Abstract
Background
Current neurointerventional procedures are expanding the use of large bore microcatheters, of up to 0.033” inner diameters, to accommodate intrasaccular flow disruptors or neck-bridging devices, including flow diverters. The use of large bore microwires may mitigate the ledge gap between wire and catheter, facilitate navigation and offer support in distal tortuous anatomy. We aim to report our early experience using the novel Aristotle (Scientia Vascular, West Valley City, UT) 18 and 24 microwires in neurovascular interventions.
Methods
We analysed neurointerventional procedures in which the Aristotle 18 and 24 microwires were used at a single centre. Prospectively collected data, from March 2022 to February 2023, including patient's clinical outcome (successful target vessel, aneurysm catheterisation, peri-procedural complications (thromboembolic, haemorrhagic, vessel dissection or perforation) were analysed.
Results
Overall, the use of Aristotle 18 and 24 microwires was recorded in 84 neurointerventional procedures during the study period, including endovascular aneurysm treatment (n = 30), endovascular thrombectomy (n = 46), dural venous sinus manometry/stent placement (n = 7), and extracranial carotid artery stent placement (n = 1). The Aristotle 18 microwire was used in conjunction with 0.021” microcatheters and the Aristotle 24 microwire with the 0.027 or 0.033” microcatheters. In all cases (100%), the target vessel or aneurysm was reached with the microwire, allowing seamless advancement of the selected microcatheters. No procedure related complications were recorded.
Conclusions
The use of the Aristotle 18 and 24 microwires in neurointerventional procedures is feasible and safe. The microwires provide reduced ledge gap, improved torquability, support and safety over standard 0.014” microwires.
Introduction
Micro-guidewires used in neurointerventional procedures typically range from 0.007” to 0.014” and are used to navigate microcatheters to the desired vessel or anatomic structure. To achieve successful, safe and seamless endovascular navigation, guidewires available for commercial use offer different advantages according to their technical properties. The wires are primarily selected depending on the microcatheter size of choice, ease of navigation and support to achieve the desired outcome. The different technical properties include variations in their length, diameter, stiffness, visibility under fluoroscopy, torque, trackability, steerability, shape and shape retention.
Current neurointerventional procedures are increasingly expanding the use of large bore microcatheters, of up to 0.033” inner diameters, to accommodate larger intrasaccular flow disruptors or neck-bridging devices, such as the woven endovascular bridge (WEB) (Microvention, Aliso Viejo, CA), Contour (Cerus Endovascular inc, Fremont, CA) device, flow diverting stents for the treatment of large and wide necked aneurysms, as well as large stent retrievers for endovascular thrombectomy (EVT).1–3 However, these large bore microcatheters are commonly used with markedly smaller 0.014” microwires. The disparity in the microcatheter and microwire diameters causes larger gaps between the two, known as the ledge gap, likely creating a “ledge effect” during endovascular navigation, particularly around tortuous anatomy and branching vessels. 4 The ledge effect experienced may increase the risk of endothelial injury and preclude successful microcatheter navigation to the desired vascular target.
The Aristotle microwires are a new generation of guidewires used in neurovascular procedures and are available in 0.014” (14), 0.018” (18) and 0.024” (24) diameters sizes (Figure 1). 5 The larger diameter of these microwires is designed to offer increased support, smoother navigation and helps to mitigate the ledge effect, whilst maintaining the distal microwire softness and tip shape (Figures 2 and 3). Herein, we describe our early experience with the Aristotle 18 and 24 microwires during neurointerventional procedures at a single centre.
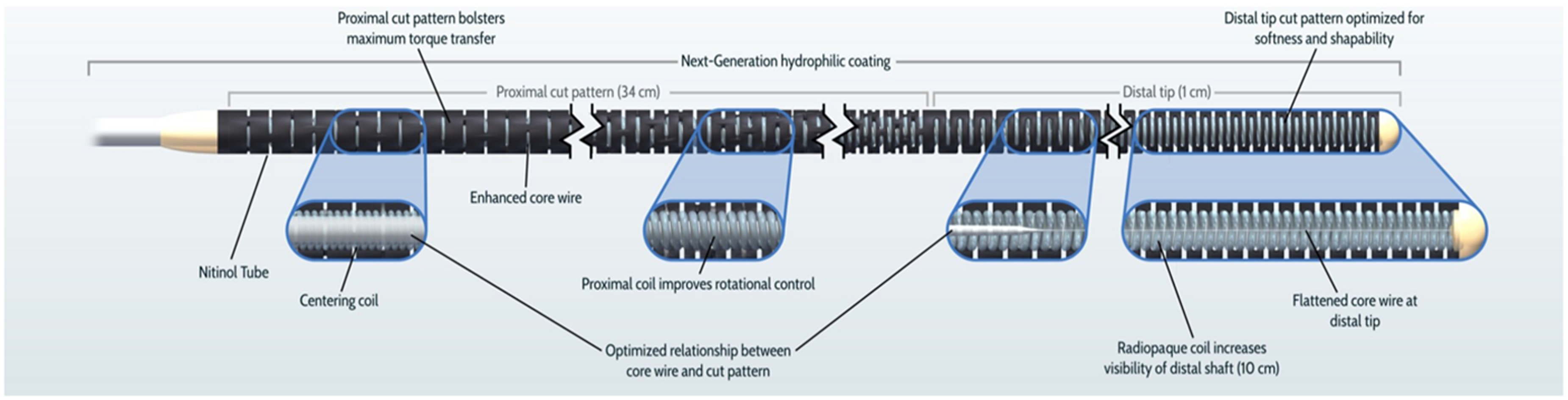
Schematic diagram illustrating the structure and properties of the Aristotle microwire. (Reproduced with permission from Scientia Vascular Inc).
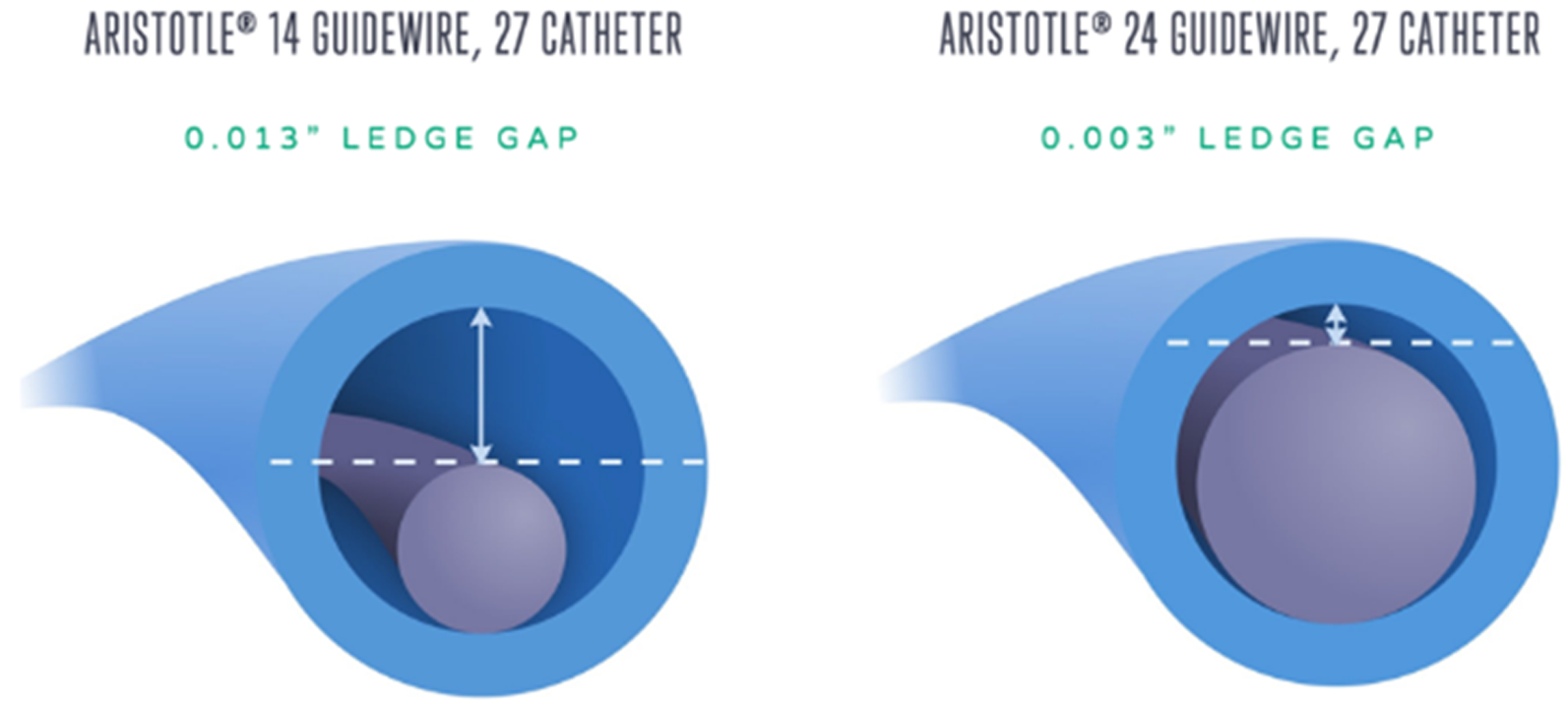
Schematic diagram demonstrating the ledge gap when the Aristotle 14 and Aristotle 24 microwires are used in combination with an 0.027 microcatheter. (Reproduced with permission from Scientia Vascular Inc).
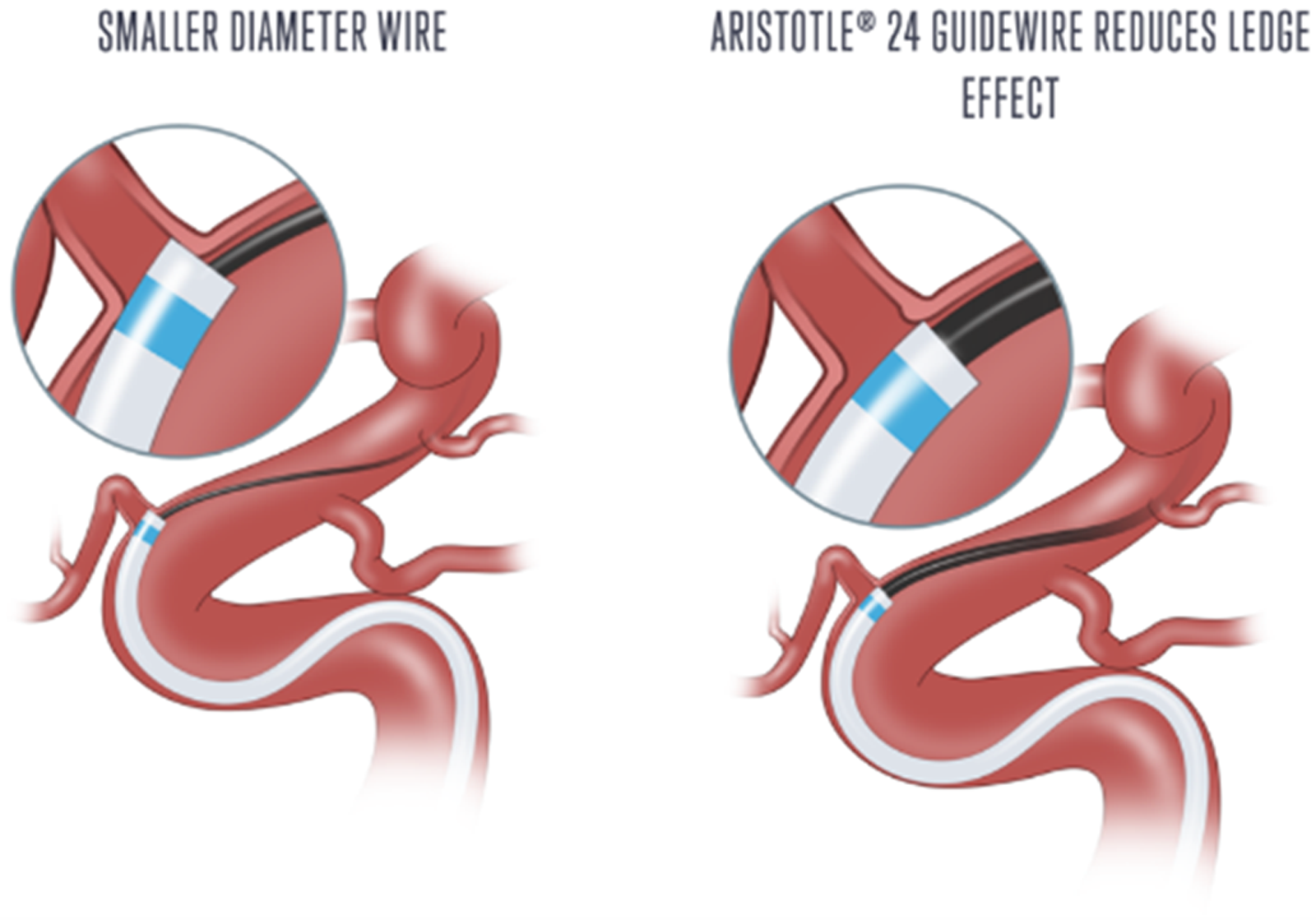
Schematic diagram demonstrating the reduced dimensional differences between a microcatheter and the Aristotle 24 guidewire which minimises the catheter “ledge effect” for smoother tracking through vascular anatomy. (Reproduced with permission from Scientia Vascular Inc).
Methods
Ethics
This study was registered with and approved by the local institutional board review. Retrospective patient consent was not required for this study which was conducted in a de-identified manner. Data that support the findings of this study are available upon reasonable request.
Data source and study design
We performed a retrospective analysis on prospectively collected data according to the Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) guidelines, for all adult (≥18 years) patients undergoing consecutive neurointerventional procedures using the Aristotle 18 and 24 microwires at a single tertiary neuroscience centre, between 1st March 2022 and 28th February 2023 (primary study period). We also retrospectively reviewed 50 consecutive neurointerventional procedures which utilised the 0.014 Synchro microwire between 1st July 2021 to 1st January 2022 (secondary study period). The inclusion criteria for this study included any emergent or elective neurointerventional procedure aiming endovascular treatment for haemorrhagic and ischaemic stroke, extracranial carotid artery stent placement, dural venous sinus manometry and stent placement during which the Aristotle 18 or 24 microwire, or the Synchro 0.014 microwire was utilised.
Neurointerventional procedures
Except for elective internal carotid artery stenting, dural venous sinus manometry and three mechanical thrombectomies, all other procedures were performed under general anaesthesia. At our institution, patients undergoing intracranial flow diversion, elective endovascular coil embolisation and WEB intrasaccular device implantation are loaded with 300 mg oral aspirin and 300 mg oral clopidogrel in the night before and in the morning of the procedure. Prior to the procedure, we routinely assess the P2Y12 inhibition with VerifyNowTM to guide the antiplatelet therapy. The procedures are performed either via transradial or transfemoral approaches, with systemic heparinisation targeting ACT levels 2.5 times the baseline value.
The procedures were performed with either biaxial or triaxial platform, consisting of a guide catheter (long sheath), an intermediate catheter and a microcatheter. During the primary study period, the microwire of choice for 021 microcatheters was the Aristotle 18 200 cm and for the 027 and 033 microcatheters was the Aristotle 24 200 cm.
The patients are followed up with serial imaging, consisting of CT head and neck angiogram at one month, MRI head and neck vessel angiogram at three months and catheter cerebral angiogram at six months post discharge. Additionally, the patients are followed up with telephone call and/or outpatient clinic assessment.
Tracking of each patient's clinical outcomes (successful target vessel/aneurysm catheterisation/peri-procedural complications (thromboembolic, haemorrhagic, vessel dissection or perforation) was performed.
Results
Endovascular neurointerventions in 84 patients (57 female and 27 male, mean age 67 years), using the Aristotle microwires during the primary study period were recorded: aneurysm treatment (n = 30), EVT in acute ischemic stroke (n = 46), dural venous sinus manometry and stenting (n = 7), as well as internal carotid artery stenting (n = 1). The Aristotle 18 microwire was used in conjunction with 0.021”. microcatheters (n = 30) and the Aristotle 24 microwire with the 0.027” (n = 51) or 0.033” microcatheters (n = 3). The target intracranial vessel locations for the endovascular aneurysm and EVT procedures are described in Table 1.
Target intracranial vessel locations for the endovascular aneurysm and thrombectomy procedures s dichotomised according to the type of microwire used.

Footnote: MCA – middle cerebral artery, ACA – anterior cerebral artery, BA – basilar artery, PCA – posterior cerebral artery, ICA – internal carotid artery, ACOM – anterior communicating artery.
The Aristotle 18 and 24 microwires were utilised in 16 and 30 EVT procedures respectively (total n = 46). Of this, first-line contact aspiration thrombectomy only was performed successfully in 33 cases, without the need to advance the microwire or microcatheter beyond the clot interface in all cases (100%). In 13 cases, the first-line combined technique of contact aspiration and stentretriever was used.
In 100% of the cases, the target vessel or aneurysm was reached with the Aristotle microwire, including advancement of the selected microcatheter. No procedure related complications were recorded.
Of the 50 cases using the 0.014 microwire during the secondary study period, 32 cases were EVT procedures, which were performed with a 0.021 microcatheter. Of the 32 EVT cases, 18 were performed with first-line contact aspiration only. Of these 18 procedures, 6 required crossing the clot/occlusion with the microwire/catheter to facilitate navigation of the large bore aspiration to the clot interface.
Overall, the target vessel and/or aneurysm was reached in all cases using the Synchro 0.014 microwire, and no procedural related complications were recorded.
The procedural characteristics are demonstrated in Table 2.
Procedural metrics dichotomised according to the type of microwire used.
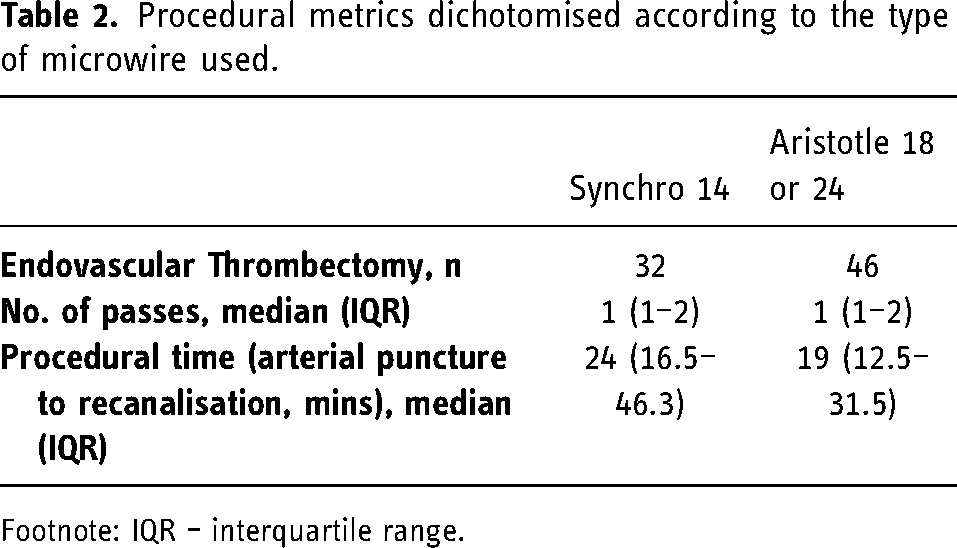
Footnote: IQR – interquartile range.
Discussion
In our early clinical experience, the new Aristotle 18 and 24 microwires have been shown to be safe and feasible in neurointerventional procedures, with successful endovascular navigation achieved in every case. No procedural related complications were attributed to the microwires.
The new family of Aristotle microwires has been an extremely useful tool at our institution. The smooth navigation of the larger diameter microwires in the distal intracranial vascular territory, the seamless advancement of the microcatheters into the anatomic targets and the significant decrease of the “ledge effect”, particularly at the ophthalmic artery origin, have contributed substantially to the success of the neurointerventional procedures, with a reduced risk of vessel or endothelial injury. 4
The wires are particularly useful to accommodate large bore microcatheters, which are required to advance intrasaccular flow disruptors or flow diverting stents used for endovascular aneurysm treatment. Previous reports have described the safe and effective ‘buddy-wire’ technique of concomitant use of two 0.014” microwires within large bore microcatheters particularly for flow diversion treatment of wide necked intracranial aneurysms. 6 The new Aristotle microwires would invariably negate the need for the ‘buddy-wire’ technique and may be more cost effective in such situations.
Another advantage of larger microcatheters and microwires consists of additional support to facilitate safe navigation of large bore aspiration catheters to the proximal aspect of the clot for aspiration thrombectomy in acute ischaemic stroke. 7 Contact aspiration technique in EVT, particularly with the advent of larger aspiration catheters, is particularly advantageous potentially reducing the time taken to achieve successful recanalisation and first pass effect.8,9 In addition, the use of a smaller microcatheter and an 0.014” microwire may involve crossing the clot advancing the microwire and microcatheter to the distal vasculature for support (usually requiring deployment of a stentretriever) to allow navigation of the large aspiration catheters to the clot interface, particularly in tortuous vascular anatomy. Crossing the clot may increase the risk of clot fragmentation and distal embolisation, which is associated with worse functional outcomes.10,11 To mitigate this effect, previous in vitro studies have demonstrated that the use of a wedge catheter reduces the ledge effect and facilitates the delivery of large aspiration catheters to the target vessel, whilst reducing the interaction with the occlusion site. 7 Similarly, the larger Aristotle microwires reduce any clot interaction during the navigation of larger aspiration catheters. Hence, there is a decreased risk of clot fragmentation, distal embolisation and, possibly, decreased procedure time. Of the 18 EVT procedures using the 0.014 microwire in our study, 6 required crossing the clot/occlusion with the microwire/catheter to facilitate navigation of the large bore aspiration to the clot interface. In comparison, none of the 33 EVT cases with first-line contact aspiration technique using the larger bore microwires/microcatheters required the need to advance the microwire/microcatheter beyond the clot/occlusion to facilitate advancement of the large bore aspiration catheter. Furthermore, there was a marginally increased procedural time (5 min) during the EVT cases where the 0.014 microwire was utilised, compared to those cases where larger bore microwires were used. This difference in procedural time may have been associated with the higher proportion of first-line contact aspiration technique used during EVT at our institution in the primary study period when larger bore microwires were used.
There are important factors for consideration in the selection of microwires for neurointerventional procedures, depending on the desired outcome or treatment target. For instance, microwires with less support due to size or appreciable transition from the softer tip to the stiffer proximal aspect, may require navigation into the distal and smaller vasculature to assist microcatheter navigation, particularly in challenging and tortuous anatomy. The tip stiffness is also of particular importance in neurointerventional procedures, given the fragility of the distal vessels and any perceived vascular abnormalities. These factors together may influence the risk of vessel perforation. Furthermore, the shape of the soft microwire tip and, subsequently, its intended response is frequently lost over time. This may necessitate the use of additional microwires, which invariably adds to the procedural costs and the length of the procedure. Overall, the use of the larger Aristotle microwires provide sufficient support which facilitates easier microcatheter navigation, without requiring advancement of the microwire into the distal vascular territory. In addition, the soft tip of the larger microwires could be likened to a blunt tip, with more rounded edges decreasing the risk of endothelial injury and inadvertent selection of perforator vessels, compared to the 0.014” microwires.
There are a few limitations of this study. First, due to the observational nature of this study, inherent selection biases may have influenced the results. However, this was minimised with the consecutive case selection for review. Second, although indirect comparison of procedural efficacy was reviewed with the Synchro 0.014 microwire, procedural comparison with other 0.014 microwires was not performed. Third, the cost effectiveness and procedural times of the neurointerventional procedures were likely confounded by multiple other procedural factors and devices, which precluded accurate comparisons with current standards.
Conclusion
The Aristotle microwires used in neurointerventional procedures are feasible and safe. Aristotle 18 and 24 microwires may provide reduced ledge gap, improved torquability, support and safety over standard 0.014” microwires.
Footnotes
Contributorship
Conception and drafting of the manuscript: VSN, PSH, LDV, LD, HR. Data collection and analysis: VCN, JPL, MB. Critical revision of the manuscript: All authors. All authors approved the final version of the manuscript.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical approval
This study was registered with and approved by the local institutional board review (EX/2023/QGC/97536). Retrospective patient consent was not required for this study which was conducted in a de-identified manner.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
