Abstract
We herewith report a young patient who had an incidental spinal vascular malformation of the cervicomedullary junction discovered during a work-up for anosmia. Angiography demonstrated a perimedullary spinal arteriovenous fistula with supply from lateral spinal arteries arising from bilateral V3 level segmental arteries. It was decided to manage the patient conservatively with magnetic resonance imaging monitored biannually. On a recent follow-up magnetic resonance, nearly 10 years later, we noted a subtle change in caliber and imaging characteristics at the posterior margin of the cervical medullary junction. Repeat digital-subtraction angiography showed no evidence of early venous filling from the previously involved branches. Microcatheter exploration of the right lateral spinal artery confirmed spontaneous occlusion of the spinal perimedullary arteriovenous fistula, without any persistent shunting. Spontaneous resolution of a spinal vascular malformation is rare; this case demonstrates the dynamic nature of shunting vascular malformations and that spontaneous obliteration of arteriovenous shunts is possible.
Case report
In 2013, at that time an 11-year-old patient had a work-up for anosmia during which a spinal vascular malformation of the cervicomedullary junction was incidentally discovered. The patient was asymptomatic neurologically, and magnetic resonance (MR) imaging of the spine showed no signs of spinal venous congestion and no signs of recent or remote hemorrhage. Angiography was performed and demonstrated a perimedullary spinal arteriovenous fistula with supply from lateral spinal arteries arising from bilateral V3 level segmental arteries. The fistula was located on the dorsal surface of the cord. There were no angioarchitecture weak-points such as feeding artery aneurysms, or venous outflow obstruction (Figure 1). Management options were discussed with the patient and family. Given the unclear natural history of asymptomatic spinal arteriovenous malformations (AVMs) and the potential risks of treatment, it was decided to manage the patient conservatively with yearly imaging follow-up and the patient was subsequently monitored with MR imaging biannually.
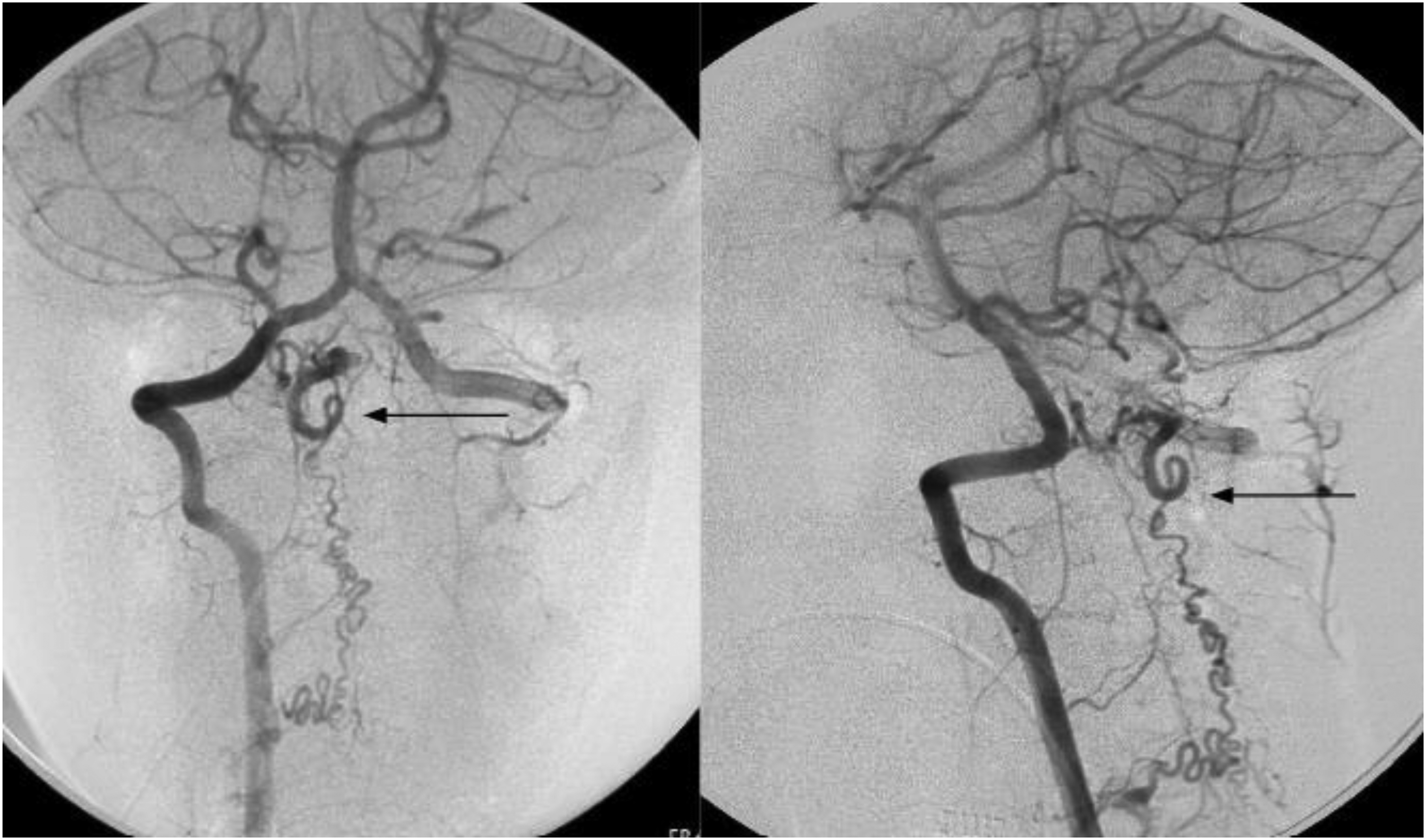
Index digital subtraction angiography demonstrated a pial AV fistula with feeders arising from the V3 segment of the right and left vertebral arteries (arrows) (left—AP view and right—lateral view).
On a recent follow-up MR as a now 21-year-old adult, MR imaging of the cervical spine (Figure 2) noted a subtle change in caliber and imaging characteristics at the posterior margin of the cervical medullary junction. There was no evidence of edema within the adjacent brainstem or interval hemorrhage. However, the subtle change in imaging characteristics, as well as advances in digital-subtraction angiography (DSA) imaging and overall endovascular management of spinal vascular malformations as well as a better understanding of the natural history of spinal vascular malformations prompted us to repeat the DSA to better inform the patient about current management options.
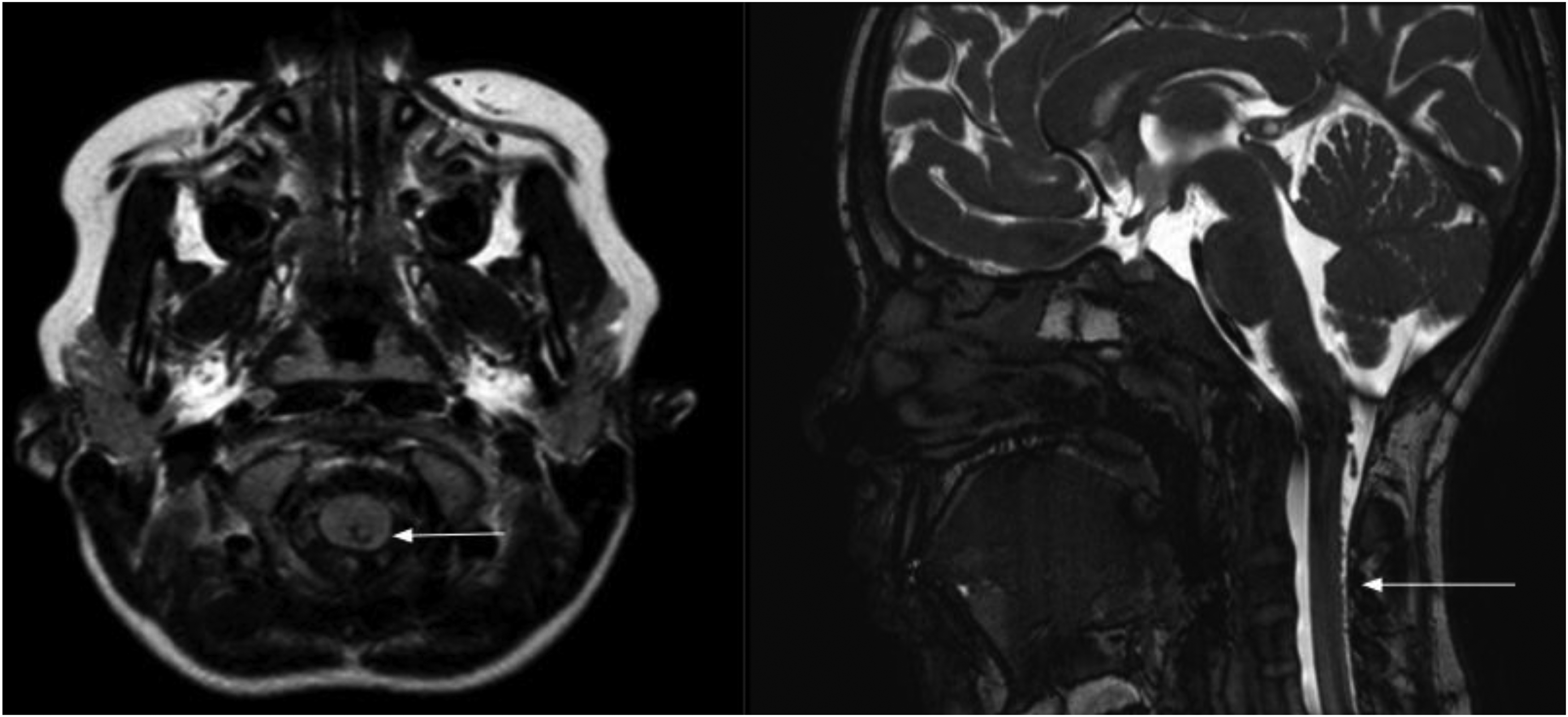
Magnetic resonance (MR) brain showing small flow voids seen within the central aspect of the posterior margin of the cervical medullary junction at the C1 level (left—axial view and right—sagittal view), which appeared to represent perimedullary veins (arrows).
On repeat DSA (Figure 3) there was now no longer evidence of early venous filling from the previously involved branches of the right and left vertebral artery V3 segments. The ASA and PSA show normal filling and emptying from other segmental arteries. Microcatheter exploration was performed of the right lateral spinal artery that confirmed spontaneous occlusion of the spinal perimedullary arteriovenous fistula, without any persistent shunting.
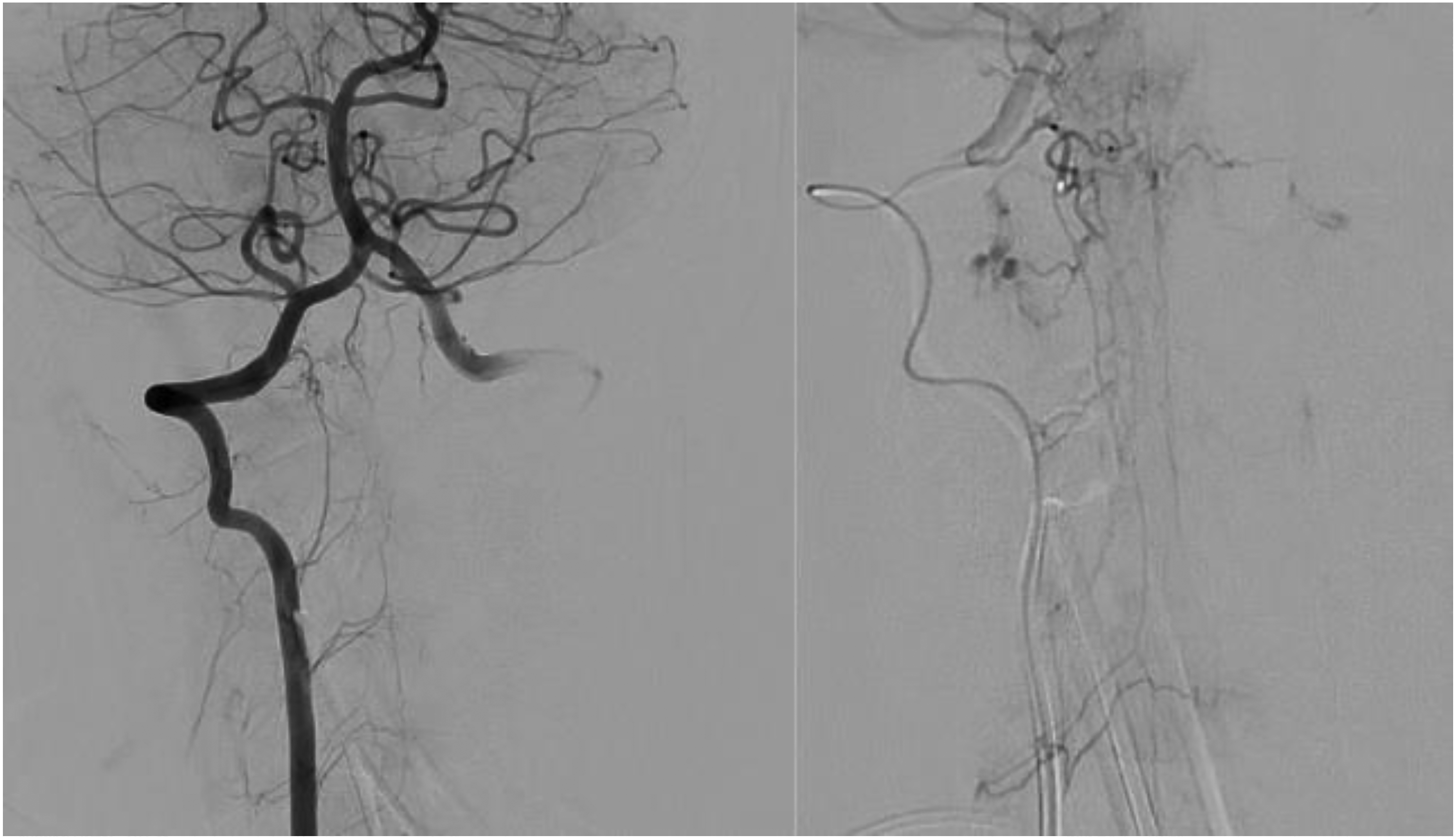
Repeat digital-subtraction angiography (DSA) showed no evidence of early venous filling from the previously involved branches of the right and left vertebral artery V3 segments. There was spontaneous occlusion of the spinal perimedullary arteriovenous fistula, without any persistent shunting (left—AP view and right—microcatheter injection through the feeder showing evidence of venous thrombosis).
Discussion
Spinal vascular malformations are rare, accounting for only 5%–9% of all central nervous system vascular malformations. 1
They can be classified 2 depending on the differentiation as shunting versus nonshunting lesions (cavernomas). Shunting lesions can be further classified depending on their feeding artery supply: those shunts fed by radiculomeningeal arteries constitute the dural arteriovenous fistulas, while shunts fed by the radiculomedullary and radiculopial are named the pial cord arteriovenous malformations. Pial AVMs can be further classified into glomerular (plexiform or nidus-type) AVMs with a network of intervening vessels in between the artery and vein and the fistulous pial AVMs. Depending on whether a fistula has a high or a low shunting volume, they can be further subdivided into “macro-” and “micro” fistulas. 3 Based on the classification our case is an intermediate flow perimedullary fistulous AVM with the shunt being fed by radiculopial arteries arising from the vertebral artery with no demonstrable nidus.
Spinal cord AVMs can present clinically either with progressive myelopathy or acute hemorrhage (subarachnoid or intramedullary). Acute neurological deficits which are non-hemorrhagic can also occur due to acute thrombosis of venous pouches with mass effect and disturbance of venous outflow. Nidus-type AVMs tend to have an increased risk of hemorrhage, while fistulous AVMs present more frequently with progressive myelopathy. 4 Treatment options for spinal vascular malformations include surgery or endovascular treatment. Surgery involves disconnection of the draining vein at the point where it emerges from the fistula. Endovascular treatment similarly requires complete obliteration of the proximal portion of the draining vein. In case of incomplete obliteration, other arterial feeders may be recruited, and recanalization of the fistula may occur. 5
The spontaneous resolution of a spinal vascular malformation is rare, as there are very few cases reported in the literature. Spontaneous obliteration has been described for dural AVF and low-flow epidural AVFs 6 but has not been described for perimedullary intermediate-flow AVFs. Mechanisms explaining the spontaneous resolution of vascular malformations include anatomical or hemodynamic factors such as single-channel venous drainage and draining vein thrombosis, or arterial vessel wall dissection. 7 Most of these causes eventually cause thrombosis as a common final event. Other contributing factors may include dehydration, trauma, and, catheter angiography procedures.8,9
We believe that this rare case can raise awareness of the dynamic nature of shunting vascular malformations and that spontaneous obliteration of arteriovenous shunts is possible.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: Dr Krings acknowledges the generous support from the Patricia Holt-Hornsby & Dan Andreae Vascular Research Unit and UMIT (University Medical Imaging Toronto).
