram for inclusion is demonstrated in Figure 1. Flowchart of inclusion of studies.
Study characteristics
The selected six studies contained controls and estimated the odds ratio between pemphigus and thyroid disease. The quality assessment showed that three of the six eligible studies were rated six or higher.8,9,11 Among the six studies included, five were reported for pemphigus and one for pemphigus vulgaris. In total, there were two studies recording for hypothyroidism, thyroid cancer and Graves' disease, three studies for Hashimoto’s thyroiditis, and one study for AITD.
Characteristics of included studies which evaluated the association between pemphigus and thyroid disease.

aNOS (Newcastle-Ottawa scale): 9–7, low risk of bias; 4–6, moderate risk of bias; 0–3, high risk of bias.
bAITD: Autoimmune thyroid disease.
Meta-analysis of the association between pemphigus and thyroid disease
According to the heterogeneity results, the fixed effect model was applied to the group hypothyroidism (heterogeneity I2 = 11.9%), while the random effect model to the group thyroid cancer and AITD (heterogeneity I2 > 50%). The overall results indicated that pemphigus was significantly correlated with hypothyroidism (OR 1.70, 95% CI 1.54–1.87), while not with thyroid cancer and AITD (Thyroid cancer: OR 0.93, 95% CI 0.41–2.11; AITD: OR 1.64, 95% CI 0.91–2.95). (Figures 2–4) Forest plot showing association between pemphigus and hypothyroidism. Forest plot showing association between pemphigus and thyroid cancer. Forest plot showing association between pemphigus and AITD.
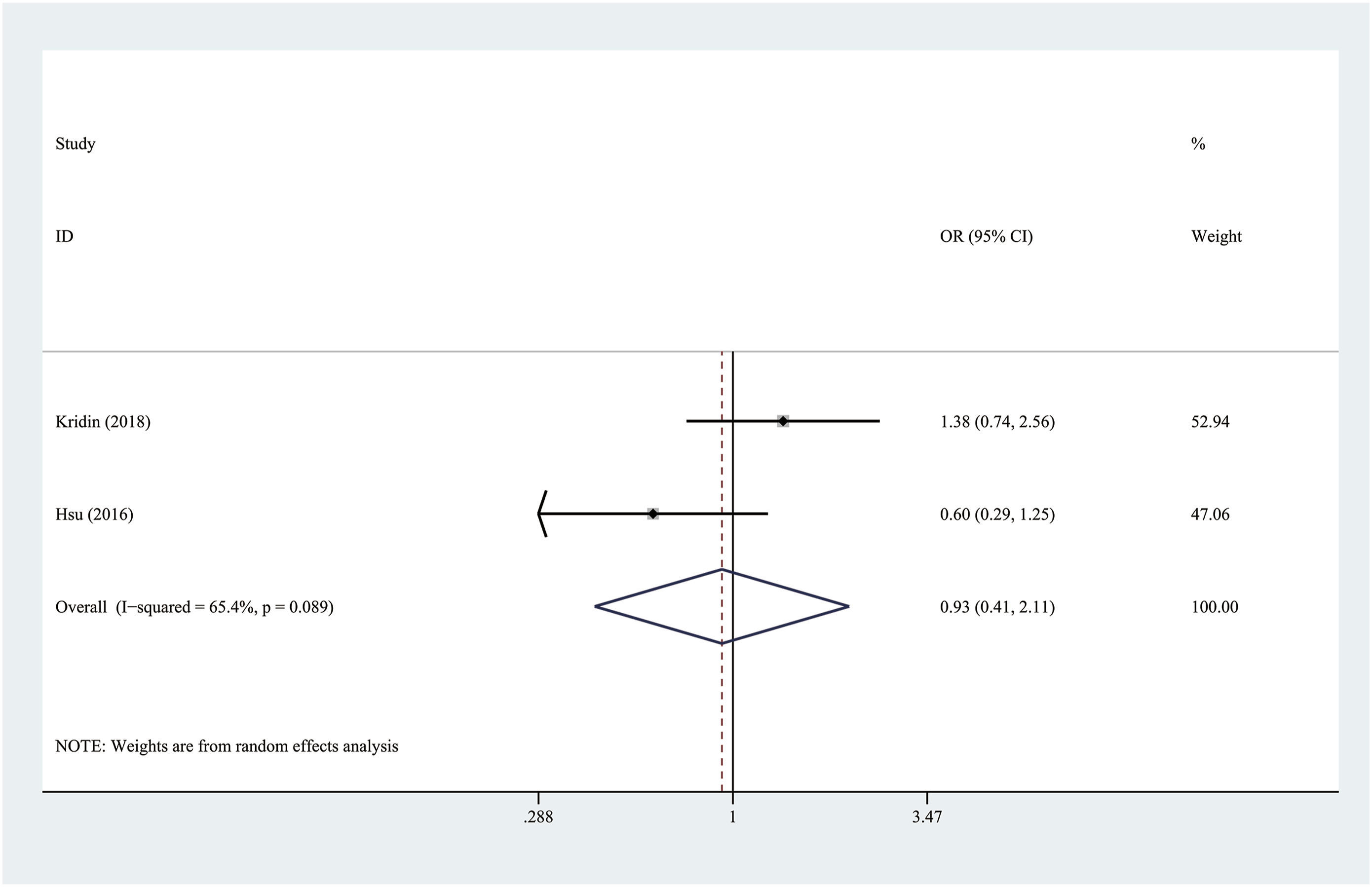

To further address the relatively high heterogeneity in AITD (I2 = 87.5%), the subgroup analysis based on different types of AITD was performed. It was noted that pemphigus was also not associated with Graves' disease and Hashimoto’s thyroiditis. (Graves' disease: OR 0.97, 95% CI 0.63–1.49; Hashimoto’s thyroiditis: OR 1.32, 95% CI 0.88–1.97). (Figure 4). Moreover, owing to the limited number of eligible studies in hypothyroidism and thyroid cancer, the sensitivity analysis and Egger’s test were conducted only for the AITD group. It demonstrated that the final results were reliable (Figure 5) and no significant publication bias existed in the analysis (p = 0.341; Figure 6). Sensitivity analysis in group AITD. Egger’s tests showing publication bias in group AITD.

Discussion
It is accepted that thyroid autoimmune antibodies can help diagnose some thyroid diseases. Thyroid autoimmune antibodies, such as anti-thyroid stimulating hormone receptor (anti-TR), anti-thyroid peroxidase (anti-TPO) and anti-thyroglobulin (anti-TG) antibodies, are important laboratory indicators of AITD, 13 and high titers of anti-TPO and anti-TG autoantibodies are risk factors for hypothyroidism and thyroid cancer.14–16 Kristina et al. evaluated anti-TPO levels in 280 pemphigus patients and 167 controls. It demonstrated that the rate of anti-TPO activity was significantly higher in pemphigus patients than controls, resulting from the human leukocyte antigen status and absence of desmoglein reactivity. 17 A recent study in China found that anti-TPO and anti-TG antibody levels and antibody positivity increased in pemphigus patients compared to controls. 18 Kavala et al.observed that titers of thyroid autoimmune antibodies in the pemphigus group increased significantly. 3 Overall, the above evidence suggested that there may exist a link between pemphigus and diverse thyroid diseases.
However, a study, enrolling patients without steroid therapy, revealed that there was no significant difference in thyroid autoantibodies between pemphigus and controls. And it was unnecessary to routinely screen for thyroid autoantibodies in pemphigus patients. 19 It should be noted, as the main treatment of pemphigus, that steroids may contribute to the development of thyroid diseases. A 38-year-old woman developed Graves' disease during the period of glucocorticoid treatment for pemphigus. Bartalena et al. inferred that its onset was promoted by chronic low-dose glucocorticoid therapy. 20 A retrospective study found that patients with endogenous Cushing’s syndrome had a very high incidence of primary thyroid disease, and the alleviation of hypercortisolism appeared to induce AITD. 19 Since the included studies in our analysis did not exclude the influence of hormones, it may affect the results as a confounding factor. Moreover, serum cortisol can affect the hypothalamic–pituitary–thyroid axis activity and is negatively correlated with TSH and T4, which may cause central hypothyroidism.21,22 A significant association was found in group hypothyroidism, but considering the influence of steroids, the association between the two conditions needs further exploration. Additional studies excluding the variable steroid are needed in the future.
Hypothyroidism is characterized as primary, central or peripheral depending on the pathology of thyroid, pituitary or hypothalamus, or peripheral tissue. Primary hypothyroidism is defined as thyroid failure caused by disease of the thyroid gland itself, accounting for over 99% of total hypothyroidism. For adults, hypothyroidism is most often caused by Hashimoto’s thyroiditis.23,24 Pemphigus is significantly associated with hypothyroidism in our findings, indicating that pemphigus is probably related to Hashimoto’s thyroiditis. Compared with the controls, Firooz et al. 25 found an increased prevalence of AITD, juvenile rheumatoid arthritis and type 1 diabetes in 830 relatives of pemphigus patients, and each of these diseases was associated with the presence of certain HLA-DR and HLA-DQ allc1es. Using the basic principal component methods, the analysis indicated that patients with pemphigus developed a specific cluster for AITD, rheumatoid arthritis and type 1 diabetes, which were also the most common autoimmune diseases among relatives of pemphigus patients. 10
Some explanations regarding the coexistence of the two conditions are below. First, pemphigus and AITD may have a common susceptibility gene or allele, but show different phenotypes influenced by various genetic and environmental factors. Meanwhile, there may exist a common environment triggering the autoimmune pathogenesis of both.10,26 Second, HLA alleles related to the disease may express similar autoantigen epitopes in different tissues. We hypothesized that the antigen epitope of pemphigus may be similar to that of thyroid, and there may exist a cross-reactivity between them. 10 Finally, besides the primary target desmoglein (Dsg3, Dsg1), Sajda et al. have demonstrated that TPO, an enzyme mainly expressed in thyroid tissue and not expressed in keratinocytes, is also the target of pemphigus autoantibodies. They also speculated that antibodies against TPO have an impact on some keratinocyte antigens. 27
Considering that pemphigus patients were not prone to have AITD compared with controls in our result, we hypothesize that the prevalence of AITD in our result was underestimated and several reasons may account for this: First, to treat pemphigus, most patients will take immunosuppressants, which may reduce the incidence of AITD. Then, according to reports, most autoimmune diseases occurred late in life. So the AITD that occurred after our data collection will be missed. 10 Finally, pemphigus patients are regarded as individuals with autoimmune diathesis, Compared with controls, they are indeed more likely to have AITD. In other words, pemphigus is significantly associated with autoimmune diathesis rather than AITD. It just increases the susceptibility to AITD, which still requires certain etiopathogenetic variables to trigger.
Strengths and limitations
It is the first meta-analysis aiming to measure the relationship between pemphigus and thyroid disease. The eligible studies had a large sample size and recorded different types of thyroid diseases. The limitations are listed below. First, there were only two studies included in group hypothyroidism and thyroid cancer, which still need more researches to identify their relationship. Second, the group AITD showed relatively high heterogeneity among included studies. To solve it, we used the random-effect model and conducted the subgroup analysis based on different types of AITD. Furtherly, we also provided possible mechanisms for their relationship. Thirdly, Parameteswaran et al. 10 developed a cross-sectional study enrolling 794 cases and found that pemphigus was associated with AITD (OR 6.03, 95% CI 3.53–10.31), but they did not provide sufficient information on which types were included in AITD. Besides, the cause of hypothyroidism was not clear in the reports, which may influence the subgroup result of AITD in the meta-analyse.
Conclusion
Our study shows a significant correlation between pemphigus and hypothyroidism.
Considering other relevant studies, we also speculate that patients with pemphigus have a higher prevalence of AITD than controls. Further studies involving large samples and excluding confounding factors are warranted in the future.
Footnotes
Acknowledgements
The authors are grateful to Professor Na Wang for her invaluable instruction in this paper.
Author contributions
Linxi Zeng: Statistical analysis, study design, collecting data, evaluation and discussion;
Xin Huang: Collecting data, evaluation and discussion, the manuscript writing;
Yue Yao: Statistical analysis, the manuscript writing;
Guoqiang Zhang (Corresponding author): Review and approval of the manuscript.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Informed consent
All authors agreed and approved to submit our manuscript to this journal.
