Abstract
To explore the relationship between IL-17 mediated immune response and HPV-negative cervical cancer, we established the co-culture system of cervical cancer C-33A cells and PBMC, and treated with different concentrations of rhIL-17. PBMC were extracted from 10ml anticoagulant blood provided by healthy female volunteers and colleagues in our hospital, which were co-cultured with cervical cancer C-33A cells. After treatment with different concentrations of rhIL-17, the proliferation, apoptosis, invasion behavior and VEGF expression level of cancer cells in each group, were determined by CCK-8, flow cytometry, transwell invasion assay and ELISA, respectively. The proliferation rate of C-33A cells slightly increased with the ascending of IL-17 concentration, but no statistical significance was found among each group (P > 0.05). When at low concentration of IL-17, the cell apoptosis rate seems to slightly decline. With the increase of concentration, the decrease of apoptosis rate became more obvious (P < 0.05). However, differing from those shown above, we found that IL-17 slightly inhibited the cancer cell invasion at high concentration, while it was more obvious at low concentration (P < 0.05). Furthermore, we found that there was no significant correlation between IL-17 and VEGF (P > 0.05). In summary, there is a close correlation between IL-17 mediated immune response and HPV-negative cervical cancer. Also, we think that IL-17 may play a dual role in tumor progression and could be a possible significant influence on tumor proliferation, apoptosis, and metastasis, which provides a basic theoretical basis for the further study of immunotherapy measures for cervical cancer.
Introduction
As the most common malignant tumor in gynecological reproductive tract, cervical cancer threatens many women’s life and health and its morbidity and mortality are increasing year by year, especially in developing countries. According to the latest data from WHO in 2018, 1 there are 569,800 new patients and 311,400 deaths of cervical cancer every year worldwide, meanwhile, 2 China was the country with the highest number of cases (106, 000) and the deaths (48, 000) was just slightly behind India (60, 000). Although the cause of cervical cancer has been identified as the infection of human papillomavirus (HPV), there are still some cervical cancer patients with HPV negative, and the specific etiology of these patients is still unknown. 3 Related studies deemed that the prognosis of these cervical cancer patients is worse than that of HPV-positive patients.4,5 Similarly, in other HPV-associated tumors, the prognosis of HPV-positive patients was also better than HPV-negative ones, just like vaginal cancers. 6 The same things happened in the sinonasal carcinoma, and the most important reason of which might be sensitive to chemotherapy and radiation in HPV-positive ones.7,8 In recent decades, we know that IL-17 is an important kind of cytokines with a strong ability of the activation of neutrophils, which is mainly derived from T helper (Th) 17 cells, and is also very important in the immunologic process of infection, tumors, as well as autoimmune diseases and so on.9,10 For instance, one study suggested that the expression of IL-17 was significantly higher in the serum from HPV-positive women, when compared to healthy patients. 11 Also, the result of another study showed a close correlation between IL-17 mediated immune response and HPV-positive cervical cancer. 12 At present, there was little study on IL-17 and HPV-negative cervical cancer. For further research on the function of IL-17 in HPV-negative cervical cancer, we detected the tumor growth mechanism of cervical cancer C-33A cells, in order to further understand the role of IL-17 mediated immune response in the tumor progression of cervical cancer.
Materials and methods
Blood sample preparation
Peripheral anticoagulant blood (10 mL) of 15 healthy female volunteers and colleagues in our hospital from September 2017 to June 2020 were collected for the extraction of PBMC. The selection criterion was healthy women of child-bearing age, non-menstrual period and both normal results of cytology and HPV test. Participants with active or chronic infection, autoimmune disease, malignant tumors and so on were excluded. Venous blood (10 mL) was collected and immediately processed in the lab. PBMC was isolated by lymphocyte separation fluid (p8610, Solarbio, Beijing). The study was approved by the Medical Ethical Committee of The First Affiliated Hospital of Wenzhou Medical University. Written informed consent was obtained from each participant before the study.
Cell culture and co-culture
This study is exploratory research on cell model in vitro. C-33A (CM-H184, GAINING BIOLOGICAL, Shanghai) is cervical cancer cell line with negative HPV DNA and RNA. It was cultured in fresh MEM medium (KGM41500S, KeyGEN BioTECH, Jiangsu) supplemented with 10% FBS (E600001-0500, BBI Life Sciences, Shanghai), 1% double antibiotic mixture (100X, P1400, Solarbio, Beijing) and in an incubator with 37°C and atmosphere containing 5% CO2 until they were in good condition. After trypsin (T1300, Solarbio, Beijing) digestion, C-33A cells were resuspended and co-cultured with PBMC in a 1:1 ratio for 48 h in order to conduct subsequent experiments. Meantime, culture plate was shaken per 6 h to avoid PBMC cells adherent. The co-culture system between C-33A cells and PBMCs simulates human immune process in vitro, because the function of IL-17 requires immune cells.
Study groups
After adding different concentrations of recombinant human IL-17 (rhIL-17, C774, Novoprotein, Shanghai), C-33A cells and PBMC co-cultured system were divided into two groups: 50 pg/mL in the high concentration group and 5 pg/mL in the low concentration group. The group without treated were used as control group.
Cell proliferation assay
After treating with rhIL-17 in the co-cultured cells for 48 h, CCK-8 (KGA317, KeyGEN BioTECH, Jiangsu) assay was performed to detect the growth of C-33A cells. According to the results of the optical density at 450 nm, the proliferation rate of C-33A cells in each group was calculated. The proliferation rate of control group was defined as 100%.
Flow cytometry analysis
Discard supernatant, remove suspended cells, 1 × 106–3 × 106 C-33A cells were resuspended, centrifuged, washed twice. A test tube was subsequently added with 300 μL cell suspension, 3 μL Annexin V-FITC and 5 μL PI-PE (AP101-100-kit, MULTI SCIENCES, Zhejiang) for 10 min incubation in the dark. Then, the apoptosis cells in each group were detected by flow cytometry.
Transwell assay
Medium in the transwell room with 24-well plates was removed and washed. After that, 0.1% crystal violet (G1061, Solarbio, Beijing) was added for cell staining and wiped off the non-invasive cells remaining in the inner chamber. The numbers of staining cells were counted under the microscope. After taking photographs, the staining fluid was removed and 1 mL 33% acetic acid added into each well to dissolve the dye solution in the cells, after well mixed, 200 μL cell suspension from each well was placed into 96-well plates, then the optical density at 570 nm was measured. 200 μL 33% acetic acid per well was used as a control. The optical density of invaded cells represents the invasive ability of the tumor cells.
ELISA analysis
The expression levels of VEGF in supernates saved from each well after 48 h of co-culture were measured by ELISA kits (MM-0115H1, MEIMIAN, Jiangsu). We draw the standard curve based on the optical density at 450 nm, then the expression levels of VEGF were obtained.
Statistical analysis
The results were described as the Mean ± SEM and showed a normal distribution. After the tests of normality and homogeneity of variance, the data were analyzed using GraphPad Prism 7.0 with ANOVA followed by Bonferroni method. p < 0.05 was considered significantly difference.
Results
IL-17 showed the role of promoting tumor local growth of cervical cancer
To explore the function of IL-17 in the growth of HPV-negative cervical cancer cells, the proliferation and apoptosis rate of C-33A cells were detected by CCK-8 assay and flow cytometry respectively. The proliferation rate of cancer cells in the control group was defined as 100%. After co-culturing for 48 h, the rate of C-33A cells in low concentration group was 109.52 ± 5.12%, and 110.48 ± 7.16% in high concentration group. The proliferation rate of C-33A cells slightly increased with the ascending of IL-17 concentration, but no statistical significance was found among each group (p > 0.05, Figure 1).
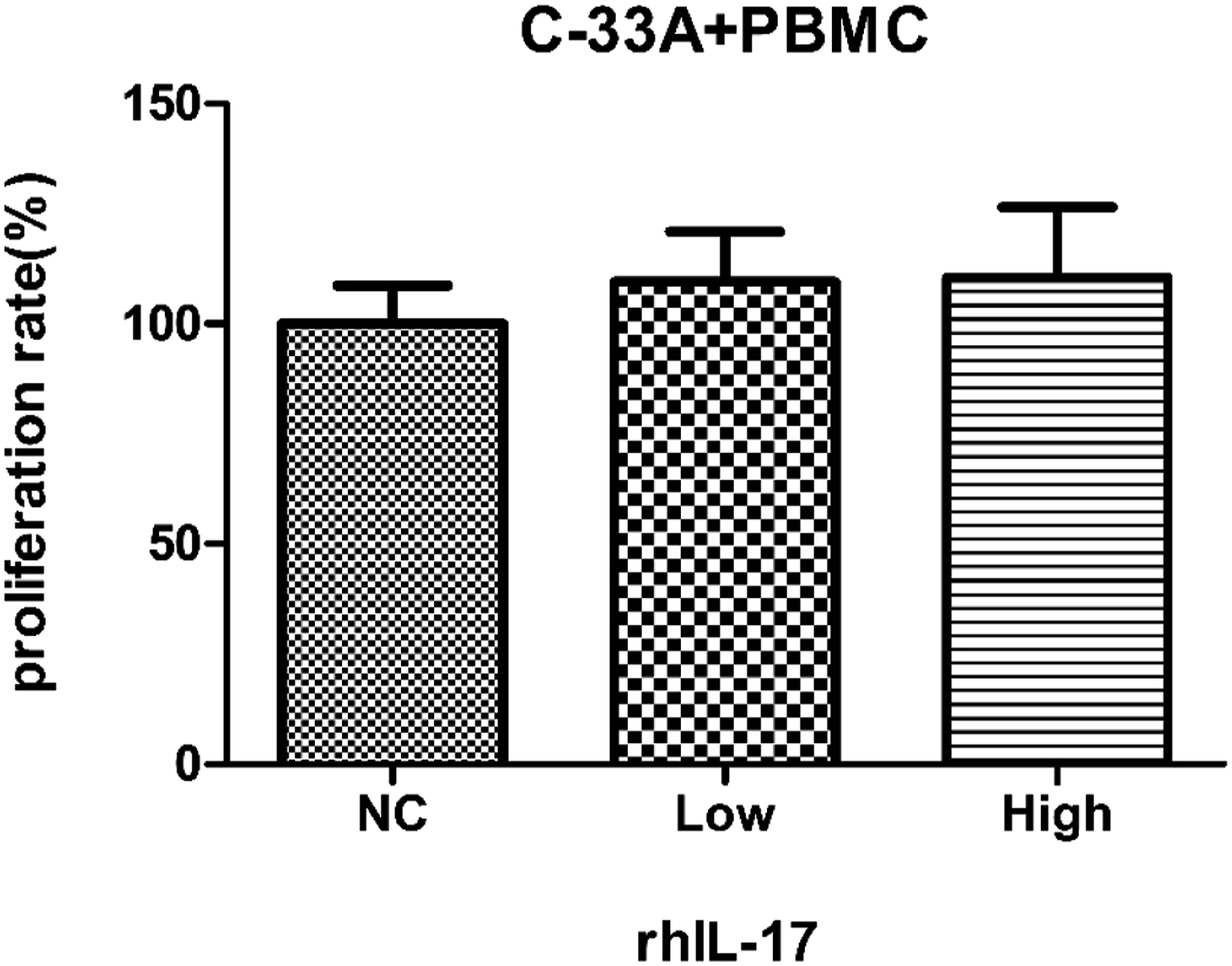
The effects of IL-17 on the proliferation of C-33A cervical cancer cells. The proliferation rate of C-33A cells was assessed by CCK-8 assay after the C-33A cells and PBMCs co-culture system were treated with different concentrations of rhIL-17 (0, 5 and 50 pg/mL) for 48 h. The proliferation rate of C-33A cells in the control group was defined as 100%. Data are the mean of five independent experiments ± SEM, p > 0.05. Notes: NC, negative control; Low, 5 pg/mL; High, 50 pg/mL; PBMC, peripheral blood mononuclear cells; rhIL-17, recombinant human IL-17.
Flow cytometry staining results of each group are shown in Figure 2. The apoptosis rate of high concentration group was 15.86 ± 0.42%, which was significantly lower than that of low concentration group (18.05 ± 0.29%) and control group (18.25 ± 0.59%) (p < 0.05), however, there was no difference between the latter two groups (p > 0.05, Figure 3). Therefore, with the increasing of concentration, IL-17 inhibited cell apoptosis of C-33A cells. The above results indicated that IL-17 showed a promoting tumor effect. The effects of IL-17 on the apoptosis of C-33A cervical cancer cells. The apoptosis rate of C-33A cells was assessed by flow cytometry after the C-33A cells and PBMCs co-culture system were treated with different concentrations of rhIL-17 (0, 5 and 50 pg/mL) for 48 h. (a, b) Cell apoptosis in the control group; (c, d) Cell apoptosis in the low concentration group; (e, f) Cell apoptosis in the high concentration group. Each experiment repeated three times. Notes: NC, negative control; Low, 5 pg/mL; High, 50 pg/mL. The effects of IL-17 on the apoptosis of C-33A cervical cancer cells. The quantitative percentage of apoptotic C-33A cells was calculated by flow cytometry after the C-33A cells and PBMCs co-culture system were treated with different concentrations of rhIL-17 (0, 5 and 50 pg/mL) for 48 h. Data are the mean of three independent experiments ± SEM, *p < 0.05. Notes: NC, negative control; Low, 5 pg/mL; High, 50 pg/mL; PBMC, peripheral blood mononuclear cells; rhIL-17, recombinant human IL-17.

IL-17 showed the role of suppressing cell invasion
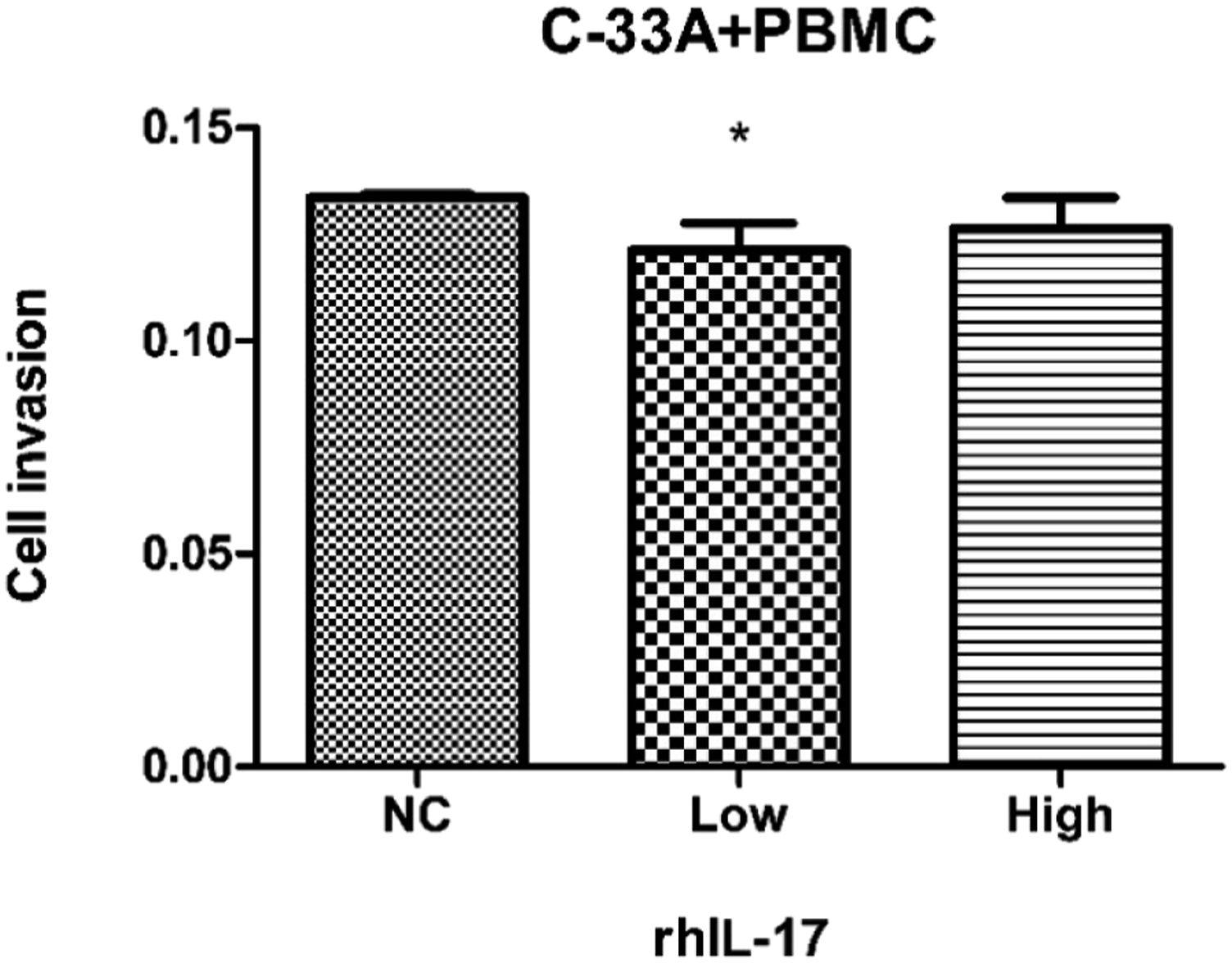
Transwell assay were used to explore the effect of IL-17 on the cell invasion ability. The cancer cells passing through the membrane in each group was stained and identified as invaded cells (Figure 4). The number of invaded cells was used as an indicator of invasion. The results showed the invaded cells in the low concentration group was significantly less than that of high concentration group and control group (p < 0.05), however, there was no difference between the latter two groups (p > 0.05) (Figure 5). Therefore, the above results indicated that IL-17 suppressed the metastasis and invasion of cancer cells to a certain extent and showed an antitumor metastasis effect. The effects of IL-17 on the invasive ability of C-33A cervical cancer cells. The invasive ability of C-33A cells was identified by transwell assay after the C-33A cells and PBMCs co-culture system were treated with different concentrations of rhIL-17 (0, 5 and 50 pg/mL) for 48 h. Each experiment repeated six times. Notes: NC, negative control; Low, 5 pg/mL; High, 50 pg/mL; PBMC, peripheral blood mononuclear cells. The effects of IL-17 on the invasive ability of C-33A cervical cancer cells. The number of invasive C-33A cells was calculated by OD value after the C-33A cells and PBMCs co-culture system were treated with different concentrations of rhIL-17 (0, 5 and 50 pg/mL) for 48 h. Data are the mean of six independent experiments ± SEM, *p < 0.05. Notes: NC, negative control; Low, 5 pg/mL; High, 50 pg/mL; PBMC, peripheral blood mononuclear cells; rhIL-17, recombinant human IL-17.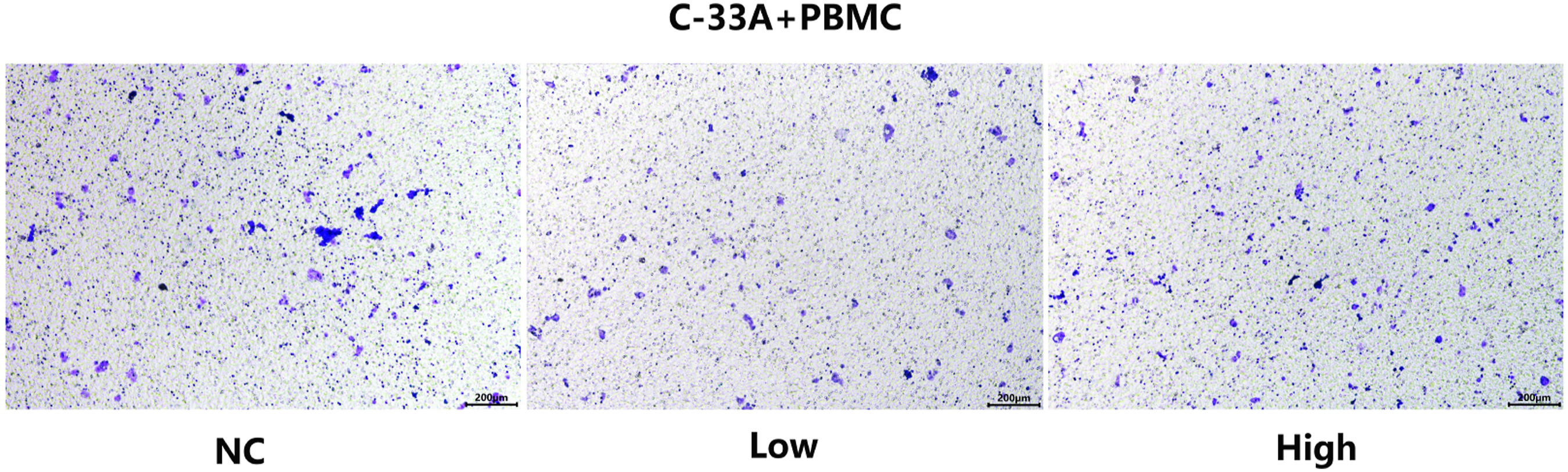
IL-17 is not correlated with expression of VEGF
Vascular endothelial growth factor was very important in tumor angiogenesis. To identify the effects of IL-17 on the expression of VEGF in co-culture system, ELISA was used to detect the levels of supernatant VEGF secreted from the C-33A and PBMC cells. The results showed that there was no difference among each group (p > 0.05) (Figure 6). These results mean that IL-17 may not participate in the expression of VEGF and may also be not involved in tumor angiogenesis. The effects of IL-17 on the tumor angiogenesis ability of C-33A cervical cancer cells. The expression levels of VEGF were detected by ELISA after the C-33A cells and PBMCs co-culture system were treated with different concentrations of rhIL-17 (0, 5 and 50 pg/mL) for 48 h. Data are the mean of seven independent experiments ± SEM, p > 0.05. Notes: NC, negative control; Low, 5 pg/mL; High, 50 pg/mL; PBMC, peripheral blood mononuclear cells; rhIL-17, recombinant human IL-17; VEGF, vascular endothelial growth factor.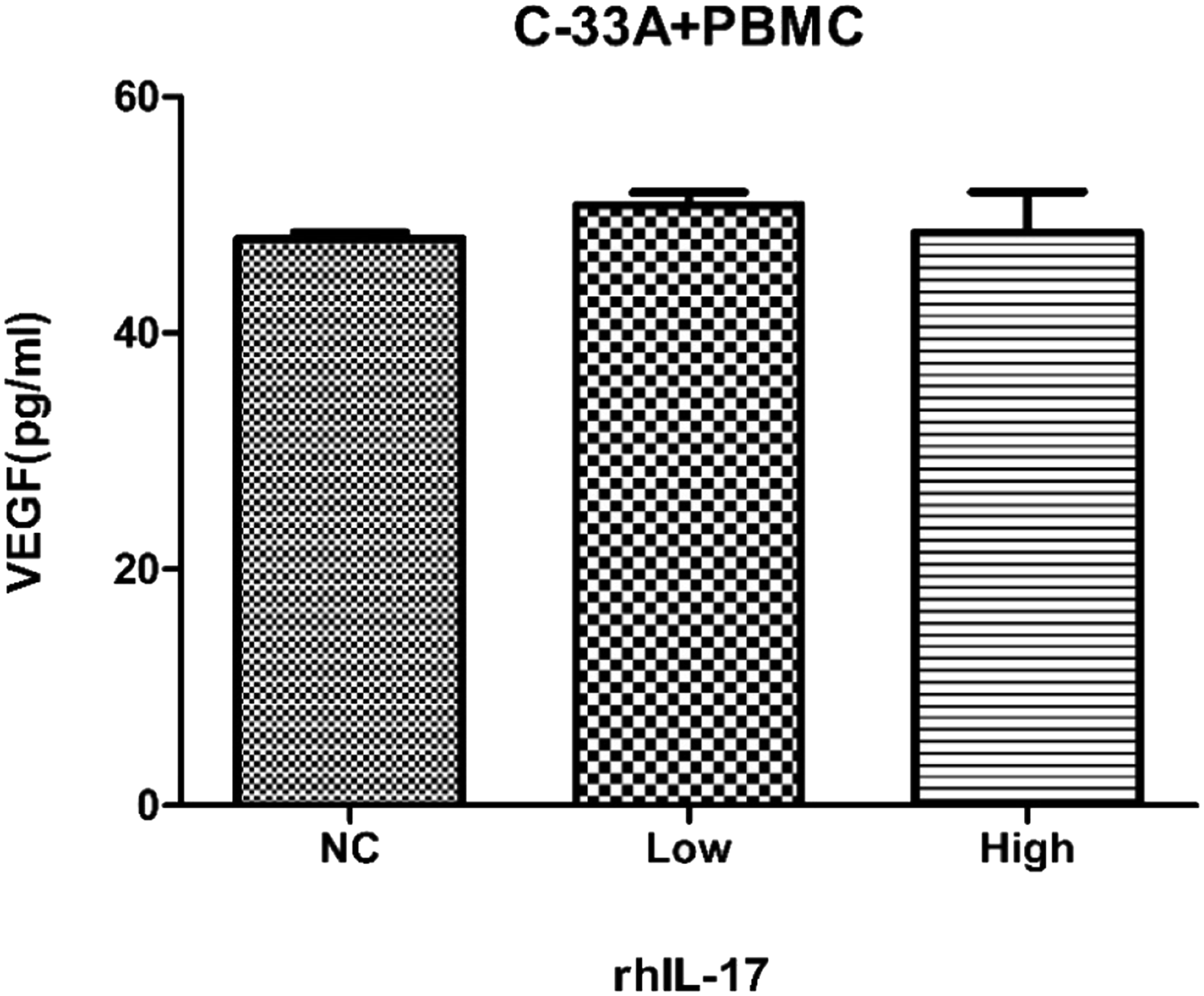
Discussions
Interleukin-17 (IL-17) was a kind of multifaceted cytokine that was discovered in the 1990s, and can be secreted by multiple sources, the most important of which is the Th17 cells. 13 Moreover, IL-17 involved in a variety of physiological and pathological physiology, including cancer, autoimmune diseases, infectious diseases of the immune response.14–16 With the further development of research, the role of IL-17 in many diseases has received widespread attention. According to the results of many researches, IL-17 plays an important role in various diseases.17–22 Most studies suggested that the function of IL-17 was pathogenic rather than protective in the course of the disease. The study of Tartour et al. 23 were the earliest research to support the tumor-promoting effect of IL-17. They found that cervical cancer cells cultured with IL-17 had no influence on cancer cell proliferation in vitro, but the transplanted tumor inoculated with IL-17 cDNA transfected cells in nude mice grew significantly faster. Alves et al. 24 also suggested that Th17 and IL-17 inhibit host immune response instead of protective immune response, and leading to HPV replication and persistent infection, and promoting the growth and progression of cervical tumors. But recently, studies indicated that the role of IL-17 had dual functions of promoting and protecting tumors, in other words, IL-17 supports tumor growth in the early stages of carcinogenesis, while in the established tumors, IL-17 enhances anti-tumor immunity.25,26 The previous studies on IL-17 related to cervical cancer mostly focused on HPV positive side, while only a few studies in correlation with HPV negative have been mentioned in the previous introduction. Therefore, this study was to clarify the relationship between IL-17 mediated immune response and HPV-negative cervical cancer. For this purpose, we established the co-culture system of cervical cancer C-33A cells and PBMC, treated with different concentrations of rhIL-17, and detected the proliferation using CCK-8 method. The results showed that the proliferation rate of C-33A cells slightly increased with the ascending of IL-17 concentration, but there was no difference among each group (p > 0.05). Meantime, after treatment with different concentrations of rhIL-17, we detected the apoptosis using flow cytometry. The apoptosis rate of high concentration group was significantly lower than that of low concentration group and control group (p < 0.05), however, there was no difference between the latter two groups (p > 0.05). The results suggested that IL-17 inhibited cell apoptosis of C-33A cells. Combined with CCK-8, we believed that the increasing of IL-17 concentration could promote the growth of cervical cancer cells, showing a pro-tumor effect in the early stage of carcinogenesis.
Meanwhile, to clarify effects of IL-17 mediated immune response on cervical cancer metastasis and invasion, we detected the invasion ability of cervical cancer cells in co-cultured system, using transwell assay. The results showed the invaded cells in the low concentration group was significantly less than that of high concentration group and control group (p < 0.05), however, there was no difference between the latter two groups (p > 0.05). Therefore, the above results indicated that IL-17 suppressed the metastasis and invasion of cancer cells to a certain extent and showed an antitumor metastasis effect. In addition, to clarify effects of IL-17 in tumor angiogenesis, we detected the levels of VEGF in cervical cancer cells co-cultured system using ELISA assay. The results showed that there was no difference among each group (p > 0.05). It was mean that IL-17 might not participate in the expression of VEGF and had no function in tumor angiogenesis. Combined with the results of transwell assay and ELISA, we speculated that IL-17 can inhibit the development and distant metastasis of cervical cancer in the further stage of tumor.
Based on these, we can see that IL-17 could promote the growth of cervical cancer cells, but inhibit the cancer development and cell distant metastasis. It is like our clinical experience that cervical cancer is often local growth, and less distant metastasis. Therefore, we think that IL-17 is a promising immunotherapeutic target in current cervical cancer research. Nonetheless, this study has some limitations. For example, in this study, the HPV negative C-33A cells were used but a comparison with HPV positive cervical cancer cells is lacking that would underline the findings of the study concerning rhIL-17 and C-33A cells. Moreover, the study was small and there was no power calculation was done for estimation of sample size selected, and IL-17 treatment including various duration and doses must be tried to confirm its effects.
Conclusions
In summary, there is also a close correlation between IL-17 mediated immune response and HPV-negative cervical cancer, showing dual effects in different stages of tumor development, and could be a possible significant influence on tumor proliferation, apoptosis, and metastasis. Therefore, IL-17 is a promising immunotherapeutic target in current cancer research, and the results of this study provide a new supplement of the immunotherapy related to IL-17. The implementation of a one-size-fits-all treatment plan may not be idea, and further studies of immunotherapeutic measures for cervical cancer were needed.
Footnotes
Acknowledgements
The authors would like to thank the participating volunteers and colleagues for the source of blood samples.
Author contributions
Y.P. prepared the blood samples and co-drafted the manuscript. X.L. performed the experiments. J.M. and Z.F. helped with the data statistical analysis and prepared the figures. Y.H. revised the manuscript. J.X. designed the study and drafted the manuscript. All authors approved this manuscript.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: Funding from the program of Wenzhou Municipal Science and Technology Bureau (No. Y20170119).
Ethical approval
Ethical approval for this study was obtained from the Medical Ethical Committee of The First Affiliated Hospital of Wenzhou Medical University (approval no: YS2018-010).
Informed consent
Written informed consent was obtained from each participant before the study. Informed consent declared that all blood samples would be used for the research.
