Abstract
Objectives
Mediterranean spotted fever is a common zoonosis in Europe caused by Rickettsia conorii bacterium. Among its wide range of clinical presentations, arterial thrombosis of large vessels has never been described before.
Methods
We report a case of a complete acute infrarenal aortic thrombosis in a 61-year-old male with R. conorii infection.
Results and Conclusion
The patient was successfully operated using open aortic surgery and subsequent treatment with doxycycline. To our knowledge, this is the first report of aortic thrombosis associated with infection by this parasite, extending the clinical spectrum of the disease.
Introduction
Mediterranean spotted fever (MSF) is an infection caused by Rickettsia conorii (RC) bacterium. It induces a state of hypercoagulability and vasculitis, which leads to an increased risk of developing thrombotic complications. 1 Complete acute occlusion of the infrarenal abdominal aorta is a rare event with a mortality rate of up to 75%. 2
We report a case of complete acute thrombosis of the infrarenal aorta in a patient diagnosed with RC infection. To our knowledge, this is the first report of aortic thrombosis associated with infection by this parasite, extending the clinical spectrum of the disease.
Case report
A 61-year-old male, current smoker, was admitted to the Emergency Department (ED) for low back pain with 48 Hours evolution, lower limbs pain and fever. On admission, blood pressure was 108/58 mmHg, temperature was 38°C, and no arrhythmias were detected. Patient was confused and with deteriorated general condition. There were no neurological, cardiorespiratory, or abdominal symptoms. Physical examination revealed maculopapular rash on the trunk and upper limbs and two necrotic center injuries, one in the right groin and the other in the outer peroneal malleolus (Figure 1). Vascular examination revealed pulseless, coldness, and paleness lower limbs. Laboratory tests showed serum creatinine of 1.26 mg/dL, a C-reactive protein concentration of 153 mg/L, a procalcitonin value of 0.64 ng/mL, a leukocyte count of 7.21 × 10−3/μL with 79% neutrophils, and a platelet count of 104 × 10−3/μL. Standard coagulation parameters were in normal range. Tache noire: Ulcerative lesion, covered by a black eschar and surrounded by an erythematous halo.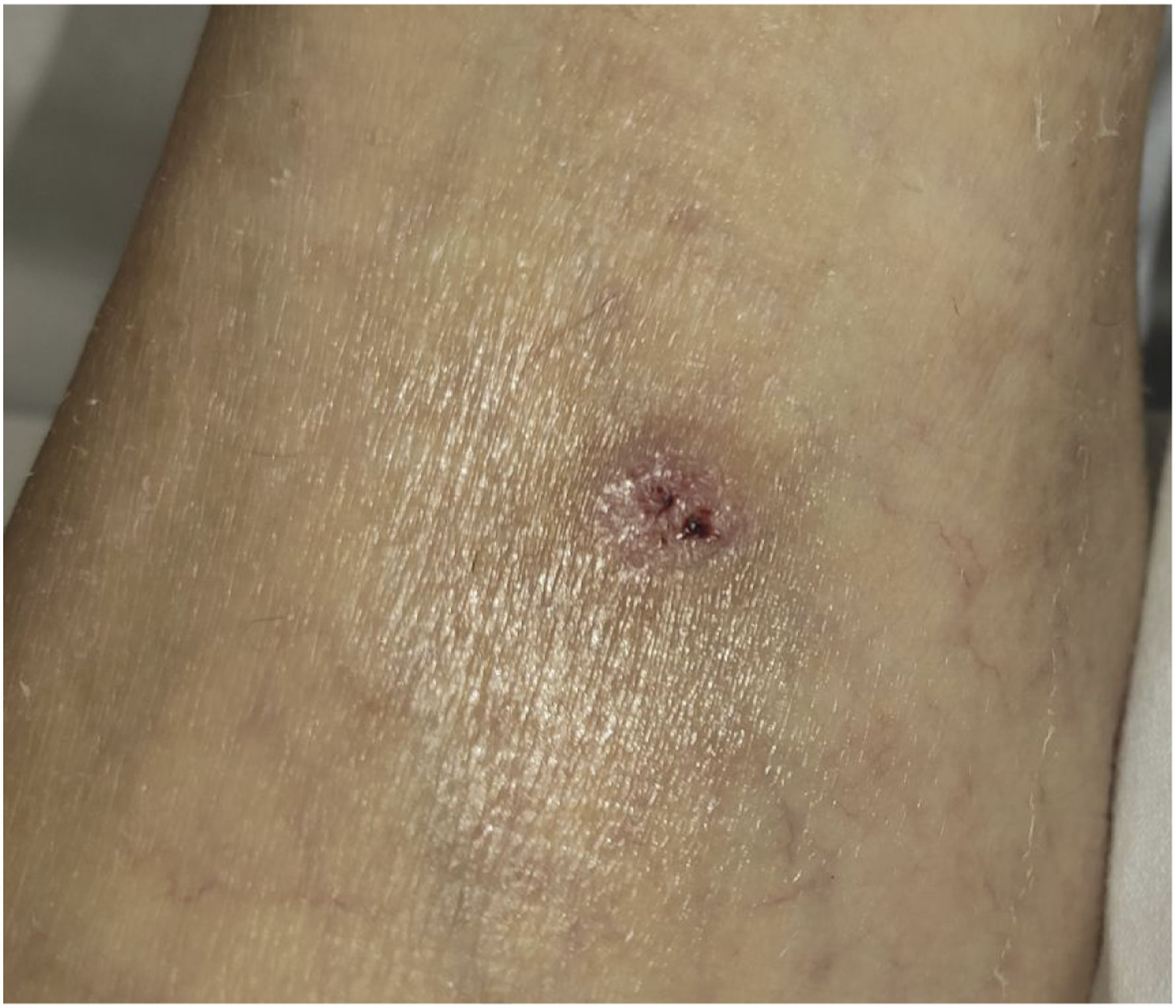
Lumbar magnetic resonance imaging did not reveal infectious foci or spinal pathology. Computed tomography angiography (CTA) scan showed the presence of anechoic thrombus in the aorta, which extended from the celiac trunk to the iliac bifurcation, and which was occlusive immediately below the renal arteries (Figure 2). Renal, femoral, superior, and inferior mesenteric arteries were permeable. Computed tomography angiography scan showed the presence of anechoic thrombus in the aorta, which extended from the celiac trunk to the iliac bifurcation, and which was occlusive immediately below the renal arteries.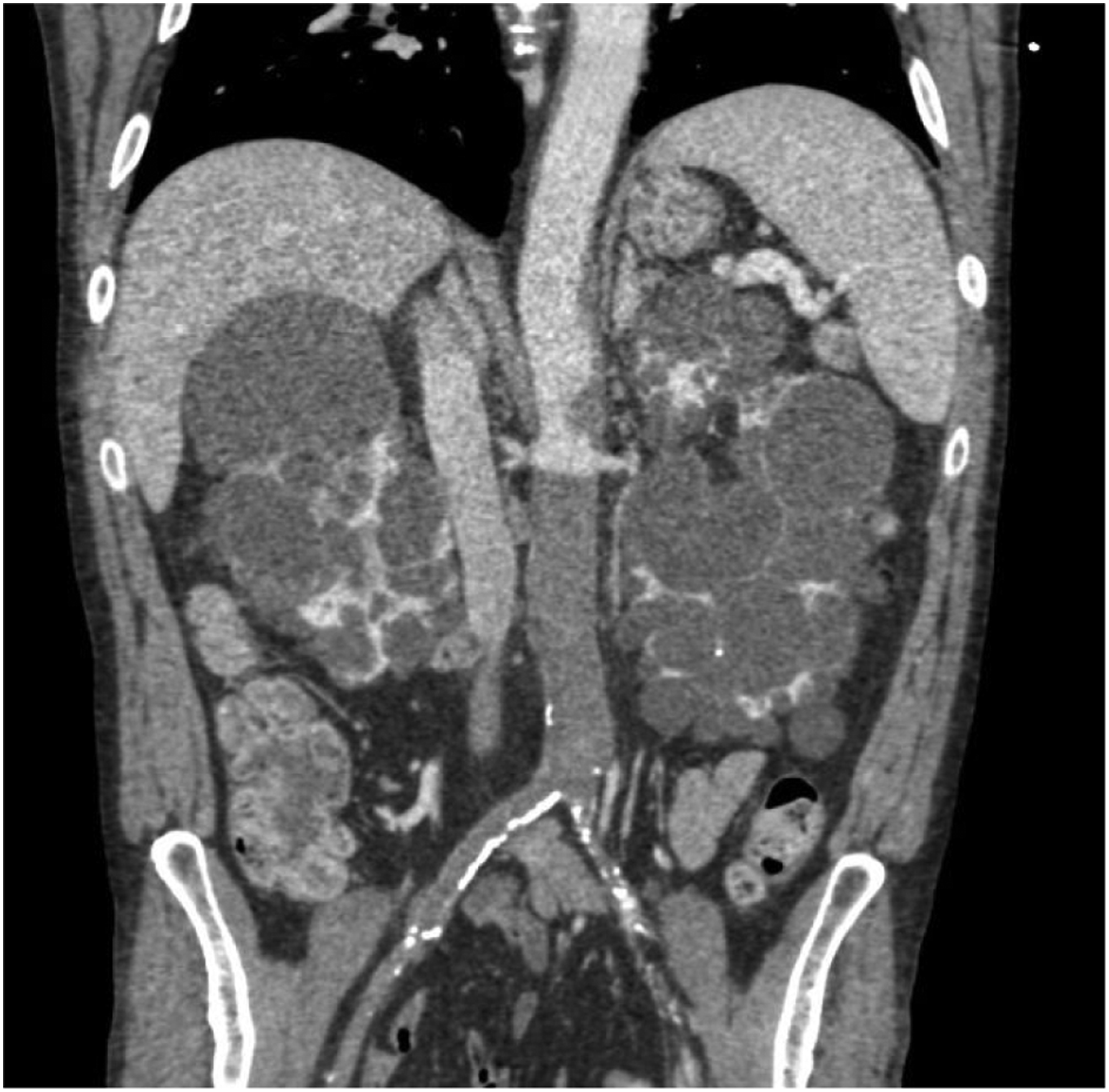
Since the patient was haemodynamically stable, without abdominal symptoms and lower limb pain was under control, it was decided to start treatment with systemic anticoagulants and broad-spectrum antibiotics pending ruling out infectious foci. Transthoracic echocardiogram, blood culture, central venous catheter culture, serologies for hepatitis B virus, hepatitis C virus, human immunodeficiency virus, treponema pallidum, and SARS-CoV-2 tests were negative, so it was oriented as fever of unknown origin in the context of acute aortic thrombosis.
In the following days, the patient improved without new febrile peaks. Thus, it was decided to perform surgical treatment of the aortoiliac occlusive pathology. Aortobifemoral bypass with 16 × 8 mm Dacron bifurcated graft was performed. Intraoperatively, acute thrombus and atherosclerosis plaques were visualized in the wall of the arteries. In addition, small arterial caliber and abnormal fragility of the vessels were highlighted.
The patient improved with resolution of the back and lower limbs pain and without new febrile peaks. The patient was discharged on the 12th postoperative day with a good general condition and presence of distal pulses in both lower limbs.
Seven days after discharge, the patient was admitted to the ED for a new febrile peak of 38°C. CTA scan ruled out infectious foci and showed post-surgical changes in relation to the aortobifemoral bypass. In the physical examination, the persistence of an injury with a necrotic center on the left ankle was noted. This injury resembled a sting, so the patient was interviewed about this. He reported that during SARS-CoV-2 lockdown, 1 month before aortic surgery, he was in contact with tick-carrying dogs; this fact was not previously mentioned. Taking into account the findings of fever, contact with dogs and the injury with necrotic center, MSF was suspected and Rickettsia serology was requested. IgM and IgG test were positive for RC. Targeted treatment with intravenous doxycycline was started with satisfactory evolution and normalization of the analytical parameters of infection and inflammation. The patient was discharged with oral antibiotic treatment (200 mg doxycycline for 15 days).
Seven days later, the patient returned with episodes of dizziness with hypotension. CTA scan revealed left acute renal artery thrombosis, aortobifemoral bypass was permeable without complications. Since serum creatinine was similar to this seen in earlier hospital admissions with maintained diuresis, a conservative approach with systemic anticoagulation treatment were decided. Thrombophilia and autoimmunity studies were requested with negative results. In the following days, the patient did not suffer any new episodes of dizziness or hypotension. Therefore, he was discharged with low molecular weight heparin anticoagulation (LMWH).
In the last follow-up, 15 months after the intervention, the patient remained asymptomatic and reported walking without claudication. Doppler ultrasound showed permeability of the aortobifemoral bypass without any complication.
Discussion
MSF is the most frequent rickettsiosis in Europe. 1 It is caused by RC, which is a Gram-negative obligate intracellular bacterium.1,3 The main vector of MSF is the dog tick, Rhipicephalus sanguineus. The usual hosts are dogs, while humans constitute an accidental host in the biological cycle of ticks. 1 Between 85% and 91% of patients with MSF report previous contact with dogs. 4
The disease incidence has a seasonal variation, being more prevalent in the hottest months. 1 Typical clinical features include fever, headache, myalgias, generalized maculopapular rash, and inoculation eschar “tache noir” at the site of the tick bite.1,3 The course of the disease is usually benign, but in up to 10% of cases more severe symptoms can be observed, with a mortality of 2.5–5%.3,5,6
Detection of specific antibodies (IgM and IgG) by indirect immunofluorescence is the most commonly used method for its diagnosis due to its availability, sensitivity, specificity, and speed. 5 The treatment of choice is doxycycline. 7
MSF shares with other rickettsiosis one dominant feature, widespread microvascular injury. The pathophysiologic effects of vascular injury include increased vascular permeability and activation of inflammatory and coagulation mechanisms. Endothelial dysfunction caused by Rickettsia infection results in haemostostatic alterations that lead to a state of hypercoagulability, due to platelet activation and the release of clot-promoting factors. 6
Several cases of Rickettsia infection with associated vascular thrombosis have been reported in the literature. Vicente et al. describe three cases of deep vein thrombosis of the lower limbs in patients with MSF. 8 Prete et al. report a case of encephalitis in the context of MSF due to thrombosis of the upper ophthalmic vein and the inner middle brain vein. 3 Landau describes a case of mesenteric vein thrombosis as a complication of MSF. 9 Beselga et al. publish a case of retinal artery occlusion in the context of MSF. 5 Ben Brahim et al. give a case of pulmonary thrombosis as a complication of MSF. 6 However, no case of aortic thrombosis associated with Rickettsia infection has been previously reported.
Complete acute infrarenal abdominal aortic occlusion is a rare but potentially catastrophic event, with described mortality rates of up to 75% and the major amputation rate can reach 30%. 2 Its actual incidence is unknown, but some authors refer to 1–4%. 10 The most common cause is of a thrombotic origin, either in patients with atherosclerotic pathology, patients with aortic aneurysm, or with a state of hypercoagulability or vasculitis. 10 Hypercoagulable states may play an important role in aortic occlusive disease, especially when they are superimposed on preexisting large vessel arteritis or atherosclerotic arterial disease. 2 The most common symptoms are pain, pallor, coldness, pulselessness, paresthesia, and paralysis of the lower extremities. Sometimes the peripheral neurological symptoms predominate, which can lead to a clinical picture of spinal pathology or stroke. This may cause aortic lesions to be overlooked and lead to delays in diagnosis.2,10
Possibilities for surgical treatment include thromboembolectomy, thrombolysis, open aortic surgery with anatomical or extraanatomical bypass reconstruction, and endovascular treatment using covered stents. 2
We report a case of acute infrarenal aortic thrombosis in a patient diagnosed with Rickettsia infection. Ischemic symptoms of the lower limbs were present, although they were attenuated due to the presence of collateral circulation. This allowed surgical delay until a complete preoperative study of the patient was carried out. Due to the extension of the thrombosis to iliac bifurcation and the patient’s age, it was decided to perform an aortobifemoral bypass with a 16 × 8 mm Dacron bifurcated graft.
It should be noted that no surgical samples were sent for analysis because no infectious disease was suspected. However, the clinical picture, the typical rash, the positive serology for RC and the season of the year (early summer), led to suspect that this was a case of aortic thrombosis caused by Rickettsia infection.
Despite a late diagnosis of Rickettsia infection, the patient improved after surgery and targeted antibiotic treatment with doxycycline. The fact that the patient had renal artery thrombosis made us suspect that he still had a hypercoagulable state, since antibiotic treatment had not been completed and, therefore, the infection was not completely resolved. This was the reason why it was decided to keep up anticoagulant treatment with LMWH. In follow-up at 15 months the patient was asymptomatic and without complications.
Conclusion
In conclusion, although MSF is usually benign, serious vascular complications could develop. In this sense, R. conorii infection should be considered in the differential diagnosis of patients presenting with large vessel thrombosis and fever, especially if it includes previous contact with (tick-carrying) dogs. After confirm the diagnosis, anticoagulant treatment should be evaluated until the infection has been resolved to avoid spreading thrombosis in other areas.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Informed consent
Consent was obtained from the patient for the publication of this case report.
