Abstract
Introduction
Middle meningeal artery embolization (MMAE) has emerged as a promising new treatment for patients with chronic subdural hematomas (cSDH). Its efficacy, however, upon the subtype with a high rate of recurrence—septated cSDH—remains undetermined.
Methods
From our prospective registry of patients with cSDH treated with MMAE, we classified patients based on the presence or absence of septations. The primary outcome was the rate of recurrence of cSDH. Secondary outcomes included a reduction in cSDH thickness, midline shift, and rate of reoperation.
Results
Among 80 patients with 99 cSDHs, the median age was 68 years (IQR 59–77) with 20% females. Twenty-eight cSDHs (35%) had septations identified on imaging. Surgical evacuation with burr holes was performed in 45% and craniotomy in 18.8%. Baseline characteristics between no-septations (no-SEP) and septations (SEP) groups were similar except for median age (SEP vs no-SEP, 72.5 vs. 65.5, p = 0.016). The recurrence rate was lower in the SEP group (SEP vs. no-SEP, 3 vs. 16.7%, p = 0.017) with higher odds of response from MMAE for septated lesions even when controlling for evacuation strategy and antithrombotic use (OR = 0.06, CI [0.006–0.536], p = 0.012). MMAE resulted in higher mean absolute thickness reduction (SEP vs. no-SEP, −8.2 vs. −4.8 mm, p = 0.016) with a similar midline shift change. The rate of reoperation did not differ (6.2 vs. 3.1%, p = 0.65).
Conclusion
MMAE appears to be equal to potentially more effective in preventing the recurrence of cSDH in septated lesions. These findings may aid in patient selection.
Introduction
With a global aging population, chronic subdural hematoma (cSDH) will become one of the most commonly encountered neurosurgical diseases by 2030. 1 The treatment of cSDH has traditionally involved surgical evacuation via craniotomy or burr hole drainage, however, this management is plagued by a high recurrence rate of ∼11%. 2 As a sentinel health event with high rates of recurrence and mortality despite surgical evacuation, middle meningeal artery embolization (MMAE) may be a promising primary or adjunctive treatment option for cSDHs.3,4
Traumatic damage to the dural border cell layer along with blood products from the hemorrhage promotes a proinflammatory cascade that leads to the formation of new membranes (or septations) and fragile capillaries within these and the outer subdural membrane. Fragile capillaries result in fluid leakage and microhemorrhages that lead to subdural accumulation and a subsequent self-propagating cycle. 5 In fact, septated cSDHs, which possess both of these pathological structures, have higher rates of recurrence.6–8 Unfortunately, septations pose a unique challenge to surgical evacuation given the formation of loculated collections and other septations that frequently extend beyond the surgical exposure. Because septations are believed to be vascularized by meningeal arteries, MMAE has been suggested as a promising treatment. 9 Despite these theoretical explanations, which in certain practices lead to patient selection, evidence to confirm the benefit of MMAE in septated cSDH over non-septated lesions is lacking. We sought to uncover the relative efficacy of MMAE among patients with septated cSDH as compared to those without septations.
Methods
Study design
This was a retrospective, single-center cohort study performed at a Level 1 Academic Trauma Medical Center from January 2018 to July 2022. Consecutive patients who underwent MMAE during this time period were included and categorized into septated and non-septated cSDH groups. A cSDH was classified as septated on CT imaging if it contained one or more linear hyperdensities within the lower-density hematoma as previously defined in the literature10,11 and exemplified herein (Figure 1). Non-septated cSDH was defined as hypodense, isodense, or mixed-density subdural hematoma with no evidence of linear hyperdensities within the hematoma. MMAE as either sole treatment or adjunctive to surgical intervention (burr holes or craniotomy) was performed at the discretion of the treating physician. The choice of embolization materials was also at the discretion of the neurointerventionalist and embolic materials were used in an off-label but well-supported fashion. The study was approved by the Institutional Review Board (#HSC-MS-21-0792). Informed consent was obtained from all patients or their legal guardians prior to the procedure.
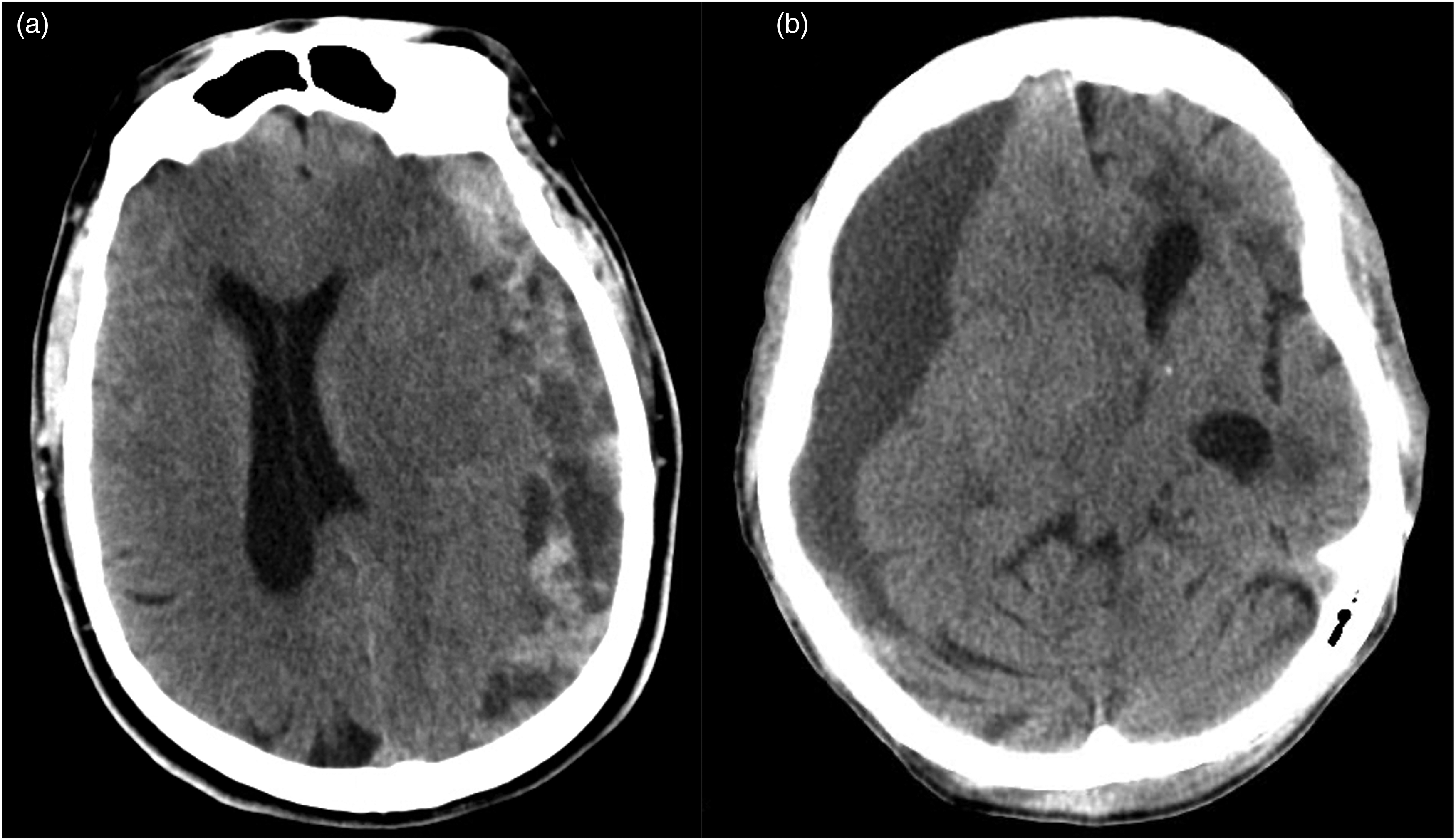
Representative noncontrast head CTs of (a) septated and (b) non-septated cSDHs.
Outcome measures
The primary outcome of the study was a recurrence of the cSDH within a follow-up period of 3 months post-MMAE. Follow-up inclusion time frame was selected based on prior literature and current ongoing MMAE clinical trial endpoints.12–16 Recurrence was defined as any increase in cSDH thickness or presence of new hemorrhage in the subdural space on repeat imaging within the follow-up period. Pre-embolization and post-surgical (when applicable) scans were used as the baseline. Secondary outcomes included rate of reoperation, change in cSDH thickness and midline shift during the same time period.
Imaging analysis
cSDH were identified on hospital admission based on computed tomography (CT) scan demonstrating a mixed density or hypodense subdural collection. Radiographic measurements were performed by neuroendovascular physicians. cSDH thickness was defined as the longest distance in millimeters on coronal CT imaging between the brain surface to the perpendicular inner table of the skull using scale bars. Similarly, midline shift was measured based on the degree of lateral displacement of the septum pellucidum at the level of the foramen of Monro.
Statistical analysis
The Student's t-test for continuous variables and Fisher's exact test for categorical variables were used to compare the baseline characteristics, on a per-patient basis, and clinical outcomes, on a per-subdural basis, between the septated and non-septated groups. A Kaplan–Meier approach stratified by group was used to construct recurrence-free survival curves, with differences between the curves assessed using a Cox proportional hazard test. For missing data points, there was no imputation performed. A significance level of p < 0.05 for two-tailed test was set and analyses were performed using STATA 16.0 (StataCorp, College Station).
Results
A total of 80 patients who underwent 96 embolizations (19 bilateral) were included. The median age was 68 years [IQR 59–77] and 25% were females. Pre-embolization and post-operative (when applicable) mean SDH thickness was 14.1 mm and mean midline shift was 4 mm. Evacuation of the cSDH with burr holes was performed in 45% and craniotomy in 18.8% of the total number of cSDHs. MMAE was performed with liquid embolic agents only (27/96), coils only (10/96), particles only (8/96), particles in addition to coils (47/96), and liquid embolic agents and coils (4/96).
Within the cohort, 28/80 patients (35%) had a septated cSDH. cSDHs in this group were older (SEP vs. no-SEP, 72.5 vs. 65.6, p = 0.016) and had a larger SDH baseline thickness (SEP vs. no-SEP, 17.4 vs. 12.4 mm, p < 0.001). There was no significant difference in other baseline characteristics including rate and type of surgical evacuation or embolization material (Table 1). Median follow-up CT scan was similar between groups (SEP vs. no-SEP, 25 vs. 24 days p = 0.85).
Baseline characteristics by treatment group. Data analyzed by student's t-test for continuous variables, or fisher's exact for categorical variables.
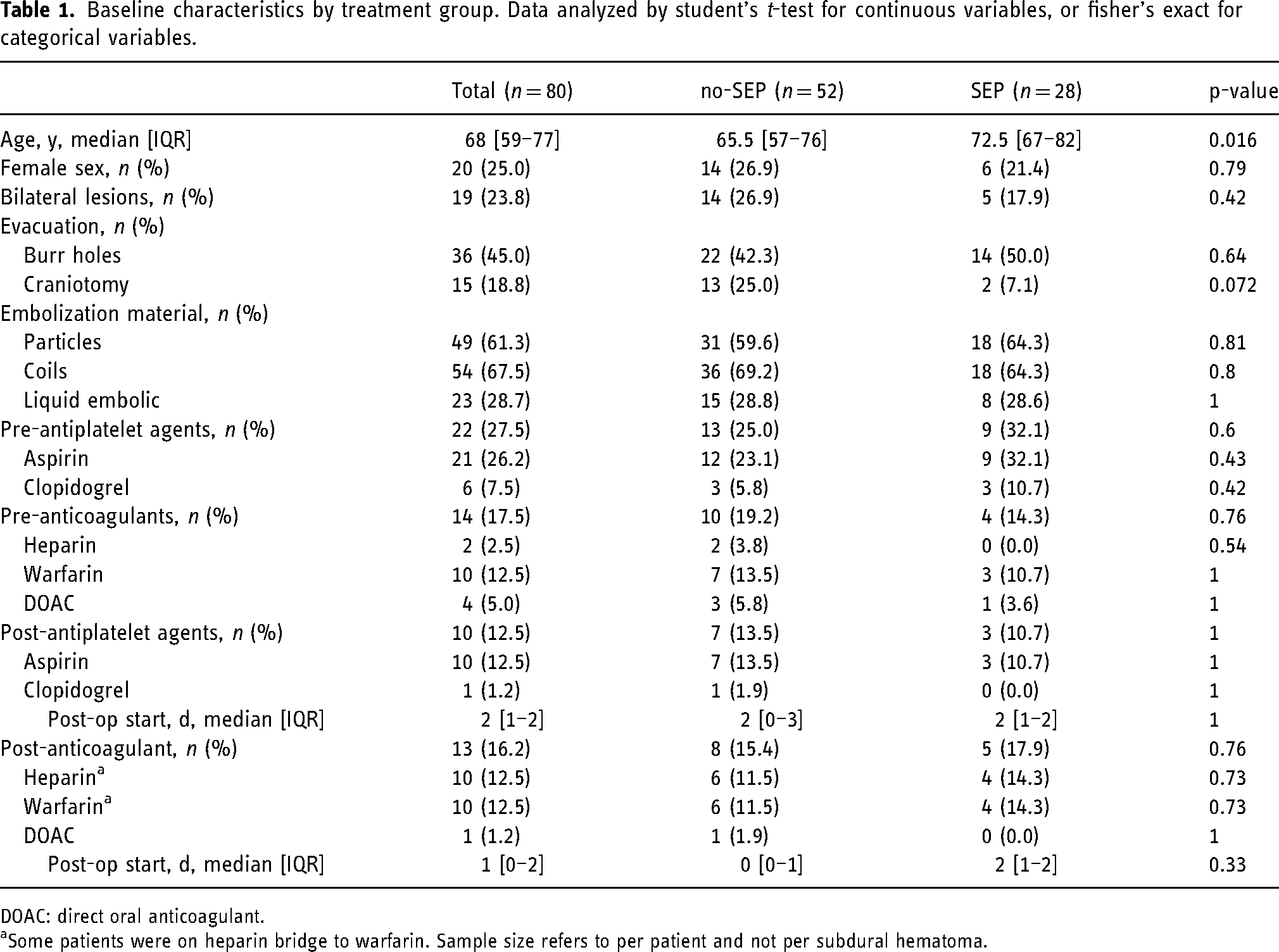
DOAC: direct oral anticoagulant.
aSome patients were on heparin bridge to warfarin. Sample size refers to per patient and not per subdural hematoma.
The primary outcome of the recurrence rate was lower in the septated group (SEP vs. no-SEP, 3.1% vs. 23.4%, p = 0.017) with only one patient having a recurrence in the septated group (Table 2). Interestingly, the only patient with septations who suffered recurrence was anticoagulated throughout the pre- and post-MMAE time periods for mechanical aortic valve and heart failure with reduced ejection fraction. Septated patients were less likely to experience recurrence after MMAE even when controlling for evacuation strategy and use of antithrombotics before or after treatment (OR = 0.06, CI [0.01–0.53], p = 0.012). Recurrence-free survival was significantly improved among embolized patients with septated cSDH (Figure 2, p = 0.0147). The mean change in cSDH thickness was greater in the septated group (SEP vs. no-SEP, −8.2 vs. −4.8 mm, p = 0.03), despite a thicker baseline SDH in the septated group (Table 2). There was no significant difference in midline shift change after MMAE. The rate of reoperation was similar between groups (septated vs. non-septated, 3.1 vs. 6.2%, p = 0.66). In total, there were four peri-procedural complications in the cohort. These included new embolic strokes in two patients, one peripheral seventh nerve palsy and monocular blindness in one patient.
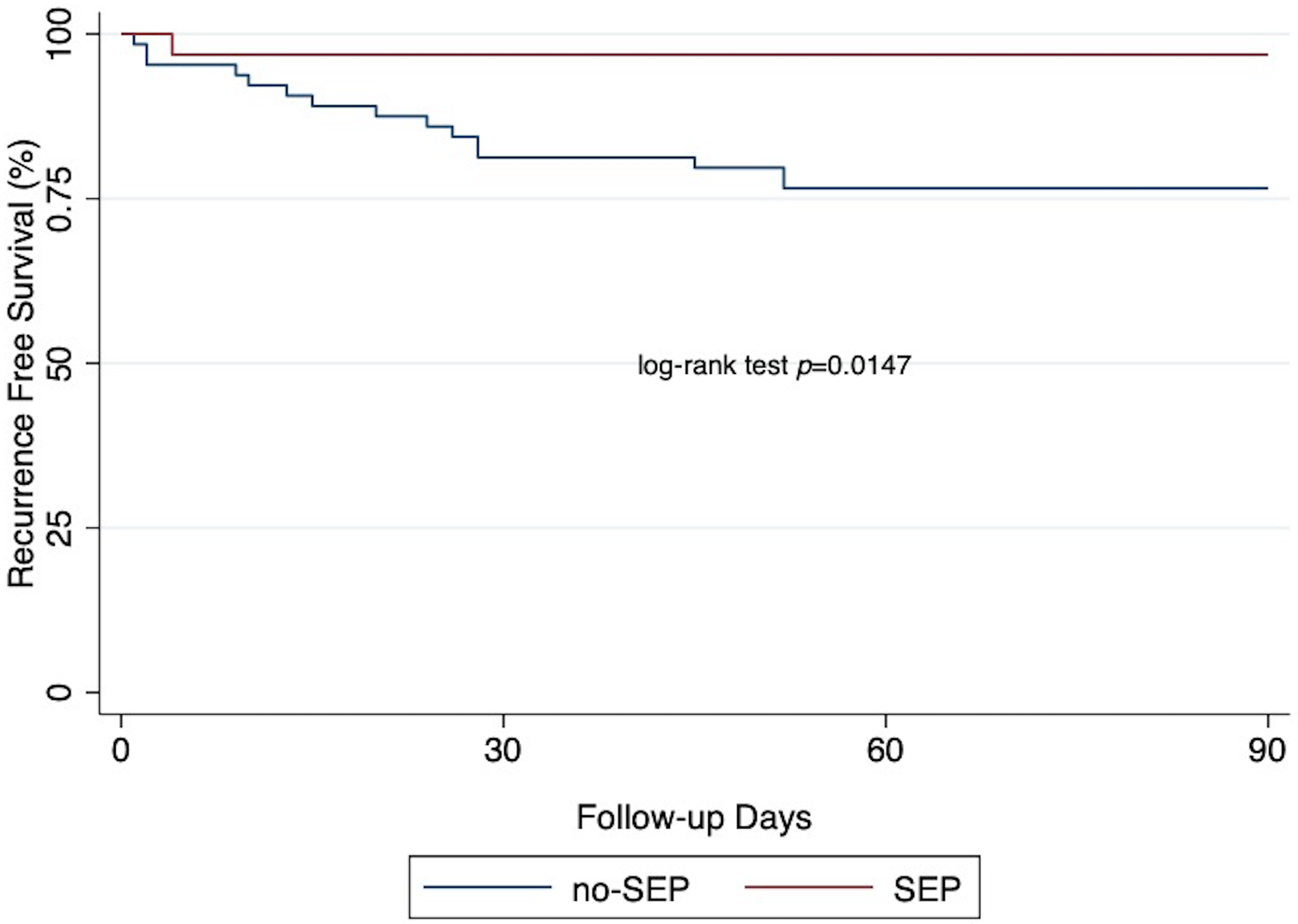
Kaplan–Meier curves for septated (SEP) and non-septated (no-SEP) groups. Curves show recurrence-free survival percentage over time within 90 day follow up period. Survival curve for SEP is significantly different from those in the no-SEP group (p = 0.0147, log-rank test).
Lesion characteristics and outcomes by treatment group.
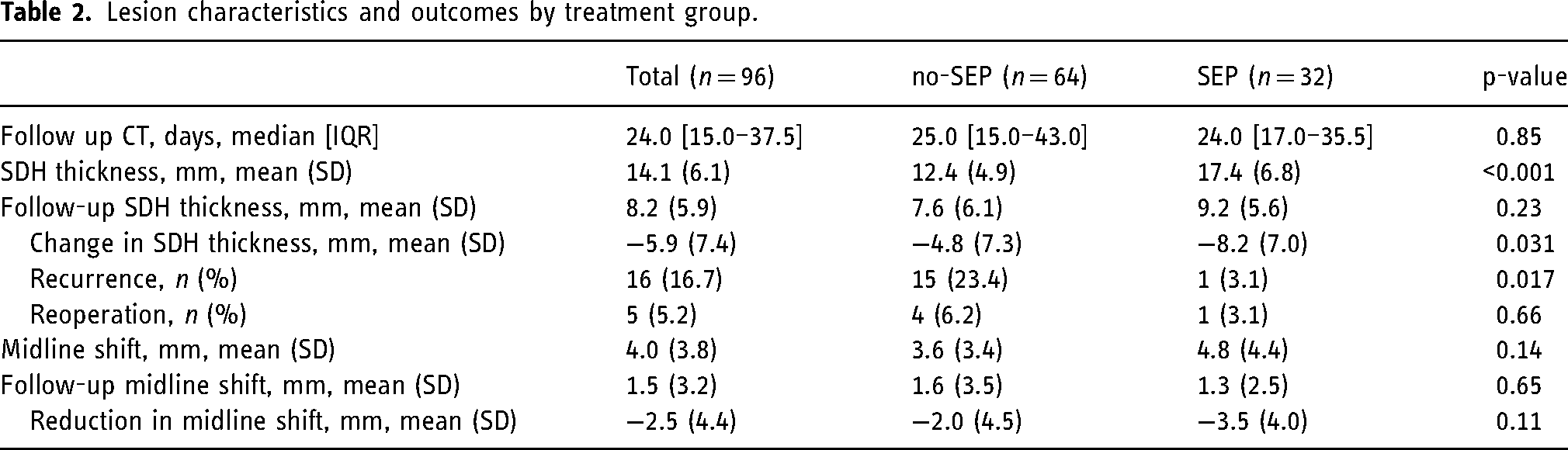
Discussion
cSDH is increasingly prevalent in the aging population and is projected to become one of the most frequent neurosurgical diseases within the next decade. 1 MMAE has emerged as a promising primary or adjunctive treatment for the prevention of the recurrence of cSDH. Septated cSDH represents a unique subgroup with both lower success rate of a complete evacuation and higher rates of recurrence. In our cohort, patients with septations had significantly lower rates of recurrence following MMAE (SEP vs. no-SEP, 3.1% vs. 23.4%, p = 0.017) with similar rates of reoperation. After controlling for clinically relevant factors including evacuation strategy and use of antithrombotics, embolized septated patients had significantly lower odds of recurrence.
The presence of septations is thought to occur in the later stages of cSDH 10 and may represent a more mature and more densely neovascularized environment, a putative target for MMAE. Our findings are contrary to a recent study by Khorasanizadeh et al. which found no significant difference in the rate of recurrence by cSDH morphologies. 17 Several possible explanations exist. Our larger sample size of septated lesions (35% vs. 17%) is likely an important distinction. Moreover, their morphological classification was wider and not focused exclusively on septated cSDHs. Also, our study included surgically evacuated cSDHs, a more representative cohort which in turn also highlights the potential synergistic effect between surgery and MMAE.
Our findings suggest that despite their notoriously higher rates of recurrence, septated cSDHs respond equally or better than their non-septated counterparts. Importantly, this benefit of MMAE in septated lesions does not preclude benefit in non-septated cSDHs. Our study was not designed or powered to make this conclusion. While the presence of septations may be a treatment effect modifier, our results should be interpreted with caution as to not exclude patients from undergoing this promising intervention. Using less restrictive criteria, similar to the ongoing randomized trials, will likely lead to a higher number of treated individuals and potentially a larger populational benefit than restricting candidacy. As such, our study is not meant to promote restrictive selection criteria, but to inform the likelihood of benefit from MMAE while we await the results of ongoing randomized trials.
Our retrospective study has several limitations. First, we did not compare outcomes to a non-embolized cohort which limits our ability to make overreaching conclusions. We excluded patients with no follow-up imaging, possibly introducing selection bias. In addition, our follow-up period was 90 days, which was in line with some, but not all ongoing pivotal trials, and longer-term follow-up may be needed to fully uncover the effects of MMAE. The optimal timing for follow-up MMAE-treated patients is unknown and outcome discrepancies in the literature are the norm. 18
Conclusions
Septated cSDH represents a challenging entity with poor surgical evacuation outcomes and a higher risk of recurrence. However, the high density of neovascularized membranes and septations makes them a prime target for MMAE. Our findings suggest that septated cSDH benefits from MMAE perhaps even more than non-septated cSDH. While we await randomized trial results, the presence of septations may inform on the likelihood of response to MMAE.
Footnotes
Authors’ Notes
Juan Carlos Martinez-Gutierrez and Salvatore A. D’Amato contributed equally.
Authors’ contribution
JCMG and SAD contributed to the conception, writing, and acquisition of clinical data; JCMG and YK performed statistical analysis; HAZ, MIN, MJK, and HWK contributed to the acquisition of clinical data; BHD, PRC, SLB, SAS, GS, CJC, AM, RSK, and MJD contributed to the critical appraisal of the manuscript.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
