Abstract
Background
Non-syndromic hereditary aortic diseases are caused by mutations in genes encoding for connective tissue components, involving structural integrity of aortic tissue. Amongst them, MYH11 gene mutation is a known causative factor for aortic diseases, especially in young patients.
Research Design
We report the case of a 37 years-old male which came to our attention for an acute DeBakey type I aortic dissection. In three different operations he was submitted to a total aortic substitution with a Bentall operation, a Frozen Elephant Trunk and a Thoracoabdominal Aortic open repair. During the last two operations particular technical tips, which are reported in this work, have been adopted to optimize surgical strategy.
Introduction
Connective Tissue Diseases (CTD) are an important risk factor for the development of aortic aneurysms and dissections, especially in young patients. 1 Recent advances in DNA sequencing technologies have identified several causative genes for hereditary aortic diseases, especially in syndromic disorders like Marfan, Loeys–Dietz, and vascular Ehlers–Danlos syndrome. However, a not negligible part of genetically triggered aortic aneurysms and dissections is not part of syndromic diseases. These non-syndromic hereditary aortic diseases (HTAD) result from altered components in the contractile apparatus of vascular smooth muscle cells, which are encoded by genes like ACTA2, MYH11, MYLK, etc. 2 The first reported genetic defect in the smooth muscle contraction apparatus was a mutation in MYH11 gene, encoding for a smooth muscle-specific myosin isoform, the myosin heavy chain 11. 3 However, considering the vastity and complexity of all the possible genetic mutations in potentially involved genes, the largest part of discovered mutations are Variants of Uncertain Significance (VUS), and the field of non-syndromic hereditary aortic diseases remains largely unexplored. Concerning the surgical treatment of these patients, latest guidelines recommend a lower threshold for aortic repair than in general population, being 50 mm or even less in specific cases. Rapid increase in aortic size is at the same time a strong indication for surgery. Regarding the surgical strategy, open repair has always been considered the gold standard in the treatment of aortic diseases in patients with CTD. 4 Endovascular therapy is usually reserved for redo operations or as a bridge in the emergency settings. 5 However, with the refinement of techniques and materials, endovascular therapy is always more and more proposed to these patients, with acceptable results in the midterm follow-up. 6 On the other hand, endovascular interventions for aortic disease in patients with CTD are associated with many device- and aorta-related complications in the long term. Notably, due to the extreme aortic tissue fragility, these patients are particularly subject to two life-threatening endograft-related complications: stent graft-induced new entry tears (SINEs) and retrograde type A aortic dissection (RTAD). Open surgery, on the other hand, provides good long-term results but perioperative morbidity and mortality rates are not negligible. 7 In this scenario, we report the case of a very young man affected by an unknown mutation of the MYH11 gene which was submitted to a three-stage total aortic substitution after a type I DeBakey aortic dissection with a rapid aneurysmal degeneration. The complexity of the case brought us to introduce in the surgical strategy innovative technical tips, which are described and illustrated in this work. The patient provided informed written consent for the publication of this case report.
Description of the case
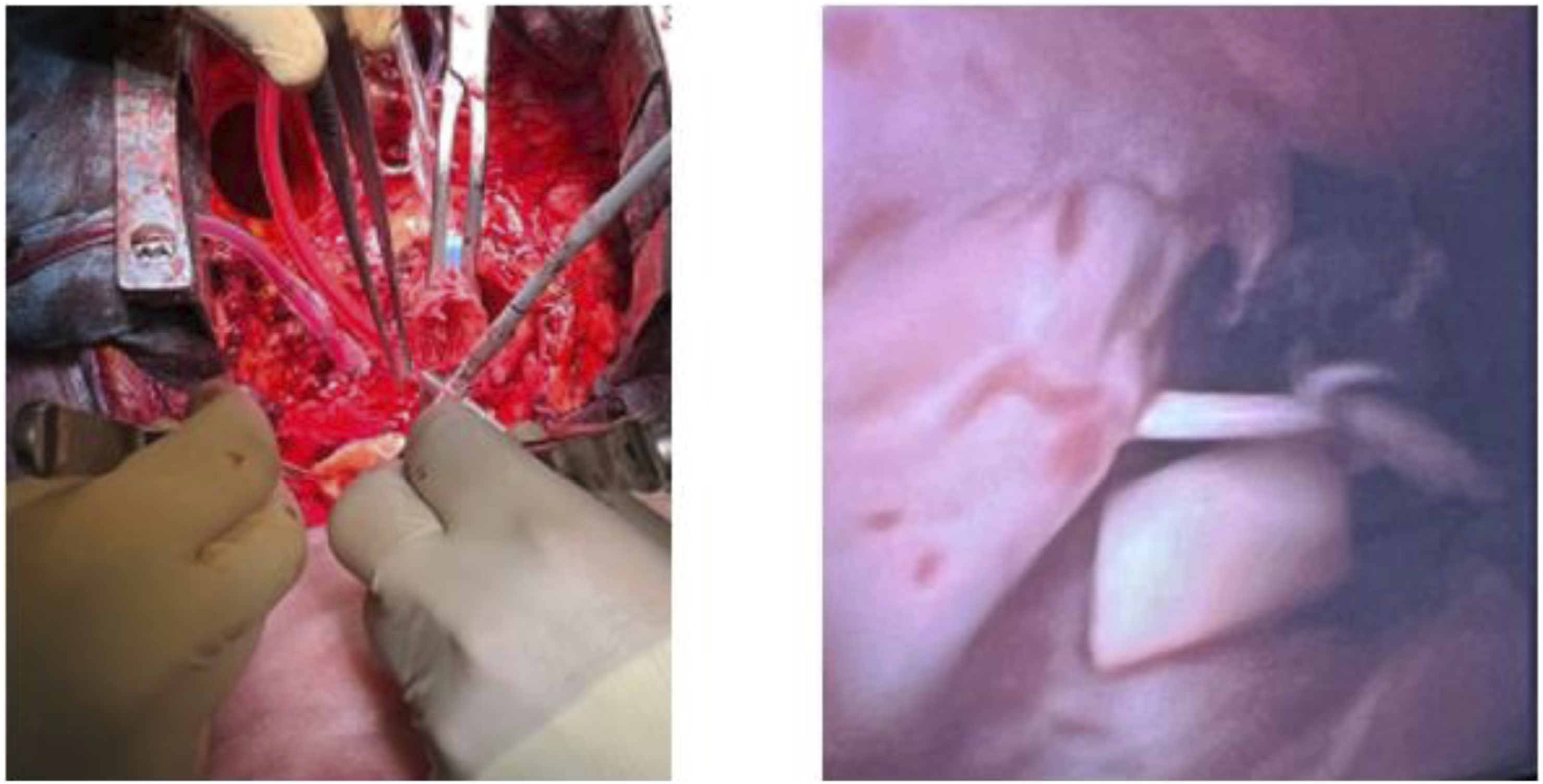
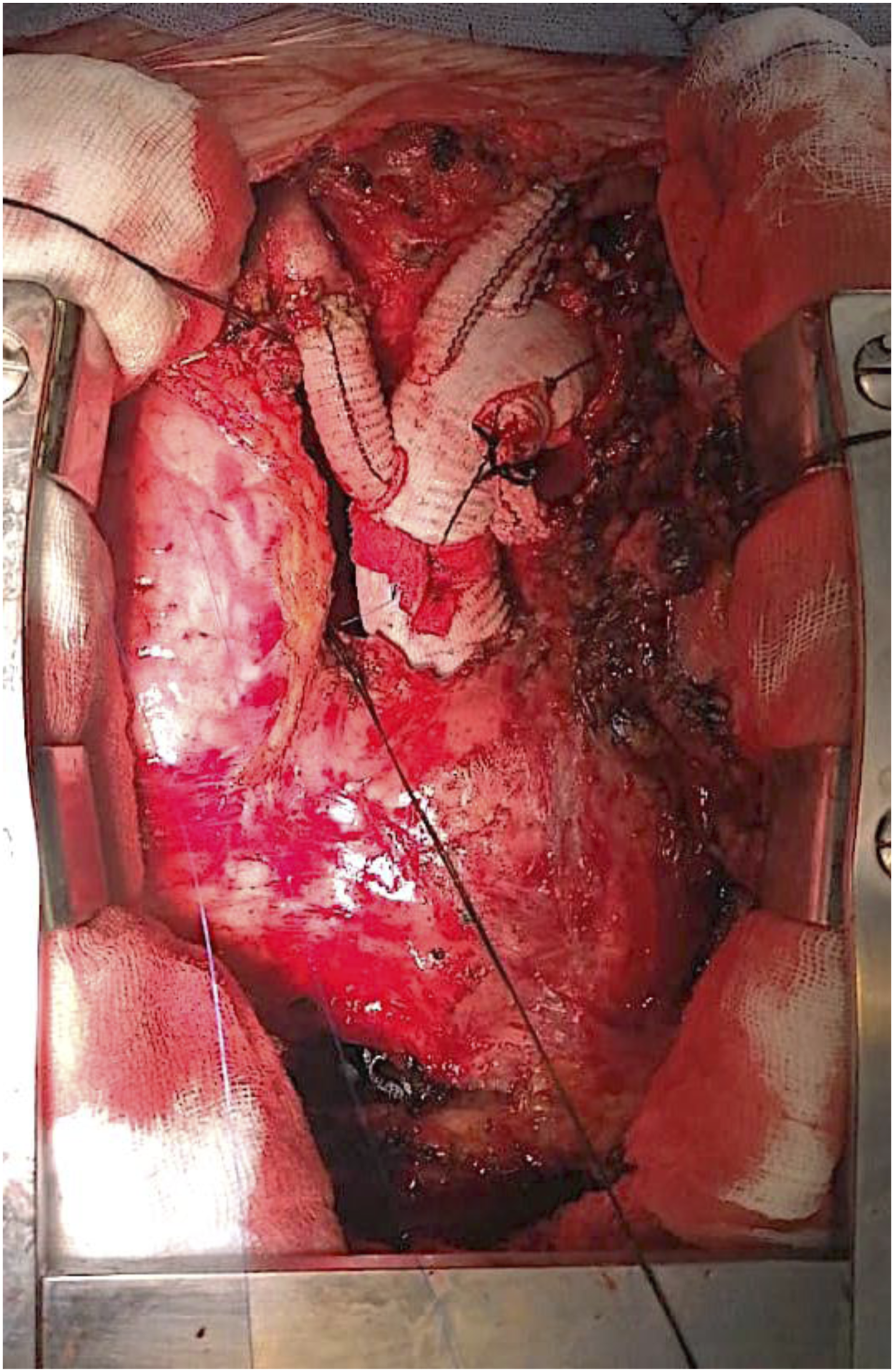
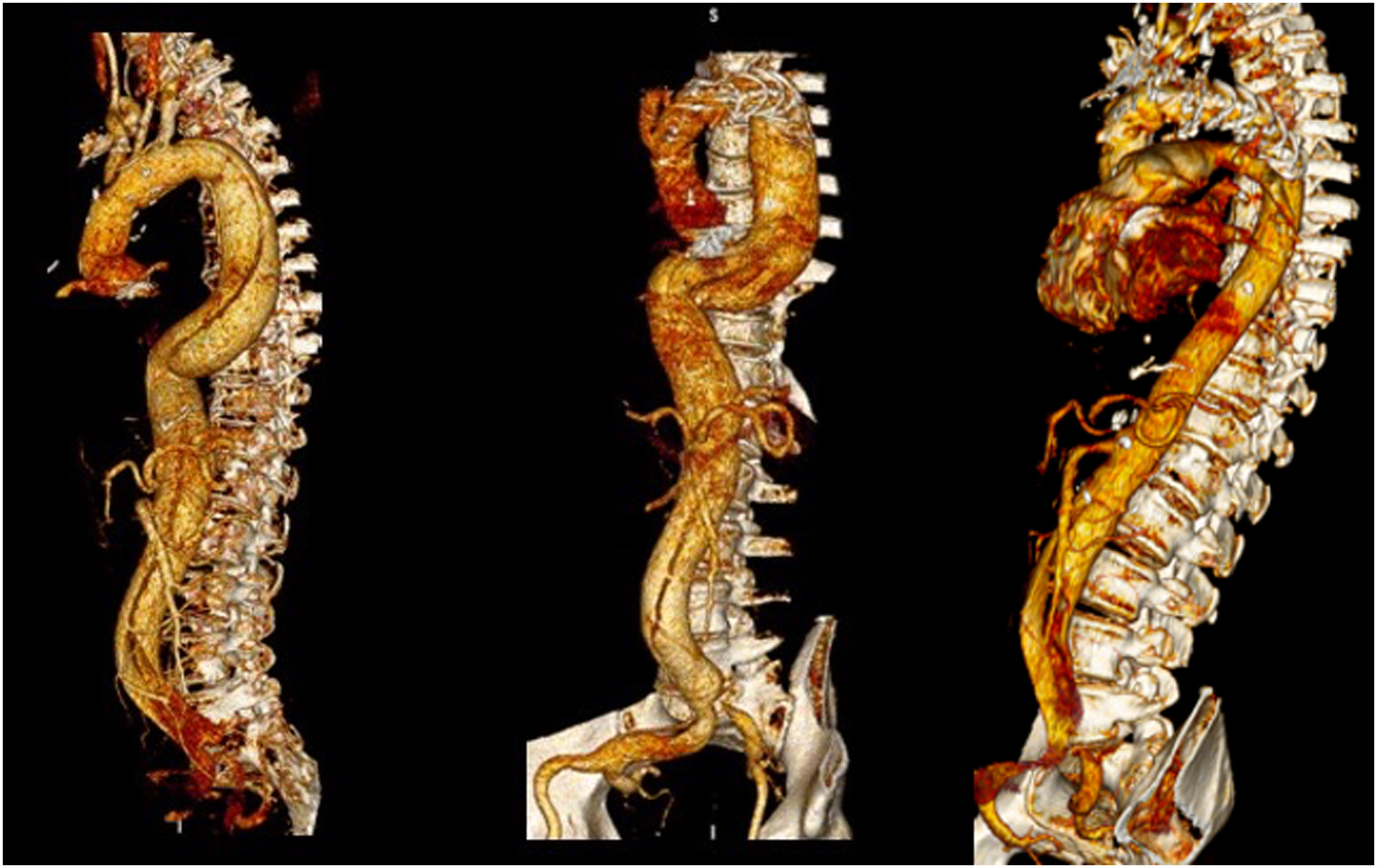
A 37-year-old man with a past medical history of sleeve gastrectomy presented to our attention for an acute DeBakey type I aortic dissection. Maximum diameter of the ascending aorta was 76 mm at the admission Computerized Tomography Angiography (CTA). He was submitted in emergency to a Bentall operation with a mechanical aortic valved graft. (Figure 1) Postoperative course was uneventful. The patient was submitted to a DNA Next Generation Sequencing (NextSeq550DX-Illumina), which resulted in an unknown mutation of MYH11 gene [MYH11(ENST00000300036.6):c.500A>G (p.GIn167Arg)]. The mutation was not known before, so it was considered a Variant of Uncertain Significance (VUS). Patient was regularly followed in the subsequent months until, at the second follow-up CTA, an increase of 5 mm in the diameter of the aorta at the midthoracic level and at the thoracoabdominal junction was noticed. The notable aortic diameter increase occurred in less than 4 months, in comparison to the previous CTA. The maximum aortic diameter reached the threshold of 50 mm, so a decision of an open repair of the rapidly enlarging thoracoabdominal aorta was made, after a surgical repair of the dissected aortic arch. Patient was therefore planned for a Total Aortic Arch. Replacement (TAR) with the Frozen Elephant Trunk Technique in first intention and, after, for total reconstruction of the thoracoabdominal aorta. Patient was submitted to a redo median sternotomy and a surgical preparation of the two axillary arteries. Right atrium was cannulated in standard fashion, an 8 mm Dacron graft was sutured to the two axillary arteries and Cardio-Pulmonary Bypass (CPB) was started. Under Hypothermic Circulatory Arrest at 26°C, aortic arch. was opened, and the dissection lamella was identified and removed under direct vision until Ishimaru Zone 3. Triple selective antegrade cerebral perfusion was started through the interposed Dacron grafts on the axillary arteries and the left common carotid artery, after direct cannulation, according to Kazui technique. To directly inspect the descending thoracic aorta (DTA) a flexible illuminated fiber-optic endoscope (Ambu® aScope™ 4 Large, Ambu A/S, Ballerup, Denmark) was used. A flexible laparoscopic scissor (Aesculap, Inc. Corporate Parkway Center Valley, PA) was linked to the endoscope and introduced into the descending thoracic aorta to perform an extended laminectomy under vision in the DTA, creating a single lumen in the native aorta. (Figure 2) At this point the hybrid prosthesis for FET (Thoraflex Hybrid graft - Vascutek, Inchinnan, Scotland) was deployed. Siena collar was sutured in Ishimaru Aortic Arch. Zone 3. Proximal anastomosis was performed with the distal end of the already replaced ascending aorta. Supra-aortic trunks were sequentially anastomosed to the three dedicated Thoraflex branches (Figure 3). Total CPB time was 130 minutes while HCA time was 30 minutes. Patient returned to ward from intensive care unit on postoperative day (POD) 3. Recovery was uneventful and he was discharged home on POD seven without any complication. After a complete recovery, the patient was scheduled for second operation after 3 months from the TAR. A preoperative CTA showed a further increase in aortic size and a good surgical result of the previous operation. (Figure 4) For the subsequent operation the patient was prepared and monitored in the usual fashion.
8
A spinal drain catheter was placed for cerebrospinal fluid drainage (CSFD). A thoraco-phreno-lombotomy was performed. Thoracic cavity was entered through the fifth intercostal space and the whole descending thoracic aorta was prepared. Abdominal aorta and its branches were carefully dissected through a retroperitoneal approach. The patient had a separate direct origin of the common hepatic and the splenic artery from the aorta. Left Heart Bypass (LHBP) was instituted by cannulating the left atrium via the left inferior pulmonary vein with a 24 Fr cannula and the right femoral artery with a 16 Fr cannula. Left common femoral artery was not used for retrograde perfusion for a flow-limiting dissection of the common iliac artery. A CytoSorb® cartridge was included in the LHBP circuit.
9
Prior to proximal aortic clamping, an intraoperative echography directly on the aortic aneurysm wall was performed to precisely locate the end point of the Thoraflex endograft (VIDEO). This point was marked on the aortic wall, to facilitate the identification of the proximal clamping site. A straight Dacron graft (Vascutek, Inchinnan, Scotland) was chosen for repair. The extremity of the Thoraflex Hybrid graft was clamped inside the native aorta. During aortic clamping, Hepatic Artery (HA) and Superior Mesenteric Artery (SMA) were selectively perfused with isothermic blood from LHB through 9 Fr Pruitt catheters while renal arteries were selectively perfused with 700 mL of Custodiol® solution (Dr Franz Köhler Chemie, Bensheim, Germany) through coronary cannulae.
8
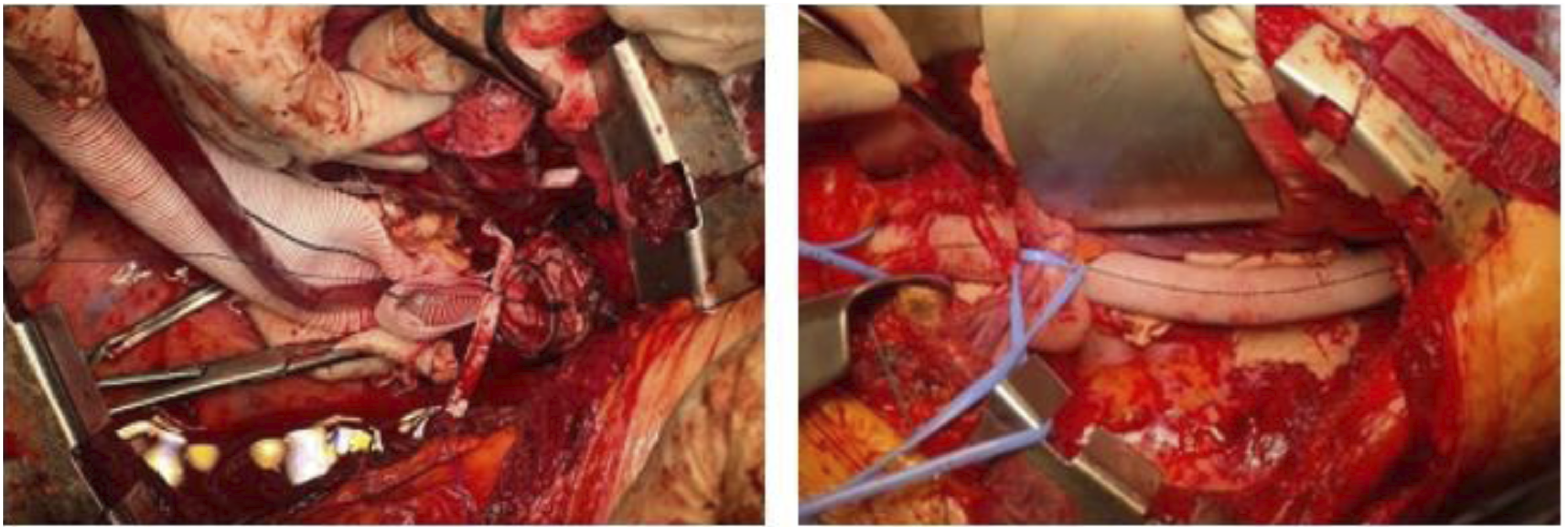
Splenic artery was ligated. The proximal anastomosis was performed directly between the Thoraflex extremity and the Dacron graft. Distally a bevelled anastomosis was performed to include the right renal artery. Left renal artery, HA and SMA were directly reimplanted on the prothesis. (Figure 5, VIDEO). Total LHB time was 110 minutes. Patient was extubated on POD 1, transferred to ordinary ward on POD 5 and discharged home on POD 9. At 6 months follow-up the patient has no operation-related sequelae. Final intraoperative picture of Bentall operation. Intraoperative pictures showing the septotomy of the Descending Thoracic Aorta (DTA) performed under vision thanks to a flexible laparoscopic scissor linked to an endoscope (left) and the interior vision of the dissected DTA (right). Final intraoperative picture of the Total Aortic Arch Replacement (TAR) with the Frozen Elephant Trunk (FET) technique. Postoperative Aortic 3-D reconstructions after Bentall operation (left), Frozen Elephant Trunk (middle), and open ThoracoAbdominal Aortic repair (right). Intraoperative pictures showing the proximal anastomosis between the distal end of the FET hybrid prosthesis and the Dacron graft used for the thoracoabdominal aortic reconstruction (left) and the final result after the Thoracoabdominal Aortic Aneurysm (TAAA) open repair (right).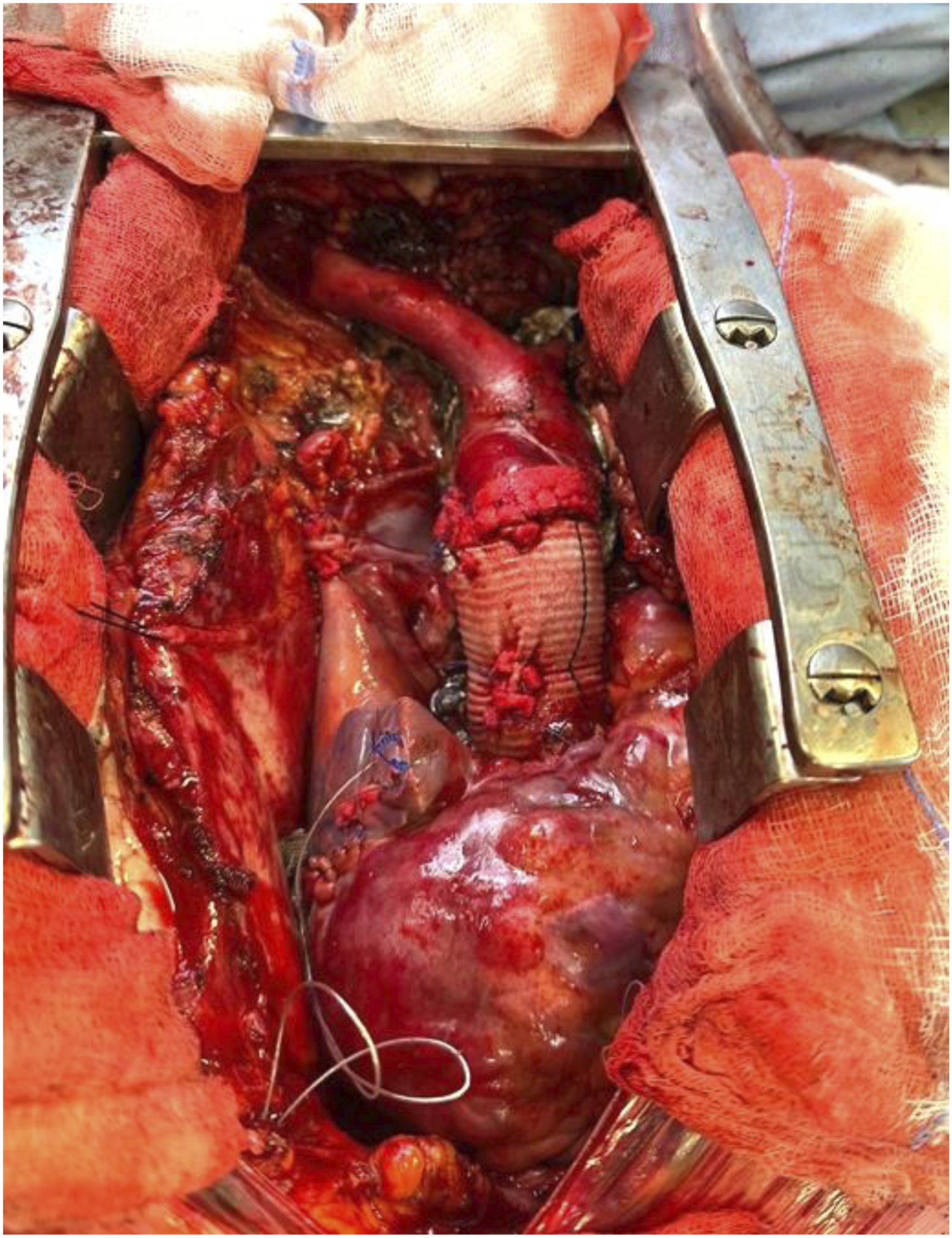
Discussion and conclusions
Connective Tissue Diseases have a role of the utmost importance in the development of aortic aneurysms and dissections in young patients. Even if this population is younger and with less comorbidities than patients who develop degenerative aortic aneurysms, the complexity of the underlying disease and the multiple aortic operations often make the surgical strategy really challenging. Open repair is still considered the gold standard for CTD- related aortic diseases, with low aortic-related mortality rate and procedure-related reintervention rate at follow-up. However, perioperative morbidity and mortality rates are considerable, especially considering the population of patients who is submitted to extensive aortic substitutions. 10 On the other hand, it is easily predictable that endovascular surgery will be always more frequently proposed to these patients in the next future. We reported the case of a very young man with a non-syndromic hereditary aortic disease, namely, a MYH11 gene mutation who suffered of a DeBakey type I aortic dissection. For a rapid aneurysmatic progression, this patient was successfully submitted to a three-stage complete aortic substitution, starting from the aortic root and finishing to the infrarenal aorta. Furter studies are needed to better investigate the population of CTD-related aortic diseases and to provide them better open, endovascular or hybrid surgeries in the next future.
Supplemental Material
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Supplemental Material
Supplemental material for this article is available online.
Appendix
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
