Abstract
Since May 2022, monkeypox has been gradually spreading across countries. In past reports and treatment consensus, monkeypox is most widely known for its characteristic skin lesions, which are hard, spherical rashes that appear as herpes and pustules and are widely distributed centrifugally over all parts of the body. Prior to the appearance of the rash, carriers of monkeypox are likely to spread the virus to more susceptible people. Attention to the early atypical mucosal manifestations of monkeypox allows for early identification of potential cases of monkeypox, thereby controlling the further spread of the epidemic.
To the editor,
Since May 2022, the monkeypox epidemic was first detected in the United Kingdom and gradually spread from Western countries to countries around the world, and the World Health Organization declared the highest level of public health alert, calling the monkeypox epidemic a public health emergency of international concern. According to WHO, as of 9 September 2022, the cumulative number of confirmed monkeypox cases worldwide has exceeded 62,000. 1
An observational analysis published recently suggests that it is highly likely that monkeypox virus is further transmitted in men who have sex with men (MSM) by forming local inoculum through close skin or mucosal contact. 2 This mode of transmission is closely related to the recent emergence of a series of atypical clinical manifestations of monkeypox. And it can be understood as direct contact transmission closely related to sexual intercourse. Here we focus on the atypical mucosal lesions that may occur in patients with monkeypox under a specific route of transmission and review nine cases in this paper.
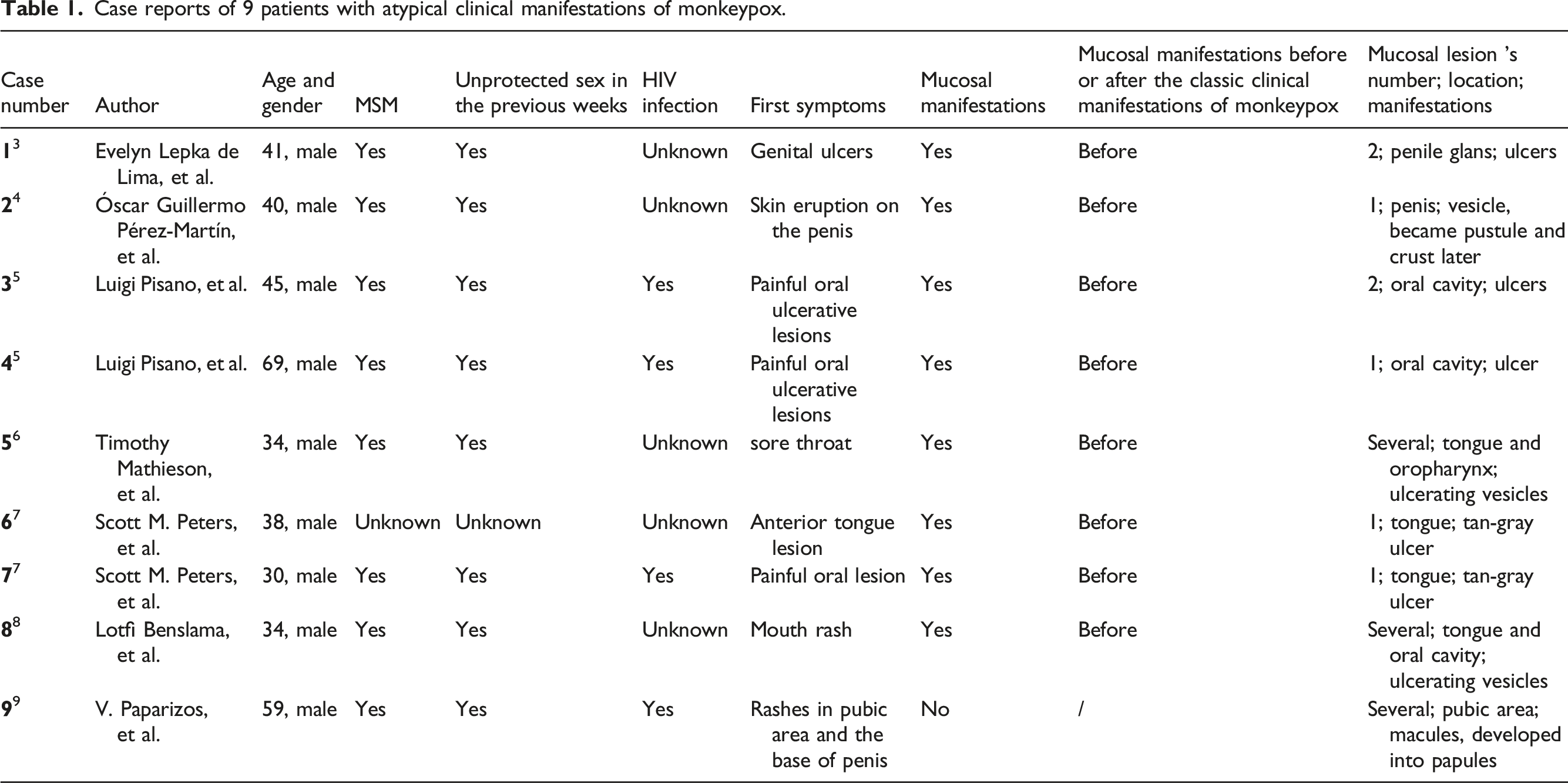
Case reports of 9 patients with atypical clinical manifestations of monkeypox.
Summary of 3 retrospective analysis literatures of monkeypox case.

Monkeypox is a zoonotic disease caused by infection with monkeypox virus. In past reports and treatment consensus, the typical clinical manifestations of monkeypox have been highlighted, including an incubation period of 5 to 21 days and non-specific systemic symptoms (chills, fever, headache, lethargy, malaise, myalgia, lymph node enlargement). Monkeypox is most widely known for its typical skin lesions, which are hard, spherical rashes that appear as pseudopustules without liquid content and are widely distributed centrifugally over all parts of the body. 14 To initiate the screening and diagnosis only after the appearance of the characteristic lesions of monkeypox could be late. Before the rash appears, monkeypox carriers are likely to transmit the virus to a wider susceptible population.
In an article (Kristi L. Koenig 2022), clinicians are urged to raise awareness of the atypical presentation of monkeypox. 15 Early identification of potential monkeypox cases is the top priority to control the further spread of the epidemic. Based on the characteristics of the nine cases listed above and the relevant literature, it can be assumed that when MSM develops oral or perineal mucosal lesions, especially HIV-infected people, after unprotected sex, the monkeypox infection needs to be ruled out. We should perform PCR testing for monkeypox virus on their lesions as soon as possible, thus enabling early diagnosis, isolation and control of monkeypox. Because there are few descriptions and reports of mucosal symptoms in monkeypox cases, only the above seven articles are included in this article as arguments. When more relevant information is available, we can further study the pattern and characteristics of mucosal lesions caused by monkeypox virus.
Footnotes
Acknowledgements
The authors thank the reviewers for their precious comments and the editor Miss Seema Kandari for her patient help.
Author contributions
YH has made substantial contributions to the conception and design of the work; YH and BW have made substantial contributions to the acquisition, analysis, and interpretation of data for the work; BW and LZ drafted the work and revised it critically for important intellectual content; GZ provides approval for publication of the content; GZ agrees to be accountable for all aspects of the work in ensuring that questions related to the accuracy and integrity of any part of the work are appropriately investigated and resolved. All authors contributed to the article and approved the submitted version.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This research received financial support from Hebei Medical University ’s 2018 Higher Education Reform Project (2018-88) for authorship, and publication of this article.
