Abstract
Massicotte A. A practice tool for the new oral anticoagulants. Can Pharm J (Ott) 2014;147:25-32. (Original DOI: 10.1177/1715163513513869).
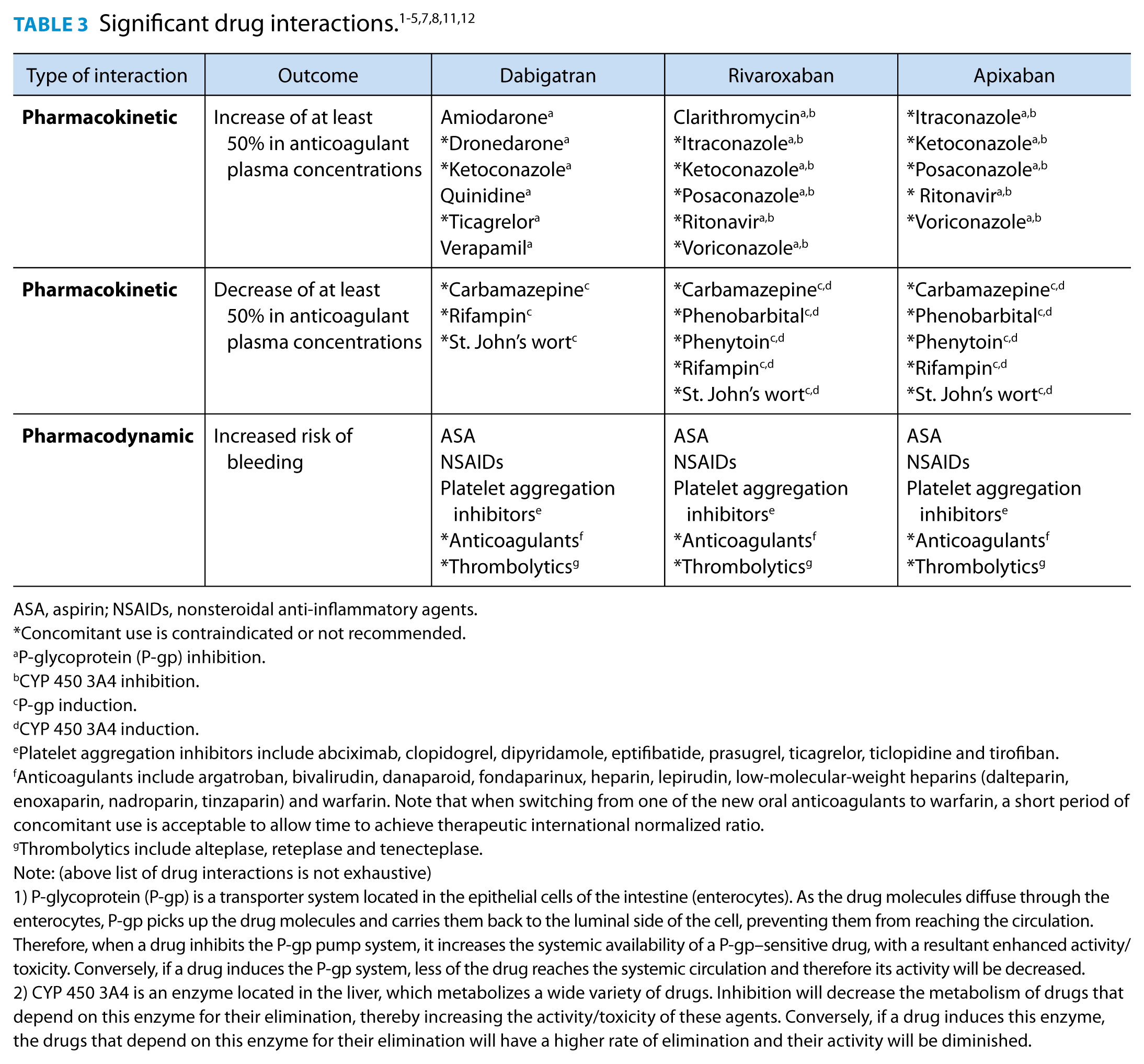
In Table 3 of the above article, there were several footnotes that were incorrectly referenced. The corrected table appears below.
Significant drug interactions.1-5,7,8,11,12 ASA, aspirin; NSAIDs, nonsteroidal anti-inflammatory agents. Concomitant use is contraindicated or not recommended. P-glycoprotein (P-gp) inhibition. CYP 450 3A4 inhibition. P-gp induction. CYP 450 3A4 induction. Platelet aggregation inhibitors include abciximab, clopidogrel, dipyridamole, eptifibatide, prasugrel, ticagrelor, ticlopidine and tirofiban. Anticoagulants include argatroban, bivalirudin, danaparoid, fondaparinux, heparin, lepirudin, low-molecular-weight heparins (dalteparin, enoxaparin, nadroparin, tinzaparin) and warfarin. Note that when switching from one of the new oral anticoagulants to warfarin, a short period of concomitant use is acceptable to allow time to achieve therapeutic international normalized ratio. Thrombolytics include alteplase, reteplase and tenecteplase. Note: (above list of drug interactions is not exhaustive) 1) P-glycoprotein (P-gp) is a transporter system located in the epithelial cells of the intestine (enterocytes). As the drug molecules diffuse through the enterocytes, P-gp picks up the drug molecules and carries them back to the luminal side of the cell, preventing them from reaching the circulation. Therefore, when a drug inhibits the P-gp pump system, it increases the systemic availability of a P-gp–sensitive drug, with a resultant enhanced activity/toxicity. Conversely, if a drug induces the P-gp system, less of the drug reaches the systemic circulation and therefore its activity will be decreased. 2) CYP 450 3A4 is an enzyme located in the liver, which metabolizes a wide variety of drugs. Inhibition will decrease the metabolism of drugs that depend on this enzyme for their elimination, thereby increasing the activity/toxicity of these agents. Conversely, if a drug induces this enzyme, the drugs that depend on this enzyme for their elimination will have a higher rate of elimination and their activity will be diminished.
Type of interaction
Outcome
Dabigatran
Rivaroxaban
Apixaban
Increase of at least 50% in anticoagulant plasma concentrations
Amiodarone
a
Clarithromycina,b
*Itraconazolea,b
*Dronedarone
a
*Itraconazolea,b
*Ketoconazolea,b
*Ketoconazole
a
*Ketoconazolea,b
*Posaconazolea,b
Quinidine
a
*Posaconazolea,b
* Ritonavira,b
*Ticagrelor
a
*Ritonavira,b
*Voriconazolea,b
Verapamil
a
*Voriconazolea,b
Decrease of at least 50% in anticoagulant plasma concentrations
*Carbamazepine
c
*Carbamazepinec,d
*Carbamazepinec,d
*Rifampin
c
*Phenobarbitalc,d
*Phenobarbitalc,d
*St. John’s wort
c
*Phenytoinc,d
*Phenytoinc,d
*Rifampinc,d
*Rifampinc,d
*St. John’s wortc,d
*St. John’s wortc,d
Increased risk of bleeding
ASA
ASA
ASA
NSAIDs
NSAIDs
NSAIDs
Platelet aggregation inhibitors
e
Platelet aggregation inhibitors
e
Platelet aggregation inhibitors
e
*Anticoagulants
f
*Anticoagulants
f
*Anticoagulants
f
*Thrombolytics
g
*Thrombolytics
g
*Thrombolytics
g
Get full access to this article
View all access options for this article.
